Feb 18, 2026

You started tirzepatide to lose weight. Maybe to fix your blood sugar. But somewhere around week three, something unexpected happened. You felt lighter. Not just on the scale. In your body. In your head. You woke up before your alarm. You finished a full day of work without reaching for a fourth cup of coffee.
Or maybe the opposite happened.
Maybe you feel drained. Exhausted. Like someone pulled the plug on your batteries and forgot to tell you. And now you are reading this because you want to know: does tirzepatide actually give you energy, or is this medication supposed to make you feel like you ran a marathon in your sleep?
The honest answer is both. And neither. It depends on where you are in treatment, how your body metabolizes fuel, what you are eating, and a dozen other variables that most articles gloss over with vague reassurances. This guide goes deeper. We will walk through the actual mechanisms behind tirzepatide energy changes, what the clinical data from peer-reviewed research shows about energy expenditure and fat oxidation, why some people feel supercharged while others feel flattened, and what you can do to land on the right side of that equation. Whether you are just getting started with peptides or months into your tirzepatide protocol, the information here draws from clinical trial data, published metabolic studies, and thousands of real-world experiences from the SeekPeptides community.
How tirzepatide changes the way your body produces energy
Before you can understand whether tirzepatide gives you energy, you need to understand how it rewires your entire metabolic engine. This is not a stimulant. It does not work like caffeine or phentermine. There is no jolt.
What tirzepatide does is far more fundamental.
The dual receptor mechanism and why it matters for energy
Tirzepatide activates two receptors simultaneously: GLP-1 (glucagon-like peptide-1) and GIP (glucose-dependent insulinotropic polypeptide). Most weight loss peptides in the GLP-1 class only hit one of these. Semaglutide, liraglutide, and the older incretin drugs are pure GLP-1 agonists. Tirzepatide is different because it engages both pathways.
Why does this matter for energy?
GLP-1 receptor activation primarily handles appetite suppression, blood sugar regulation, and slowing gastric emptying. These are the mechanisms most people associate with GLP-1 medications. But GIP receptor activation does something GLP-1 alone cannot. Research published in Cell Metabolism shows that GIP receptor agonism modulates how your body stores and releases energy from fat cells. In the fasting state, GIP activation promotes energy release from adipose tissue. In the fed state, it supports efficient energy storage. This metabolic flexibility, the ability to switch smoothly between burning stored fat and using incoming nutrients, is the foundation of sustained energy.
A study from the American Diabetes Association demonstrated that tirzepatide has direct effects on insulin secretion, insulin sensitivity, appetite regulation, and adipose tissue metabolism. These are not separate effects. They are interconnected parts of one metabolic overhaul. When insulin sensitivity improves, cells absorb glucose more efficiently. When adipose tissue metabolism shifts, stored fat becomes accessible fuel. When appetite regulation stabilizes, the blood sugar rollercoaster that causes energy crashes flattens out.
Understanding how peptides work at this level makes the energy question much clearer. Tirzepatide does not inject energy into your system. It removes the metabolic roadblocks that were preventing your body from accessing energy it already had.
Fat oxidation: your body learning to burn its own fuel
A landmark study published in Cell Metabolism in 2025 by researchers at Pennington Biomedical Research Center provided the first direct evidence of how tirzepatide affects energy metabolism during weight loss. The findings were striking.
Tirzepatide significantly reduced 24-hour and sleeping respiratory quotient values. Lower respiratory quotient means more fat oxidation and less carbohydrate burning. In simple terms, participants on tirzepatide were burning more fat for fuel, even while sleeping.
Here is the critical detail. The study also found that tirzepatide did not impact metabolic adaptation. Metabolic adaptation is the process where your metabolism slows down during weight loss, making you feel tired and making further weight loss harder. Every diet triggers it. But tirzepatide, despite causing significant fat loss, did not make this slowdown worse compared to placebo after adjusting for body weight and composition changes.
What does this mean for energy? It means your body is switching to fat burning without the usual metabolic penalty. You are accessing stored energy more efficiently. You are burning fat during sleep. And your metabolic rate is holding steadier than it would on a typical calorie-restricted diet. That is a recipe for better energy, not worse. The fat burning peptide research community has been watching these results closely because they suggest that tirzepatide dual mechanism provides metabolic advantages beyond simple appetite suppression.
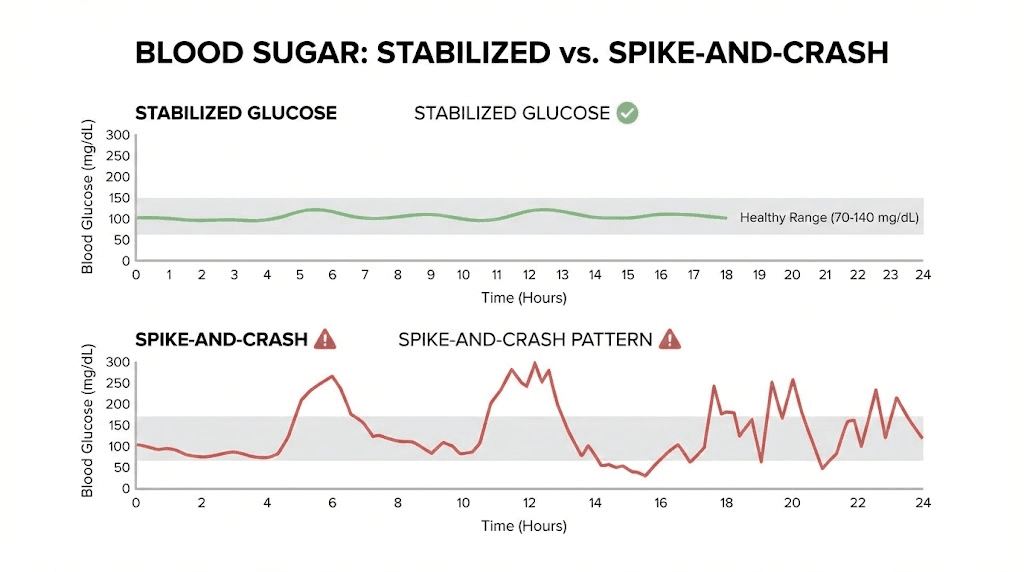
Blood sugar stabilization eliminates the crash cycle
If you have ever felt that 2 PM slump where your eyelids get heavy and your brain turns to fog, you have experienced a blood sugar crash. For people with insulin resistance, pre-diabetes, or type 2 diabetes, these crashes can happen multiple times daily. They are exhausting. Literally.
Tirzepatide addresses this directly.
By enhancing insulin secretion in a glucose-dependent manner and improving insulin sensitivity, tirzepatide flattens the blood sugar spikes and crashes that drive energy fluctuations. Instead of glucose flooding your bloodstream after a meal and then plummeting two hours later, levels rise gently and decline gradually. The brain, which uses about 20% of your total energy and relies heavily on steady glucose supply, functions better when fuel delivery is consistent.
In the SURPASS clinical trials studying tirzepatide for type 2 diabetes, 79% of participants in exit interviews reported increased energy levels. Not just stable energy. Increased. These were people who had been living with the metabolic dysfunction of diabetes, where cells cannot efficiently use available glucose despite having plenty circulating in the blood. When tirzepatide fixed that dysfunction, the subjective experience was a significant energy boost. For a deeper look at how tirzepatide works over time, the blood sugar stabilization pathway is one of the earliest benefits most people notice.
This is fundamentally different from stimulant energy. Stimulants override your fatigue signals. Tirzepatide fixes the metabolic dysfunction causing the fatigue in the first place. One is a band-aid. The other is a repair. If you have been exploring the best peptides for energy, understanding this distinction between masking fatigue and resolving its root cause changes how you evaluate every option.
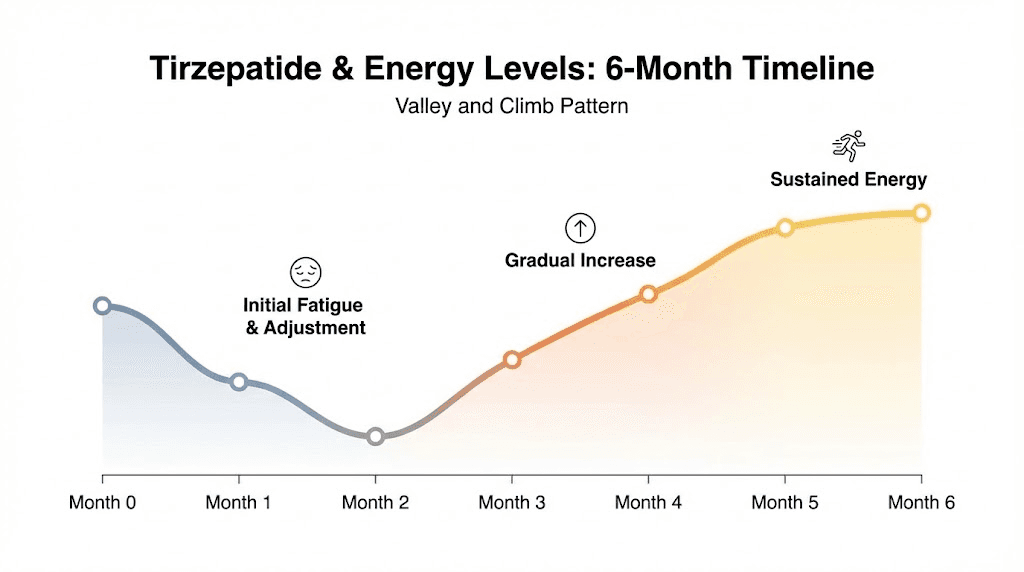
The timeline: when energy changes actually happen
Energy changes on tirzepatide follow a predictable pattern. But the pattern is not linear. It looks more like a valley and then a climb. Understanding where you are on this timeline prevents premature conclusions about whether the medication is working for or against your energy.
Weeks 1 through 4: the adjustment valley
Most people start tirzepatide at 2.5 mg weekly. This is a tolerability dose, not a therapeutic dose. Even at this low level, your body notices something has changed.
Appetite decreases. Caloric intake drops. If you were eating 2,200 calories daily and suddenly only want 1,500, your body experiences an abrupt energy deficit. Not a metaphorical one. A literal thermodynamic one. You have less fuel coming in than your body is accustomed to burning.
The result? Fatigue. For some people, mild. For others, significant.
Clinical data from Eli Lilly shows that fatigue affects approximately 5% of people at the 5 mg dose. But community reports suggest the number is higher when you include people who experience mild tiredness without formally reporting it. The tirzepatide fatigue guide covers this in extensive detail if you are in this phase right now.
This initial fatigue is not a sign that something is wrong. It is your body adjusting to a new fuel supply. Think of it like switching from gasoline to diesel in a hybrid engine. The engine needs time to recalibrate. During that recalibration, performance dips temporarily.
Weeks 4 through 8: the adaptation phase
Around the four-week mark, something shifts. Your body begins upregulating fat oxidation enzymes. Mitochondria adapt to processing more fatty acids for fuel. Blood sugar patterns stabilize into a new, smoother rhythm. The caloric deficit that felt like starvation starts feeling like normal.
This is when many people first notice energy improvements. Not dramatic. Not overnight. But a gradual sense that you have more in the tank than you did two weeks ago. Morning brain fog clears. Afternoon slumps become less severe. You find yourself wanting to go for walks instead of collapsing on the couch.
The research from the Pennington Biomedical study supports this timeline. Fat oxidation increases significantly within the first weeks of treatment, and as your body becomes more efficient at accessing stored fat, the energy that was locked away in adipose tissue becomes available for daily use.
For people who are also dealing with blood sugar issues, this is when the 79% energy improvement statistic from the Mounjaro trials starts to make sense. The metabolic machinery has been repaired. Cells are absorbing glucose properly. The brain has steady fuel. Energy follows naturally. Understanding how fast tirzepatide works helps set realistic expectations for this transition period.
Weeks 8 through 16: the energy dividend
By the two to four month mark, most of the metabolic adaptation has occurred. Your body is running on a new operating system. Fat oxidation is elevated. Blood sugar is stable. And if you have been doing any physical activity, you are now doing it in a lighter body.
This is where the compounding benefits stack up.
You weigh less, so every movement requires less energy. You sleep better because weight loss improves sleep quality and can reduce sleep-related issues like snoring and apnea. Systemic inflammation has decreased because you have less inflammatory adipose tissue. Your cardiovascular system is under less strain. All of these improvements feed into a single subjective experience: more energy.
Many long-term users describe this phase as feeling better than they have in years. Some say decades. The energy is not artificial or temporary. It is the natural result of a body that is metabolically healthier.
Month 6 and beyond: the new normal
After six months of treatment, the energy landscape stabilizes at a level that typically exceeds pre-treatment baseline. The reasons compound further at this stage.
Significant weight has been lost, reducing the daily physical burden. Blood sugar regulation has been consistent for months. Inflammation markers continue to improve. Exercise capacity has increased because a lighter body moves more efficiently. Mood often improves from the accomplishment of meaningful health changes.
This mirrors the experience seen across other peptide transformation journeys. Short-term discomfort during adaptation gives way to long-term benefits that justify the investment. The before and after results in energy are often as dramatic as the physical changes.
Five mechanisms through which tirzepatide boosts energy
The energy improvements on tirzepatide are not random. They trace back to specific, measurable biological changes. Understanding each one helps you maximize the benefit.
1. Reduced physical burden from weight loss
This is the most straightforward mechanism. Every pound of excess body weight increases the energy cost of movement. Walking, climbing stairs, standing, even breathing requires more effort when you carry more mass. A person carrying 60 extra pounds uses significantly more energy for every daily activity than someone at a healthy weight.
When tirzepatide drives weight loss, this physical tax decreases proportionally. People who lose 40, 60, or 80 pounds consistently report dramatic improvements in how easy daily life feels. The stairs that left them breathless become routine. The walk to the car is not an ordeal. Playing with children or grandchildren does not require a recovery period afterward.
The SURMOUNT-1 trial demonstrated average weight loss of 22.5% of body weight over 72 weeks with tirzepatide 15 mg. For a 250-pound person, that is over 56 pounds. The energy saved from not carrying 56 extra pounds through every moment of every day is substantial. It is the difference between hiking with a loaded backpack and hiking free. The tirzepatide before and after stories frequently highlight energy as the most impactful quality-of-life change, even more than the visual transformation.
2. Improved insulin sensitivity and cellular energy production
Insulin resistance is an energy thief.
When cells become resistant to insulin, they cannot efficiently absorb glucose from the bloodstream. Glucose piles up in the blood, causing hyperglycemia, while cells simultaneously starve for fuel. This paradox, too much sugar in the blood but not enough in the cells, is one of the primary drivers of the fatigue that accompanies metabolic syndrome and type 2 diabetes.
Tirzepatide dramatically improves insulin sensitivity. The mechanism involves both GLP-1 and GIP receptor pathways. GIP receptor activation enhances insulin signaling at the cellular level, augmenting glucose uptake. Research published in Cell Metabolism showed that GIPR agonism augmented glucose uptake and increased the conversion of glucose to glycerol in a cooperative manner with insulin.
In practical terms, your cells start absorbing glucose efficiently again. The fuel that was floating uselessly in your bloodstream is now being delivered where it is needed. Mitochondria, the energy-producing structures in every cell, have adequate substrate to produce ATP. More ATP production means more cellular energy. More cellular energy means you feel more energized.
This mechanism explains why people with insulin resistance and type 2 diabetes often experience the most dramatic energy improvements on tirzepatide. They had the most dysfunction to correct. Fixing a severe problem produces more noticeable results than fine-tuning a system that was already working adequately. Anyone exploring the fundamentals of peptides will find that this cellular-level mechanism, improving how cells produce and use energy, is a common thread across many therapeutic peptide applications.
3. Better sleep from weight loss and reduced sleep apnea
Poor sleep and low energy are inseparable. You cannot have sustained energy without restorative sleep. And obesity is one of the primary causes of poor sleep, largely through obstructive sleep apnea.
The SURMOUNT-OSA trials tested tirzepatide specifically in people with obesity and moderate-to-severe sleep apnea. The results were remarkable. Tirzepatide significantly reduced the apnea-hypopnea index, improved sleep quality scores on validated measures, and reduced daytime sleepiness as measured by the Epworth Sleepiness Scale.
Among treated participants, 71.7% of those classified as non-fatigued at baseline and 69.7% of those classified as fatigued rated their fatigue as meaningfully better after treatment. A post-hoc analysis presented at the 2025 SLEEP Annual Meeting showed that participants who were moderately to very sleepy at baseline showed even greater improvements in sleep-related outcomes.
Better sleep means better energy. Not through any direct pharmacological mechanism. Through fixing a structural problem, excess weight compressing the airway during sleep, that was destroying sleep quality every single night. For the millions of people with undiagnosed sleep apnea who just think they are always tired, tirzepatide-driven weight loss may be the most effective energy intervention available.
If sleep quality is a concern during your protocol, understanding optimal injection timing can also help minimize nighttime GI disruptions that interfere with rest. The semaglutide fatigue guide covers similar sleep optimization strategies that apply to tirzepatide users as well.
4. Reduced systemic inflammation
Chronic inflammation is invisible fatigue. You cannot see it. You cannot point to it. But it sits in your body like a slow drain on a battery, steadily pulling energy away from where it is needed.
Excess adipose tissue is an active endocrine organ that produces inflammatory cytokines, including TNF-alpha, IL-6, and CRP. These molecules create a state of chronic low-grade inflammation that causes fatigue, brain fog, muscle aches, and reduced motivation. If you have ever had the flu, you know what inflammation-driven fatigue feels like. Now imagine a milder version of that, persistent, unrelenting, lasting for years.
Tirzepatide reduces inflammatory markers through multiple pathways. Direct anti-inflammatory properties of GLP-1 receptor activation combine with the indirect inflammation reduction from losing visceral fat. Clinical studies have documented improvements in endothelial dysfunction and reductions in pro-inflammatory biomarker release. A narrative review on tirzepatide in lipedema specifically highlighted its ability to bridge metabolism, inflammation, and fibrosis, demonstrating that the anti-inflammatory effects extend beyond simple weight loss.
As inflammation decreases, the fatigue it caused resolves. Many people describe it as a fog lifting. They did not realize how much their chronic low-grade inflammation was affecting their energy until it was gone. This is one reason why energy improvements on tirzepatide can feel disproportionate to the weight lost. Losing 15 pounds should not transform how you feel. But if that 15 pounds of adipose tissue was pumping inflammatory chemicals into your bloodstream 24 hours a day, removing it absolutely can. The inflammation peptide research explores how various compounds address systemic inflammation, and tirzepatide dual agonism represents one of the more powerful approaches available.
5. Enhanced fat oxidation as a fuel source
We covered the Pennington Biomedical Research Center study earlier, but the energy implications deserve their own spotlight.
When your body runs primarily on glucose, it needs constant refueling. Glucose stores in the form of glycogen are limited, roughly 2,000 calories worth in liver and muscle tissue. Once those are depleted, you need to eat again or your energy crashes.
Fat stores, by contrast, are enormous. Even a lean person carries 40,000 to 80,000 calories of stored fat. An overweight person may carry 150,000 or more. This is a massive energy reserve that most people cannot efficiently access because their metabolism is locked into glucose-burning mode.
Tirzepatide shifts this. The reduced respiratory quotient values measured in the clinical study indicate that participants were burning significantly more fat relative to carbohydrates. This metabolic shift means your body is learning to tap into a nearly unlimited fuel source instead of relying on a small, easily depleted one.
The practical energy implication is significant. When your body can smoothly transition from burning incoming food to burning stored fat, the energy dips between meals disappear. You do not crash at 2 PM because your body has seamlessly shifted to fat oxidation. You do not bonk during exercise because fatty acids are available as backup fuel. You feel more consistent energy throughout the day because your body is no longer dependent on frequent glucose refueling.
This is what researchers mean by metabolic flexibility, and it may be the single most important energy benefit of tirzepatide treatment. The best peptides for energy and focus all share this common thread: they improve how cells generate and use energy rather than simply masking fatigue. The MOTS-c peptide, for instance, directly targets mitochondrial energy production, while tirzepatide achieves similar metabolic flexibility through a completely different receptor pathway.

Why some people feel drained instead of energized
Not everyone experiences an energy boost on tirzepatide. Understanding why helps you troubleshoot if you are on the wrong side of this equation.
The caloric deficit went too far
Tirzepatide is powerful appetite suppression. Some people go from 2,200 calories daily to under 1,000 without realizing it. When you eat that little, no amount of metabolic optimization will overcome the raw energy deficit. Your body simply does not have enough fuel to function normally.
The solution is counterintuitive: eat more. Not more junk. More protein-rich, nutrient-dense food. If you are consuming fewer than 1,200 calories daily as a woman or 1,500 as a man, you are likely in too aggressive a deficit. Your body is in conservation mode, slowing everything down to preserve reserves. The guide to eating on tirzepatide and the foods to avoid on tirzepatide resource both address this caloric floor issue in detail.
Protein matters most here. Research consistently shows that protein intake below 1.2 grams per kilogram of body weight accelerates muscle loss during weight loss. Muscle loss reduces metabolic rate, which deepens fatigue, which reduces motivation to eat, which worsens the deficit further. A vicious cycle. Breaking it requires deliberate, strategic eating even when you are not hungry.
Dehydration and electrolyte depletion
The gastrointestinal side effects of tirzepatide, nausea in 24% to 31% of users, diarrhea in 18% to 23%, vomiting in 8% to 12%, create fluid and electrolyte losses that many people do not adequately replace. Sodium, potassium, and magnesium are essential for cellular energy production. When they drop, fatigue is one of the first symptoms.
Most people respond to nausea by drinking less. This makes everything worse. A minimum of 64 ounces of water daily is a floor, not a ceiling. If GI side effects are active, increase to 80 to 100 ounces. Add a sugar-free electrolyte supplement twice daily. Check your urine color: pale yellow means adequate hydration, dark yellow means you need fluids immediately.
This is one of the most common mistakes beginners make with peptides of any kind. Adequate hydration is as fundamental to results as proper peptide reconstitution is to potency. You can have the perfect protocol and still feel terrible if you are dehydrated.
Micronutrient deficiencies creeping in
When you eat less food, you get fewer vitamins and minerals. This obvious fact has serious consequences that most prescribers gloss over.
Iron deficiency causes fatigue through reduced oxygen transport. B12 deficiency impairs energy metabolism at the cellular level. Vitamin D deficiency, already present in 35% to 40% of adults, worsens with reduced food intake. Magnesium, involved in over 300 enzymatic reactions including energy production, is depleted both by reduced intake and by GI-related losses.
If your fatigue persists beyond the expected 4 to 8 week adaptation window, get blood work. Ferritin, B12, vitamin D, and magnesium levels will identify the most common correctable causes. The supplements to take with tirzepatide guide covers the evidence-based supplement stack that addresses these specific risks.
Lean mass loss reducing metabolic capacity
Not all weight lost on tirzepatide is fat. Research shows that lean tissue accounts for 20% to 34% of total weight lost. Muscle is metabolically active tissue. When you lose it, your baseline energy production decreases. Daily activities that previously felt easy start requiring more relative effort.
This is the strongest argument for combining tirzepatide with resistance training. The mechanical stimulus of lifting weights tells your muscles they are needed, preserving them during caloric restriction. Without that signal, the body is content to catabolize muscle along with fat. The muscle growth peptide research emphasizes that maintaining lean mass is not just about appearance. It is about preserving the metabolic machinery that produces energy.
Aim for at least three resistance training sessions weekly. Focus on compound movements: squats, deadlifts, rows, presses. Pair training with adequate protein, 1.4 to 1.6 grams per kilogram of body weight daily. These two interventions, protein and resistance training, have more impact on energy during tirzepatide treatment than any supplement or injection timing strategy.
Tirzepatide energy versus semaglutide energy: key differences
If you have experience with semaglutide or are comparing the two medications, the energy profiles differ in meaningful ways.
The GIP advantage
Semaglutide is a pure GLP-1 receptor agonist. It suppresses appetite, slows gastric emptying, and improves blood sugar. But it does not activate GIP receptors.
GIP receptor activation, unique to tirzepatide in the approved medication space, provides additional metabolic benefits that relate directly to energy. As the Cell Metabolism research demonstrated, GIP agonism modulates both storage and release of high-energy macronutrients. In the fasting state, energy release is stimulated. In the fed state, energy storage is stimulated. This intelligent, context-dependent metabolic regulation is something pure GLP-1 agonists cannot provide.
The practical difference? Some people who felt persistently tired on semaglutide report better energy on tirzepatide. The dual agonism appears to produce a smoother metabolic transition during weight loss. The semaglutide versus tirzepatide side effects comparison covers the full spectrum of differences between these medications, but energy is one area where tirzepatide dual mechanism may offer an advantage.
Greater weight loss, greater energy potential
Tirzepatide produces more weight loss than semaglutide at equivalent timepoints. The tirzepatide versus semaglutide dosage comparison shows different dose escalation patterns, but the bottom line is that tirzepatide typically drives a larger total weight reduction.
More weight loss means more reduction in the physical burden of daily activity, more improvement in sleep quality, more reduction in inflammation, and more correction of metabolic dysfunction. All of these compound into a greater total energy improvement over time.
The tradeoff is that the initial adaptation phase may be more intense. A sharper caloric deficit in the early weeks can mean more pronounced initial fatigue. But for most people, this deeper valley leads to a higher peak on the other side. People who switch from semaglutide to tirzepatide should understand the transition dynamics and the conversion charts to minimize disruption during the switch.
Individual variation matters most
Some people feel incredible energy on semaglutide. Some feel better on tirzepatide. Some feel tired on both. The receptor activation profiles create different responses in different bodies, and there is no way to predict which medication will work better for any individual without trying them.
If energy is a primary concern alongside weight loss, tirzepatide theoretical advantage through dual agonism is worth considering. But it is not a guarantee. Metabolic individuality overrides receptor pharmacology in many cases. The semaglutide energy guide covers how energy changes work on GLP-1-only therapy if you are evaluating both options.
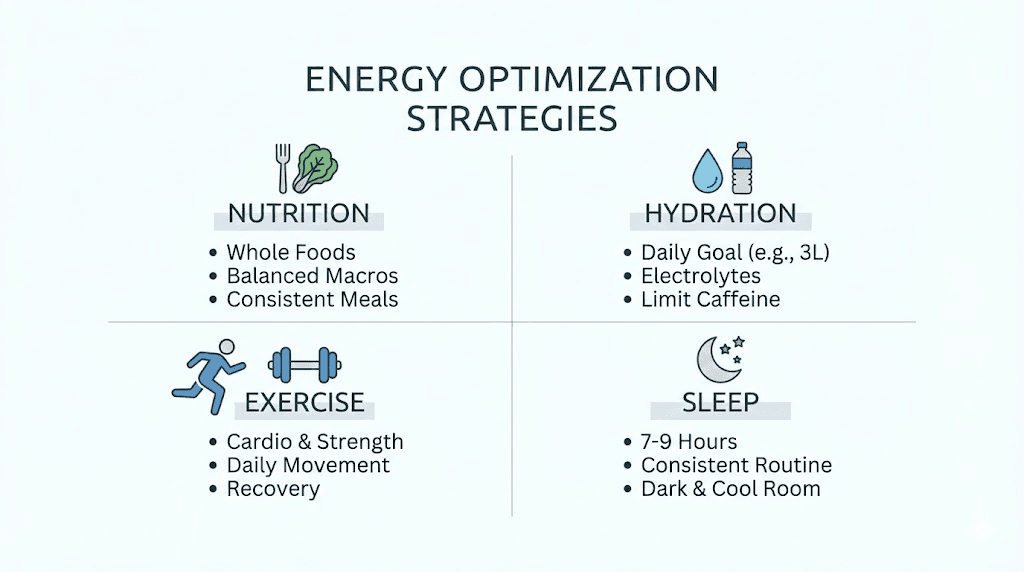
How to maximize energy while on tirzepatide
Whether you are in the early fatigue phase or looking to optimize energy during maintenance, these strategies address the specific mechanisms behind tirzepatide energy changes.
Nutrition: the non-negotiable foundation
Everything starts with food. Even though you are not hungry, what you eat determines how much energy your body can produce.
Protein first, always. Target 1.2 to 1.6 grams per kilogram of body weight daily. For a 180-pound person, that is 98 to 131 grams minimum. When appetite is suppressed, protein shakes become tools, not luxuries. A shake with 40 grams of protein, blended with nut butter and a banana, delivers substantial nutrition in a form that works with suppressed appetite rather than against it.
Eat frequently in small amounts. Four to five small protein-rich meals beat three normal-sized meals that your appetite will not allow. Smaller, more frequent eating keeps blood sugar stable, provides consistent amino acid availability, and avoids the extended post-meal sluggishness that comes from large meals sitting in a stomach with delayed gastric emptying.
Do not fear calorie-dense foods. Nuts, avocados, olive oil, full-fat dairy, and fatty fish deliver more energy per bite than high-volume, low-calorie options. When you can only eat small amounts, caloric density matters. A handful of almonds provides more sustained energy than a giant salad. Use the peptide calculator for dosing precision, and apply that same precision to your nutrition.
Complex carbohydrates deserve attention too. Sweet potatoes, oats, quinoa, and brown rice provide sustained glucose release without the spike-and-crash pattern of simple carbohydrates. The tirzepatide diet plan and tirzepatide meal plan resources provide detailed frameworks for eating strategically during treatment.
Hydration: the overlooked energy lever
Dehydration causes fatigue before it causes thirst. By the time you feel thirsty, your body has already been operating at reduced capacity for hours.
Minimum 64 ounces of water daily. Increase to 80 to 100 ounces if experiencing GI side effects or exercising. Sip throughout the day rather than drinking large volumes at once, since large boluses on a stomach with delayed gastric emptying can worsen nausea.
Electrolyte supplementation is essential, not optional, when GI side effects are present. Sodium, potassium, and magnesium participate directly in cellular energy production. Sugar-free electrolyte packets twice daily can produce noticeable energy improvements within days. This is one of the simplest and most effective interventions available. The connection between proper hydration and peptide safety applies universally across all compounds.
Movement: the paradox that works
When you are tired, the last thing you want to do is exercise. But research consistently shows that moderate exercise improves fatigue, even when the fatigue is medication-related.
During the early adaptation phase, walking 20 to 30 minutes daily is enough. Do not try to maintain your pre-tirzepatide exercise intensity. Your body is adjusting. Meet it where it is.
As energy improves, introduce resistance training. Two to three sessions per week focusing on compound movements preserves lean mass, maintains metabolic rate, and actually generates energy rather than depleting it. The process of building and maintaining muscle increases mitochondrial density, which increases the capacity of every cell to produce ATP. More mitochondria means more energy production capacity. It is biological infrastructure investment. For specific guidance, the fat burning protocols for men and belly fat reduction approaches include exercise protocols designed to work alongside GLP-1 therapy.
Many long-term tirzepatide users report that exercise is the single most impactful energy intervention beyond adequate nutrition. The combination of a lighter body, improved cardiovascular fitness, and preserved muscle mass creates an energy level that exceeds pre-treatment baseline.
Sleep: where energy is manufactured
Sleep is not rest. Sleep is active metabolic recovery. During deep sleep, growth hormone is released, tissues are repaired, memories are consolidated, and the glymphatic system clears metabolic waste from the brain. Without adequate sleep, none of the other energy strategies matter.
Aim for 7 to 9 hours of actual sleep nightly. Not time in bed. Time asleep. Consistent sleep and wake times are more important than total hours. Your circadian rhythm responds to regularity.
Injection timing can influence sleep. Some users find morning injections work best because GI side effects settle by bedtime. Others prefer evening injections because the initial side effect peak passes during sleep. There is no universal answer, but experimenting intentionally is worthwhile.
Magnesium glycinate (200 to 400 mg) at bedtime serves double duty: supporting energy production during the day and improving sleep quality at night. It is one of the most efficient supplements you can add. For deeper sleep optimization strategies alongside peptide protocols, the DSIP peptide research covers how sleep-specific compounds work, and the pineal peptide guide explores circadian rhythm support.
The supplement stack that supports energy
Targeted supplementation addresses the specific gaps created by reduced food intake:
Electrolyte supplement (sugar-free, with sodium, potassium, magnesium): daily, twice daily if GI symptoms present
Magnesium glycinate (200 to 400 mg at bedtime): energy production and sleep quality
B-complex vitamin: daily, for energy metabolism pathways
Vitamin D3 (2,000 to 5,000 IU daily): based on tested levels, for muscle function and energy
Iron (only if ferritin is low): as directed by healthcare provider
Omega-3 fatty acids (2 to 3 grams combined EPA/DHA): for inflammation reduction and brain function
This is not an expensive or complicated supplement list. These are basic, evidence-supported nutrients that address the specific deficiency risks created by eating less food while your body undergoes significant metabolic changes. The same attention to quality that applies to peptide storage and reconstitution applies to your supplement choices.
Energy at different tirzepatide doses
Energy experiences shift as dose increases. Here is what to expect at each level.
2.5 mg: the entry point
At the starting dose, energy changes are typically mild. Some people notice a slight decrease in energy from reduced caloric intake. Others notice no change at all. A small percentage actually feel more energetic from early blood sugar improvements.
This is the time to build habits that will protect your energy at higher doses. Establish your hydration routine. Start tracking protein intake. Begin or maintain light exercise. Get baseline blood work so you can identify deficiencies that develop later. Think of this dose as your preparation phase.
5 mg: where things get real
Appetite suppression intensifies at this dose. The caloric deficit deepens. Fatigue is more likely, affecting approximately 5% of users formally, though many more experience mild tiredness.
This is also where blood sugar benefits become more pronounced. For people with insulin resistance, the improved glucose utilization at this dose can offset the caloric deficit fatigue. Some people experience a net energy gain at 5 mg because their blood sugar regulation improves more than their caloric intake decreases. Use the tirzepatide dosing guide to understand the precise amounts at each level.
10 mg: the metabolic shift
By 10 mg, most metabolic adaptation has occurred if you have been gradually escalating. Fat oxidation is elevated. Blood sugar is more stable. The body has learned to access stored fuel. Many people report that energy at 10 mg is better than at 5 mg, despite the higher dose, because the metabolic improvements have outpaced the caloric deficit effects.
The risk at this dose is inadequate nutrition. Appetite may be profoundly suppressed. You need to eat strategically even when you do not feel like it. A protein shake with added calories from nut butter or olive oil can bridge the gap between what your appetite allows and what your body needs. The compound dosage chart helps ensure precision at higher doses.
15 mg: maximum dose, maximum attention needed
The highest approved dose produces the most weight loss and the most profound appetite suppression. Energy can go either way. If nutrition is maintained, the metabolic benefits at this dose are substantial. If nutrition falls off because appetite is virtually absent, fatigue can be severe.
Not everyone needs 15 mg. If you are achieving your goals at a lower dose with good energy, the highest dose is not necessarily better. The minimum effective dose principle guides every smart peptide protocol: use the least amount that achieves your objectives with the fewest side effects.
Special populations and energy considerations
Different people experience tirzepatide energy effects differently based on their starting metabolic state, age, and health conditions.
People with type 2 diabetes
This group often experiences the most dramatic energy improvements. The 79% of Mounjaro trial participants reporting increased energy were people with type 2 diabetes whose cells were starving for glucose despite having plenty in their bloodstream. Fixing that dysfunction produced energy improvements that were profound and sustained.
If you have type 2 diabetes and start tirzepatide, expect energy improvements to be one of the earlier and most noticeable benefits. The blood sugar stabilization alone can transform how you feel within the first few weeks, even before significant weight loss occurs.
Women over 40
Hormonal changes during perimenopause and menopause compound the energy equation. Declining estrogen affects serotonin production, sleep quality, and metabolic rate. Adding tirzepatide caloric restriction on top of these changes can create a more pronounced fatigue picture initially.
The upside is that the long-term energy benefits may be even more impactful for this group. Weight loss reduces the inflammatory burden that amplifies menopausal symptoms. Improved sleep quality from reduced sleep apnea can be transformative. Blood sugar stabilization addresses the increased insulin resistance that accompanies declining estrogen. Peptide protocols for women over 40 need to account for these hormonal interactions, but the net energy outcome is typically positive once adaptation is complete. The menopause weight loss guide addresses the specific challenges this demographic faces during GLP-1 therapy.
Athletes and active individuals
Athletes face a unique challenge. Their caloric demands are higher due to training, and tirzepatide appetite suppression can create deficits that are too aggressive for athletic performance. A runner burning 3,000 calories daily who can only eat 1,800 is in a 1,200-calorie deficit, far more than intended.
The solution is conscious caloric supplementation. Liquid calories from protein shakes, smoothies with added fats, and calorie-dense recovery meals become essential. Athletes on tirzepatide should use the lowest effective dose and may need to eat beyond satiety to maintain training performance. The cardio endurance peptide research offers additional strategies for maintaining performance during weight loss protocols.
People with existing fatigue conditions
Thyroid disorders, chronic fatigue syndrome, fibromyalgia, and depression all cause fatigue that can compound with tirzepatide effects. If you have a pre-existing condition that affects energy, starting tirzepatide requires closer monitoring.
The good news is that weight loss itself often improves these conditions. Thyroid function can improve with reduced adiposity. Depression often lifts as physical health improves. Fibromyalgia symptoms sometimes decrease with reduced inflammation. But the initial adaptation phase may be harder, and working closely with healthcare providers is essential. Resources on peptide therapy guidance and clinical support can help connect you with providers experienced in managing GLP-1 therapy alongside other conditions.
When to worry about energy on tirzepatide
Most energy changes on tirzepatide are normal and temporary. Some are not.
Red flags that need medical attention
Fatigue that worsens over time instead of improving. Normal adaptation fatigue improves. Getting progressively more tired suggests an underlying cause that needs investigation.
Severe dizziness or lightheadedness upon standing. This indicates significant dehydration, electrolyte imbalance, or hypotension. Not normal adjustment.
New onset of cold intolerance, hair loss, or constipation alongside fatigue. These suggest thyroid dysfunction, which rapid weight loss can trigger or unmask.
Inability to perform daily activities. If fatigue is so severe you cannot work, drive safely, or care for yourself, the dose may need adjustment or the medication may need temporary discontinuation.
Mental health changes. Persistent sadness, loss of interest, or feeling hopeless alongside fatigue may indicate depression. This requires immediate professional attention. The peptide anxiety and depression resource covers the intersection of metabolic health and mental health.
Blood work to request
If energy is not improving on the expected timeline, these tests identify the most common correctable causes:
Complete blood count (screens for anemia)
Ferritin (iron stores, the best indicator of iron status)
Vitamin B12
25-hydroxyvitamin D
TSH and free T4 (thyroid function)
Comprehensive metabolic panel (electrolytes, kidney, liver)
Magnesium (often not included in standard panels)
Fasting glucose and HbA1c
These are inexpensive, widely available tests. The information they provide can mean the difference between months of unnecessary fatigue and a targeted fix that resolves the problem within weeks. Applying the same systematic troubleshooting approach used in peptide dosage calculations to your health metrics ensures you are addressing root causes rather than guessing.
The bigger picture: tirzepatide as a metabolic reset
Zoom out from the daily energy fluctuations and look at what tirzepatide is actually doing to your metabolic system over months and years.
It is not giving you energy in the way caffeine gives you energy. It is rebuilding the metabolic infrastructure that produces energy naturally. It is fixing insulin resistance so cells can absorb fuel. It is shifting fuel utilization toward fat oxidation so you have a virtually unlimited energy reserve. It is reducing the physical burden of excess weight. It is clearing the inflammatory fog that dulls every process in your body. It is improving sleep quality so your body can recover properly.
Each of these changes individually improves energy. Together, they represent a fundamental metabolic reset. The temporary fatigue during adaptation is the cost of this reset. The long-term energy improvement is the return on that investment.
A 2025 study in Cell Metabolism confirmed that tirzepatide reduces calorie intake at meals by an estimated 524.6 calories compared to placebo. It decreases overall appetite, food cravings, tendency to overeat, perceived hunger, and reactivity to foods. Simultaneously, it increases fat oxidation without worsening metabolic adaptation. This is a medication that makes you eat less while making your body more efficient at using what it has. The energy implications of that combination are overwhelmingly positive once the initial adjustment passes.
Comparing tirzepatide to other approaches for peptide-based weight management reinforces this point. Compounds like retatrutide, the triple agonist now in clinical trials, may eventually offer even more pronounced metabolic benefits. Cagrilintide targets amylin pathways for additional appetite and metabolic effects. But for now, tirzepatide dual GLP-1/GIP agonism represents the most advanced approved approach to metabolic resetting available, and its energy effects reflect the depth of that reset.
For researchers serious about understanding and optimizing their metabolic health, SeekPeptides provides evidence-based guides, detailed protocols, and a community of experienced researchers navigating these exact questions. From dosage calculations to stacking strategies, the platform covers the full spectrum of peptide research with the depth and specificity that informed decisions require.
Frequently asked questions
Does tirzepatide give you energy directly like a stimulant?
No. Tirzepatide does not act as a stimulant. It does not contain caffeine, amphetamines, or any stimulant compounds. Instead, it improves the metabolic pathways that produce energy naturally, including cellular energy production through better insulin sensitivity, enhanced fat oxidation, and blood sugar stabilization. The energy improvements are real but come from fixing metabolic dysfunction rather than overriding fatigue signals.
How long until I feel more energy on tirzepatide?
Most people experience initial fatigue during the first 4 to 8 weeks as their body adjusts to reduced caloric intake and new metabolic patterns. Energy typically starts improving around weeks 4 to 8 as fat oxidation increases and blood sugar stabilizes. By 3 to 6 months, most users report energy levels that exceed their pre-treatment baseline. People with type 2 diabetes and significant insulin resistance often notice energy improvements earlier than those without metabolic dysfunction.
Why do some people feel tired on tirzepatide while others feel energized?
The difference usually comes down to nutrition, hydration, and baseline metabolic status. People who maintain adequate protein intake (1.2 to 1.6 g/kg daily), stay well hydrated, and supplement electrolytes tend to experience energy improvements. Those who eat too little, become dehydrated, or develop micronutrient deficiencies experience fatigue. Baseline health matters too. People with insulin resistance and type 2 diabetes often see dramatic energy gains because the medication fixes severe metabolic dysfunction.
Will I lose the energy boost if I stop tirzepatide?
If you stop tirzepatide and regain weight, the metabolic improvements that produced the energy boost will gradually reverse. Weight regain brings back the physical burden, inflammation, insulin resistance, and sleep disruption that caused low energy before treatment. In the SURMOUNT-1 extension study, participants who stopped tirzepatide regained approximately two-thirds of lost weight within one year. Maintaining weight loss through continued treatment or other means is necessary to preserve energy benefits.
Does tirzepatide affect energy differently than semaglutide?
Tirzepatide dual GLP-1/GIP agonism may provide metabolic advantages for energy compared to semaglutide pure GLP-1 agonism. GIP receptor activation enhances fat metabolism and promotes context-dependent energy release from adipose tissue, something GLP-1 alone does not provide. In the Mounjaro diabetes trials, 79% of participants reported increased energy. No comparable statistic exists for semaglutide. However, individual responses vary significantly, and some people do better on one medication than the other. See our semaglutide versus tirzepatide comparison for a complete breakdown.
Can I take energy-boosting supplements alongside tirzepatide?
Basic nutritional supplements like B-complex vitamins, magnesium, vitamin D, and electrolytes are generally safe and recommended to address the nutritional gaps created by reduced food intake. Avoid stimulant-based energy supplements that can worsen dehydration and anxiety. For research-grade compounds, the guide to combining peptides and peptide stack calculator can help evaluate combinations, though any additions to your protocol should be discussed with your healthcare provider.
Does exercise help or hurt energy on tirzepatide?
Exercise helps. The paradox is real but consistent across research: moderate physical activity improves fatigue even when you feel tired. During early treatment, walking 20 to 30 minutes daily is sufficient. As adaptation progresses, resistance training becomes critical for preserving muscle mass, which is one of the most important factors in maintaining long-term energy and performance. The lighter body from weight loss makes exercise progressively easier and more rewarding.
At what tirzepatide dose do people feel the most energy?
There is no universal best dose for energy. Many users report that 10 mg provides the best balance between appetite suppression, weight loss, and manageable energy levels. Some do better at 5 mg with less aggressive appetite suppression. Others need 15 mg for adequate weight loss and ultimately feel better at that dose once adapted. The right dose is the one that achieves your health goals while maintaining quality of life. Use the dosing in units guide to understand the precise amounts at each level.
External resources
Cell Metabolism: Tirzepatide fat oxidation and metabolic adaptation study
Diabetes Care: Tirzepatide reduces appetite, energy intake, and fat mass
In case I do not see you, good afternoon, good evening, and good night. May your metabolism stay flexible, your energy stay consistent, and your protocols stay optimized.