Mar 20, 2026

Some tirzepatide users report unrelenting thirst from the moment they start their first injection. Others barely notice a change in how much water they drink. And a small group actually finds they are less thirsty than before, forgetting to drink water altogether because the medication suppresses their desire for fluids.
The difference between these experiences comes down to biology, dosage, hydration habits, and a fascinating contradiction buried deep in the pharmacology of GLP-1 receptor agonists. If you have been searching for answers about why tirzepatide and dry mouth seem to go hand in hand, or why your water bottle is suddenly your constant companion, you are not imagining things. Thirst on tirzepatide is real. But the reasons behind it are more complex than most articles will tell you. This guide breaks down every mechanism, every research finding, and every practical strategy you need to understand what is happening in your body, when to worry about it, and how to manage it effectively. Whether you are on a compounded tirzepatide starting dose of 2.5 mg or titrating up through higher doses, this article covers the full picture of tirzepatide and thirst, from GLP-1 receptor biology in the kidneys to simple hydration strategies that actually work.
The short answer: yes, and here is why
Tirzepatide can make you thirsty. But here is the thing most people miss: thirst is not listed as a direct side effect in the FDA prescribing information for Mounjaro or Zepbound. That does not mean it is not happening. It means the thirst you experience is almost always a secondary effect, a downstream consequence of other well-documented changes tirzepatide triggers in your body.
Think of it this way. Tirzepatide activates both GLP-1 and GIP receptors. These receptors exist in your gut, your pancreas, your brain, your kidneys, and even your salivary glands. When you activate all of them simultaneously, the ripple effects are enormous. Some of those ripple effects make you lose fluid. Others reduce saliva production. A few change how your brain perceives thirst itself.
The result is complicated.
An estimated 1 to 10 percent of tirzepatide users report noticeable thirst, though this number likely underrepresents reality because many people do not report mild symptoms to their healthcare provider. The thirst usually shows up within the first few weeks of treatment or after a dose increase, and for most users it settles down within 2 to 4 weeks on a stable dose. Understanding what to expect after your first dose of tirzepatide helps set realistic expectations. Your body needs time to adjust. Most of these fluid-related symptoms are temporary. But knowing why they happen gives you the power to manage them effectively rather than just suffering through them.
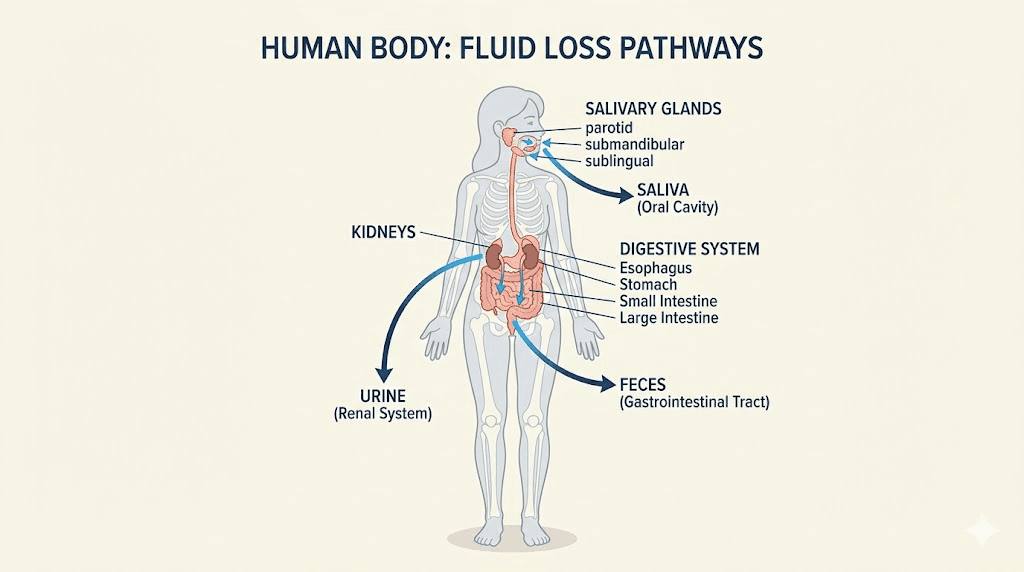
The mechanisms fall into five major categories. Gastrointestinal fluid loss. Kidney-level sodium excretion. Salivary gland suppression. Reduced food and fluid intake. And blood sugar normalization. Each one contributes to the overall sensation of thirst, and most tirzepatide users experience at least two or three of these simultaneously. If you have been dealing with tirzepatide fatigue alongside your thirst, the connection between dehydration and tiredness is stronger than you might think.
Five reasons tirzepatide makes you thirsty
Reason one: gastrointestinal fluid loss
The most obvious culprit. Nausea affects 15 to 30 percent of tirzepatide users. Diarrhea hits 13 to 24 percent. Vomiting occurs in 6 to 12 percent. Every episode of vomiting or diarrhea pulls water and electrolytes out of your body. Even nausea without vomiting can reduce your desire to drink, creating a paradox where you need more fluid but consume less.
This matters more than most people realize.
When you lose fluid through GI side effects, your blood volume drops. Your kidneys detect this decrease and signal your brain that you need water. The result is thirst. If you are experiencing tirzepatide diarrhea, your fluid losses can be substantial, sometimes exceeding a liter per day beyond normal. That is a liter of water your body needs to replace just to stay at baseline. Pair that with tirzepatide bloating that makes you not want to drink, and you have a recipe for persistent dehydration and the thirst that comes with it. Managing tirzepatide constipation also requires adequate fluid intake, so getting your hydration right addresses multiple GI concerns at once.
Reason two: kidney natriuresis and fluid shifts
This is where the science gets interesting. GLP-1 receptors are not just in your gut. They sit on the cells of your kidneys, specifically in the proximal tubules where sodium reabsorption happens. When tirzepatide activates these renal GLP-1 receptors, it increases sodium excretion, a process called natriuresis. Sodium pulls water with it. So you lose both sodium and water through your urine.
Your body notices immediately.
The drop in sodium triggers a thirst response designed to restore electrolyte balance. This is the same mechanism that makes you thirsty after eating a bag of potato chips, except in reverse. Instead of too much sodium making you thirsty, losing sodium makes you thirsty because your body wants to dilute what remains. The SURPASS-4 clinical trial actually showed kidney-protective effects from tirzepatide, likely through this same natriuretic mechanism that reduces fluid overload and blood pressure. So the same process causing your thirst may actually be protecting your kidneys long-term. Tirzepatide is not a diuretic in the traditional sense. It does not force your kidneys to dump water the way furosemide or hydrochlorothiazide would. But the natriuretic effect creates a mild, constant increase in urinary fluid and sodium loss that adds up over time.
Understanding whether tirzepatide increases metabolism helps complete this picture, because metabolic changes also influence fluid requirements.
Reason three: salivary gland effects and dry mouth
GLP-1 receptors exist in your salivary glands. Activation of these receptors may reduce saliva production, creating a sensation of dry mouth that many people interpret as thirst. But dry mouth and thirst are not the same thing. We will explore this critical distinction in a later section.
There is also a mechanical component. Tirzepatide suppresses appetite dramatically. You eat less. You chew less. Chewing stimulates saliva production through a reflex arc that runs from the muscles of mastication through the brainstem and back to the salivary glands. When you chew less, this reflex fires less often. Saliva production drops. Your mouth feels dry. You reach for water. The connection between tirzepatide and dry mouth is well-documented by users, even though it does not appear prominently in clinical trial data. Some researchers believe the autonomic nervous system effects of GLP-1 receptor activation also play a role, altering the parasympathetic signaling that controls salivary gland function.
Reason four: reduced food and fluid intake
People forget that a huge portion of daily water intake comes from food. Fruits, vegetables, soups, sauces, all of these contribute to your hydration. When tirzepatide cuts your appetite and you eat 30 to 50 percent less food, you also lose that food-associated fluid intake. If you are following a tirzepatide diet plan, you need to account for this gap.
The math is straightforward. A typical diet provides 500 to 700 mL of water from food alone. Cut your food intake in half, and you lose 250 to 350 mL of daily water, roughly the equivalent of a large glass. That does not sound like much. But over days and weeks, a consistent 300 mL daily deficit adds up. Your body adapts by triggering thirst signals to compensate. Knowing what to eat on tirzepatide becomes essential not just for nutrition but for maintaining hydration through food sources. Choosing water-rich foods like cucumbers, watermelon, and soups can partially offset this deficit without requiring you to force down extra glasses of water. Check out tirzepatide meal plans that account for hydration alongside nutrition.
Reason five: blood sugar normalization and metabolic water shifts
Tirzepatide lowers blood sugar. Significantly. For people with elevated glucose levels before starting treatment, this normalization changes how the kidneys handle water. High blood sugar causes osmotic diuresis, where glucose spills into urine and pulls water with it. When tirzepatide brings blood sugar down, the osmotic diuresis stops. But the transition period can create temporary shifts in how your body distributes fluid between cells and the bloodstream.
Some people experience this as thirst.
During the first few weeks, your body is recalibrating its fluid balance mechanisms to account for a new metabolic reality. The first month on tirzepatide involves numerous adjustments happening simultaneously, and thirst is just one of them. Your kidneys are adapting. Your gut is adapting. Your brain is recalibrating its thirst and hunger signals. All at once. That is why the first month tends to be the most intense for side effects, including thirst, and why symptoms generally improve as your body reaches a new equilibrium. Monitoring how fast tirzepatide works alongside your side effect timeline helps you understand where you are in the adjustment process.
The GLP-1 thirst paradox: why the science seems contradictory
Here is something that will confuse you. Research from SUNY Buffalo, led by Daniels and colleagues, demonstrated that GLP-1 receptor agonists actually suppress water intake in animal models. They called it the "hypodipsic effect," a reduction in the desire to drink that is independent of food intake effects. Central nervous system GLP-1 receptor activation directly suppresses water-seeking behavior.
Wait. How can a medication that suppresses thirst in research also make users thirsty?
The answer lies in the difference between central and peripheral effects. In the brain, GLP-1 receptor activation tells your thirst centers to calm down. You do not want water as much. But in the periphery, in your kidneys and gut and salivary glands, tirzepatide is causing real, measurable fluid losses. Your body is genuinely dehydrating. So you have two competing signals: a brain saying "you do not need water" and a body that desperately does.
This creates the paradox.
Some users experience the central suppression more strongly. They do not feel thirsty even though they are dehydrated. These are the people who need to set reminders to drink because their thirst mechanism is being chemically overridden. Other users experience the peripheral dehydration more strongly. They feel constantly thirsty because their body fluid losses overpower the central suppression. And then there is a middle group that fluctuates between the two, feeling thirsty one day and forgetting to drink the next.
The animal research makes this even more fascinating. Exendin-4, a GLP-1 receptor agonist similar to the GLP-1 component of tirzepatide, suppressed water intake in rats for more than 4 hours after administration. Liraglutide, another GLP-1 agonist, suppressed water intake for up to 12 hours. Native GLP-1 only suppressed intake for about an hour due to its short half-life. These findings suggest that the longer a GLP-1 agonist stays active in your system, the stronger the central thirst suppression becomes. Tirzepatide has a half-life of approximately 5 days, meaning this suppression could be constant. Yet users still report thirst. The peripheral dehydration mechanisms are that powerful. If you are comparing medications and side effect profiles, understanding the differences between semaglutide and tirzepatide side effects helps put this in perspective. Some users find that how semaglutide makes you feel differs from tirzepatide in terms of thirst specifically because tirzepatide activates both GLP-1 and GIP receptors.
The practical implication is critical. Do not rely on your thirst signals alone while taking tirzepatide. They may be suppressed even when your body needs fluid. Track your water intake. Watch for signs of dehydration that have nothing to do with thirst, like dark urine, headaches, and fatigue.
Dry mouth versus true thirst: two different problems
People use the word "thirsty" to describe two completely different sensations. And on tirzepatide, distinguishing between them matters for how you respond.
True thirst: a systemic dehydration signal
True thirst originates in the hypothalamus. It is your brain responding to changes in blood osmolality, the concentration of dissolved particles in your blood. When osmolality rises above approximately 285 mOsm/kg, osmoreceptors in the hypothalamus fire. You feel an urgent, deep need for water. This is not a mouth sensation. It is a body sensation. You feel it in your throat, your chest, your gut. Drinking water satisfies it relatively quickly, usually within 10 to 15 minutes, because the osmoreceptors detect the incoming fluid before it even fully absorbs.
On tirzepatide, true thirst signals dehydration from fluid losses through the GI tract, increased urinary output from natriuresis, or inadequate fluid intake from reduced appetite. It responds well to drinking water.
Dry mouth: a local salivary problem
Dry mouth feels different. It is a sensation confined to the mouth itself. Your tongue feels sticky. Your lips feel dry. Speaking becomes difficult. Swallowing without liquid feels uncomfortable. But critically, drinking water provides only temporary relief. You take a sip, your mouth feels better for 30 seconds, and then the dryness returns.
This is because dry mouth on tirzepatide is not caused by insufficient total body water. It is caused by reduced saliva production from GLP-1 receptor effects on salivary glands and from reduced chewing stimulation. No amount of water will fix a salivary gland that is producing less saliva. You need different strategies.
How to tell which one you have
Ask yourself these questions. Does drinking a full glass of water resolve the sensation for more than 5 minutes? If yes, you are experiencing true thirst. Drink more water throughout the day. Is your urine dark yellow or amber? True thirst and dehydration. Increase fluid intake. Does the sensation return immediately after sipping water? Dry mouth. You need saliva-stimulating strategies, not just more water. Is the discomfort limited to your mouth, or does it feel like a whole-body need? Mouth only equals dry mouth. Whole-body equals true thirst.
Many tirzepatide users experience both simultaneously, which makes management trickier. Understanding whether tirzepatide gives you energy or drains it can also help distinguish dehydration-related fatigue from medication effects. If you are also dealing with tirzepatide headaches, dehydration is often the first thing to rule out, and headache treatment on tirzepatide frequently starts with improving hydration.
Management strategies by type
For true thirst, the solution is straightforward. Increase your total daily fluid intake. Aim for the National Academies recommendation of 3.7 liters per day for men and 2.7 liters per day for women, then add extra to account for GI losses and natriuresis. Spread intake throughout the day rather than chugging large amounts at once.
For dry mouth, try these approaches. Chew sugar-free gum to stimulate saliva production through the mastication reflex. Suck on ice chips for slow, continuous oral moisture. Use a humidifier at night if you wake up with severe dry mouth. Limit caffeine and alcohol, both of which worsen dry mouth. Consider an alcohol-free mouthwash designed for dry mouth conditions. Breathe through your nose rather than your mouth, especially during sleep. If you want to know whether you can drink alcohol on tirzepatide, the dry mouth consideration is just one more reason to be cautious. Alcohol dehydrates and reduces saliva production, compounding both problems.
How common is thirst on tirzepatide
Quantifying thirst prevalence on tirzepatide is tricky because it is not a primary endpoint in clinical trials. The SURPASS and SURMOUNT trials did not specifically track thirst as a standalone adverse event. What they did track were related symptoms: dry mouth, nausea, diarrhea, and vomiting, all of which contribute to thirst indirectly.
Based on available data and user reports, here is what we know.
Approximately 1 to 10 percent of tirzepatide users report thirst as a noticeable symptom. This estimate comes from post-marketing surveillance data, patient forums, and the prevalence of related GI side effects that cause dehydration. The actual number is likely higher because mild thirst often goes unreported. People simply drink more water and move on. Comparing this to semaglutide versus tirzepatide side effects, the thirst profile appears similar between both GLP-1 receptor agonists, suggesting the mechanism is primarily GLP-1 mediated rather than GIP mediated.
When thirst typically appears
Most users notice thirst in one of three windows. The first window is days 1 through 7 after the very first injection. Your body encounters GLP-1 and GIP receptor activation for the first time. Everything is new. GI side effects tend to peak during this window, and the associated fluid losses trigger thirst. Understanding what to expect after your first dose can help you prepare with adequate fluids before the side effects hit.
The second window is dose escalation. Every time you increase your dose, whether from 2.5 mg to 5 mg, or from 10 mg to 12.5 mg, GI side effects can flare again. Each escalation brings a new round of fluid shifts and GI disruption that triggers thirst. Following a tirzepatide dosing guide helps you plan your hydration around each step up. Some users find that microdosing tirzepatide reduces the intensity of side effects, including thirst, by allowing more gradual receptor adaptation.
The third window is the first 2 to 4 weeks on any given dose. After this adaptation period, most users find that thirst normalizes as GI side effects subside and their kidneys adjust to the new level of GLP-1 receptor activation.
Who experiences it more
Certain groups report thirst more frequently. People with pre-existing dry mouth conditions. Those taking other medications that cause dehydration, like certain blood pressure medications or stimulants. Users who start at higher doses rather than following the recommended slow titration. People who exercise heavily without adjusting their fluid intake. And individuals living in hot, dry climates where baseline fluid needs are already elevated. If you notice you are still hungry on tirzepatide, the thirst and hunger signals can sometimes get confused, especially during the adjustment period.
When thirst signals something more serious
For most people, thirst on tirzepatide is a nuisance. Annoying but manageable. Temporary. But in rare cases, it can signal something that requires medical attention.
Dehydration warning signs
Mild dehydration causes thirst, slightly darker urine, and mild fatigue. Moderate dehydration adds dry skin that stays "tented" when pinched, significantly reduced urine output, dizziness when standing, and rapid heartbeat. Severe dehydration presents with confusion, very dark or absent urine, extreme fatigue, fainting, and sunken eyes. If you reach moderate dehydration, increase fluid intake aggressively and consider oral rehydration solutions. If you reach severe dehydration, seek emergency medical care.
The connection between dehydration and other tirzepatide side effects is worth noting. Tirzepatide fatigue worsens with dehydration. Headaches on tirzepatide are frequently triggered by inadequate fluid intake. Even tirzepatide insomnia can worsen when you are dehydrated, because dehydration activates stress hormones that interfere with sleep.
SIADH: a rare but serious concern
There exists a case report in the medical literature of tirzepatide-induced syndrome of inappropriate antidiuretic hormone secretion, known as SIADH. In this condition, the body retains too much water, diluting sodium to dangerously low levels. Paradoxically, SIADH can cause thirst despite water retention because the low sodium triggers compensatory mechanisms.
This is rare. Extremely rare.
But the consequences are serious, including seizures. The reported case involved a patient who developed severe hyponatremia (low sodium) with neurological symptoms. Signs of SIADH include persistent thirst despite drinking large amounts of water, swelling in the hands or feet, nausea unrelated to the medication timing, confusion or difficulty concentrating, and in severe cases, seizures. If you are drinking adequate water and your thirst is not resolving, or if you develop swelling, confusion, or neurological symptoms, contact your healthcare provider immediately. They can check your sodium levels with a simple blood test. Gallbladder concerns on tirzepatide represent another rare but serious condition to monitor, and some symptoms can overlap with dehydration symptoms, making awareness important.
Kidney function monitoring
While the SURPASS-4 trial demonstrated kidney-protective effects from tirzepatide overall, individual responses vary. If you have pre-existing kidney disease or take other medications that affect kidney function, the natriuretic effects of tirzepatide could compound into more significant fluid and electrolyte shifts. Regular kidney function monitoring through blood tests is standard practice for anyone on GLP-1 receptor agonist therapy. Ask your prescriber about checking your BMP (basic metabolic panel) periodically, especially during dose escalation phases. Understanding the benefits of tirzepatide beyond weight loss includes recognizing its kidney-protective properties, but this does not eliminate the need for monitoring.
Your complete hydration strategy on tirzepatide
Knowing why you are thirsty is useful. But knowing what to do about it is what actually helps. Here is a comprehensive hydration strategy designed specifically for tirzepatide users.
Daily water intake targets
The National Academies of Sciences, Engineering, and Medicine recommend 3.7 liters per day of total water intake for men and 2.7 liters per day for women. This includes water from food, which typically accounts for about 20 percent. On tirzepatide, you should aim for the higher end of these recommendations and then add extra to compensate for GI losses and natriuresis.
A practical target: 2.5 to 3.5 liters of actual drinking water per day for women on tirzepatide. 3.0 to 4.0 liters for men. Adjust upward if you exercise, live in a hot climate, or are experiencing active GI side effects.
But do not overdo it.
Drinking excessive water without adequate electrolyte intake can worsen hyponatremia, the very condition we discussed in the SIADH section. More is not always better. Balance is the goal. Taking appropriate supplements with tirzepatide supports this balance, particularly electrolyte supplements during the adjustment period.
Timing your fluid intake
When you drink matters almost as much as how much you drink. Front-loading your water intake in the morning helps because you wake up mildly dehydrated after 7 to 8 hours without fluid. Drink 500 mL within the first hour of waking. Then maintain steady intake throughout the day, aiming for 200 to 300 mL every hour during waking hours. Reduce intake 2 hours before bed to minimize nighttime bathroom trips that disrupt sleep.
On injection day, pay extra attention. Whether you find the best time to take your tirzepatide shot is morning or evening, increase your fluid intake by 500 mL on injection day and the day after. This is when GI side effects tend to peak, and proactive hydration can reduce their severity. Some users take their injection on a specific day of the week that allows them to manage the initial side effect window at home where they have easy access to fluids.
Beyond plain water
Plain water is not always the best hydration strategy. When you are losing sodium through natriuresis and electrolytes through GI effects, water alone can dilute your remaining electrolytes further. Consider these alternatives. Coconut water provides natural electrolytes, including potassium. Bone broth delivers sodium, potassium, and protein. Oral rehydration solutions like Pedialyte or LMNT provide precisely balanced electrolytes. Herbal teas count toward fluid intake and provide variety. Diluted fruit juices (1 part juice to 3 parts water) add flavor and mild electrolytes. If you are looking at the best time of day to inject tirzepatide, consider choosing a time that allows you to focus on hydration during the peak side effect window.
Avoid relying on caffeinated beverages as your primary fluid source. Coffee and tea have mild diuretic effects that can compound the natriuresis from tirzepatide. One or two cups per day is fine. But your baseline hydration should come from non-caffeinated sources.
Foods that fight dehydration on tirzepatide
When your appetite is suppressed and you are eating less, every bite counts, not just for calories and nutrients but for hydration too. Choosing water-rich foods can add 500 mL or more of daily fluid intake without requiring you to drink extra glasses of water.
The most hydrating foods to prioritize
Cucumbers contain 96 percent water by weight. They are the hydration champion of the produce section. Slice them into salads, dip them in hummus, or just eat them plain with a little salt. The salt actually helps here because it replaces the sodium you are losing through natriuresis.
Watermelon is 92 percent water. Strawberries come in at 91 percent. Cantaloupe at 90 percent. Oranges at 87 percent. These fruits provide water, natural sugars for energy, and potassium for electrolyte balance. On a tirzepatide diet plan, incorporating these fruits as snacks helps address multiple needs simultaneously.
Soups and broths deserve special attention. A cup of chicken broth provides roughly 200 mL of fluid along with sodium, potassium, and amino acids. If your appetite is severely suppressed and eating solid food feels impossible, broth-based soups can deliver hydration, electrolytes, and some nutrition in a format that many tirzepatide users tolerate well. Finding GLP-1 dinner ideas that center around soups and stews is a smart strategy during periods of heightened side effects.
Yogurt is 85 percent water and also provides probiotics that may help with GI side effects. Combining it with hydrating fruits creates a simple, well-tolerated meal. For breakfast ideas that prioritize hydration, explore GLP-1 breakfast ideas that feature smoothie bowls, overnight oats with fruit, and yogurt parfaits.
Foods that worsen dehydration
Some foods pull water from your body rather than contributing to hydration. Highly processed snacks with excessive sodium cause temporary water retention followed by increased urinary output. Sugary foods trigger osmotic effects that can worsen GI symptoms. Alcohol is a potent dehydrator that compounds every mechanism of tirzepatide-related thirst. Review the full list of foods to avoid on tirzepatide for a comprehensive guide. If you choose to drink, understanding the best alcohol choices on tirzepatide can help minimize additional dehydration.
Protein-heavy meals without adequate water can also increase dehydration. Protein metabolism produces urea, which requires water for kidney excretion. If you are prioritizing protein intake to preserve muscle mass during weight loss, and you should be, increase your water intake proportionally. A general guideline: add 30 to 50 mL of water for every 10 grams of protein consumed above your baseline. Following guidance on what to eat on tirzepatide helps you balance macronutrients with hydration needs.
Electrolyte balance: the missing piece of the thirst puzzle
Drinking more water without addressing electrolytes is like filling a leaky bucket. You can keep pouring, but if sodium and potassium are leaking out through natriuresis and GI losses, the water will not stay where your body needs it.
Why electrolytes matter more on tirzepatide
Electrolytes, specifically sodium, potassium, and magnesium, control how water distributes between cells, blood, and extracellular fluid. When tirzepatide increases sodium excretion through the kidneys, it creates an electrolyte imbalance that plain water cannot fix. In fact, drinking large amounts of plain water when your sodium is already low can make the imbalance worse by diluting what remains.
This is why some tirzepatide users report that they drink and drink and drink but still feel thirsty. Their thirst is not for water. It is for electrolytes. Their body is sending a "drink" signal because it does not have a separate signal for "you need salt." The body can only say "thirsty." It cannot say "your sodium is low, please eat something salty and then drink water."
Sodium: the primary electrolyte concern
Tirzepatide-induced natriuresis primarily affects sodium. The recommended daily sodium intake for most adults is 1,500 to 2,300 mg, but on tirzepatide, some users may need to be at the higher end of this range to compensate for urinary losses. This is one of the rare situations where adding a pinch of salt to your water can actually help. Not enough to taste salty. Just a small pinch, about 200 to 400 mg of sodium, per liter of water.
But be careful.
If you have hypertension or heart failure, increasing sodium intake requires guidance from your prescriber. The benefit of replacing lost sodium must be weighed against the risks of sodium on blood pressure.
Potassium: the overlooked partner
Potassium works in partnership with sodium to maintain fluid balance. GI losses from diarrhea and vomiting can deplete potassium rapidly. Low potassium causes fatigue, muscle cramps, weakness, and, yes, increased thirst. Foods rich in potassium include bananas, avocados, sweet potatoes, spinach, and coconut water. If you are experiencing muscle pain on tirzepatide or joint pain, potassium depletion could be a contributing factor alongside dehydration. Consider a B12 supplement alongside tirzepatide as well, since nutrient absorption can be affected by reduced food intake.
Magnesium: the sleep and muscle connection
Magnesium losses through GI effects can contribute to a cluster of symptoms that includes thirst, muscle cramps, poor sleep, and anxiety. If you are dealing with tirzepatide anxiety alongside thirst, magnesium supplementation may address both. Magnesium glycinate is generally well tolerated and does not worsen GI symptoms. Magnesium citrate can worsen diarrhea in some users, so choose the form carefully. A comprehensive approach to supplements on tirzepatide should address all three of these electrolytes. Some users also benefit from glycine supplementation with tirzepatide, which supports sleep quality that dehydration may be disrupting.
Practical electrolyte strategy
Option one: use a commercial electrolyte supplement designed for active hydration, like LMNT, Liquid IV, or Drip Drop. Take one serving per day, preferably in the morning or after exercise.
Option two: make your own. Mix 1/4 teaspoon of salt, a squeeze of lemon juice, and a small splash of fruit juice into 500 mL of water. This approximates the electrolyte balance of commercial products at a fraction of the cost.
Option three: prioritize electrolyte-rich foods. Bone broth for sodium. Bananas and avocados for potassium. Nuts and dark leafy greens for magnesium. This approach works best for people who tolerate solid food well on tirzepatide.
Review the best fiber supplements for GLP-1 users as part of your overall supplementation plan, since fiber also plays a role in GI symptom management. And probiotics for GLP-1 users can help reduce the diarrhea that depletes electrolytes in the first place.
How thirst changes during dose escalation
Tirzepatide uses a gradual dose escalation protocol. You start at 2.5 mg and can increase every 4 weeks through 5, 7.5, 10, 12.5, and up to 15 mg. Each step up brings a potential resurgence of side effects, including thirst. Understanding this pattern helps you prepare rather than react.
At 2.5 mg: the introduction phase
Most users experience mild to moderate side effects at the starting dose. Thirst at this level is typically subtle, a slight increase in how much water you want throughout the day. GI effects are usually manageable. This is your baseline adaptation period. Your body is meeting GLP-1 and GIP receptor activation for the first time. Use this phase to establish your hydration routine before it becomes critical at higher doses. Learning the tirzepatide dosage in units helps you understand exactly how much medication you are receiving and correlate it with your symptoms.
At 5 mg: the first real test
The jump from 2.5 to 5 mg is a doubling of dose. Many users report a noticeable increase in side effects at this level, including thirst. GI symptoms that had resolved on 2.5 mg may return. This is often the dose where users first need to implement deliberate hydration strategies rather than relying on thirst-driven drinking. Check the tirzepatide dose chart to understand the progression and plan accordingly.
At 7.5 mg through 10 mg: peak adjustment
Many users find that 7.5 to 10 mg is where side effects, including thirst, hit their peak. The GLP-1 receptor activation at these doses is substantial, and both GI effects and natriuresis increase proportionally. If you are going to experience significant thirst on tirzepatide, it will likely emerge or worsen during this dose range.
This is also where the weight loss timeline typically accelerates, meaning your body composition is changing, your fluid requirements are shifting, and your nutritional needs are evolving all at the same time. Paying attention to hydration during this phase is not optional. It is essential.
At 12.5 mg through 15 mg: adaptation or escalation
By the time you reach these higher doses, one of two things has happened. Either your body has adapted to GLP-1 receptor activation and side effects have diminished significantly, or you are still experiencing considerable effects that need management. For most users, thirst at higher doses is less intense than it was during the middle dose range, not because the medication effect is weaker but because the body has adapted. Those who continue experiencing severe thirst at 12.5 or 15 mg should discuss this with their prescriber, as it may indicate electrolyte imbalances or other issues worth investigating.
Some users explore microdosing tirzepatide or following a microdose schedule to minimize side effects while maintaining efficacy. Others find that splitting their tirzepatide dose twice a week reduces the peak side effect intensity, including thirst, by creating more even medication levels. Whether you choose to take tirzepatide every 5 days or stick with the standard weekly schedule, hydration management remains the same priority.
When to call your healthcare provider about thirst
Most thirst on tirzepatide resolves with better hydration and electrolyte management. But certain situations require professional medical evaluation.
Red flags that demand immediate attention
Call your provider right away if you experience any of the following. Thirst that persists despite drinking more than 4 liters of water daily. Urine output that has dropped significantly or stopped. Confusion, disorientation, or difficulty concentrating. Muscle weakness that is not explained by normal post-exercise fatigue. Heart palpitations or irregular heartbeat. Swelling in your hands, feet, or ankles that is new. Seizures or tremors of any kind. Severe, intractable vomiting that prevents you from keeping fluids down for more than 12 hours.
These symptoms could indicate severe dehydration, dangerous electrolyte imbalances, or rare complications like SIADH that need blood work and medical intervention.
Yellow flags worth discussing at your next appointment
These are not emergencies but deserve conversation with your prescriber. Thirst that has not improved after 4 weeks on a stable dose. Dry mouth that interferes with speaking, eating, or sleeping. Frequent nighttime urination that disrupts sleep. Persistent headaches that correlate with your injection schedule. Fatigue that worsens despite adequate sleep and nutrition. If you are dealing with body aches on tirzepatide alongside thirst, the combination may point to electrolyte depletion worth investigating through blood work.
Your prescriber can check a basic metabolic panel, including sodium, potassium, kidney function markers, and blood glucose, to ensure everything is within normal ranges. If your electrolytes are off, targeted supplementation or a dose adjustment may help. Understanding the tirzepatide dosing for weight loss in units helps you have an informed conversation with your provider about whether a dose adjustment might be appropriate.
The role of other medications
Tirzepatide does not exist in isolation. If you take diuretics for blood pressure, they compound the fluid and electrolyte losses from tirzepatide natriuresis. If you take metformin, GI side effects can overlap and worsen dehydration. If you take lithium, the fluid shifts from tirzepatide can affect lithium levels. SGLT2 inhibitors cause their own osmotic diuresis that stacks on top of tirzepatide effects. Always tell your prescriber about every medication you take so they can monitor for interactions that affect fluid balance. The question of tirzepatide and testosterone also comes up frequently, and hormonal changes can independently affect fluid retention and thirst signals. Similarly, if you are considering how tirzepatide affects your period, hormonal fluid shifts during your cycle add another variable to the hydration equation.
Practical tips from people who have been through it
Beyond the science, here are strategies that real tirzepatide users report working for them.
Carry a marked water bottle. Physically seeing how much you have consumed versus your target creates accountability. A 1-liter bottle with time markers printed or taped on the side works well. Aim to finish one bottle by noon, a second by 5 PM, and a third by bedtime.
Set phone alarms. Every 60 to 90 minutes, a reminder to drink 200 mL. This sounds annoying. It works.
Eat before your injection. Having food in your stomach before injecting can reduce GI side effects, which reduces fluid losses, which reduces thirst. Experiment with taking tirzepatide at night if daytime nausea is causing you to avoid drinking.
Pre-hydrate before dose escalation. In the 2 to 3 days before stepping up your dose, deliberately increase your fluid and electrolyte intake. This builds a buffer that helps your body handle the adjustment. Check your compound dosage chart to know exactly when your next increase is scheduled.
Track your symptoms. A simple daily log of fluid intake, thirst level (1 to 10), GI symptoms, and energy level reveals patterns you would otherwise miss. You might notice that your thirst spikes 24 to 48 hours after injection, or that certain foods worsen it, or that electrolyte supplements make a meaningful difference. If you are also not losing weight on tirzepatide as expected, adequate hydration is one factor worth examining since dehydration can slow metabolism and impair fat oxidation.
Freeze fruit into ice cubes. Drop frozen strawberry or cucumber slices into your water. It adds subtle flavor, a visual cue to keep drinking, and additional micronutrients. Small changes like this make the difference between someone who hits their daily fluid target and someone who forgets.
Proper tirzepatide storage and proper injection technique do not directly affect thirst, but following best practices for medication handling ensures you get the full benefit and predictable side effect profile from each dose. Proper storage matters. Check whether tirzepatide that has gotten warm is still effective, and understand how long tirzepatide lasts in the fridge to avoid using degraded medication that could produce unpredictable effects.
How tirzepatide compares to other GLP-1 agonists for thirst
If you are wondering whether switching medications would help, here is a brief comparison. Semaglutide (Ozempic, Wegovy) activates only GLP-1 receptors, not GIP. The thirst profile is similar to tirzepatide, suggesting that GLP-1 receptor activation, not GIP, is the primary driver of thirst-related mechanisms. Some users report that semaglutide fatigue and dizziness are more pronounced, which could indicate different dehydration patterns. The bloating profile on semaglutide also differs somewhat.
For users considering a change, understanding semaglutide versus tirzepatide in detail helps make an informed decision. The conversion chart from semaglutide to tirzepatide is useful if you decide to switch, and knowing whether tirzepatide works if semaglutide did not can guide your decision. Some users also compare results with newer options like retatrutide.
If you are experiencing insomnia on semaglutide or constipation on semaglutide, switching to tirzepatide may or may not improve those specific symptoms, but the thirst issue will likely persist because the underlying GLP-1 mechanism is the same. The process of switching between the two medications should be guided by your prescriber. Understanding how long GLP-1 medications take to start working sets expectations if you do decide to make a change.
Long-term hydration habits for sustained use
If you plan to use tirzepatide long-term, and many people do for sustained weight management, building durable hydration habits matters more than any short-term fix.
Make water accessible everywhere. A bottle at your desk. A glass on your nightstand. A jug in the fridge. Environmental design beats willpower every time.
Connect drinking to existing habits. Every time you check your phone, take a sip. Every time you walk through the kitchen, drink 100 mL. Before every meal, drink a full glass. These habit stacks turn hydration into an automatic behavior rather than a conscious effort.
Monitor your urine color as a simple hydration gauge. Pale yellow means adequately hydrated. Dark yellow or amber means drink more. Clear and colorless means you might be overdoing it and should add electrolytes. This is the easiest, most accessible way to check your hydration status without any equipment or testing.
If you are working toward maintaining weight loss after tirzepatide, the hydration habits you build during treatment carry forward into maintenance. Good hydration supports metabolism, joint health, skin elasticity, cognitive function, and virtually every other body system affected by significant weight loss. Even if you eventually wean off tirzepatide, the hydration practices you developed will serve you well. Just know that if you stop tirzepatide cold turkey, the thirst and dry mouth typically resolve within 2 to 3 weeks as the medication clears your system, though some users experience withdrawal-type symptoms that temporarily affect fluid regulation.
Your overall weight loss journey on tirzepatide benefits enormously from proper hydration. Fat metabolism requires water. Muscle preservation requires water. Joint protection during increased physical activity requires water. The connection between hydration and results is direct, measurable, and often underestimated. Looking at tirzepatide before and after results, the users who maintain excellent hydration tend to report better energy, fewer side effects, and more consistent weight loss.
Special considerations for exercise and hot weather
Exercise and heat independently increase fluid requirements. When combined with tirzepatide, the total fluid demand can catch people off guard.
During moderate exercise, you lose 500 to 1,000 mL of fluid per hour through sweat. On tirzepatide, your baseline fluid needs are already elevated. Add exercise-related losses, and you can easily fall behind. Drink 200 to 300 mL of fluid every 15 to 20 minutes during exercise, not just when you feel thirsty. Remember the GLP-1 thirst paradox: your brain might not signal thirst even when your body desperately needs fluid. Understanding whether tirzepatide burns fat or just suppresses appetite can help you design an exercise program that works with the medication rather than against it. Some users who have hit a tirzepatide plateau find that improving hydration during exercise helps restart progress.
In hot weather, sweat losses increase further. The combination of heat-related sweating, tirzepatide GI effects, and renal natriuresis can create dangerous dehydration scenarios surprisingly quickly. If you exercise outdoors in summer, double your normal fluid intake on those days and prioritize electrolyte-containing beverages over plain water. If you are exploring whether tirzepatide makes you cold, know that temperature regulation changes on tirzepatide affect how your body handles both heat and cold exposure, with implications for fluid management in both directions.
Post-exercise hydration is equally important. Weigh yourself before and after exercise. Every pound lost during exercise represents approximately 470 mL of fluid that needs replacement. On tirzepatide, replace 150 percent of that amount, because you continue losing fluid through natriuresis even after you stop sweating. The GLP-1 fat loss treatment works best when your body is properly fueled and hydrated, and exercise is a key component of that equation.
Understanding injection site and hydration connections
While injection site and hydration are not directly linked in terms of mechanism, well-hydrated tissue absorbs medication more predictably than dehydrated tissue. Proper hydration supports consistent medication absorption, which in turn creates more predictable side effect profiles, including thirst patterns.
Whether you inject in your stomach, thigh, or another approved location, following proper injection technique matters. If you experience an injection site reaction, know that inflammation at the injection site can independently trigger mild fluid shifts in the surrounding tissue. Understanding how to treat injection site reactions and recognizing when a red and itchy injection site needs attention helps you manage the complete side effect picture. Explore the full guide to injection site locations for best practices. If you use compounded tirzepatide, understanding how to reconstitute tirzepatide and the proper bacteriostatic water ratios ensures accurate dosing, which helps keep side effects predictable. Understanding syringe dosage and unit conversions supports precision in your protocol.
The bigger picture: thirst as part of your overall experience
Thirst does not exist in isolation on tirzepatide. It is one piece of a larger puzzle of side effects and adaptations your body goes through. Understanding how it connects to other experiences helps you manage everything more effectively.
GLP-1 fatigue and thirst often appear together because dehydration directly causes tiredness. Fix the hydration, and the fatigue often improves. GLP-1 headaches frequently trace back to dehydration as well, making hydration the first-line treatment for multiple symptoms at once. Even sulfur burps on GLP-1 and burping on semaglutide can worsen when dehydration slows gastric emptying further.
Consider your thirst management as part of a comprehensive approach to your GLP-1 experience. Proper hydration, adequate nutrition, electrolyte balance, appropriate supplementation, and good injection practices all work together. B6 supplementation and niacinamide are two additional supplements worth exploring as part of your overall protocol. The complete guide to GLP-1 supplements covers the full range of options.
If you are interested in broader peptide topics beyond GLP-1 agonists, peptide safety and risks provides important context. The peptide dosing guide covers dosing principles across peptide types, and getting started with peptides is an excellent foundation for anyone new to the field. SeekPeptides offers comprehensive resources on peptides for fat loss and peptides for gut health, both of which intersect with GLP-1 agonist therapy.
Tools like the peptide calculator and semaglutide dosage calculator help you manage dosing with precision, which contributes to more predictable side effect profiles. Whether you want to understand how long tirzepatide takes to suppress appetite or how long semaglutide takes, these tools and guides help you track your experience systematically. Understanding how long tirzepatide takes to work overall gives you a timeline against which to measure all your side effects, including thirst. Additional resources on GLP-1 injection site reactions, how to inject GLP-1, where to inject GLP-1, and the best time to take your GLP-1 shot are all available through SeekPeptides. For those exploring alternative administration methods, GLP-1 drops may present different side effect considerations. And if autoimmune concerns are part of your health picture, microdosing GLP-1 for autoimmune conditions covers an emerging area of research. If you have been curious about whether GLP-1 is the same as Ozempic, that guide clarifies the relationship. Some users who have been asking about taking tirzepatide a day early do so when side effects taper off too quickly before their next dose, and understanding the timing can also help manage hydration patterns. Users who are dealing with unexpected weight gain on tirzepatide should consider whether water retention from electrolyte imbalances could be the cause rather than true fat gain. And for those wondering about tirzepatide and bone loss or erectile dysfunction, proper hydration supports both bone metabolism and cardiovascular function.
For women who have specific concerns, understanding whether tirzepatide is compatible with breastfeeding involves considerations about maternal hydration that relate directly to the topic of this article. And semaglutide period effects may help contextualize hormonal fluid shifts. Reading about feeling cold on semaglutide can also be informative if you are comparing your experience across GLP-1 agonists. Additional useful reads include understanding tirzepatide color to verify medication integrity, the shelf life of tirzepatide, and whether tirzepatide expires. Understanding the first week on semaglutide can help those transitioning between medications.
The semaglutide plateau phenomenon parallels the tirzepatide not working anymore experience, and in both cases, proper hydration is one factor worth examining. Resources on how fast semaglutide works, losing weight on semaglutide without exercise, the best foods on semaglutide, foods to avoid on semaglutide, and the full food list for semaglutide provide additional context.
And the before and after tirzepatide weight loss results show what well-managed treatment can achieve, including when hydration is part of the protocol. Exploring GLP-1 hair loss is also worthwhile since nutritional deficiencies from reduced intake, compounded by dehydration, can affect hair health during treatment.
Frequently asked questions
Does tirzepatide cause dehydration?
Tirzepatide does not cause dehydration directly in the way a diuretic would. However, it creates multiple conditions that increase your risk of dehydration. GI side effects like nausea, vomiting, and diarrhea cause fluid loss. Renal natriuresis increases sodium and water excretion through urine. Reduced food intake eliminates food-associated fluid. And the central GLP-1 thirst suppression can mask your body need for water. The combination of these factors means tirzepatide users need to be more intentional about hydration than they were before starting treatment. If you are feeling tired on tirzepatide, dehydration could be contributing.
How much water should I drink on tirzepatide?
Aim for 2.5 to 3.5 liters of drinking water per day for women, and 3.0 to 4.0 liters for men. These targets exceed the general population recommendations from the National Academies to account for tirzepatide-related fluid losses. Increase by an additional 500 to 1,000 mL on days with heavy exercise, hot weather, or active GI symptoms. But do not drink excessively without electrolytes, as this can dilute sodium and cause hyponatremia.
Will the thirst go away on its own?
For most users, yes. Thirst typically resolves or significantly improves within 2 to 4 weeks on a stable dose. However, it may return with each dose escalation. If your thirst has not improved after 4 weeks at the same dose, consult your healthcare provider to check for underlying electrolyte imbalances. Following a proper dosing guide and hydration strategy accelerates adaptation.
Is dry mouth on tirzepatide dangerous?
Dry mouth itself is not dangerous in the short term, but chronic dry mouth increases the risk of dental problems including cavities, gum disease, and oral infections. Saliva protects your teeth and gums. Without adequate saliva, bacteria thrive. If you experience persistent dry mouth on tirzepatide, maintain rigorous dental hygiene, chew sugar-free gum to stimulate saliva, and mention the symptom to both your prescriber and your dentist. Review the full tirzepatide dry mouth guide for comprehensive management strategies.
Can electrolytes help with tirzepatide thirst?
Absolutely. Electrolyte supplementation addresses a root cause of thirst that plain water cannot fix. When tirzepatide increases sodium excretion through the kidneys, replacing that sodium (along with potassium and magnesium lost through GI effects) helps your body retain the water you drink. A daily electrolyte supplement or electrolyte-rich foods can make a significant difference. Check the complete guide to supplements on tirzepatide for specific recommendations.
Should I drink more water on injection day?
Yes. Increase your fluid intake by approximately 500 mL on the day of your injection and the day after. This is when GI side effects are most likely to peak, and proactive hydration can reduce their severity. Choosing the best time for your injection can help you plan hydration around the peak side effect window.
Can I drink alcohol on tirzepatide if I am already thirsty?
Alcohol is a potent dehydrator that compounds every mechanism of tirzepatide-related thirst. It suppresses antidiuretic hormone, increases urinary output, worsens GI symptoms, and impairs the liver fluid regulation processes. If you are already experiencing thirst, alcohol will make it significantly worse. If you choose to drink, do so in moderation, alternate alcoholic beverages with water, and prioritize electrolyte-containing beverages before and after. Read the full guide on drinking on tirzepatide for detailed guidance.
Does the thirst get worse at higher doses?
Not necessarily. Many users find that thirst peaks during the middle dose range (7.5 to 10 mg) and then improves at higher doses as the body adapts to sustained GLP-1 receptor activation. However, each dose escalation may cause a temporary flare of symptoms, including thirst, that resolves within 2 to 4 weeks. Using microdosing strategies can help smooth out dose transitions and minimize side effect spikes.
External resources
FDA Prescribing Information for Mounjaro (Tirzepatide) - Official prescribing information including complete side effect data from clinical trials
New England Journal of Medicine SURPASS Trials - Primary clinical trial data on tirzepatide efficacy and safety
National Academies Dietary Reference Intakes for Water - Evidence-based hydration guidelines for adults
Daniels et al. GLP-1 Receptor Agonists and Water Intake Suppression (SUNY Buffalo) - Research on the hypodipsic effects of GLP-1 receptor agonists in animal models
National Kidney Foundation - Dehydration Signs and Prevention - Comprehensive resource on recognizing and preventing dehydration
SeekPeptides members gain access to detailed protocols, dosing guides, and expert resources on managing every aspect of GLP-1 therapy, from hydration strategies to supplement stacks to injection techniques. If you are navigating tirzepatide for the first time or looking to optimize your experience at any dose level, membership provides the depth of information that surface-level articles simply cannot offer. The tools, calculators, and community resources are built specifically for people who take their peptide protocols seriously.
In case I do not see you, good afternoon, good evening, and good night. May your hydration stay balanced, your side effects stay manageable, and your protocols stay effective.