Feb 12, 2026

Before you eat another meal on tirzepatide, read this. Because the wrong food choices are not just slowing your results. They are making your side effects worse, wasting the peptide working inside your body, and turning what should be a smooth protocol into a daily battle with nausea, bloating, and frustration.
Most guides about tirzepatide and diet focus on what to eat. That is useful information. But knowing what to avoid matters just as much, if not more, because a single bad meal can trigger hours of gastrointestinal distress that derails your entire day. And here is the part nobody talks about: tirzepatide fundamentally changes how your digestive system processes food. The mechanism of action slows gastric emptying, alters appetite signaling, and shifts your relationship with food in ways that make certain previously harmless foods suddenly problematic.
This guide covers every food category you should limit or eliminate while on tirzepatide therapy. We will go deep into the science behind why these foods cause problems, provide specific alternatives for each category, and give you practical strategies for navigating real-world eating situations. Whether you are on your first dose or months into your protocol, understanding these dietary landmines will make the difference between suffering through side effects and sailing through your weight loss journey with minimal disruption.
How tirzepatide changes your digestion
Understanding why certain foods become problematic on tirzepatide requires understanding what the peptide actually does to your digestive system. This is not just academic knowledge. It is the foundation for every food decision you will make on this protocol.
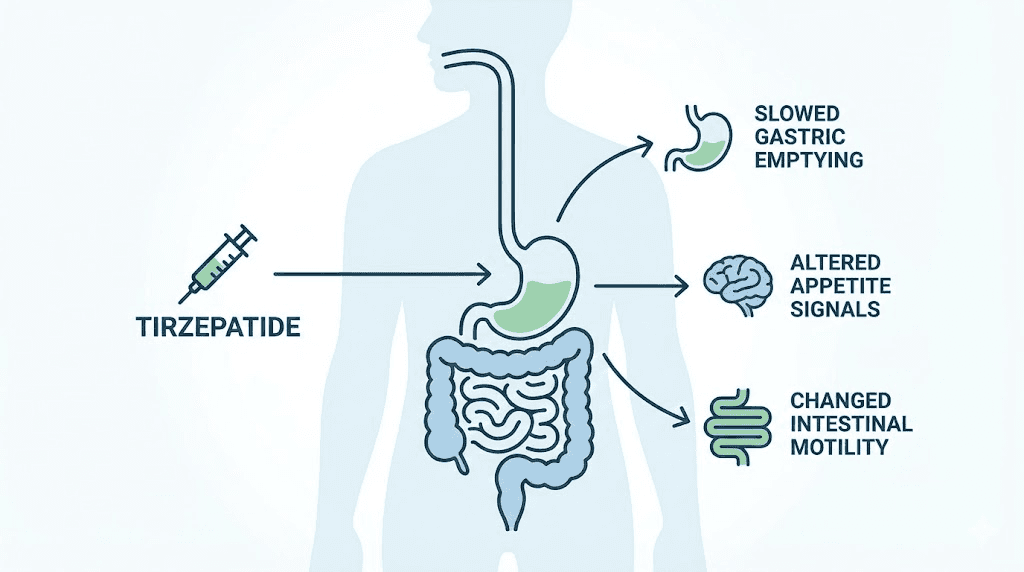
Tirzepatide is a dual GIP/GLP-1 receptor agonist. That means it activates two different incretin pathways simultaneously, which is why it produces more significant weight loss results than single-receptor medications. But those same mechanisms create specific digestive changes that interact with your food choices in predictable ways.
Gastric emptying slows dramatically
The most significant change is delayed gastric emptying. Under normal circumstances, your stomach empties its contents into the small intestine within two to four hours after eating. Tirzepatide extends this timeline substantially, particularly during the first few weeks of treatment and after each dose escalation.
Research published in the Journal of Clinical Endocrinology and Metabolism found that GLP-1 receptor agonists and tirzepatide delay gastric emptying in a dose-dependent manner, with the most pronounced effects occurring after the initial dose. This delay serves a purpose. It reduces postprandial glucose spikes and limits triglyceride absorption. But it also means food sits in your stomach longer than your body is accustomed to.
Think about that for a moment. If your stomach already takes longer to process a meal, and you eat foods that independently slow gastric emptying, like high-fat meals, you are compounding the delay. Food that would normally clear your stomach in three hours might sit there for six or more. That is where the nausea, bloating, and discomfort come from.
Appetite signals shift
Tirzepatide works on the hypothalamus to suppress appetite through central nervous system pathways. This means your hunger cues change. Foods you previously craved may suddenly seem unappealing. Portion sizes that felt normal before now feel massive. And your body sends fullness signals much earlier in a meal than it used to.
This is actually a benefit. But it creates a trap. When you do eat, you have a smaller window of comfortable intake. Fill that window with the wrong foods and you will feel terrible for hours. Fill it with the right foods and you barely notice you are on medication at all.
Intestinal motility changes
Beyond the stomach, tirzepatide affects how quickly food moves through your entire digestive tract. Some people experience constipation because the colon absorbs more water from slower-moving contents. Others experience diarrhea because the altered motility disrupts normal water absorption patterns. The side effect profile varies significantly between individuals, but food choices play a major role in which direction your system tips.
Fried and high-fat foods: the number one trigger
If there is one food category that causes the most problems on tirzepatide, it is fried and high-fat foods. Not close. Not debatable. This is the biggest dietary landmine you will face.
Here is why. Dietary fat is the macronutrient that most significantly delays gastric emptying under normal physiological conditions. Your stomach already takes longer to process fat than protein or carbohydrates. Now add tirzepatide, which independently slows gastric emptying. You are stacking two delays on top of each other.
The result? Prolonged nausea lasting several hours. Early satiety that prevents you from getting adequate nutrition. Gastroesophageal reflux symptoms. Abdominal cramping, bloating, and sometimes vomiting.
Specific fried foods to eliminate
French fries and onion rings sit heavy in the stomach for hours. Fried chicken, even when you remove the skin, retains oil throughout the meat that your slowed digestive system struggles to process. Donuts combine fried dough with sugar, creating a double trigger. Fish and chips, corn dogs, fried mozzarella sticks, tempura, and deep-fried anything should move to the "not right now" list for the duration of your tirzepatide protocol.
This does not mean you can never eat these foods again. It means that while tirzepatide is actively affecting your digestion, these foods will cause disproportionate discomfort compared to their nutritional value.
High-fat cuts of meat
Ribeye steak. Pork belly. Lamb chops with visible fat. Dark meat poultry with the skin on. Bacon. Sausage. Salami and other processed meats high in saturated fat. These all slow digestion and can trigger the same cascade of GI symptoms.
The alternative is simple. Choose lean proteins instead. Chicken breast, turkey, lean cuts of beef like sirloin or tenderloin, white fish, shrimp, and egg whites all provide excellent protein without the fat load that causes problems. Protein is actually the most important macronutrient on tirzepatide because it helps preserve muscle mass during weight loss. Research shows that people on tirzepatide should aim for 1.2 to 1.6 grams of protein per kilogram of ideal body weight daily, distributed as 25 to 40 grams per meal.
Full-fat dairy products
Whole milk, heavy cream, regular cheese, ice cream, and cream-based sauces all fall into this category. Full-fat dairy delivers a concentrated dose of saturated fat that compounds the gastric emptying delay. Additionally, tirzepatide can temporarily affect lactose digestion, making some people experience symptoms of lactose intolerance that they never had before.
Switch to low-fat or nonfat dairy options. Greek yogurt (nonfat or low-fat) is particularly good because it provides substantial protein. Skim milk, reduced-fat cheese in moderate amounts, and cottage cheese are all better tolerated. If dairy in general causes problems, plant-based alternatives like almond milk, oat milk, or soy-based products can work well.
Rich desserts and pastries
Cheesecake. Croissants. Cream puffs. Pie with buttery crust. These combine high fat with refined carbohydrates and sugar, creating a triple threat for your already-sensitive digestive system. Even a small portion can trigger significant discomfort that lasts for hours. If you want something sweet, fresh fruit, a small portion of dark chocolate, or angel food cake (which is virtually fat-free) are much safer options that will not leave you regretting the choice two hours later.
Refined carbohydrates and sugar: the blood sugar saboteurs
Tirzepatide works partly by improving your body response to insulin and managing blood sugar levels. Eating foods high in refined carbohydrates and sugar directly works against this mechanism. You are essentially fighting the medication with your fork.
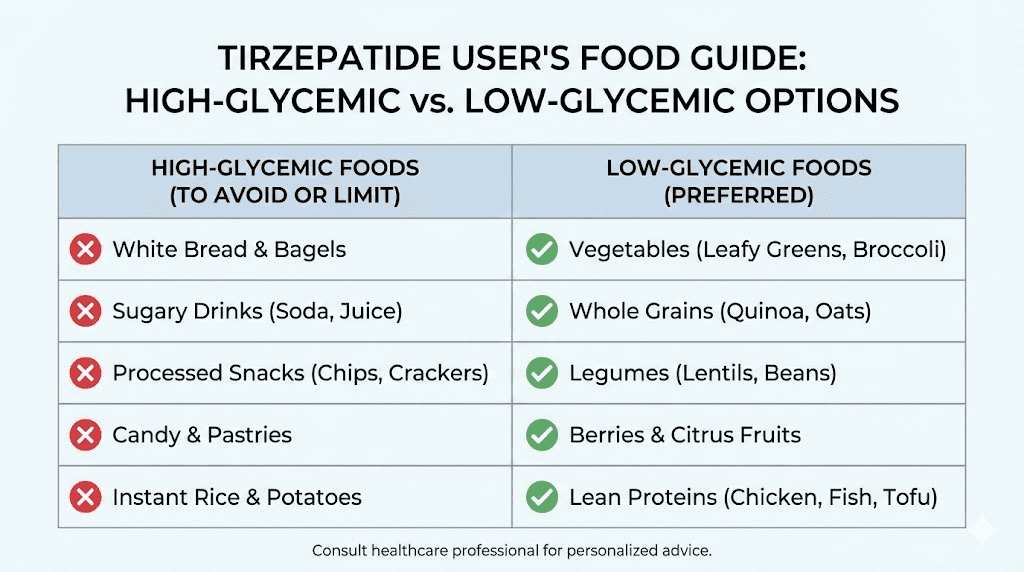
White bread, pasta, and refined grains
White bread, regular pasta, white rice, and products made with refined flour convert rapidly into glucose after digestion. This creates blood sugar spikes that tirzepatide is actively trying to prevent. The spikes trigger insulin surges, followed by crashes that leave you feeling tired, hungry, and reaching for more refined carbs. It becomes a cycle that undermines your weight loss progress.
Whole grain alternatives are significantly better tolerated and more effective alongside tirzepatide. Brown rice, quinoa, whole wheat bread, oats, and sweet potatoes provide complex carbohydrates that break down slowly, maintaining stable blood sugar levels that complement rather than fight the medication mechanism.
Sugary beverages
Soda, fruit juice, sweetened tea, energy drinks, and any drink with added sugar deliver a concentrated sugar hit with zero fiber to slow absorption. A single 12-ounce can of regular soda contains roughly 39 grams of sugar. That enters your bloodstream rapidly, causing the exact glucose spike tirzepatide is working to prevent.
Water should be your primary beverage. Unsweetened tea and black coffee (in moderation, more on caffeine later) are also fine. If you need flavor, try infusing water with cucumber, mint, or citrus slices. Sparkling water, however, falls into a separate problem category that we will address shortly.
Candy, cookies, and processed sweets
Candy bars, cookies, cake, brownies, gummy bears, and similar processed sweets are among the worst choices on tirzepatide. They combine high sugar with refined flour and often significant fat content. The sugar causes blood sugar instability. The fat slows digestion. The refined flour adds empty calories with minimal nutritional value.
But there is a nuance here that most guides miss. Sugar cravings typically diminish significantly on tirzepatide. The appetite suppression affects not just hunger but also cravings for highly palatable foods. Many people report that sweets they previously could not resist suddenly seem uninteresting. Use this biological advantage. Do not fight the reduced craving by forcing yourself to eat sweets out of habit.
High-glycemic fruits in excess
This is where it gets nuanced. Fruit is healthy. Nobody should avoid fruit entirely. But certain high-glycemic fruits like bananas, pineapple, grapes, and watermelon can cause blood sugar fluctuations when consumed in large quantities. The key word is "excess." A medium banana as part of a balanced meal is fine. Eating three bananas as a snack on an empty stomach is problematic.
Lower-glycemic fruits like berries, apples, pears, and citrus fruits are better choices. They provide vitamins, minerals, and fiber without the sharp blood sugar impact. And fiber, as we will discuss, is actually your friend on tirzepatide when consumed in appropriate amounts.
Spicy foods: the gastric lining aggravator
Spicy foods and tirzepatide are a difficult combination. Not impossible. But difficult, especially during the first few months.
Here is the mechanism. Capsaicin, the compound that makes peppers hot, irritates the gastric lining. Under normal circumstances, your stomach handles this irritation without major issues because food moves through at a normal pace. The exposure is temporary. But when tirzepatide slows gastric emptying, spicy food sits against your stomach lining for an extended period. The irritation compounds over time.
The result is often worsened nausea, heartburn, acid reflux, and abdominal pain that lasts much longer than it would without the medication. Research notes that hot peppers, curry dishes, and heavily spiced foods may be poorly tolerated, particularly when food remains in the stomach for extended periods.
Which spicy foods cause the most problems
The worst offenders combine spice with fat. Think buffalo wings (fried plus spicy), creamy curry dishes (high fat plus spice), spicy sausage (fatty meat plus spice), and nachos loaded with jalapenos and cheese. These create a compounding effect where multiple triggers hit simultaneously.
Pure spice without fat is somewhat better tolerated. A grilled chicken breast with hot sauce causes less trouble than fried chicken with hot sauce. But during dose escalation periods, when your dosage is increasing and GI side effects are most pronounced, even moderate spice can be problematic.
How to reintroduce spice gradually
Most people can tolerate some spice once their body adjusts to tirzepatide, typically after four to eight weeks at a stable dose. Start with mild seasonings like paprika, ginger, and garlic. Move to moderate heat like mild salsa or a small amount of hot sauce. If tolerated well, gradually increase the heat level.
Pay attention to timing. Spicy foods are better tolerated earlier in the day when your stomach has not yet accumulated a full day of slower-emptying meals. A mildly spicy lunch is generally safer than a spicy dinner, which would sit in your stomach while you try to sleep.
Carbonated beverages: the hidden discomfort trigger
This one surprises people. Sparkling water seems healthy. Diet soda seems like a reasonable alternative to regular soda. But carbonated beverages of any kind can cause significant discomfort on tirzepatide.
The reason is straightforward. Carbonation introduces gas into your stomach. Under normal conditions, your stomach processes and releases this gas relatively quickly. But with delayed gastric emptying, that gas has nowhere to go. It builds up, causing bloating, pressure, discomfort, and often triggering nausea in people who are already prone to it on tirzepatide.
All carbonated drinks count
Regular soda. Diet soda. Sparkling water. Seltzer. Beer. Champagne. Energy drinks with carbonation. Kombucha. All of them introduce the same carbon dioxide gas that causes problems when stomach emptying is delayed.
The solution is simple. Switch to still water, herbal tea, or other non-carbonated beverages. If you are someone who relies on sparkling water for hydration, this adjustment might feel significant. But most people find that after a few days of flat water, the discomfort reduction from eliminating carbonation far outweighs the taste preference.
The beer problem
Beer deserves special mention because it combines carbonation with alcohol, creating a double problem. The carbonation causes bloating and gas buildup. The alcohol interacts with tirzepatide in ways we will cover in the next section. If you are going to have an occasional drink, a small glass of wine or a measured spirit with a non-carbonated mixer is a much better choice than beer.
Alcohol: the dangerous interaction most people underestimate
Alcohol while on tirzepatide is not just about comfort. It is about safety.
There is no official contraindication listed on the tirzepatide label that prohibits alcohol entirely. But the interaction between the two creates risks that go well beyond a worse hangover. If you are following a tirzepatide protocol, understanding these risks is essential.
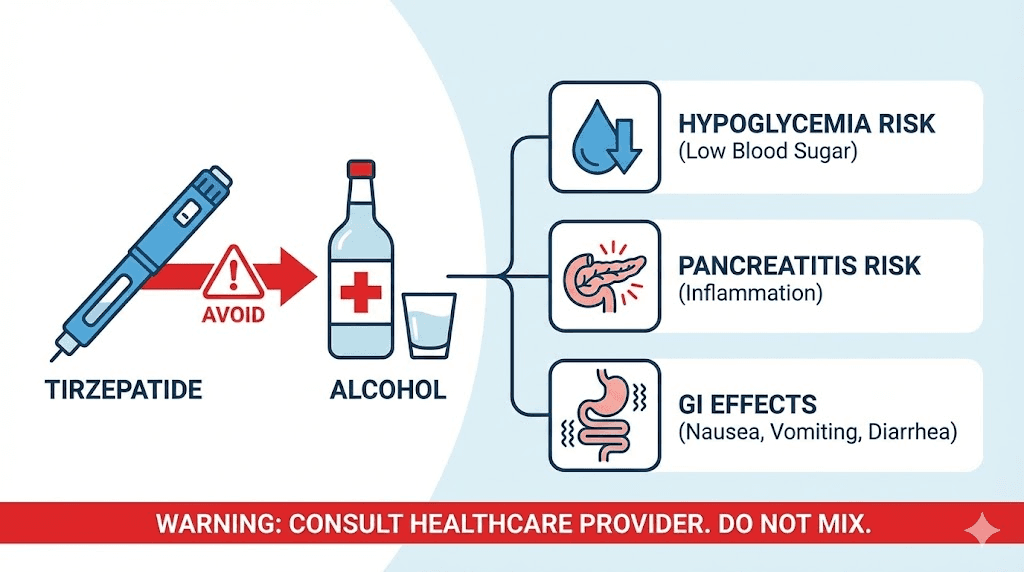
Hypoglycemia risk
This is the most dangerous interaction. Alcohol prevents your liver from releasing emergency glucose stores when blood sugar drops. Tirzepatide, by its mechanism of action, can lower blood sugar. Combine the two and you create a scenario where blood sugar can drop to dangerously low levels with your body unable to mount its normal corrective response.
This risk is even higher if you are also taking insulin or sulfonylureas alongside tirzepatide. The combination of alcohol, tirzepatide, and other glucose-lowering medications can cause severe hypoglycemia that requires medical attention.
Symptoms of hypoglycemia include shakiness, sweating, confusion, rapid heartbeat, irritability, and in severe cases, loss of consciousness. And here is the troubling part: alcohol can mask these symptoms. You might attribute the shakiness and confusion to being tipsy when your blood sugar is actually dropping to dangerous levels.
Pancreatitis risk amplification
Both alcohol and tirzepatide independently carry a small risk of pancreatitis. Research shows that combining them may amplify this risk. Pancreatitis is a serious medical condition involving inflammation of the pancreas that can require hospitalization. The risk is not enormous for moderate, occasional drinkers, but it is real and increases with heavier consumption.
Intensified GI side effects
Alcohol irritates the stomach lining and alters gut motility independently of tirzepatide. When you add alcohol on top of the GI changes tirzepatide already causes, the combination frequently produces more severe nausea, vomiting, and diarrhea than either would cause alone. Many people on tirzepatide report that their alcohol tolerance drops significantly. One drink might feel like three used to feel.
If you choose to drink occasionally
Complete abstinence from alcohol is the safest choice on tirzepatide. But if you choose to drink occasionally, here are evidence-based guidelines to minimize risk:
Always eat food containing both carbohydrates and protein before drinking. Never drink on an empty stomach. Limit consumption to one drink for women and two for men, maximum. Choose wine or spirits with non-carbonated mixers over beer or champagne. Monitor blood sugar before drinking, periodically during consumption, before bed, and the following morning, as hypoglycemia risk persists for up to 24 hours after alcohol consumption.
If you have been following a protocol detailed in our guide to alcohol and GLP-1 medications, similar principles apply to tirzepatide. The interaction mechanism is nearly identical.
Caffeine and coffee: the complicated relationship
Coffee and tirzepatide do not have a direct pharmacological interaction. No drug-drug conflict exists between caffeine and tirzepatide. But that does not mean coffee is problem-free on this protocol.
Caffeine increases gastric acid secretion. It can relax the lower esophageal sphincter, allowing stomach acid to reflux into the esophagus. It stimulates intestinal motility. All of these effects, layered on top of tirzepatide gastrointestinal changes, can amplify nausea, acid reflux, and diarrhea in sensitive individuals.
How to handle coffee on tirzepatide
Limit daily intake to one to two cups of plain black coffee, especially during dose escalation periods. Never drink coffee on an empty stomach while on tirzepatide. Consuming it with or immediately after a meal containing protein significantly reduces gastric irritation. Avoid coffee within three hours of taking your tirzepatide injection if possible, as the combined gastric effects peak during this window.
If you experience persistent nausea or acid reflux that correlates with coffee consumption, try switching to tea (lower caffeine, less gastric acid stimulation) or decaffeinated coffee for a few weeks to see if symptoms improve. Many people find that their coffee tolerance normalizes after their body adjusts to each dose level, which typically takes four to six weeks.
What about energy drinks
Energy drinks combine caffeine, carbonation, sugar (or artificial sweeteners), and often other stimulant compounds. This creates a quadruple problem on tirzepatide. The caffeine irritates the stomach. The carbonation causes bloating. The sugar spikes blood glucose. And compounds like taurine and guarana add additional gastrointestinal stimulation. Energy drinks should be at the top of your "avoid" list, not just limited.
Sugar alcohols and artificial sweeteners: the stealth disruptors
This is the food category that flies under the radar. Most people do not even know sugar alcohols are causing their problems.
Sugar alcohols include sorbitol, mannitol, xylitol, erythritol, maltitol, and isomalt. They are found in sugar-free gum, mints, diet candies, protein bars marketed as low-carb, sugar-free ice cream, and many "keto-friendly" processed foods. These compounds are incompletely absorbed in the small intestine, which means they reach the large intestine where gut bacteria ferment them, producing gas, bloating, and osmotic diarrhea.
Under normal digestive conditions, small amounts of sugar alcohols cause minimal symptoms. But tirzepatide altered gut motility changes the equation. The slower transit time means more fermentation, more gas production, and more discomfort.
Specific products to watch for
Sugar-free gum is one of the most common culprits. Many people chew gum to manage dry mouth or occupy their appetite on tirzepatide, not realizing the sorbitol or xylitol is causing their bloating and diarrhea. Diet candies, sugar-free chocolates, certain protein bars (check the label for sugar alcohols), and "no sugar added" ice creams frequently contain maltitol, one of the worst offenders for GI symptoms.
Read labels carefully. If a product contains any of these sugar alcohols and you are experiencing digestive issues on tirzepatide, eliminating them for a week is a simple diagnostic test. Many people are surprised at how much better they feel once these stealth disruptors are removed.
What about stevia and monk fruit
Stevia and monk fruit extract are not sugar alcohols. They are natural high-intensity sweeteners that are generally well tolerated on tirzepatide because they do not undergo the same fermentation process in the large intestine. If you need a sweetener, these are better options. However, some products marketed as stevia-sweetened also contain erythritol or other sugar alcohols as bulking agents, so always check the full ingredients list.
Gas-producing vegetables: navigating fiber carefully
This category requires nuance. Vegetables are essential on tirzepatide. They provide vitamins, minerals, and fiber that support healthy weight loss and prevent nutritional deficiencies. You should absolutely eat vegetables. But certain vegetables produce significant gas during digestion, and that gas combined with delayed gastric emptying creates problematic bloating.
Cruciferous vegetables
Broccoli, cauliflower, cabbage, Brussels sprouts, kale, and bok choy contain raffinose, a complex sugar that the human body lacks the enzyme to fully digest. Bacteria in the large intestine ferment raffinose, producing gas. On tirzepatide, this gas production is amplified by the slower digestive transit, and the gas gets trapped longer, causing more significant bloating and discomfort.
This does not mean you should eliminate cruciferous vegetables entirely. They are among the most nutritious foods available. Instead, cook them thoroughly (cooking breaks down some of the problematic fibers), eat smaller portions spread across meals rather than large amounts at once, and introduce them gradually if you were not eating them regularly before starting tirzepatide.
Legumes and beans
Beans, lentils, chickpeas, and other legumes are excellent sources of plant protein and fiber. They are also notorious gas producers due to their high content of oligosaccharides, specifically galactooligosaccharides. On tirzepatide, the bloating from legumes can be more pronounced and longer-lasting than usual.
If you want to include legumes in your diet (and they are worth including for their protein and fiber content), try these strategies: soak dried beans overnight and discard the soaking water before cooking (this reduces oligosaccharide content by 25-50%), start with small portions and increase gradually, choose lower-gas legumes like lentils and canned chickpeas over dried beans, and consider using a digestive enzyme supplement containing alpha-galactosidase when eating legumes.
How much fiber is right on tirzepatide
Fiber is important on tirzepatide. It helps prevent constipation, feeds beneficial gut bacteria, and supports steady blood sugar levels. But too much fiber too quickly can worsen bloating and gas, especially when digestive motility is already altered.
Start with 20 to 25 grams of daily fiber and gradually increase to 25 to 30 grams as your body adjusts. Prioritize soluble fiber sources like oats, psyllium husk, apples, and sweet potatoes, which are generally better tolerated than insoluble fiber sources like wheat bran and raw vegetables. And critically, increase water intake alongside fiber increases. Fiber without adequate water can actually worsen constipation rather than relieve it.
For those experiencing constipation on tirzepatide (which affects approximately 12-16% of users according to clinical trial data), fiber is part of the solution, not the problem. But it needs to be introduced thoughtfully. Our guide on peptide safety covers additional strategies for managing common side effects.

Large meals: the portion problem
This is not about a specific food. It is about quantity. And it might be the most impactful change you can make.
Large meals are fundamentally incompatible with tirzepatide digestive changes. Your stomach empties slower. Your appetite signals come earlier. Your capacity is reduced. Eating a large meal forces your already-strained digestive system to process a volume of food it is no longer equipped to handle efficiently.
The three-meal-a-day trap
Many people on tirzepatide try to maintain their pre-medication eating pattern of three large meals per day. This almost always leads to problems. A large breakfast sits heavy all morning. A large lunch compounds on top of the slowly-digesting breakfast. And a large dinner leads to nighttime nausea, reflux, and poor sleep.
The solution is shifting to five to six smaller meals or three small meals with two to three snacks. Each eating occasion should contain 20 to 30 grams of protein, a moderate portion of complex carbohydrates, and a small amount of healthy fat. The total calories may be the same as three larger meals, but the distribution across the day matches your altered digestive capacity much better.
Eating speed matters
Eating too fast overwhelms your stomach before your brain receives the "I am full" signal. On tirzepatide, this signal comes faster than it used to, but if you eat quickly, you can still overshoot. Clinical guidance recommends consuming meals over 20 to 30 minutes with thorough chewing. Put utensils down between bites. This simple habit prevents the overeating that triggers most meal-related nausea episodes.
Timing your last meal
Avoid eating within two to three hours of lying down. With delayed gastric emptying, food is still actively sitting in your stomach when you lie down, which increases reflux and nausea. Many people on tirzepatide find that their worst side effects occur at night simply because their dinner has not finished digesting by bedtime. Moving your last meal or snack earlier in the evening is one of the highest-impact changes you can make.
Processed and ultra-processed foods: the hidden sabotage
Ultra-processed foods represent a particularly problematic category on tirzepatide because they typically combine multiple trigger factors in a single product.
A frozen pizza, for example, combines refined carbohydrates (white flour crust), high fat (cheese and processed meats), high sodium (which can cause water retention and bloating), and often additives that independently affect digestion. A bag of chips combines refined carbohydrates with fat and sodium. Fast food burgers combine all of the above with a large portion size.
Why ultra-processed foods are particularly bad on tirzepatide
Beyond the individual trigger factors, ultra-processed foods are engineered to be hyperpalatable. They are designed to override your body natural satiety signals and make you eat more than you need. Tirzepatide is actively working to reduce your appetite and improve your satiety response. Ultra-processed foods directly fight this mechanism.
Studies consistently show that people consume more calories when eating ultra-processed foods compared to whole foods, even when the macronutrient profiles are identical. On tirzepatide, this battle between the medication and the food engineering often results in eating past comfort, followed by hours of digestive misery.
Common ultra-processed foods to minimize
Frozen dinners and TV meals. Fast food from drive-throughs. Packaged snacks (chips, crackers, snack cakes). Processed meats (hot dogs, deli meat with additives, processed sausage). Instant noodles. Microwave popcorn. Flavored yogurt with high sugar content. Breakfast cereals with added sugar. Granola bars with more candy than granola.
Replacing these with whole-food alternatives does not have to be complicated. A baked chicken breast takes 25 minutes and provides clean protein. Steamed vegetables with a squeeze of lemon take 10 minutes. Brown rice cooks while you do other things. A simple meal of whole foods almost always works better on tirzepatide than anything that comes in a brightly colored package with a long ingredient list.
High-sodium foods: the bloating amplifier
Sodium does not directly interact with tirzepatide. But high-sodium foods cause water retention, which amplifies the bloating that many tirzepatide users already experience from delayed gastric emptying. The combined effect can make you feel uncomfortably distended and puffy, even when you have not overeaten.
Hidden sodium sources
The obvious high-sodium foods are chips, pretzels, and heavily salted snacks. But the bigger culprits are often hidden. Canned soups frequently contain 800-1200mg of sodium per serving. Restaurant meals average 50-100% more sodium than home-cooked equivalents. Bread and bread products are among the largest sodium sources in the American diet, not because each slice is extremely salty but because people eat bread frequently.
Soy sauce, teriyaki sauce, many salad dressings, pickled foods, processed cheese, and deli meats all contribute significant sodium. Research suggests that foods with over 600mg of sodium per serving may exacerbate gastrointestinal distress during the first four to eight weeks of tirzepatide treatment.
Sodium guidelines on tirzepatide
Aim to keep total daily sodium intake under 2,300mg, which aligns with general dietary guidelines. Cook more meals at home where you control the salt content. Use herbs, spices (mild ones, given the spice discussion above), lemon juice, and vinegar to add flavor without sodium. When eating out, request sauces and dressings on the side and ask for low-sodium preparation when available.
What to eat instead: building your tirzepatide-friendly plate
Knowing what to avoid is only half the equation. Building meals that support your tirzepatide protocol is just as important. Here is a framework for creating meals that work with the medication rather than against it.
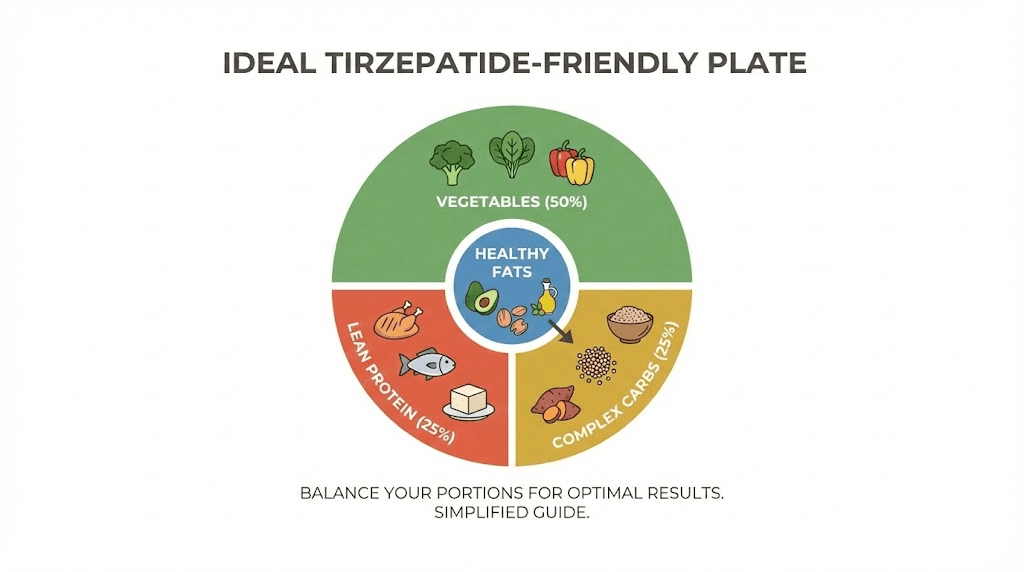
The ideal tirzepatide plate composition
Fill roughly half your plate with non-starchy vegetables. Cooked, not raw, if you are experiencing significant GI symptoms. A quarter of the plate should be lean protein. And the remaining quarter should be complex carbohydrates. Add a small amount of healthy fat from sources like olive oil, avocado (in moderation), or a small handful of nuts.
This composition provides adequate nutrition within a smaller volume that your altered digestive system can handle comfortably. It prioritizes protein (critical for maintaining muscle mass during weight loss), provides fiber from vegetables and complex carbs, and limits but does not eliminate fat.
Best proteins on tirzepatide
Grilled or baked chicken breast. Turkey breast. White fish like cod, tilapia, and halibut. Shrimp and other shellfish. Egg whites (whole eggs in moderation). Tofu and tempeh. Lean ground turkey or chicken. Greek yogurt (nonfat or low-fat). Cottage cheese. These all provide high protein per calorie with minimal fat, making them easy on your digestive system while supporting muscle preservation.
Best carbohydrates on tirzepatide
Oatmeal (not the instant flavored kind, which has added sugar). Sweet potatoes. Brown rice. Quinoa. Whole grain bread in moderate amounts. Berries. Apples. Lentils in small portions. These provide sustained energy and fiber without the blood sugar spikes that refined carbohydrates cause.
Best fats on tirzepatide
Fat is not eliminated on tirzepatide. It is moderated. Choose sources that provide maximum nutritional benefit per gram of fat. Extra virgin olive oil (1-2 tablespoons for cooking or dressing). A quarter of an avocado. A small handful of almonds, walnuts, or pistachios. Flaxseeds or chia seeds added to oatmeal or yogurt. These provide essential fatty acids and fat-soluble vitamin absorption without the heavy digestive load of fried foods or fatty meats.
Meal timing and hydration strategies
What you eat matters enormously. But when you eat and how you hydrate can be equally important for managing side effects and maximizing results.
Hydration: the underrated factor
Tirzepatide can suppress thirst signals alongside appetite. Many people on the medication become mildly dehydrated without realizing it because they simply do not feel thirsty. Dehydration worsens constipation, concentrates stomach acid (worsening nausea), and can cause headaches and fatigue that get attributed to the medication when they are actually caused by insufficient water intake.
Aim for eight to ten glasses of water per day. Do not wait until you feel thirsty. Set reminders if necessary. And here is an important nuance: drink water between meals, not during meals. Large volumes of fluid during meals can fill your already-limited stomach capacity and worsen feelings of fullness and nausea. Sipping small amounts with meals is fine, but keep your main hydration between eating occasions.
Meal timing around injection day
Most tirzepatide users find that GI side effects are most pronounced in the 24 to 48 hours following their weekly injection. Planning lighter, simpler meals during this window can significantly reduce discomfort. For injection day and the following day, stick to the most easily digestible options: clear soups, plain grilled chicken, steamed rice, cooked vegetables, and small portions.
As the week progresses and the peak side effects subside, you can gradually incorporate a wider variety of foods. Some people find that by days five through seven after injection, they can tolerate foods that would cause problems on days one and two. Keeping a food diary helps identify your personal pattern.
The food and symptom diary approach
Clinical guidance recommends maintaining a food and symptom diary during the first few months of tirzepatide treatment. Track what you eat, when you eat it, and how you feel afterward. Patterns emerge quickly. You might discover that dairy causes you problems but moderate spice does not. Or that small amounts of fried food are tolerable at lunch but not at dinner. These personal insights are more valuable than any general guide (including this one) because digestion is highly individual.
Week-by-week adaptation: what to expect
Your tolerance for different foods will change over time on tirzepatide. Understanding this timeline helps you make better decisions and avoid unnecessary dietary restrictions that your body has actually moved past.
Weeks 1-4: the adjustment period
This is when side effects are most pronounced and dietary restrictions matter most. During these early weeks, stick strictly to the guidelines above. Eat small, frequent meals. Avoid all major trigger categories. Stay hydrated. Focus on lean proteins, cooked vegetables, and simple carbohydrates. This is not permanent. This is getting through the initial adaptation.
Many people make the mistake of judging tirzepatide by how they feel during this period. The nausea, the bloating, the dietary restrictions, it feels overwhelming. But it is temporary for most people. The medication timeline shows that side effects typically peak during the first two to four weeks and then gradually diminish.
Weeks 5-8: cautious expansion
As your body adapts to the current dose, you can begin cautiously reintroducing foods. Start with one category at a time. Try a small amount of moderately spiced food. If tolerated, try it again a few days later to confirm. Then try a moderate-fat meal. Then a small serving of cruciferous vegetables. Introduce one variable at a time so you can identify what your body specifically tolerates and what it does not.
If you are escalating your dose during this period, expect a temporary return of heightened sensitivity with each increase. The adaptation process partially resets with dose changes.
Weeks 9 and beyond: personalized approach
By this point, most people have developed a clear understanding of their personal food tolerances on tirzepatide. Some people find they can eat almost anything in moderate portions. Others have a few specific trigger foods that consistently cause problems regardless of timing or quantity. Your food diary data from the first two months guides your long-term eating patterns.
The tachyphylaxis effect also plays a role here. Research shows that tirzepatide effect on gastric emptying diminishes somewhat with continued use. This means your digestive system partially normalizes over time, and foods that were completely off-limits in week one may be manageable (in moderation) by month three or four.
Specific meal situations and how to navigate them
Restaurant dining on tirzepatide
Restaurants present unique challenges because you do not control the cooking method, portion sizes, or ingredient quality. But with some strategies, you can dine out successfully on tirzepatide.
Choose grilled, baked, or steamed preparations over fried. Ask for sauces and dressings on the side. Order appetizer portions instead of entrees, or plan to take half home before you start eating. Avoid the bread basket entirely, not because bread is terrible but because it fills your limited stomach capacity with refined carbohydrates before your protein and vegetables arrive. And do not feel pressured to clean your plate. On tirzepatide, leaving food is not waste. It is wisdom.
Social eating and gatherings
Holiday meals, parties, barbecues, and potlucks are challenging because the food options are typically heavy on exactly the categories to avoid: fried appetizers, rich main courses, sugary desserts, and alcohol. The best strategy is eating a small, tirzepatide-friendly meal before the event so you are not hungry when you arrive. Then you can selectively sample foods without the pressure of needing to eat a full meal from the available options.
Travel eating
Traveling while on tirzepatide requires planning. Airport food is predominantly fast food, processed snacks, and heavy restaurant meals. Pack protein-rich snacks like jerky (low-sodium versions), individually wrapped cheese sticks, nuts in measured portions, and whole fruit. These travel well, do not need refrigeration for short trips, and provide reliable nutrition without the GI triggers that airport and gas station food would cause.
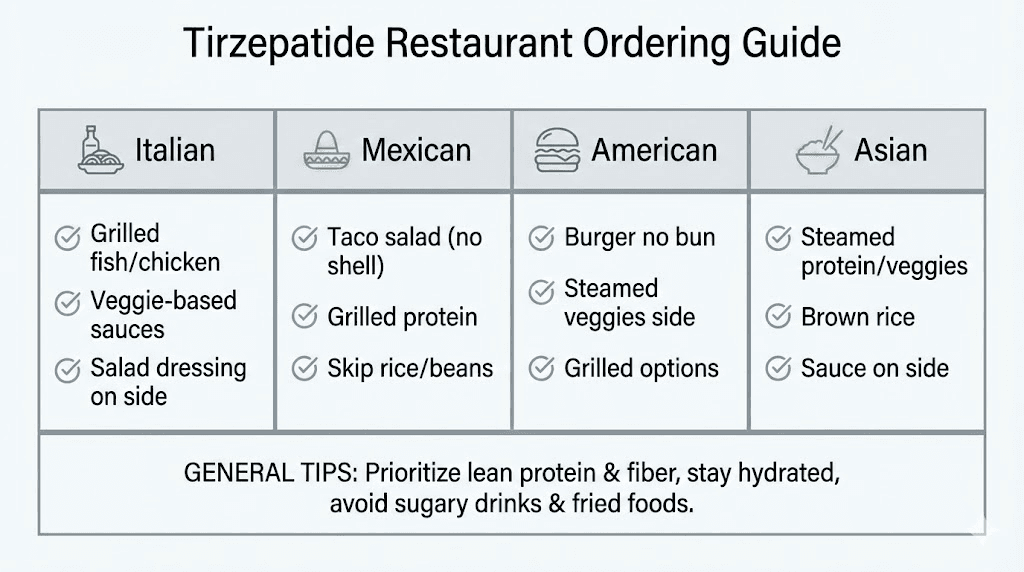
For longer trips, identify restaurants at your destination that offer grilled proteins and vegetables. Most cuisines have tirzepatide-friendly options once you know what to look for. Japanese (sashimi, grilled fish, edamame), Mediterranean (grilled meats, salads, hummus in small amounts), and many Thai dishes (steamed options, clear soups) work well.
The protein priority: why this deserves special attention
Every food discussion on tirzepatide needs to address protein specifically because inadequate protein intake during GLP-1 mediated weight loss has serious consequences.
Research on tirzepatide and body composition shows that approximately 75% of weight lost is fat mass and 25% is lean mass. That 25% lean mass loss represents muscle, which is metabolically active tissue that burns calories at rest. Losing excessive muscle slows your metabolism, making weight regain more likely after stopping the medication and reducing physical function and strength.
The primary defense against muscle loss is adequate protein intake combined with resistance training. Clinical guidance recommends 1.2 to 1.6 grams of protein per kilogram of ideal body weight daily. For a person with an ideal body weight of 70kg, that translates to 84-112 grams of protein per day, distributed as 25-40 grams per meal.
The challenge: eating enough protein with reduced appetite
Here is the catch. Tirzepatide reduces appetite. You eat less overall. If you fill your reduced food intake with carbohydrates and fat instead of prioritizing protein, you risk inadequate protein consumption even while eating "enough" total calories. This is why protein needs to be the foundation of every meal and snack on tirzepatide.
Practical protein strategies: eat protein first at every meal before vegetables and carbohydrates. Use protein shakes or smoothies (with low-fat protein powder) as snacks if solid food is hard to tolerate. Keep pre-cooked chicken, hard-boiled eggs, and cottage cheese readily available for quick, high-protein options when appetite is low.
For those tracking their progress on tirzepatide, monitoring protein intake is arguably more important than monitoring total calories. The scale will go down regardless thanks to the medication appetite effects. But whether that weight loss preserves your muscle depends heavily on protein prioritization.
Common mistakes people make with food on tirzepatide
After analyzing thousands of tirzepatide user experiences, certain patterns emerge. These are the most common dietary mistakes people make on this protocol.
Mistake 1: eating nothing when nauseous
When nausea hits, the instinct is to stop eating entirely. This is counterproductive. An empty stomach on tirzepatide often makes nausea worse because stomach acid with no food to work on irritates the lining. Small, bland bites, even just a few crackers or a piece of plain toast, often reduce nausea more effectively than fasting through it.
Mistake 2: overcompensating with "healthy" foods
Someone starts tirzepatide and decides to eat "perfectly healthy" by loading up on raw vegetables, beans, nuts, and whole grains all at once. Each of these foods is individually healthy. Together, all at once, on a system with delayed gastric emptying? Massive bloating, gas, and discomfort. Healthy foods need to be introduced gradually just like anything else.
Mistake 3: drinking calories instead of eating them
Some people switch to smoothies and shakes exclusively because solid food feels uncomfortable. While an occasional protein shake is fine, replacing all meals with liquid calories often leads to blood sugar instability (liquid calories absorb faster) and inadequate satiety (chewing and the act of eating contribute to feeling satisfied). A balance of solid food and occasional liquid supplements works better than all-liquid approaches.
Mistake 4: being too restrictive long-term
The dietary caution appropriate for weeks one through four is not necessary at month six. People who maintain extreme restrictions indefinitely develop an unhealthy relationship with food, miss out on nutrition from eliminated food groups, and set themselves up for binge eating when the restrictions inevitably break down. Gradually expand your diet as your body adapts.
Mistake 5: ignoring individual variation
Not everyone on tirzepatide has the same trigger foods. Some people tolerate moderate dairy perfectly well. Others can eat mildly spicy food without any issues. The general guidelines in this article are starting points. Your personal food diary data is the definitive guide for your specific body and digestion.
Tirzepatide foods to avoid: the complete reference table
Here is the comprehensive summary of foods to avoid, limit, or approach carefully on tirzepatide, organized by severity of impact:
Category | Avoid entirely | Limit significantly | Approach carefully |
|---|---|---|---|
Fats | Deep-fried foods, pork belly, fatty processed meats | Ribeye, full-fat dairy, rich desserts | Moderate cheese, dark meat poultry |
Sugars | Soda, candy, sugary drinks | White bread, pasta, pastries | High-glycemic fruits in excess |
Spicy | Extremely hot dishes (first 4-8 weeks) | Moderately spicy foods | Mild seasonings (usually fine) |
Carbonation | Energy drinks | Soda, beer | Sparkling water (some tolerate) |
Alcohol | Heavy consumption, spirits on empty stomach | Beer, cocktails | Small glass of wine with food |
Caffeine | Energy drinks, coffee on empty stomach | More than 2 cups coffee daily | 1-2 cups with food |
Sweeteners | Sorbitol, maltitol in large amounts | Sugar-free gum, diet candy | Small amounts of erythritol, stevia |
Gas producers | Large portions of beans (initially) | Raw cruciferous vegetables | Cooked cruciferous in small portions |
Processed | Fast food, frozen dinners | Processed snacks, deli meats | Minimally processed convenience foods |
Sodium | Excessively salty processed foods | Restaurant meals, canned soups | Moderate seasoning while cooking |
Special considerations by dose level
Your dietary sensitivity on tirzepatide correlates with your current dose level and how long you have been at that dose.
Starting dose (2.5mg)
At the 2.5mg starting dose, most people experience the least severe GI side effects. Dietary modifications should still be implemented, but this is the most forgiving dose level. Use this period to establish good eating habits that will serve you well at higher doses. If you cannot tolerate a food at 2.5mg, it will almost certainly be worse at higher doses.
Escalation doses (5mg, 7.5mg, 10mg)
Each dose increase can temporarily increase GI sensitivity. In the week following a dose escalation, revert to your most conservative dietary approach, the same strategy that worked during your first few weeks. Once side effects stabilize at the new dose (usually within two to four weeks), gradually reintroduce foods as tolerated.
At the 7.5mg level and above, the appetite suppression becomes more significant. This is where protein prioritization becomes critical because the reduced appetite can make it difficult to consume adequate protein without deliberate effort.
Maintenance doses (10mg, 12.5mg, 15mg)
At maintenance doses, your body has had weeks to months to adapt. Most people find that their food tolerances have expanded significantly from where they were during initial treatment. Some people at maintenance doses can eat small amounts of previously problematic foods without issues. But individual variation is large, and some people remain sensitive to specific triggers throughout their treatment.
When food problems might signal something else
While most GI symptoms on tirzepatide are diet-related and manageable, certain symptoms warrant medical attention.
Severe abdominal pain that does not improve with dietary changes could indicate pancreatitis, a rare but serious side effect. Persistent vomiting that prevents any food or fluid intake requires medical evaluation to prevent dehydration and nutritional deficiency. Bloody or black stools suggest GI bleeding and need immediate attention. Symptoms of severe hypoglycemia (confusion, loss of consciousness, seizures) require emergency treatment.
These are uncommon, but they are important to recognize. The difference between normal GI adjustment and a medical concern usually comes down to severity and duration. Mild nausea after eating fried food? Normal adjustment, modify your diet. Severe upper abdominal pain radiating to your back that does not go away? See a doctor immediately.
Our comprehensive safety and risks guide covers additional warning signs and when to seek medical attention across all peptide protocols.
Supplements that can help with food tolerance
Certain supplements may improve food tolerance and reduce GI symptoms on tirzepatide. These are not replacements for dietary modifications but can provide additional support.
Ginger
Ginger has well-documented anti-nausea properties. Fresh ginger tea, ginger capsules (250mg four times daily), or ginger chews can reduce nausea, particularly around meal times. This is one of the most widely recommended natural remedies for tirzepatide-related nausea.
Digestive enzymes
Broad-spectrum digestive enzyme supplements containing lipase (for fat digestion), protease (for protein digestion), and amylase (for carbohydrate digestion) can help your body process food more efficiently despite the delayed gastric emptying. Some people find these particularly helpful when they occasionally eat richer meals.
Probiotics
Tirzepatide altered gut motility can affect the gut microbiome. A quality probiotic supplement may help maintain digestive balance, particularly if you are experiencing diarrhea or alternating constipation and diarrhea. Look for products with well-researched strains like Lactobacillus rhamnosus GG or Saccharomyces boulardii.
Psyllium husk for constipation
If constipation is your primary GI issue (affects 12-16% of tirzepatide users), psyllium husk fiber is the most effective over-the-counter option. Start with one teaspoon daily in a full glass of water and increase gradually to two to three teaspoons as needed. Always take with plenty of water to prevent the fiber from worsening constipation.
Connecting diet with your broader tirzepatide protocol
Food choices do not exist in isolation. They connect to every other aspect of your tirzepatide protocol.
Your dosing schedule affects which days require the most dietary caution. Your reconstitution and preparation practices affect potency, which in turn affects the intensity of GI side effects. Your storage practices affect stability. And your understanding of shelf life ensures you are using effective product.
For those considering switching between GLP-1 options, know that the dietary principles are largely similar across tirzepatide and semaglutide. Both slow gastric emptying, both alter appetite, and both make the same food categories problematic. The intensity of effects may differ, but the dietary strategy remains fundamentally the same.
If you are tracking your results with before and after documentation, note that dietary adherence often correlates strongly with the quality of results. People who manage their diet well on tirzepatide tend to lose more weight, experience fewer side effects, and maintain better body composition than those who continue eating problematic foods and fight through the consequences.
SeekPeptides members get access to comprehensive protocol management tools, including detailed dietary frameworks that complement their peptide protocols. The intersection of nutrition and peptide therapy is one of the most important but least discussed aspects of getting optimal results from any GLP-1 medication.
The psychological side of food avoidance
We need to talk about something most medical guides skip entirely. The psychological impact of food restriction on tirzepatide.
Telling someone to avoid a long list of foods can trigger anxiety, guilt, and an unhealthy relationship with eating. This is especially true for people who have a history of yo-yo dieting, restrictive eating, or eating disorders. If reading this article makes you feel anxious about every meal, please understand this: the goal is not perfection. The goal is awareness.
You will eat fried food sometimes. You will have a sugary dessert at a birthday party. You might have a glass of wine at dinner. These are not failures. They are normal human experiences. The purpose of understanding trigger foods is to make informed choices, not to create a prison of dietary rules.
When you eat a trigger food and experience discomfort, it is not a punishment. It is data. Your body is telling you how it responds to that food under the current conditions of your protocol. Use the information. Adjust next time. And move on without guilt.
Frequently asked questions
Can I eat fruit while taking tirzepatide?
Yes. Fruit is encouraged on tirzepatide for its vitamins, minerals, and fiber. Focus on lower-glycemic options like berries, apples, pears, and citrus fruits. Limit high-glycemic fruits like bananas, pineapple, and grapes to moderate portions as part of balanced meals rather than large quantities on an empty stomach.
How long do food-related side effects last after eating a trigger food?
Due to delayed gastric emptying, side effects from trigger foods on tirzepatide can last three to eight hours, significantly longer than they would without the medication. High-fat meals tend to cause the longest-lasting discomfort. This duration typically decreases as your body adapts to the medication over the first several weeks.
Should I eat before or after my tirzepatide injection?
Eat a light, tirzepatide-friendly meal before your injection. An empty stomach at injection time can worsen initial nausea. After injection, keep meals small and simple for the following 24 to 48 hours when side effects tend to peak. Review our dosing guide for more injection timing details.
Can I drink protein shakes on tirzepatide?
Protein shakes are actually one of the best supplemental options on tirzepatide because they provide concentrated protein in an easily digestible form. Choose low-fat protein powders (whey isolate or plant-based) mixed with water or low-fat milk. Avoid shakes loaded with added sugars, fats, or sugar alcohols. Limit to one to two per day as supplements, not meal replacements for every meal.
Is it normal to not want to eat at all on tirzepatide?
Significantly reduced appetite is a common and expected effect of tirzepatide. However, eating nothing is not recommended. Aim for at minimum 1,000-1,200 calories daily with adequate protein to prevent muscle loss, nutritional deficiencies, and other complications. If you truly cannot eat, speak with your healthcare provider about dose adjustment.
Do the food restrictions apply to compounded tirzepatide too?
Yes. The food restrictions apply identically to compounded tirzepatide because the active molecule is the same regardless of the source. The mechanism of action, the effect on gastric emptying, and the resulting dietary sensitivities are identical between brand-name and compounded formulations.
Can I eat spicy food again after adjusting to tirzepatide?
Most people can reintroduce moderate spice after four to eight weeks at a stable dose. Start with mild seasonings and gradually increase heat level. Avoid combining spice with other trigger factors like high fat. If you tolerate mild spice at lunch, try slightly more next time. Build back gradually based on your individual tolerance.
What if I am not losing weight even after following these dietary guidelines?
Diet is one factor in tirzepatide weight loss outcomes. If you are following dietary guidelines but not losing weight, review your complete protocol including dose adequacy, exercise habits, sleep quality, stress levels, and medication timing. Sometimes a dose adjustment is needed. Consult with your healthcare provider if progress stalls for more than four weeks.
External resources
PMC: Tirzepatide-Induced Gastrointestinal Manifestations: A Systematic Review
PMC: Clinical Consequences of Delayed Gastric Emptying With GLP-1 Receptor Agonists and Tirzepatide
PMC: Dietary Recommendations for GI Symptom Management in GLP-1 RA Patients
For researchers serious about optimizing their peptide protocols, SeekPeptides offers the most comprehensive resource available, with evidence-based guides, proven protocols, and a community of thousands who have navigated these exact questions. Whether you need help with dosing calculations, reconstitution protocols, or connecting dietary strategy with your broader peptide research, SeekPeptides provides the tools and community support to get it right.
In case I do not see you, good afternoon, good evening, and good night. May your meals stay comfortable, your side effects stay minimal, and your results stay consistent.