Feb 24, 2026
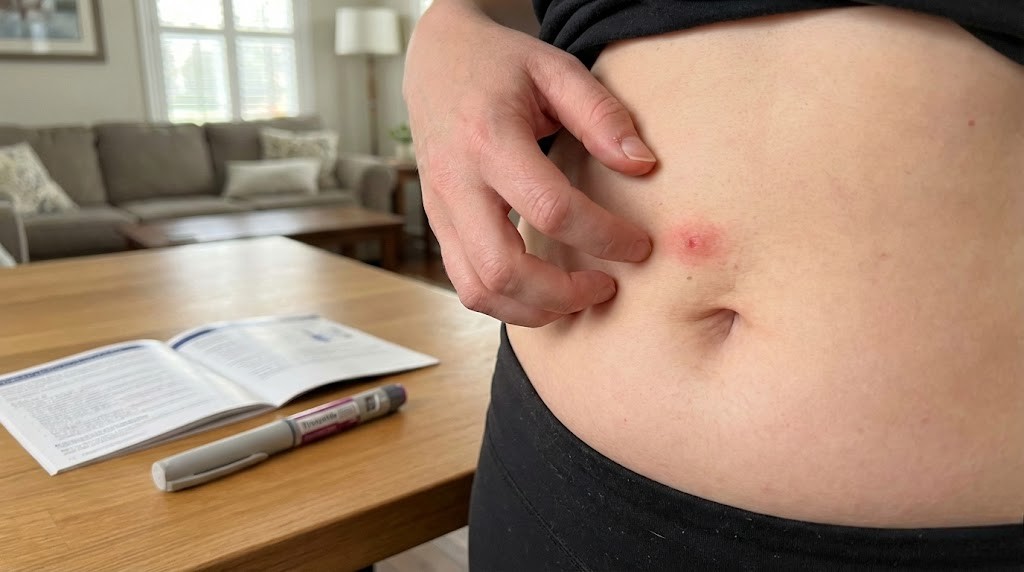
You gave yourself the injection. Everything went fine. The needle was small, the process was quick, and you went about your evening without a second thought. Then you looked down. A red blotch was forming around the injection site. It was warm to the touch. And the itching had started, that persistent, maddening itch that made you want to scratch the spot raw.
Sound familiar?
If you are using tirzepatide for weight loss or metabolic health, injection site redness and itching is one of the most common concerns that sends people searching for answers. The good news is that most of these reactions are completely normal. The inflammatory response your body mounts at the injection site is a predictable, well-documented phenomenon that clinical trials have tracked across thousands of patients. But here is the thing most guides will not tell you: there is a meaningful difference between a routine histamine response and a reaction that warrants a phone call to your healthcare provider. Knowing where that line falls can save you unnecessary panic on one hand, and potentially serious complications on the other. This guide covers exactly what causes that red, itchy spot, how to manage it effectively, when to escalate your concern, and how to prevent it from happening in the first place. Every recommendation here is grounded in clinical trial data, published case reports, and the collective experience of thousands of tirzepatide users who have navigated these exact same reactions.
Why tirzepatide injections cause redness and itching
Understanding the mechanism behind injection site reactions removes a lot of the anxiety. When you inject tirzepatide subcutaneously into the fatty tissue beneath your skin, you are introducing a foreign substance into a space your immune system actively monitors. The response that follows is not a sign that something went wrong. It is your immune system doing exactly what it was designed to do.
Multiple pathways contribute to the redness and itching you see at the injection site. Some are immunological. Some are mechanical. And some relate specifically to the formulation of the medication itself. Knowing which pathway is responsible for your particular reaction helps you choose the right management approach, rather than guessing and hoping for the best.
The histamine response
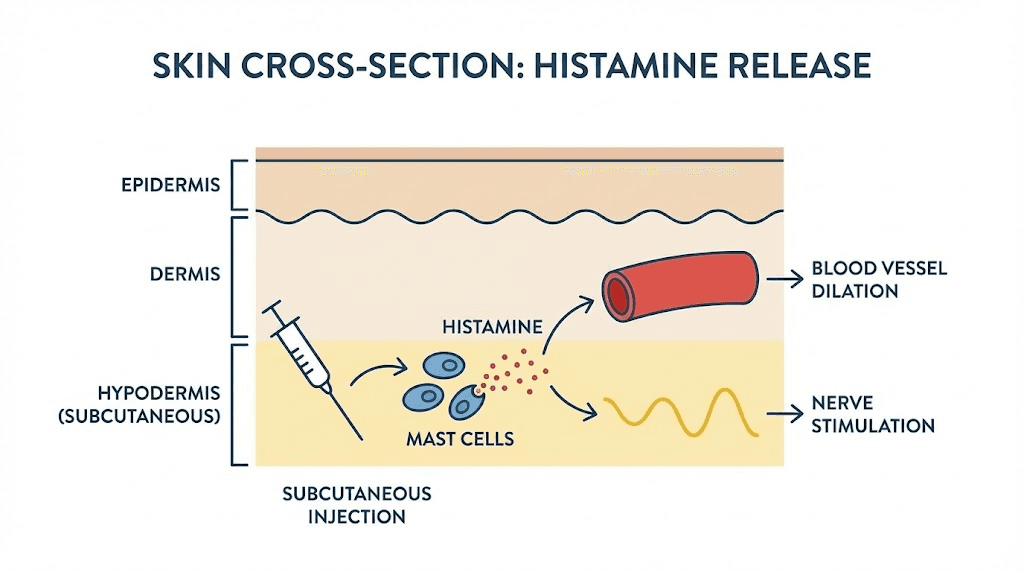
The primary driver of injection site redness and itching is histamine release from mast cells. Mast cells are immune sentinels embedded throughout your skin and connective tissue. When they detect the presence of a foreign substance, whether that is tirzepatide itself or the excipients in the formulation, they degranulate and release histamine along with other inflammatory mediators.
Histamine does several things simultaneously. It dilates local blood vessels, which is why the area turns red. It increases vascular permeability, which causes localized swelling. And it stimulates nerve endings in the skin, which produces the itching sensation. This entire cascade typically begins within minutes of the injection and peaks somewhere between 30 minutes and a few hours later.
The intensity of this response varies dramatically between individuals. Some people have a higher density of mast cells in certain skin areas. Others have mast cells that are more reactive to the specific proteins in GLP-1 receptor agonist formulations. This explains why one person might experience zero reaction while another develops a noticeable red welt every single time, even when using the exact same product and technique.
For anyone interested in how peptides interact with the body at a cellular level, this histamine response is a well-characterized phenomenon. It is not unique to tirzepatide. Semaglutide and other GLP-1 medications produce similar injection site reactions through the same mast cell pathway.
Excipient sensitivity
Tirzepatide is not just the active peptide molecule. The formulation includes excipients, inactive ingredients that stabilize the medication, maintain its pH, and preserve its potency. These excipients can independently trigger localized skin reactions in sensitive individuals.
Brand-name formulations like Mounjaro and Zepbound contain a carefully controlled set of excipients that have undergone extensive safety testing. Compounded versions, however, may contain different stabilizers, preservatives, or pH buffers. If you have switched to compounded tirzepatide and noticed an increase in injection site reactions, the excipient profile is a likely culprit rather than the tirzepatide molecule itself.
Common excipients that can irritate skin include preservatives like benzyl alcohol (sometimes present in multi-dose vials), sodium phosphate buffers, and various polysorbates. People with known sensitivities to any of these compounds should pay close attention to the specific ingredients listed in their medication formulation. Your pharmacist can provide the complete excipient list for your specific product.
Injection technique factors
Not all redness and itching comes from an immune response. Sometimes the problem is purely mechanical.
Injecting too shallow means the medication ends up in the dermal layer rather than the subcutaneous fat, which produces significantly more irritation. Injecting too quickly creates pressure that damages local tissue. Using a needle that is too large causes more trauma than necessary. And failing to pinch the skin properly can result in intramuscular injection, which changes the absorption profile and increases pain.
If you are experiencing injection site reactions specifically in the stomach area, technique refinement often makes a dramatic difference. The abdomen offers plenty of subcutaneous fat for most people, but the technique requirements differ from thigh or upper arm injections. Understanding where to inject GLP-1 medications properly is half the battle for reducing skin reactions.
Temperature matters too. Injecting cold medication straight from the refrigerator causes vasoconstriction followed by a rebound vasodilation response that amplifies redness. If you are storing your tirzepatide in the fridge, whether refrigeration is required depends on the formulation, letting it warm to room temperature for 15-30 minutes before injection reduces this thermal shock response significantly.
Normal reaction vs something more serious
This is the section most people are actually looking for. Your injection site is red. It itches. And you need to know whether this is a normal Tuesday or whether you should be concerned.
Let us establish the baseline first.
What a normal injection site reaction looks like
In the SURPASS clinical trials that evaluated tirzepatide across thousands of participants, injection site reactions were classified as a common adverse effect. The data showed that approximately 3.2% of adults receiving Mounjaro reported injection site reactions, compared to 0.4% on placebo. This means reactions are real and documented, but they affect a relatively small percentage of users.
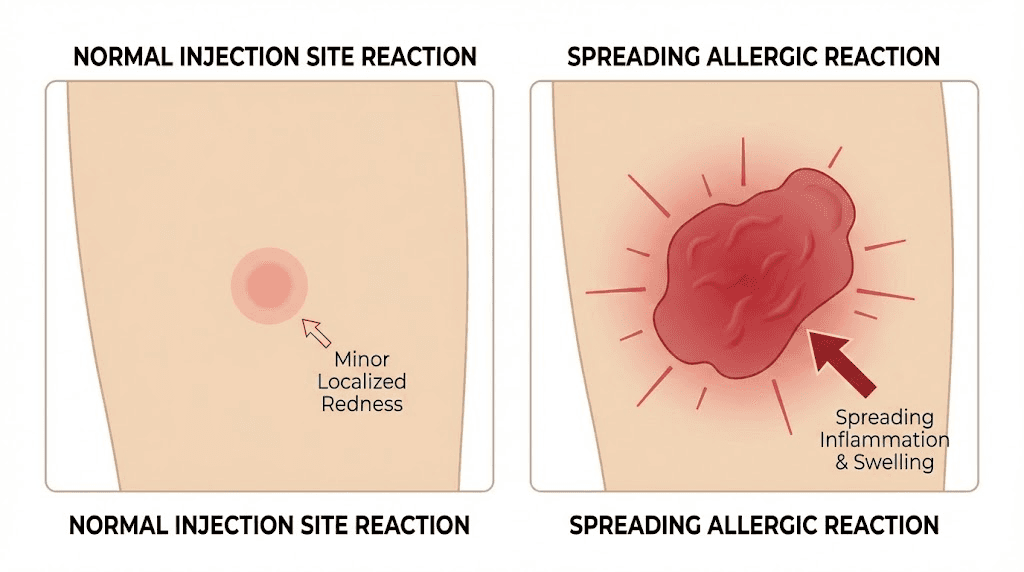
A normal reaction has specific characteristics. The redness typically stays localized to a small area, generally 1-2 inches in diameter around the injection point. The itching is mild to moderate, not severe or unbearable. The area may be slightly warm to the touch and mildly swollen. And critically, these symptoms begin improving within hours and resolve completely within 2-3 days.
Normal reactions do not spread. They do not worsen progressively over time. They do not produce fever, chills, or any systemic symptoms. And they do not interfere meaningfully with daily activities beyond the annoyance factor.
Many people on their tirzepatide weight loss journey find that these mild reactions become less noticeable over time as their body adjusts to the medication. The first few injections tend to produce the most prominent responses, with subsequent injections often causing less and less visible reaction.
Signs that something is not right
A concerning reaction looks meaningfully different from the normal pattern described above. Watch for these specific warning signs that indicate you should contact your healthcare provider.
Spreading redness is the first red flag. If the red area expands beyond 2 inches from the injection site, or if you can see it growing larger over hours rather than smaller, this suggests an infection or a more significant inflammatory response that needs medical evaluation.
Progressive worsening is another concern. Normal reactions peak within a few hours and then gradually improve. If your redness and itching are getting worse at the 24-hour mark rather than better, the trajectory is heading in the wrong direction.
Systemic symptoms change everything. Fever, chills, widespread hives beyond the injection area, difficulty breathing, throat tightness, facial swelling, dizziness, or a rapid heartbeat are all signs of a systemic allergic reaction. These symptoms require immediate medical attention. Some of these, particularly difficulty breathing and throat tightness, may indicate anaphylaxis, which is a medical emergency requiring a call to emergency services.
Pus or drainage from the injection site suggests a bacterial infection. While rare with proper injection safety practices, infections can occur if the skin was not properly cleaned before injection or if the injection site was contaminated.
Persistent hardness or a growing lump that does not resolve within a week warrants evaluation. While small, firm nodules are common and usually harmless, anything that continues growing or becomes increasingly painful needs professional assessment.
Normal vs allergic reaction comparison
Feature | Normal reaction | Allergic reaction |
|---|---|---|
Location | Localized to injection site (1-2 inches) | Spreads beyond injection area, may appear elsewhere |
Onset | Minutes to hours after injection | Can be immediate or delayed |
Duration | Resolves within 2-3 days | Persists or worsens without treatment |
Itching | Mild to moderate, localized | Severe, may include widespread hives |
Swelling | Slight puffiness at site | Progressive swelling, may affect face or throat |
Systemic symptoms | None | Fever, breathing difficulty, dizziness, rapid heartbeat |
Action needed | Home management | Contact healthcare provider or call emergency services |
Understanding this distinction is essential. If your reaction matches the left column, you are dealing with a normal histamine response that can be managed at home. If anything in the right column describes your experience, err on the side of caution and seek medical guidance. It is always better to make an unnecessary phone call than to ignore a genuine warning sign.
Timeline of a typical injection site reaction
Knowing what to expect hour by hour removes much of the anxiety. Here is the typical progression of a normal injection site reaction, broken down into clear timeframes so you can track whether your experience falls within expected parameters.
First 30 minutes
Immediately after the injection, you may notice a tiny pinpoint of redness at the needle entry site. This is normal mechanical trauma from the needle itself. Within 10-30 minutes, the histamine response begins. The redness expands to a circular area perhaps the size of a quarter to a half-dollar coin. Mild warmth develops. The first hints of itching begin, usually subtle at this point.
Some people notice a slight raised bump or welt forming, similar to a mosquito bite. This is the localized edema from histamine-mediated vascular permeability. It looks concerning but is entirely typical.
Hours 1 through 6
This is typically when the reaction reaches its peak intensity. The redness may deepen in color, and the itching often becomes more noticeable during this window. The temptation to scratch is strongest here.
Do not scratch. Scratching damages the skin barrier, amplifies the inflammatory response, and can introduce bacteria into the compromised tissue. If the itching is particularly bothersome during this peak phase, this is the ideal time to apply a cold compress or use an over-the-counter management option, which we will cover in detail in the treatment section below.
If you are tracking your reactions across multiple injections, note the peak intensity and size during this window. Consistent reactions of similar size suggest a predictable histamine response. Reactions that are dramatically larger than previous ones may indicate a change in formulation, technique, or immune sensitivity that is worth investigating.
24 to 48 hours
By this point, a normal reaction should be visibly improving. The redness fades from a bright red to a lighter pink. The itching decreases substantially or disappears entirely. Any swelling should be resolving.
You may notice the area feels slightly tender to pressure, similar to a mild bruise. This is normal residual inflammation that the body is actively clearing. The tissue repair process is underway, and the immune response is winding down.
If you are still experiencing significant redness, itching, or swelling at the 48-hour mark, you are at the outer edge of the normal timeline. Continued worsening at this point shifts the reaction from the "monitor at home" category to the "contact your provider" category.
Beyond 72 hours
At 72 hours, a normal injection site reaction should be nearly or completely resolved. You might see a faint pink mark or feel slight tenderness if you press directly on the spot, but active redness and itching should be gone.
Any significant symptoms persisting beyond 72 hours fall outside the normal window. This does not necessarily mean something dangerous is happening, but it does mean your body is responding more aggressively than typical and your healthcare provider should be aware.
For people who experience reactions that consistently last 3-4 days, your provider may recommend adjusting your dosing schedule or trying a different injection site area. Some individuals find that certain body regions produce longer-lasting reactions than others, which is another reason systematic injection rotation matters.
How to treat a red, itchy injection site
You know what is causing the reaction and you know it falls within normal parameters. Now you want it to stop itching. Here are the evidence-based approaches, ranked from simplest to most involved.
Immediate steps: cold compress
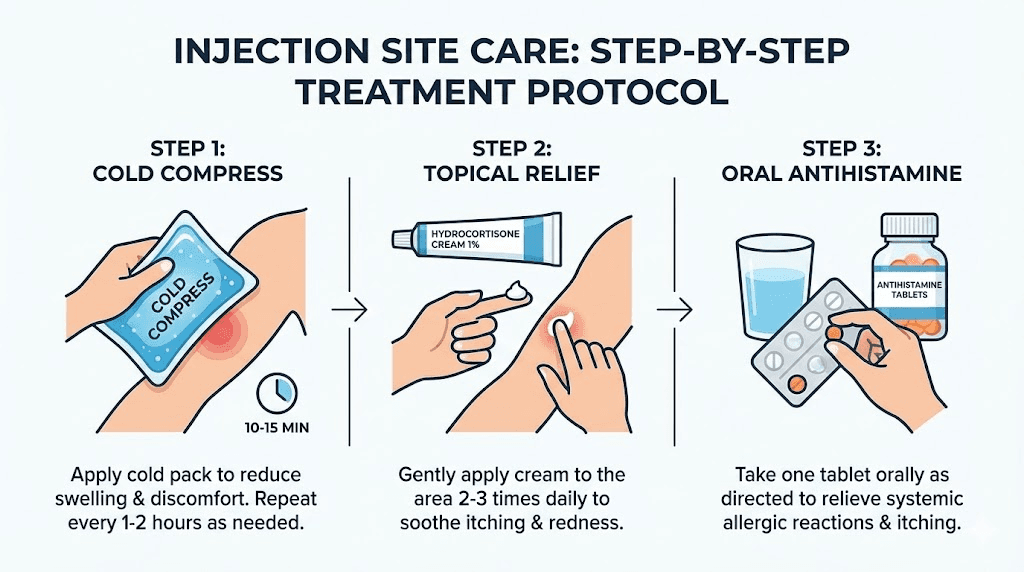
A clean, cool compress applied to the injection site for 10-15 minutes is the single most effective immediate intervention. Cold constricts blood vessels, reducing the blood flow that creates redness. It numbs local nerve endings, which decreases itching and pain. And it reduces the rate of histamine release from mast cells.
Use a clean cloth dampened with cool water, or wrap an ice pack in a thin towel. Do not apply ice directly to the skin, as this can cause cold burns and actually worsen inflammation. The goal is cool, not freezing.
You can repeat the cold compress application several times in the first few hours. Many experienced tirzepatide users make this a standard part of their injection routine, applying a compress for 10 minutes immediately after every injection regardless of whether a visible reaction has developed yet. This proactive approach often prevents the reaction from reaching its full potential intensity.
Over-the-counter options
Topical hydrocortisone cream (0.5-1%) applied sparingly to the reddened area reduces local inflammation and itching. Apply a thin layer to the affected area, not before injecting, and only to intact skin that is not broken or bleeding. Hydrocortisone works by suppressing the local immune response, which directly counteracts the histamine-driven inflammation.
Oral antihistamines provide systemic relief from the itching component. Non-drowsy options like cetirizine (Zyrtec) or loratadine (Claritin) are preferred for daytime use because they block histamine receptors without significant sedation. Diphenhydramine (Benadryl) is more potent for itching relief but causes drowsiness, making it a better choice for evening injections.
Some people find that taking an antihistamine 30-60 minutes before their injection significantly reduces the reaction intensity. If you consistently experience bothersome injection site reactions, this pretreatment approach is worth discussing with your healthcare provider.
Aloe vera gel provides a soothing, cooling effect without any anti-inflammatory medication. It is a reasonable option for people who prefer to avoid topical steroids or who want something gentle for very mild reactions.
What not to do
Do not scratch the area. This feels obvious, but it bears repeating because the urge can be intense. Scratching breaks the skin, introduces bacteria, amplifies inflammation through mechanical irritation, and extends the duration of the reaction. Cover the area with loose clothing if you find yourself unconsciously scratching.
Do not apply heat. Warm compresses dilate blood vessels and accelerate histamine release, which is the opposite of what you want. Save the heating pad for muscle aches from tirzepatide, not injection site reactions.
Do not apply topical hydrocortisone before injecting. The cream creates a barrier that can interfere with medication absorption and may trap bacteria against the puncture site.
Do not pop, squeeze, or lance any bumps that form. Injection site nodules are not pimples. They are localized deposits of medication and inflammatory cells that will resolve on their own. Attempting to drain them introduces infection risk and serves no useful purpose.
Do not apply rubbing alcohol after the injection. While cleaning the site with alcohol before injection is standard protocol, applying alcohol afterward stings, damages already-inflamed tissue, and delays healing.
Prevention strategies that actually work
Treating a reaction after it happens is fine. Preventing it from happening in the first place is better. These strategies are grounded in injection best practices validated across multiple GLP-1 receptor agonist clinical programs and refined by the practical experience of experienced users.
Systematic injection site rotation
Rotating injection sites is the single most impactful prevention strategy. When you inject into the same area repeatedly, the tissue becomes sensitized. Each subsequent injection into sensitized tissue triggers a progressively stronger inflammatory response. This is why some people report that their reactions "get worse over time" when the real issue is location repetition rather than medication sensitivity.
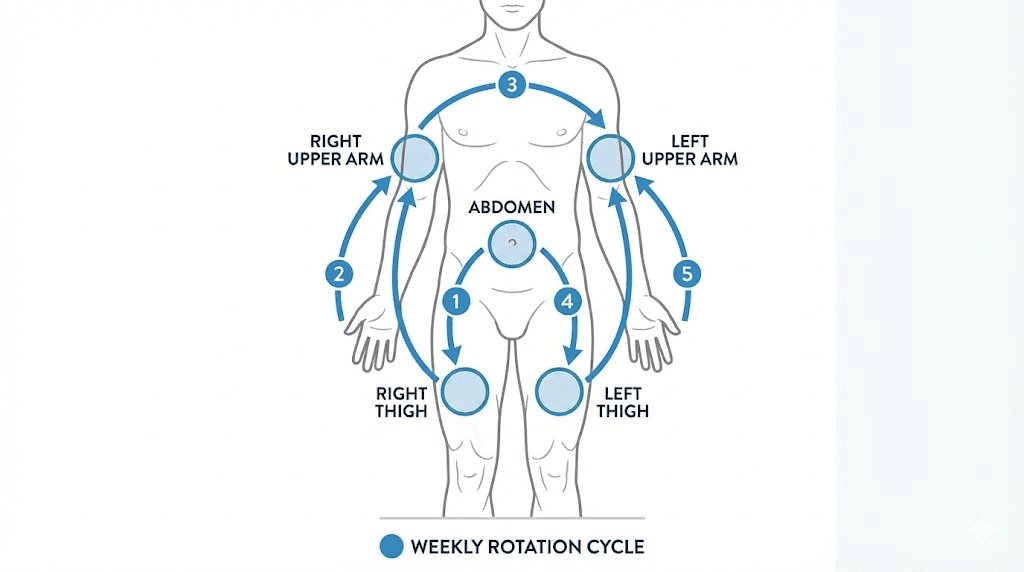
The three primary injection sites for subcutaneous tirzepatide are the abdomen (at least 2 inches from the navel), the front of the thighs, and the back of the upper arms. Establish a rotation system that moves between these three areas on a weekly basis. Within each area, never inject in exactly the same spot. Use a mental grid or tracking system to ensure each injection lands at least 1 inch away from any recent injection point.
A practical rotation schedule looks like this: Week 1 left abdomen, Week 2 right thigh, Week 3 left upper arm, Week 4 right abdomen, Week 5 left thigh, and so on. Some people keep a simple log in their phone noting the date and location. Others use a body map diagram. The specific tracking method does not matter as long as you are consistently rotating.
For detailed guidance on choosing the best injection site and understanding how different areas affect absorption, SeekPeptides provides comprehensive injection site guides that many users find helpful for establishing their rotation routine.
The room temperature rule
If your tirzepatide is stored in the refrigerator, remove it 15-30 minutes before injection to allow it to reach room temperature. Cold medication causes a temperature-shock response in the tissue. The body responds to this sudden cold by initially constricting blood vessels, followed by a rebound vasodilation that amplifies redness beyond what the histamine response alone would produce.
This is particularly relevant for compounded formulations stored in vials. If you are using refrigerated tirzepatide, gently roll the vial between your palms for 30 seconds after removing it from the fridge to warm it slightly. Do not shake the vial, as this can damage the peptide structure and reduce potency. Do not use a microwave or hot water to speed up warming, as excessive heat degrades tirzepatide.
Understanding proper peptide storage after reconstitution helps you maintain medication quality while also reducing injection site reactions. Temperature management is a factor that connects storage practices directly to injection comfort.
Proper injection technique step by step
Technique errors account for a surprising percentage of injection site reactions. Here is the correct process, refined for minimal tissue irritation.
Step 1: Clean the injection site. Use an alcohol swab in a circular motion, starting at the injection point and spiraling outward. Then wait. This step is critical. Allow the alcohol to dry completely before proceeding. Injecting through wet alcohol carries the alcohol into the tissue, where it acts as a chemical irritant and significantly amplifies burning, redness, and itching.
Step 2: Pinch the skin. With your non-dominant hand, gently pinch a fold of skin between your thumb and index finger. This lifts the subcutaneous fat away from the underlying muscle, ensuring the injection reaches the correct tissue depth. If you are using a syringe for your tirzepatide, the pinch technique is especially important for accurate placement.
Step 3: Insert the needle. Push the needle in at a 90-degree angle to the skin surface. A straight insertion creates a clean channel that heals quickly. Angled insertions create longer wound tracks that take more time to close and may leak medication back toward the skin surface, increasing irritation.
Step 4: Inject slowly. Depress the plunger steadily over 5-10 seconds. Rapid injection creates a sudden pressure wave in the subcutaneous tissue that damages cells and triggers a more aggressive inflammatory response. Slow, steady pressure allows the medication to distribute evenly without tissue trauma.
Step 5: Pause before withdrawing. After the plunger is fully depressed, hold the needle in place for 5-10 seconds. This allows the medication to begin dispersing and reduces the amount that leaks back through the needle track when you withdraw. Medication leaking onto the skin surface is a common cause of localized irritation.
Step 6: Release and cover. Withdraw the needle straight out. Do not rub the injection site. Apply gentle pressure with a clean cotton ball or gauze pad if there is any bleeding. Then leave the area alone.
Following this technique consistently when you give yourself subcutaneous injections of any GLP-1 medication dramatically reduces the mechanical component of injection site reactions.
Skin preparation dos and do nots
Beyond the alcohol cleaning step, several skin preparation factors influence reaction severity.
Do make sure your skin is clean and dry before injection. Sweat, lotion, sunscreen, or other products on the skin surface can be carried into the tissue by the needle and cause irritation.
Do avoid injecting into areas with existing skin irritation, sunburn, rashes, bruises, or scars. Compromised skin mounts a stronger inflammatory response to the additional trauma of an injection.
Do not apply numbing creams or ice before injection unless specifically recommended by your provider. While the intent is to reduce pain, these products can alter blood flow and medication absorption in unpredictable ways.
Do wear loose-fitting clothing over the injection site after your dose. Tight waistbands, compression garments, and friction from clothing can mechanically irritate the injection site and worsen both redness and itching. This is a simple adjustment that many people overlook.
Do reactions get worse with higher doses
Dose escalation is a standard part of tirzepatide therapy. You start low and gradually increase to find your effective dose. A natural question is whether higher doses mean worse injection site reactions.
Dose escalation and skin sensitivity
The relationship between dose and injection site reactions is not as straightforward as you might expect. Higher doses mean more active ingredient being deposited into the subcutaneous tissue, which theoretically provides more substrate for the immune system to react to. But clinical data shows that the correlation is modest at best.
In the SURPASS and SURMOUNT clinical trial programs, injection site reaction rates were reported at approximately 1.7-5.2% for Mounjaro and 2.4-5.3% for Zepbound across different dose levels. The range varies, but the increase from lowest to highest dose is not dramatic. Some participants actually reported fewer reactions at higher doses, possibly because their immune system had adapted to the medication over the months of dose escalation.
What does change with higher doses is the volume of injection for compounded formulations. If you are using a compounded tirzepatide formulation that requires you to inject a larger volume at higher doses, the physical distension of the subcutaneous tissue from the larger fluid volume can increase mechanical irritation independent of any immune response.
For this reason, many providers recommend using the highest available concentration so that the injection volume stays small even at higher doses. If you are calculating your tirzepatide dosage in units, understanding the relationship between concentration, volume, and injection comfort becomes important. Our peptide calculator can help you determine the exact volume for your specific concentration.
What clinical trials show
The SURPASS clinical trial data provides the most comprehensive look at injection site reactions across the tirzepatide dose range. Across all six SURPASS trials enrolling over 7,500 participants, injection site reactions were categorized as "common" (affecting up to 1 in 10 people) but were rarely severe enough to cause treatment discontinuation.
This is an important finding. It means that even when reactions occur, they are manageable enough that the vast majority of patients continue therapy. The benefit-to-inconvenience ratio strongly favors continuing treatment with appropriate management strategies rather than stopping tirzepatide due to skin reactions alone.
If you are tracking your progress using tools like the GLP-1 plotter and noticing that injection site reactions coincide with dose increases, note the pattern but do not assume it will persist. Most users find that reactions at a new dose level diminish over 2-4 weeks as the body adjusts, following the same adaptation pattern seen at the starting dose. For a broader view of how tirzepatide works over time, this initial adjustment period is a small chapter in a much longer story.
Compounded tirzepatide vs brand-name formulations
The source of your tirzepatide can influence injection site reaction rates. This is not about the tirzepatide molecule itself, which is identical regardless of source. It is about everything else in the vial or pen.
Why compounded versions may cause more reactions
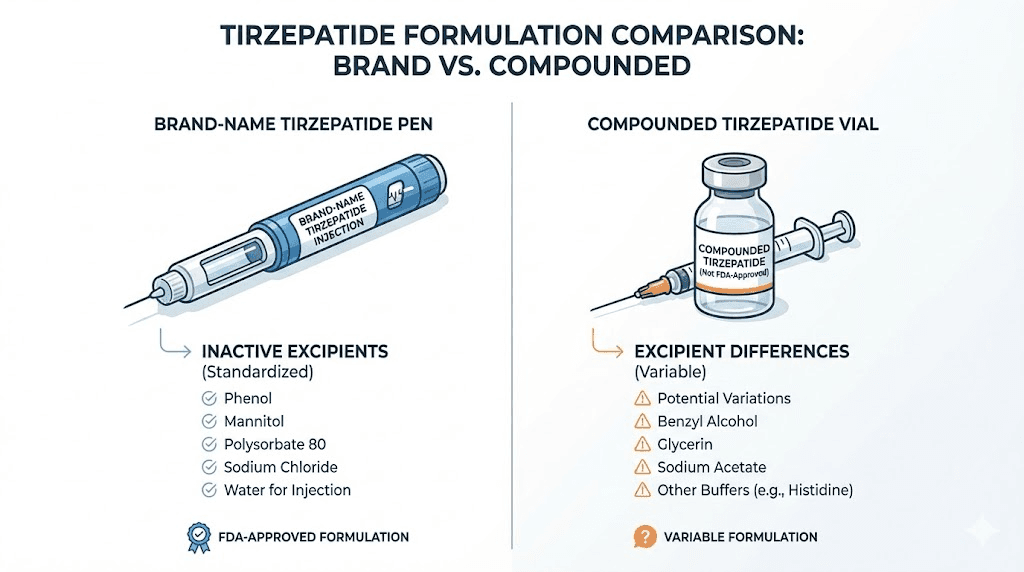
Compounded tirzepatide formulations often differ from brand-name products in several ways that directly affect injection site tolerability. The excipient profiles may differ, with different preservatives, buffers, and stabilizers that the skin has not been exposed to before. The pH may vary slightly from the precisely calibrated brand-name formulation. And the manufacturing conditions, while regulated by state pharmacy boards, do not undergo the same FDA-mandated quality control testing as brand-name products.
Some compounded formulations include additional compounds marketed as enhancers. Tirzepatide with B12, tirzepatide with glycine, and tirzepatide with niacinamide are common compound combinations. Each additional ingredient introduces another potential irritant. If you switched from plain tirzepatide to a combination product and noticed more injection site reactions, the additive is the most likely explanation, not the tirzepatide.
It is worth noting that multi-ingredient tirzepatide compounds can be beneficial for many people. Glycine and B12 each have documented benefits. But if injection site irritation is a concern, switching to a simpler formulation without additives may help you isolate whether the tirzepatide or the extras are responsible for your skin reactions.
Additives and excipients to watch for
If you are using a compounded formulation and experiencing persistent injection site reactions, ask your compounding pharmacy for the complete excipient list. Specific compounds known to cause skin irritation include:
Benzyl alcohol is a preservative commonly used in multi-dose vials. It is a well-documented skin irritant that causes burning and redness in a significant percentage of people. Single-use vials or products preserved with alternatives may be better tolerated.
Sodium phosphate buffers can cause localized stinging and redness, particularly at higher concentrations. The pH of the solution directly affects tissue comfort, and sodium phosphate at certain concentrations pushes the pH outside the comfortable range.
Niacinamide (vitamin B3) at higher concentrations can cause flushing, redness, and itching. If you are using a tirzepatide methylcobalamin combination, the methylcobalamin itself is generally well-tolerated, but any accompanying niacinamide may be contributing to your skin reactions.
Understanding the differences between compounded formulations and brand-name products helps you make informed decisions about which version works best for your body. SeekPeptides members access detailed formulation comparisons that break down exactly what is in different tirzepatide products and how each ingredient may affect tolerability.
Injection site lumps, welts, and other variations
Redness and itching are the most common injection site reactions, but they are not the only ones. Understanding the full spectrum of possible reactions helps you identify what you are experiencing and respond appropriately.
Hard lumps or nodules
Small, firm lumps beneath the skin at the injection site are commonly reported by tirzepatide users. These nodules represent localized deposits of medication that are being slowly absorbed, sometimes combined with a small inflammatory pocket. They typically feel like a firm marble or pea-sized bump under the skin.
Most injection site nodules are painless or mildly tender. They resolve on their own within 3-7 days as the body absorbs the medication depot. The abdomen tends to produce fewer nodules than the thighs for most people, likely because the abdominal subcutaneous fat provides more space for the medication to disperse.
Injection speed is the primary modifiable factor. Injecting too quickly forces the medication into a tight bolus rather than allowing it to spread naturally through the tissue. If you consistently develop lumps, try extending your injection time to 10-15 seconds and ensure you are using the appropriate needle depth for your injection site. Injection pen devices typically deliver medication at a controlled rate that minimizes this problem.
Bruising and swelling
Bruising at the injection site occurs when the needle nicks a small blood vessel during insertion. This is largely unavoidable, as subcutaneous tissue contains a dense network of capillaries that cannot be visualized through the skin. Bruising does not indicate a problem with the medication or the injection technique. It is simply bad luck with needle placement.
If you bruise easily or are taking blood-thinning medications or supplements that affect blood clotting, you may experience more frequent injection site bruising. Fish oil, vitamin E, and certain herbal supplements can increase bruising tendency. This does not mean you need to stop those supplements, but it does explain why some injection sites bruise while others do not.
Swelling that extends significantly beyond the injection site, or swelling that continues increasing in size over hours, falls outside the normal pattern and should prompt a call to your provider.
Hives beyond the injection site
Localized hives (urticaria) at the injection site represent a stronger-than-average histamine response but are still generally manageable with the treatments described above. However, hives that appear on skin areas away from the injection site indicate a systemic allergic response.
If you develop hives on your torso after injecting in your thigh, or on your arms after injecting in your abdomen, your body is mounting a systemic reaction to the medication itself rather than a localized response to the injection process. This warrants immediate contact with your healthcare provider and likely indicates that continuing tirzepatide in its current form is not safe for you.
Systemic hives accompanied by other GLP-1 side effects like difficulty breathing, dizziness, or throat tightness constitutes a medical emergency. Call emergency services immediately. Do not wait to see if the symptoms resolve on their own.
When to talk to your healthcare provider
Most injection site reactions are manageable at home. But knowing exactly when to escalate saves both time and worry.
Red flags that need medical attention
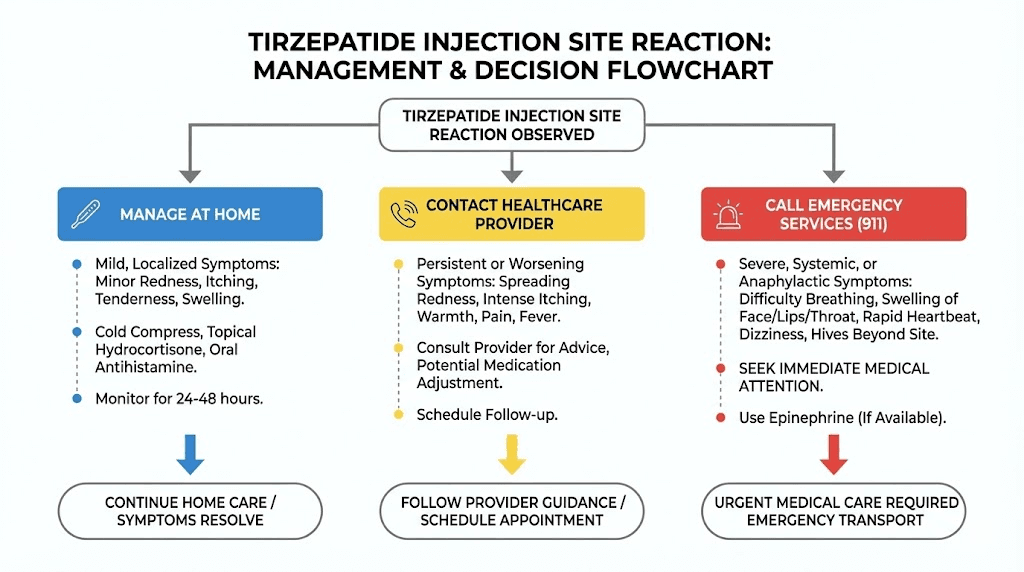
Contact your healthcare provider (not emergency services) if you experience any of the following. Redness that spreads beyond 2 inches from the injection site. Swelling that increases in size over 24 hours. Pain that worsens rather than improves over time. Warmth and redness that persist beyond 72 hours. A red streak extending outward from the injection site, which may indicate lymphangitis. Any pus, drainage, or oozing from the injection site.
Call emergency services immediately for difficulty breathing or shortness of breath. Swelling of the face, lips, tongue, or throat. Widespread hives covering large areas of the body. Feeling faint, dizzy, or losing consciousness. Rapid heartbeat accompanied by other symptoms. A sense of impending doom, which is a recognized symptom of anaphylaxis.
These emergency symptoms are rare. The published case literature includes only a small number of reports of anaphylaxis with tirzepatide. But rare does not mean impossible, and being prepared to recognize the signs could be lifesaving.
What to tell your doctor
When you contact your provider about an injection site reaction, having specific information ready makes the conversation more productive. Note when the injection was given and which site you used. Describe the timeline, specifically when symptoms started and how they have progressed. Measure the size of the reddened area and note whether it is growing or stable. Take a photo if possible. Report any systemic symptoms. And mention any recent changes to your protocol, including dose changes, switching formulations, or switching between medications.
This information helps your provider distinguish between a normal reaction, a localized allergic response, a possible infection, and a systemic reaction, each of which has a different management approach.
Will you need to stop tirzepatide
In most cases, no. The vast majority of injection site reactions do not require treatment discontinuation. Your provider may recommend adjusting your injection technique, switching injection sites, trying a different formulation, or adding pretreatment with an antihistamine.
Treatment discontinuation is typically only necessary when there is a documented systemic allergic reaction or when injection site reactions are so severe and persistent that they significantly impact quality of life despite all management measures. Even in cases where brand-name tirzepatide causes reactions, some patients tolerate a different formulation or a different GLP-1 medication like semaglutide.
If you and your provider decide that injectable tirzepatide is not suitable, there are alternative delivery methods worth discussing. Oral tirzepatide options, tirzepatide drops, and tablet formulations eliminate the injection component entirely, which removes the injection site reaction problem at its source.
How injection site reactions compare to other side effects
Injection site redness and itching, while annoying, sits near the mild end of the tirzepatide side effect spectrum. Putting it in context helps you understand where your concern should actually focus.
The most commonly reported tirzepatide side effects are gastrointestinal. Nausea, diarrhea, and constipation affect a much larger percentage of users than injection site reactions. These GI effects typically improve with time and proper dose titration, but they tend to be more disruptive to daily life than a red, itchy spot on the skin.
Fatigue and headaches are also more common than injection site reactions. Sleep disruption, anxiety, and joint pain are less common but still reported. The muscle pain some users experience tends to be more bothersome than injection site irritation for most people.
The broader GLP-1 side effect profile includes issues like hair thinning and persistent headaches that concern many users. Compared to these systemic side effects, a temporary red spot at the injection site is generally considered minor. The key word is temporary. If your injection site reactions resolve within the expected timeframe and respond to basic management, they represent one of the most manageable aspects of tirzepatide therapy.
For a comprehensive comparison of side effects between the two most popular GLP-1 medications, our semaglutide versus tirzepatide comparison page breaks down the differences in detail.
Real user experiences and what they learned
Clinical trial data tells one story. Real-world experience tells another. Both matter.
Forum discussions and patient communities consistently reveal several practical insights about injection site reactions that clinical trials do not capture in their standardized reporting.
The abdomen is generally the most forgiving injection site for minimizing reactions. Multiple users report that thigh injections produce larger, longer-lasting red marks compared to abdominal injections, likely because the thigh has less subcutaneous fat and more sensory nerve density in many people. Upper arm injections fall somewhere in between but are harder to self-administer without help.
Time of day matters more than most guides mention. Users who inject in the evening report that the reaction peaks overnight while they sleep, and by morning the worst has passed. Those who inject in the morning spend the most reactive hours during their workday, which makes the itching more noticeable and harder to manage.
Hydration status appears to influence reaction severity in some individuals. Several community reports suggest that injection site reactions are worse when the person is dehydrated, which makes physiological sense because dehydration concentrates the immune response and reduces the tissue volume available for medication dispersion.
Alcohol consumption within 24 hours of injection may amplify reactions for some people. Alcohol is a vasodilator, which can enhance the redness and warmth component of the reaction. This is worth noting if you are wondering about drinking while on tirzepatide.
Many long-term users report that their injection site reactions diminished significantly after the first 4-8 weeks of treatment. The body appears to develop tolerance to the formulation over time, which aligns with the immunological concept of desensitization through repeated low-level exposure. Users who have been on tirzepatide for several months and tracking their weight loss progress rarely cite injection site reactions as an ongoing concern.
Additional factors that influence injection site reactions
Several factors that rarely get discussed can meaningfully affect whether you develop redness and itching after your tirzepatide injection.
Skin type and sensitivity
People with sensitive skin, eczema, rosacea, or other dermatological conditions tend to experience more pronounced injection site reactions. Their skin barrier is already compromised and their mast cells are often in a heightened state of reactivity. If you have sensitive skin, you may benefit from applying a fragrance-free, hypoallergenic moisturizer to potential injection sites in the days between injections to maintain skin barrier integrity.
For people dealing with skin conditions alongside their tirzepatide therapy, coordinating with a dermatologist about injection site management can be valuable. They can recommend specific topical products that support skin healing without interfering with medication absorption.
Stress and immune activation
Cortisol and other stress hormones modulate mast cell reactivity. During periods of high stress, your immune system operates at a heightened baseline, which can amplify the histamine response to an injection. If you notice that your injection site reactions are worse during stressful periods, this physiological connection may be the explanation.
This is not a reason to delay or skip injections during stress. It is simply helpful context for understanding why your reactions vary from week to week even when nothing about your injection technique or site has changed.
Medications that affect histamine response
Certain medications amplify the histamine pathway and can worsen injection site reactions. NSAIDs like ibuprofen, while generally safe to use alongside tirzepatide, can affect the inflammatory cascade in complex ways. If you are taking phentermine alongside tirzepatide or other medications, discuss potential interactions with your pharmacist.
Conversely, people already taking daily antihistamines for allergies often report minimal injection site reactions. Their baseline histamine activity is suppressed, which dampens the local immune response at the injection site.
Menstrual cycle influence
Some female users report that injection site reactions are more prominent during certain phases of their menstrual cycle, particularly the premenstrual phase when histamine levels naturally rise. If you notice a pattern of worse reactions at consistent points in your cycle, timing your injection to avoid the highest-histamine phase may help. For more on how tirzepatide affects the menstrual cycle, understanding these hormonal interactions adds useful context.
Building your personal injection site management protocol
Everyone responds differently to tirzepatide. A cookie-cutter approach to injection site management is less effective than a personalized protocol developed through systematic observation of your own responses.
Start by tracking your reactions for the first 4-6 injections. Note the injection site, technique details, medication temperature, time of day, reaction onset time, peak intensity, duration, and size of the reddened area. After several data points, patterns emerge that are unique to your body.
Then build your protocol based on what you observe. If your thigh injections consistently produce worse reactions than abdominal injections, weight your rotation schedule toward the abdomen. If evening injections produce less noticeable reactions than morning ones, shift your injection time. If pretreatment with an antihistamine eliminates the itching, make it a standing part of your routine.
This evidence-based, personalized approach is far more effective than generically following tips from the internet. SeekPeptides members often share their personal protocols and track their reactions over time, building a collective knowledge base that helps new users optimize their approach faster than they could alone.
Using tools like the peptide reconstitution calculator ensures your medication is mixed at the proper concentration, which affects injection volume and, by extension, injection site comfort. Getting the bacteriostatic water ratios right for tirzepatide is a detail that directly connects formulation accuracy to injection site tolerability.
The bigger picture: injection site reactions in context
If you have read this far, you know more about tirzepatide injection site reactions than 99% of users. But perspective matters too.
Injection site redness and itching is, in the vast majority of cases, a minor and temporary inconvenience in the context of a medication that is producing meaningful health improvements. People using tirzepatide are typically pursuing significant weight loss goals, metabolic health improvements, or better glucose control. A temporary red spot that lasts a day or two is a small price for those outcomes.
The people who struggle most with injection site reactions are often those who lack the information to distinguish normal from concerning. Armed with the knowledge in this guide, you can confidently manage normal reactions at home, recognize warning signs that need professional attention, and implement prevention strategies that minimize reactions over time.
Your body is not rejecting the medication. It is acknowledging its presence. That is what immune systems do. The inflammation, the redness, the itching, these are all signs that your tissue is alive, responsive, and processing the medication exactly as intended.
For researchers serious about optimizing their peptide protocols, SeekPeptides offers the most comprehensive resource available, with evidence-based guides, proven protocols, and a community of thousands who have navigated these exact questions.
Frequently asked questions
Is it normal for tirzepatide injection sites to be red and itchy every time?
Yes, some people experience mild redness and itching with every injection. This is a consistent histamine response and is considered normal as long as the reaction stays localized, mild, and resolves within 2-3 days. Proper injection technique and site rotation can reduce the severity but may not eliminate the reaction entirely for some individuals.
Can I use hydrocortisone cream before my tirzepatide injection?
No. Apply hydrocortisone only after the injection, and only to the irritated area. Applying cream before injection creates a barrier that can interfere with medication absorption and may trap bacteria at the injection site. Wait until the reaction develops, then apply a thin layer of 0.5-1% hydrocortisone to the reddened area.
Should I take Benadryl before every tirzepatide injection?
This depends on the severity and consistency of your reactions. If you experience bothersome itching with every injection, taking an antihistamine 30-60 minutes before your dose can significantly reduce the reaction. Discuss this approach with your healthcare provider to ensure it is appropriate for your specific situation and does not interact with your other medications or supplements.
Does the injection site reaction mean I am allergic to tirzepatide?
Not necessarily. A localized injection site reaction (redness, mild itching, slight swelling that resolves in 2-3 days) is a histamine response to the injection process, not necessarily an allergy to the medication. A true allergic reaction involves systemic symptoms: widespread hives, breathing difficulty, facial swelling, or other symptoms beyond the injection site. If you are unsure, your provider can help distinguish between a normal reaction and an allergy.
Will my injection site reactions get better over time?
Most users report that injection site reactions diminish over the first 4-8 weeks of treatment. The body appears to develop tolerance through repeated exposure. If your reactions are getting worse over time rather than better, this is unusual and worth discussing with your provider. It may indicate sensitization to a specific excipient in your formulation.
Can switching injection sites help reduce redness and itching?
Absolutely. Different body areas have different densities of mast cells and nerve endings. Many users find that abdominal injections produce less redness than thigh injections. Rotating between the abdomen, thighs, and upper arms, and never injecting in the same exact spot twice in a row, is one of the most effective strategies for reducing injection site irritation.
Is the red, itchy reaction worse with compounded tirzepatide?
It can be. Compounded formulations may contain different excipients, preservatives, or additives that trigger more skin irritation than brand-name products. If you are using a compound with added ingredients like B12 or glycine, the additive may be causing the extra irritation rather than the tirzepatide itself. Trying a simpler formulation without additives can help isolate the cause.
How big should the red area be before I worry?
A normal injection site reaction typically produces a red area of 1-2 inches in diameter. If the redness extends beyond 2 inches, is expanding visibly over time, or is accompanied by increasing pain or warmth, contact your healthcare provider. Also seek attention if the area develops a red streak extending outward, which could indicate a developing infection.
External resources
PMC: Tirzepatide-induced injection site reaction case report
American Academy of Allergy, Asthma and Immunology: Suspected hypersensitivity to tirzepatide
ScienceDirect: Tirzepatide in dermatology comprehensive review
In case I do not see you, good afternoon, good evening, and good night. May your injection sites stay calm, your reactions stay mild, and your results stay consistent.