Feb 28, 2026

Six weeks on semaglutide. That is when Marcus finally understood what everyone kept talking about. Not the weight loss. Not the numbers on the scale. The quiet. For the first time in twenty years, his brain stopped screaming about food at 2pm. No bargaining with himself over chips. No mental negotiations about dinner while still eating lunch. Just silence. And honestly? That silence scared him almost as much as it relieved him.
His experience is not unusual. Thousands of people starting semaglutide ask the same question before their first injection: how will this actually make me feel? The clinical trials describe side effects in sterile medical language. Nausea. Decreased appetite. Gastrointestinal disturbance. But those words do not capture what it is really like. They do not tell you about the strange sensation of forgetting to eat breakfast, or the way a slice of pizza suddenly feels like eating a full Thanksgiving dinner, or the low energy that creeps in during week two because you accidentally cut your calories in half without realizing it.
This guide covers every sensation, every shift, every weird and wonderful change that semaglutide produces in your body and mind. Not the textbook version. The real version. Week by week, dose by dose, from the first injection through month six and beyond. You will learn what the research actually shows, what experienced users consistently report, and how to tell the difference between normal adjustment and something that needs medical attention. Because knowing what to expect is half the battle.
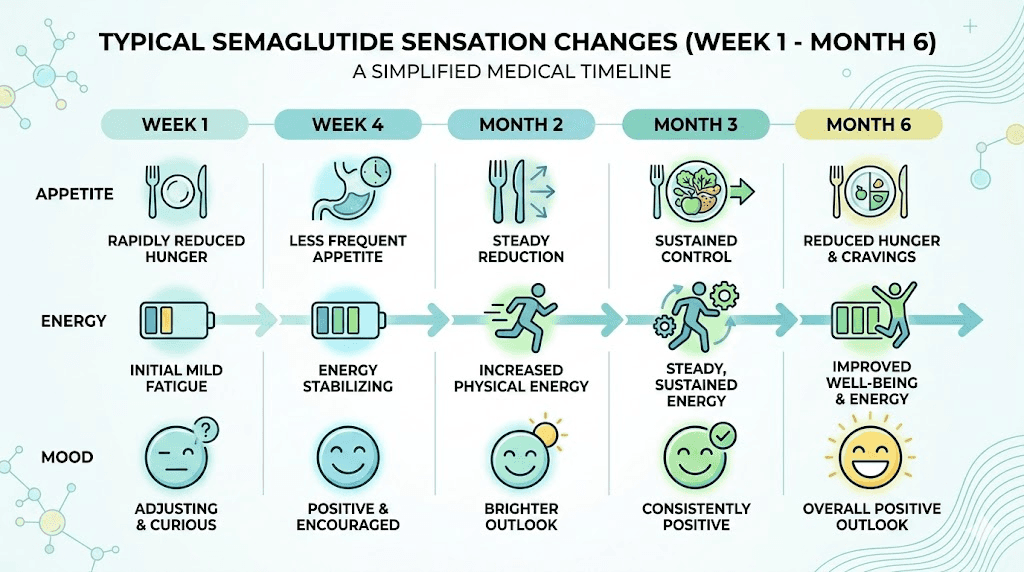
The first sensation everyone notices: food noise goes quiet
Before we get into the week-by-week breakdown, we need to talk about the single most reported experience among semaglutide users. It is not nausea. It is not weight loss. It is the disappearance of what researchers and patients call "food noise."
Food noise refers to the persistent, intrusive thoughts about food that occupy mental bandwidth throughout the day. Not hunger exactly, but a constant background hum of thinking about what you will eat next, what sounds good, whether you should snack, what is in the fridge, what you had for lunch yesterday. For many people, this mental chatter runs from the moment they wake up until they fall asleep.
Research published in PMC shows that before treatment, 62% of people reported constant food-related thoughts. After starting semaglutide, that number dropped to 16%. That is not a subtle shift. That is a fundamental rewiring of daily mental experience.
How does it work? GLP-1 receptor agonists like semaglutide cross the blood-brain barrier and act on dopamine-linked reward centers. Functional MRI scans reveal that semaglutide reduces activation in brain regions associated with food rewards while simultaneously enhancing satiety networks. In plain language, the foods that once triggered compulsive wanting simply become less interesting. Not disgusting, not repulsive. Just not particularly compelling anymore.
Users describe it differently. Some say food becomes "optional" rather than mandatory. Others describe finally being able to walk past a bakery without their brain staging a full negotiation. A few report feeling almost uncomfortable with the quiet, especially those who have spent decades using food as emotional regulation.
This happens for most people within the first one to two weeks. Sometimes sooner. And it is often the very first sign that semaglutide is working, arriving well before any visible weight loss.
Week one: what the first seven days actually feel like
The first week on semaglutide is a study in contradictions. You expect dramatic change. What you get is subtle. Then suddenly not so subtle at all.
The injection itself
Most people worry about the injection. They should not. Semaglutide is administered subcutaneously with a very thin needle, and the injection itself causes minimal discomfort. Most describe it as less painful than a mosquito bite. A small pinch. Sometimes nothing at all. Choosing the right injection site matters. The abdomen, thigh, and upper arm are standard choices, and rotating between them reduces irritation.
Hours one through twelve
Within the first twelve hours, many people notice... nothing. The starting dose of 0.25mg is intentionally low, designed to let your body adjust gradually. Some report a very mild fullness sensation, like they just finished a satisfying meal even when they have not eaten recently. Others feel completely normal.
A small percentage experience mild nausea within the first few hours. Usually gentle. More like early pregnancy queasiness than actual stomach flu. It comes and goes in waves.
Days two through four
This is when things start getting interesting. The appetite suppression, even at the low starting dose, begins to register. You sit down for lunch and realize halfway through that you are done. Not stuffed. Not nauseous. Just done. The meal that usually takes 15 minutes takes 8 because you simply stop wanting food.
Food preferences sometimes shift surprisingly fast. Research from clinical trials using the Leeds Food Preference Task found that semaglutide users showed substantially lower explicit liking for high-fat foods and decreased implicit wanting for energy-dense options. In real terms, the burger that normally sounds amazing now sounds fine but not exciting. The salad that usually feels like a punishment actually sounds appealing.
Some experience mild digestive changes during these early days. Bloating. A feeling of fullness that sits higher in the stomach than normal. Increased burping is surprisingly common, because semaglutide slows gastric emptying, meaning food sits in your stomach longer than your body is used to.
Days five through seven
By the end of week one, most people have identified their personal response pattern. Some feel almost nothing at 0.25mg. Others already notice significant appetite reduction. A few have experienced enough nausea to adjust their eating habits.
Weight loss in the first week is typically modest. One to five pounds. And most of that is water weight and reduced food volume, not fat loss. Do not judge the medication by week one results. The real changes are building beneath the surface. Your GLP-1 receptors are being primed. Your dosage will increase. And the sensations will intensify.
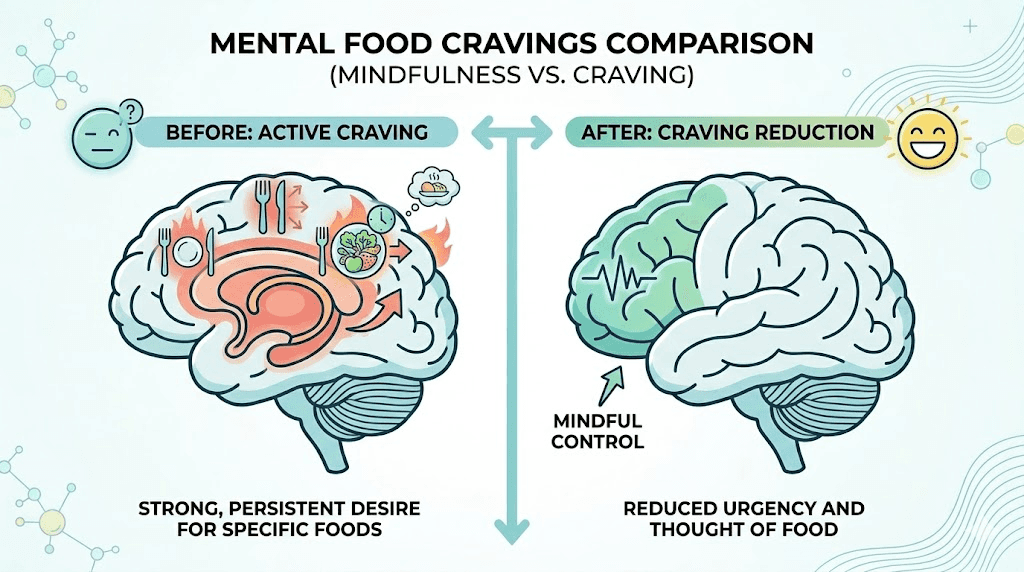
Weeks two through four: the adjustment period
This is the period that makes or breaks most people. The body is adapting to a fundamentally new hormonal signal, and it does not always go quietly.
Appetite changes intensify
The appetite suppression that felt subtle in week one becomes unmistakable by week two. Many people describe forgetting to eat entirely. Not intentionally skipping meals. Actually forgetting that eating is something humans need to do. Your alarm goes off at 7am. You get busy. Suddenly it is 1pm and you have not thought about food once.
This can feel liberating and alarming in equal measure. If you have spent years counting calories, measuring portions, fighting cravings, the sudden absence of all that mental noise is disorienting. You do not know what to do with all that freed-up bandwidth. Planning meals becomes less about restriction and more about making sure you actually eat enough.
Because here is the trap nobody warns you about. Not eating enough is a real problem on semaglutide. Your appetite drops. You eat less. You feel fine. But your body still needs protein, vitamins, minerals, and adequate calories to function. Drop too low and the fatigue hits hard.
The fatigue question
Fatigue is one of the most misunderstood side effects of semaglutide. Users blame the medication. But in most cases, the culprit is not semaglutide itself. It is the caloric deficit.
Think about it. Before semaglutide, you might have consumed 2,200 calories daily. Now, with dramatically reduced appetite, you are eating 1,200 without even trying. That is a 1,000 calorie daily deficit. Your body notices. Energy drops. Mental clarity fades in the afternoon. Workouts feel harder. Sleep might even get disrupted.
The fix is not powering through. The fix is eating deliberately. Set reminders. Prioritize protein. Nutrient-dense foods become critical because you have less total intake to work with. Every bite matters more.
Some fatigue during this period is genuinely drug-related. Semaglutide affects energy levels through multiple pathways. The slowed gastric emptying means your body processes fuel differently. Blood sugar patterns shift. Your metabolism is recalibrating. Give it time.
Nausea patterns
Nausea during weeks two through four follows a predictable pattern for most people. It tends to spike in the 24-48 hours after each weekly injection, then fade. Eating too fast makes it worse. Greasy or heavy foods make it worse. Eating past the point of comfortable fullness, which is now much lower than before, makes it significantly worse.
Clinical data shows that nausea affects roughly 20-44% of users depending on dose, but the severity matters more than the frequency. Most people describe it as mild to moderate. Manageable. Annoying but not debilitating. And critically, it tends to resolve. Research from the STEP trials found that most participants recovered from nausea episodes within a few days, though individual timelines vary.
Management strategies that consistently help include eating smaller meals more frequently, avoiding high-fat foods during the first 48 hours post-injection, staying well hydrated, using ginger tea or peppermint, and eating slowly enough that your compressed stomach has time to signal fullness before you overeat. The timing of your injection can also matter.
Digestive changes beyond nausea
Constipation is the side effect nobody wants to discuss but many experience. Semaglutide slows the entire digestive tract, not just the stomach. Food moves through your system more slowly. Less food going in combined with slower transit time means less frequent bowel movements.
Unlike nausea, constipation tends to persist longer. Data suggests it does not resolve as quickly as other GI symptoms. Fiber intake, adequate hydration, and gentle physical activity help. Some people find that magnesium supplements make a significant difference.
Bloating is also common during this adjustment phase. Your stomach is emptying more slowly, so food sits longer, creating a persistent full sensation even when you have not eaten much. This usually improves as your body adapts, but it can be uncomfortable in weeks two and three.
Mood and emotional shifts
Here is something the clinical trial data barely captures. The emotional experience of semaglutide is profound for many users. Food is not just fuel. It is comfort, celebration, stress relief, social bonding, identity. When your relationship with food changes overnight, the psychological ripple effects can be significant.
Some people feel genuinely relieved, even euphoric. After years of battling cravings, the peace is overwhelming. Others feel strangely sad, as if they lost a coping mechanism without a replacement. Some report increased anxiety in social eating situations because they can no longer participate in meals the way they used to.
Research is catching up to these reports. A study published in The Lancet observed that patients using semaglutide reported significant improvements in mood and quality of life, particularly those experiencing substantial weight loss. But other case reports document worsened depression in some individuals. The relationship between GLP-1 agonists and mental health remains an active area of investigation.
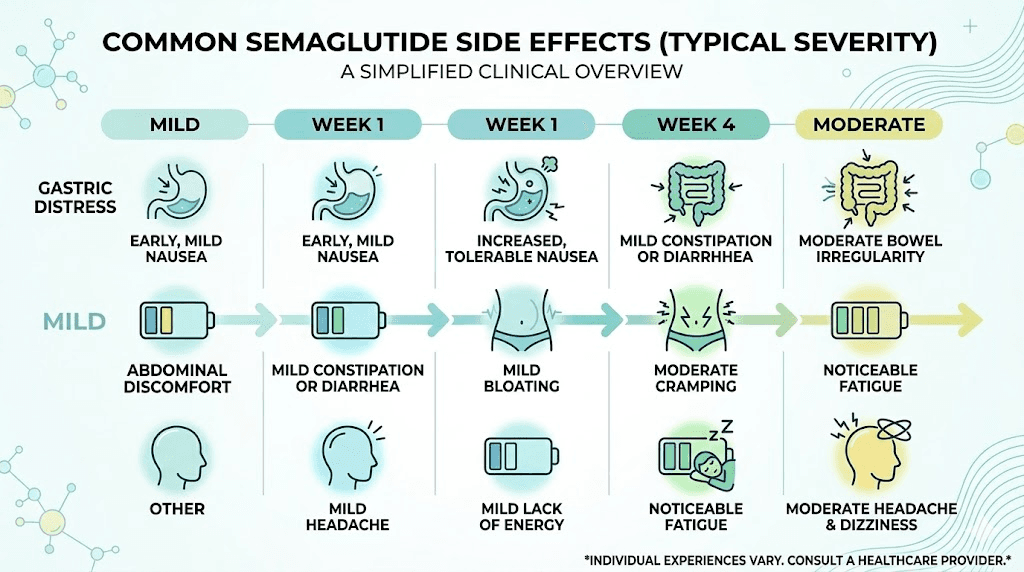
The dose escalation experience: 0.25mg to 0.5mg to 1.0mg and beyond
Semaglutide uses a gradual dose escalation protocol. You start at 0.25mg weekly for four weeks, then increase to 0.5mg for four weeks, then 1.0mg, and potentially up to 2.4mg for weight management. Each dose increase brings a new round of adaptation, and the sensations at each level are distinct.
Moving from 0.25mg to 0.5mg
This is often described as the moment semaglutide "turns on." The 0.25mg dose is essentially a warm-up. Necessary for safety. Important for tolerance building. But pharmacologically, it is doing relatively little.
At 0.5mg, the appetite suppression doubles down. People who felt moderate effects at the starting dose now feel strong ones. Meals become noticeably smaller. The food noise, if it had not already quieted completely, goes almost silent.
Nausea may return or intensify for two to three days after the first 0.5mg injection. This is normal. Your body is adjusting to a new concentration. The same management strategies apply. Eat light, avoid heavy meals, stay hydrated, and give it a few days.
One sensation people rarely expect at this dose level: temperature changes. Some users report feeling colder than usual, particularly in their extremities. This likely relates to reduced caloric intake and the body conserving energy. Keeping layers handy helps.
The 1.0mg threshold
For many people, 1.0mg is where the medication feels fully active. Appetite suppression is strong and consistent. Weight loss becomes visually noticeable, not just measurable on a scale. Energy levels, paradoxically, often improve at this stage because the body has adapted to the new eating patterns and metabolized enough fat to use as consistent fuel.
The transition to 1.0mg can bring a brief return of GI symptoms. Some people experience their worst nausea at this dose change. Others sail through. Individual variation is enormous. What matters is that each dose level gets easier with time, and the side effects that seem intense on day one of a new dose are usually manageable by day five.
A study found that semaglutide reduced ad libitum energy intake by approximately 35% at lunch and total daily intake by 24%. At the 1.0mg dose and above, these reductions become very real in daily life. You order a meal at a restaurant and eat a third of it. You buy groceries and they last twice as long. You realize that your relationship with food has fundamentally shifted.
Higher doses: 1.7mg and 2.4mg
Not everyone needs to reach 2.4mg. Some achieve their goals at lower doses. But for those who do escalate, the higher doses bring more pronounced effects across every dimension. Appetite suppression at 2.4mg is described by some as almost excessive. They have to force themselves to eat. This is where careful dosing and nutritional planning become essential.
The 12-week clinical study found that semaglutide produced a mean body weight reduction of 5.0 kg compared to a 1.0 kg gain with placebo. At higher doses over longer periods, the STEP 1 trial showed average weight loss of 9.6% of baseline body weight at three months and 13.8% at six months. Participants who maintained treatment for a full year lost approximately 15-17% of baseline weight.
Body fat loss exceeded lean mass loss by a three-fold margin in the clinical studies, which is important. The weight you lose is primarily fat, not muscle. But maintaining adequate protein intake at higher doses requires deliberate effort because your appetite makes eating enough genuinely difficult.
How semaglutide changes the way you eat
The sensations semaglutide creates around food deserve their own section because they are complex, layered, and unlike anything most people have experienced before.
Satiety arrives faster and harder
Before semaglutide, satiety is a gradual process. You eat, you feel progressively fuller, you eventually stop. On semaglutide, satiety arrives like a wall. You are eating comfortably, enjoying your food, and then suddenly you are done. Not gradually done. Done done. One more bite would feel like punishment.
This "satiety wall" catches people off guard at first. You serve yourself a normal portion. You eat half. The wall hits. The remaining food becomes genuinely unappealing. Not because you are nauseous, but because every signal in your body says stop. This is semaglutide slowing gastric emptying and amplifying the satiety hormones your gut already produces.
Learning to serve smaller portions from the start saves food waste and avoids the uncomfortable sensation of staring at a plate of food your brain will not let you finish.
Taste perception shifts
Some users report subtle changes in how food tastes. Not dramatic. Not like everything becomes bland. More like the intense pleasure response to hyper-palatable foods diminishes. The chips that used to light up your reward centers now taste like... chips. Still fine. Just not transcendent.
Research confirms that GLP-1 is expressed in taste bud cells and central gustatory pathways, providing a biological basis for sensory changes. Certain foods, particularly sweet and fatty combinations, lose their previous hold. Meanwhile, simpler foods, vegetables, lean proteins, whole grains, sometimes become more satisfying than before.
The relationship with alcohol changes
Alcohol on semaglutide deserves special attention. Many users report significantly reduced desire to drink. This goes beyond just feeling full. GLP-1 receptors in the brain overlap with reward pathways involved in alcohol consumption. Some people who previously enjoyed nightly wine find they simply do not want it anymore. Others find that alcohol hits harder because their altered digestion changes absorption patterns.
This is an area of active research. Early studies suggest GLP-1 agonists may reduce addictive behaviors broadly, not just food-related ones. But the practical implication for semaglutide users is simple: if you drink, start slow, pay attention to how it affects you differently, and do not assume your previous tolerance still applies.
Social eating becomes complicated
Nobody talks enough about this. Social situations built around food become genuinely awkward for many semaglutide users. Dinner parties where you eat a quarter of your plate. Business lunches where your colleagues eat full meals while you pick at a small salad. Holiday gatherings where turning down food invites questions and unwanted advice.
There is no pharmacological fix for this. It is a social adaptation. Most long-term users develop strategies. Ordering appetizers as mains. Eating before events so they can pick at food socially without pressure. Being honest with close friends and vague with everyone else. The reduced appetite is a feature of the medication. The social friction is an unintended side effect of living in a food-centered culture.
Energy and physical performance: the full picture
The energy story on semaglutide is not linear. It dips, recovers, and often surpasses baseline levels. Understanding the timeline prevents unnecessary panic during the rough patches.
The initial energy dip (weeks 1-4)
Most people experience reduced energy in the first month. The causes stack. Reduced caloric intake means less available fuel. The body is transitioning from running on frequent meals to running on stored fat plus smaller meals. Blood sugar patterns are shifting. Sleep may be disrupted by digestive changes.
During this phase, intense exercise feels harder. Workouts may need to be scaled back temporarily. Recovery takes longer. Mental energy in the afternoon drops. This is normal. It is temporary. And fighting through it by adding caffeine or forcing intense workouts usually makes things worse, not better.
The adaptation phase (weeks 4-8)
Between weeks four and eight, something shifts. Your body adapts to the new energy intake. Fat metabolism becomes more efficient. Blood sugar stabilizes. The initial GI side effects fade, meaning less energy is wasted on digestive distress.
Many users report a surprising uptick in energy during this phase. Not just returning to baseline, but exceeding it. They feel lighter, both physically from weight loss and mentally from the absence of food noise. Metabolic health improvements, including better blood sugar control, mean fewer energy crashes throughout the day. The spikes and valleys of a high-carb, high-sugar diet flatten into steady, sustained energy.
Research supports this. Semaglutide has been shown to provide steadier energy levels by improving metabolic health, reducing the likelihood of sugar crashes and energy dips. Your body stops running on a roller coaster and starts running on a steady supply line.
Long-term energy (months 3-6 and beyond)
By month three, most users who have maintained adequate nutrition and protein intake report energy levels equal to or better than pre-semaglutide baseline. The combination of carrying less weight, having more stable blood sugar, and experiencing improved metabolic function creates a genuinely higher energy state.
Some users report feeling the most energized they have in years. Part of this is physical. Less weight to carry means every movement requires less effort. Improved cardiovascular markers mean better oxygen delivery. Better sleep from reduced bloating and digestive discomfort means more restorative rest.
Part of it is psychological. The mental freedom from constant food thoughts creates available energy. Decision fatigue around meals disappears. The background anxiety about weight and eating evaporates. That freed-up mental energy shows up as feeling more present, more focused, more capable.
Mood, mental health, and cognitive effects
The psychological effects of semaglutide are among its most discussed and least understood dimensions. Research is still catching up to what patients report.
The positive mental effects
A pivotal study in The Lancet found that patients using semaglutide reported significant improvements in mood and quality of life. This is not surprising when you consider the cascade of positive changes: weight loss improves self-image, reduced food obsession frees mental space, metabolic improvements stabilize mood-regulating hormones, and the sense of control over eating patterns builds confidence.
Many users describe feeling more mentally clear. The constant background processing of food-related decisions consumed real cognitive resources. When that noise quiets, people notice improved focus, better concentration at work, and more present engagement in conversations. A study from Oxford found that semaglutide was safe for brain health with possible benefits for cognition and reduced nicotine dependence.
Rodent studies have consistently demonstrated that semaglutide benefits cognitive function, showing improved memory, learning, and overall mental performance. While animal studies do not directly translate to humans, they align with what many users report anecdotally, a feeling of mental sharpness that was not there before.
The complicated mental effects
Not everyone experiences psychological improvement. Some people report increased anxiety, particularly around social eating situations or the fear of regaining weight if they stop the medication. Others describe a flatness or emotional blunting, similar to the way food-related emotions have been dampened, they feel like other emotions are slightly muted too.
Case reports document worsened depression in some individuals on semaglutide. A pharmacovigilance study found significant signals for anxiety, depressed mood disorders, and suicidality with semaglutide. This does not mean semaglutide causes depression. The relationship is complex. Weight loss itself can trigger mood changes. Losing a primary coping mechanism (emotional eating) without building replacement strategies creates vulnerability. Caloric restriction can affect neurotransmitter production.
The takeaway is not to avoid semaglutide. It is to monitor mental health proactively. Track mood alongside weight. Build alternative coping strategies before they are needed. Have support systems in place. And communicate openly with healthcare providers about any emotional changes, whether positive or concerning.
Sleep changes
Sleep effects vary widely. Some people sleep better on semaglutide because reduced bloating, less acid reflux, and weight loss improve sleep quality. People with sleep apnea often notice improvement as weight decreases.
Others experience insomnia or disrupted sleep, particularly in the first few weeks. This may relate to blood sugar changes, reduced caloric intake, or digestive adjustment. Timing your injection earlier in the week (if your schedule allows) and ensuring adequate evening nutrition can help.
Physical sensations beyond the obvious
Semaglutide produces a range of physical sensations that go far beyond the headline side effects. Understanding these helps distinguish normal adaptation from something that needs medical attention.
The fullness sensation
Semaglutide creates a unique type of fullness. Not the uncomfortable stuffed feeling after overeating. More like a persistent, gentle awareness that your stomach already has enough. It sits higher in the abdomen than typical post-meal fullness. Some describe it as "wearing a light belt around your stomach all day." It is present but not painful, noticeable but not distressing.
This sensation relates to delayed gastric emptying. Food stays in your stomach longer, so the physical feeling of having food in there persists between meals. Your stomach is not actually fuller. It just empties more slowly.
Temperature sensitivity
Feeling colder than usual is a commonly reported but rarely discussed effect. Weight loss reduces insulating body fat. Reduced caloric intake means less metabolic heat production. Some users feel chilly even in warm rooms, particularly in their hands and feet.
This is not dangerous. It is uncomfortable. Layer your clothing, keep warm drinks available, and know that it improves as your body adapts to its new weight and energy balance.
Headaches
Headaches in the first two to three weeks are common. They usually relate to dehydration (you are eating less, and food provides significant hydration), blood sugar adjustment, or reduced caffeine intake (if coffee was often consumed alongside food that you are now skipping).
The fix is almost always hydration. Drink more water than you think you need. Set reminders if necessary. Many semaglutide users do not feel thirsty in the same way they used to, making intentional hydration essential.
Dizziness
Dizziness affects some users, particularly when standing quickly. This can relate to dehydration, reduced caloric intake, or blood pressure changes. Semaglutide can modestly lower blood pressure, which is generally beneficial but can cause positional dizziness in people who already have normal or low blood pressure.
Hair changes
This is a longer-term effect that catches people off guard. Hair thinning or increased shedding has been reported by some semaglutide users. This is almost certainly related to the rapid weight loss and caloric restriction rather than a direct drug effect. The medical term is telogen effluvium, where the body, under metabolic stress, shifts hair follicles into a resting phase prematurely.
Adequate protein intake (at least 60-80 grams daily) and nutritional supplementation can help mitigate this effect. Hair typically recovers once weight stabilizes and nutritional status normalizes. B12 supplementation and other nutritional support are worth discussing with your healthcare provider.
Injection site reactions
Some people develop mild reactions at the injection site, including redness, itching, or a small hard lump. These are usually mild and resolve within a few days. Rotating injection sites and ensuring proper technique minimize these reactions. Proper injection technique makes a significant difference in comfort and skin reaction.
The week-by-week feelings timeline
Here is a consolidated timeline of what most people experience. Individual responses vary, but this represents the most common pattern.
Week 1 (0.25mg)
Mild appetite reduction. Possible subtle nausea. Some digestive awareness. Food noise begins to quiet. Minimal weight change. Energy stable or slightly reduced.
Weeks 2-4 (0.25mg)
Appetite suppression becomes noticeable. Portion sizes naturally decrease. Food preferences begin shifting away from high-fat options. Some nausea around injection days. Constipation may develop. Fatigue from reduced caloric intake. One to five pounds lost, mostly water weight. Emotional adjustment to changed relationship with food begins.
Weeks 5-8 (0.5mg)
Appetite suppression strengthens significantly. Brief return of nausea possible with dose increase. Weight loss becomes measurable and potentially visible. Energy begins recovering as body adapts. Food noise minimal to absent. Digestive system stabilizing. Mood often improving. Social eating challenges emerge.
Weeks 9-12 (0.5mg to 1.0mg)
Strong, consistent appetite suppression. Another potential nausea round with 1.0mg increase. Weight loss averaging 5-10% of baseline body weight by month three. Energy often exceeds pre-treatment levels. Mental clarity improves. New routines around eating are established. Side effects generally at their mildest point so far.
Months 3-6 (1.0mg to 2.4mg)
Weight loss averaging 13.8% of baseline at six months. Appetite suppression is the new normal. Energy stable and often improved. GI side effects mostly resolved. Food relationship fundamentally different. Potential hair thinning noticed. Nutritional supplementation becomes important. Physical changes visible to others. Clothing sizes changing.
Months 6-12 (maintenance dose)
Weight loss of 15-17% of baseline at one year. Body has fully adapted. Side effects minimal. New eating patterns feel natural rather than forced. Physical performance improving with lower body weight. Risk of plateau increases. Psychological adjustment ongoing. Long-term maintenance strategies become the focus.
How semaglutide compares to other GLP-1 medications in how they feel
If you are choosing between GLP-1 options, understanding the sensation differences matters as much as the efficacy differences.
Semaglutide vs tirzepatide
Tirzepatide is a dual GIP/GLP-1 agonist, meaning it activates two receptor pathways instead of one. Users frequently report that tirzepatide produces stronger appetite suppression at equivalent therapeutic doses. The side effect profile is similar but not identical. Tirzepatide users report slightly different GI patterns, and some find one medication more tolerable than the other.
The food noise reduction appears comparable between both medications. Energy effects are similar. Weight loss outcomes tend to be slightly higher with tirzepatide in head-to-head trials, but individual response matters more than group averages.
For those who have tried semaglutide and found the side effects intolerable, switching to tirzepatide sometimes provides better tolerance, though the reverse is also true. Bodies are different. What one person finds unbearable, another barely notices.
Semaglutide vs retatrutide
Retatrutide is a triple agonist (GIP/GLP-1/glucagon) that is still in clinical trials. Early data suggests potentially stronger weight loss effects, but the sensation profile includes more pronounced appetite suppression and potentially more GI side effects during the adjustment period. Users who have tried both sometimes describe retatrutide as "semaglutide turned up to 11" in terms of appetite effects.
Injectable vs oral semaglutide
Oral semaglutide (Rybelsus) produces similar appetite and weight effects but with different GI patterns. The oral form must be taken on an empty stomach with minimal water, and nausea patterns differ because the drug is absorbed through the gut rather than injected subcutaneously. Some people who cannot tolerate the injectable form do better with oral, and vice versa. The sublingual option offers another alternative for those who prefer to avoid injections.
Managing the difficult sensations: practical strategies
Knowing what to expect is valuable. Knowing how to manage the uncomfortable parts is essential.
Nausea management protocol
The most effective nausea management follows a simple hierarchy. First, eat smaller meals more frequently. Five small meals beats three normal ones on semaglutide. Second, avoid high-fat and greasy foods, especially in the 48 hours following injection. Third, eat slowly, much more slowly than you think necessary. Your compressed stomach needs time to register fullness before you overshoot. Fourth, stay hydrated between meals rather than during them, as drinking too much fluid with food can increase that overly-full sensation.
If those strategies do not provide adequate relief, ginger in various forms (tea, supplements, chews) has strong evidence for reducing nausea. Peppermint works for some people. Glycine supplementation has been explored as a complementary approach for managing GI symptoms. Going outside for fresh air during nausea episodes is surprisingly effective, possibly because the distraction and temperature change interrupt the nausea signal.
Constipation solutions
For constipation management, fiber is the foundation. But not all fiber is equal. Soluble fiber (oats, chia seeds, beans, apples) tends to work better than insoluble fiber (wheat bran, raw vegetables) for semaglutide-related constipation. Adequate water intake, at least 64 ounces daily, makes fiber work properly. Magnesium citrate at 200-400mg daily is a gentle, effective option. Regular gentle movement, even 15-minute walks, stimulates the digestive tract.
Fighting fatigue effectively
The number one fatigue fix on semaglutide is eating enough. Track calories for a few weeks. If you are consistently below 1,200, that is almost certainly contributing to exhaustion. Prioritize protein at 60-80 grams minimum daily. Include healthy fats, they are calorie-dense, which actually helps when appetite is suppressed. B vitamin supplementation, particularly B12, supports energy production and is commonly combined with semaglutide for this reason.
Time your biggest meal (or your most protein-dense meal) around your highest energy-demand period. If you need to be sharp at work in the morning, eat a solid breakfast. If your workout is at 5pm, make sure you have a protein-rich meal by 3pm. On semaglutide, you cannot afford to eat mindlessly. Every eating decision is a strategic one.
Protecting mental health
Build emotional coping strategies BEFORE you need them. If food was your primary stress response, what replaces it? Walking? Meditation? Calling a friend? Journaling? These are not luxury questions. They are essential infrastructure for a successful semaglutide experience.
Consider working with a therapist, particularly one experienced with eating behavior and body image. The psychological shifts that semaglutide creates are real and sometimes profound. Having professional support transforms the experience from overwhelming to manageable. SeekPeptides members access community support and shared experiences that help navigate these emotional transitions with the benefit of others who understand exactly what you are going through.
What semaglutide feels like long term: the six-month perspective
The first month gets all the attention. But the long-term experience is what actually matters for outcomes.
The new normal
By month three to four, most users stop thinking of semaglutide sensations as "side effects" and start thinking of them as just how their body works now. The reduced appetite is not a side effect. It is how you eat. The smaller portions are not restriction. They are satisfaction. The absence of food noise is not weird. It is peace.
This psychological normalization is important. When semaglutide effects stop feeling like a medication and start feeling like your natural state, compliance becomes effortless. You are not fighting your body anymore. You are working with a body that finally has the right signaling.
Maintenance dose feelings
Once you reach your maintenance dose and stay there, the sensations stabilize. Nausea is gone. Digestive function has adapted. Energy is steady. Appetite is consistent. The only ongoing sensation most long-term users report is the persistent, gentle feeling of satiety that makes overeating almost impossible and undereating a real risk if they are not paying attention.
Some users describe occasional "breakthrough hunger," where the appetite suppression temporarily weakens. This can happen around stress, hormonal cycles, sleep deprivation, or illness. It is normal. It does not mean the medication stopped working. It means your body is human and complex and sometimes overrides pharmaceutical signals with biological imperatives.
What happens when you miss a dose
Missing a dose provides an inadvertent experiment in what semaglutide was actually doing. Most people who miss a weekly injection notice increased hunger within two to three days. Food noise returns. Portion sizes creep up. The mental chatter about food resumes. It is not a full return to pre-treatment baseline in a single missed dose, but it is enough to confirm that the medication was producing real, ongoing effects.
For those concerned about withdrawal, semaglutide does not produce classical withdrawal symptoms. There is no physical dependence. But the return of suppressed appetite and food preoccupation can feel psychologically jarring after months of quiet. This is one reason that treatment duration and discontinuation planning matter.
Who tends to feel the most and least on semaglutide
Individual variation is enormous. But patterns exist.
Factors that increase sensation intensity
Lower body weight generally means stronger effects at the same dose. Women tend to report more intense GI side effects than men, possibly related to body composition and hormonal interactions. People with existing GI sensitivity (IBS, GERD, gastritis) often experience amplified digestive symptoms. Rapid dose escalation increases side effects compared to standard protocols. Dehydration amplifies almost every negative sensation.
Factors that reduce sensation intensity
Higher body weight may require higher doses to achieve the same subjective effect. People with robust metabolic health sometimes adapt faster. Prior GLP-1 experience (from other medications) can reduce the adjustment period. Good baseline nutrition and hydration habits buffer against the worst side effects. Consistent dosing schedule maintenance matters more than people think.
Realistic expectations by body type and history
If you have 20 pounds to lose, your experience will differ from someone with 100 pounds to lose. The person with more weight to lose often tolerates the medication better (fewer GI side effects relative to dose) and sees faster absolute weight loss, but the proportional experience of appetite change is similar. Both groups report the same food noise reduction. Both describe the same satiety wall. The difference is mainly in side effect intensity and weight loss velocity.
If you have a history of eating disorders, the appetite suppression can trigger complicated emotions and potentially dangerous restriction patterns. This does not mean semaglutide is contraindicated, but it means extra monitoring and support are essential. SeekPeptides provides resources for navigating these complex interactions, with evidence-based guides and experienced community support.
When sensations indicate a problem
Most semaglutide sensations are normal adjustment. Some are not. Knowing the difference matters.
Normal sensations (no action needed beyond management)
Mild to moderate nausea that resolves within days. Reduced appetite and smaller portions. Occasional constipation or loose stools. Mild fatigue in the first month. Feeling colder than usual. Occasional headaches. Food preference changes. Mild injection site redness.
Sensations that warrant contacting a healthcare provider
Severe, persistent nausea or vomiting that prevents keeping any food down. Severe abdominal pain, especially in the upper abdomen radiating to the back (could indicate pancreatitis). Persistent diarrhea lasting more than a week. Signs of kidney issues, including reduced urination, dark urine, or flank pain. Yellowing of skin or eyes (possible gallbladder issues). Severe, persistent dizziness or lightheadedness. Vision changes. Significant depression or suicidal thoughts.
Serious but rare effects to monitor
Pancreatitis, gallbladder disease, and kidney damage are documented serious side effects. They are uncommon but real. Persistent severe abdominal pain should never be ignored. Gastroparesis (stomach paralysis) and intestinal blockage have been reported in post-marketing surveillance. These are rare but require immediate medical attention if symptoms suggest them.
The FDA adverse event reporting system has logged GI adverse events including gastroparesis, intestinal obstruction, and pancreatitis. Context matters. Millions of people use semaglutide. Serious events are statistically uncommon. But awareness allows early detection, and early detection dramatically improves outcomes.
Optimizing how you feel on semaglutide
The difference between a miserable semaglutide experience and a positive one often comes down to preparation and management, not luck.
Nutrition optimization
When appetite is suppressed, every calorie matters more. Prioritize protein above everything else. Aim for at least 1 gram per pound of lean body mass. This protects muscle, supports energy, and reduces hair loss risk. Choose nutrient-dense foods over empty calories. A 1,200-calorie day of processed food leaves you depleted. A 1,200-calorie day of lean proteins, vegetables, healthy fats, and complex carbs keeps you running.
Meal planning becomes a strategic advantage on semaglutide. Without planning, you end up eating whatever is convenient in the brief moments you feel like eating. With planning, every eating window delivers maximum nutrition. Prepare protein-rich snacks in advance. Keep nutrient-dense options accessible. Treat eating like a scheduled task rather than an impulse-driven activity.
Hydration strategy
Hydration is arguably the single most impactful variable you control. Adequate water intake reduces nausea, prevents headaches, combats constipation, supports energy, and protects kidney function. The problem is that semaglutide often reduces thirst signals alongside hunger signals. You may not feel thirsty even when you need water.
Set specific hydration targets. At least 64 ounces daily, more if you exercise or live in a warm climate. Use a marked water bottle to track intake. Drink between meals rather than during them to avoid exacerbating fullness. Electrolyte supplementation can help, particularly if you are eating significantly less and therefore getting fewer dietary electrolytes.
Exercise adaptation
Do not try to maintain your pre-semaglutide exercise intensity during the first month. Your body is running on significantly less fuel. Forced intense exercise on top of dramatic caloric reduction leads to burnout, injury, and excessive fatigue. Scale back intensity by 20-30% for the first four weeks. Focus on low-impact activities like walking, swimming, or yoga. Gentle movement supports digestion without overtaxing a system that is already adapting to major changes.
After the adaptation period, gradually increase intensity. Many users find that exercise feels better than before because they are carrying less weight and have more stable energy. Resistance training becomes especially important for preserving lean mass during weight loss. The combination of adequate protein and regular resistance training is the best defense against losing muscle alongside fat.
Supplementation considerations
When food intake drops by 30-50%, micronutrient intake drops proportionally. Consider supplementing with a quality multivitamin, B12 (particularly important, as semaglutide may affect absorption), vitamin D, magnesium (helps with constipation and energy), and omega-3 fatty acids. L-carnitine is another supplement some users find helpful for energy support during the caloric restriction phase.
Some formulations combine semaglutide with glycine and B12 specifically to address common nutritional gaps and support the body during weight loss. Talk with a healthcare provider about which supplements make sense for your situation.
Semaglutide sensations with specific health conditions
Pre-existing conditions change the semaglutide experience in predictable ways.
Type 2 diabetes
Semaglutide was originally developed for diabetes management. People with type 2 diabetes often report more dramatic blood sugar stabilization as an early sensation. The rollercoaster of highs and lows flattens. This alone produces significant improvements in energy, mood, and cognitive function. However, hypoglycemia risk exists, particularly for those taking other diabetes medications. Monitoring blood work closely during the transition is essential.
PCOS and hormonal conditions
Menstrual changes on semaglutide are reported by some women. Weight loss can affect hormone levels, potentially improving or disrupting menstrual regularity depending on the individual. Women with PCOS sometimes report improved symptoms as insulin resistance decreases with weight loss and semaglutide treatment.
Thyroid conditions
Semaglutide carries a boxed warning regarding thyroid C-cell tumors based on animal studies. People with thyroid conditions, including Hashimoto thyroiditis, need careful monitoring. The weight loss and metabolic changes from semaglutide can also affect thyroid medication dosing requirements, so regular thyroid function testing during treatment is important.
Autoimmune conditions
Emerging research on GLP-1 agonists and autoimmune conditions is intriguing. Some users with autoimmune conditions report reduced inflammation markers and improved symptoms, possibly related to GLP-1 anti-inflammatory effects. However, the relationship is complex, and individual responses vary significantly.
The emotional truth about how semaglutide makes you feel
Beyond the pharmacology and the clinical data, there is an emotional dimension that deserves honest discussion.
Many people feel grateful. After years of fighting their bodies, of trying every diet, of feeling broken because willpower alone was not enough, semaglutide provides relief. It feels like the playing field finally leveled. The shame around food and weight begins to lift. And that emotional weight loss is often as significant as the physical kind.
Some people feel conflicted. They worry about dependence on a medication. They wonder if this is "cheating." They question whether the weight loss "counts" because it is medication-assisted. These feelings are common, understandable, and ultimately unfounded. Nobody questions using glasses for vision or insulin for diabetes. Semaglutide corrects a biological imbalance in appetite signaling. That is not cheating. That is medicine.
Others feel loss. Food was joy, comfort, celebration, connection. When semaglutide dampens the reward response to food, some of those emotional associations fade too. Holiday meals feel different. Date nights at restaurants feel different. The relationship with food that was once too intense is now sometimes too quiet. Finding new sources of pleasure, celebration, and comfort becomes part of the journey.
And some people feel fear. Fear that the weight will return if they stop. Fear that this is temporary. Fear of the unknown long-term effects. These fears are rational. Weight regain after stopping GLP-1 agonists is documented. Long-term data is still being collected. Acknowledging these fears is healthier than pretending they do not exist.
For those navigating these emotional complexities, SeekPeptides offers comprehensive guides and a community of researchers who share their real experiences openly. Having access to evidence-based information and people who have walked the same path transforms an isolating experience into a supported one.
Frequently asked questions
How quickly will I feel something after my first semaglutide injection?
Most people notice mild appetite changes within the first 24-72 hours. Some feel subtle appetite suppression within hours, while others take a full week to notice changes. The starting dose (0.25mg) is intentionally low, so dramatic effects should not be expected immediately.
Is nausea on semaglutide constant or does it come and go?
Nausea typically comes and goes in waves. It peaks in the 24-48 hours following injection and fades throughout the week. It is usually worse after eating too much, too fast, or consuming fatty foods. Most people find nausea resolves within the first few weeks at each dose level.
Will semaglutide make me feel tired all the time?
Fatigue is common in the first month but usually relates to reduced caloric intake rather than a direct drug effect. Ensuring adequate protein, calories, and hydration typically resolves the tiredness. Most users report improved energy after the initial adaptation period.
Does semaglutide change how food tastes?
Some users report subtle taste changes. Food does not taste bad, but high-fat, high-sugar foods lose some of their previous appeal. Research shows GLP-1 receptors exist in taste bud cells, providing a biological basis for these changes. Simpler, whole foods often become more satisfying.
Can semaglutide affect my mood or mental health?
Research shows mixed results. Many users report improved mood from weight loss, reduced anxiety, and increased confidence. However, some case reports document mood changes in both directions. Monitor your mental health and communicate any concerning changes to your healthcare provider.
What does the food noise reduction actually feel like?
Users describe it as the difference between a noisy restaurant and a quiet library. Constant thoughts about food, cravings, and mental negotiations about eating simply quiet down. Many describe it as the most significant change, arriving before any weight loss is visible.
How does the fullness sensation on semaglutide differ from normal fullness?
Semaglutide fullness is often described as a gentle, persistent awareness of satiety that lasts throughout the day. It arrives faster during meals, sometimes abruptly, and sits higher in the abdomen than typical post-meal fullness. It is the result of delayed gastric emptying slowing food processing.
Will I feel the same way on semaglutide a year from now as I do in the first month?
No. The first month is the most intense adjustment period. Side effects generally diminish while appetite suppression and positive effects stabilize. By months three to four, most users describe semaglutide effects as feeling like their natural state rather than a medication side effect.
External resources
In case I do not see you, good afternoon, good evening, and good night. May your appetite stay balanced, your energy stay steady, and your journey with semaglutide stay informed.