Mar 5, 2026

Some semaglutide users breeze through their first months with barely a stomach gurgle. Others spend weeks battling nausea, bloating, constipation, and the kind of gastrointestinal distress that makes them question whether the weight loss is worth it. The difference is not always genetic. It is not always about dose titration speed or injection technique. Often, the dividing line between a smooth semaglutide experience and a miserable one comes down to something deceptively simple: gut health.
Probiotics have become one of the most discussed supplements in GLP-1 communities, and for good reason. When semaglutide slows gastric emptying and reshapes the bacterial landscape inside your intestines, the right probiotic strains can mean the difference between tolerating your medication and dreading injection day. But not all probiotics are created equal. The generic drugstore blend sitting on your shelf right now may do absolutely nothing for the specific disruptions semaglutide causes. Worse, the wrong strains might aggravate the very symptoms you are trying to fix.
This guide breaks down exactly which probiotic strains the research supports for semaglutide users, which products deliver those strains in effective doses, and how to time everything for maximum benefit. Whether you are dealing with semaglutide constipation, persistent bloating, or the dreaded sulfur burps, there is a targeted approach that goes far beyond "just take a probiotic." SeekPeptides members already know that optimizing every aspect of a peptide protocol matters, and probiotic selection is no exception.
Why semaglutide changes your gut microbiome
Semaglutide does not just suppress appetite. It fundamentally alters the environment inside your gastrointestinal tract, and that environment is home to trillions of bacteria that influence everything from digestion to immune function to mood. Understanding these changes is the first step toward choosing the right probiotic support. Resources like the peptides and semaglutide overview cover the foundational science behind GLP-1 receptor agonists.
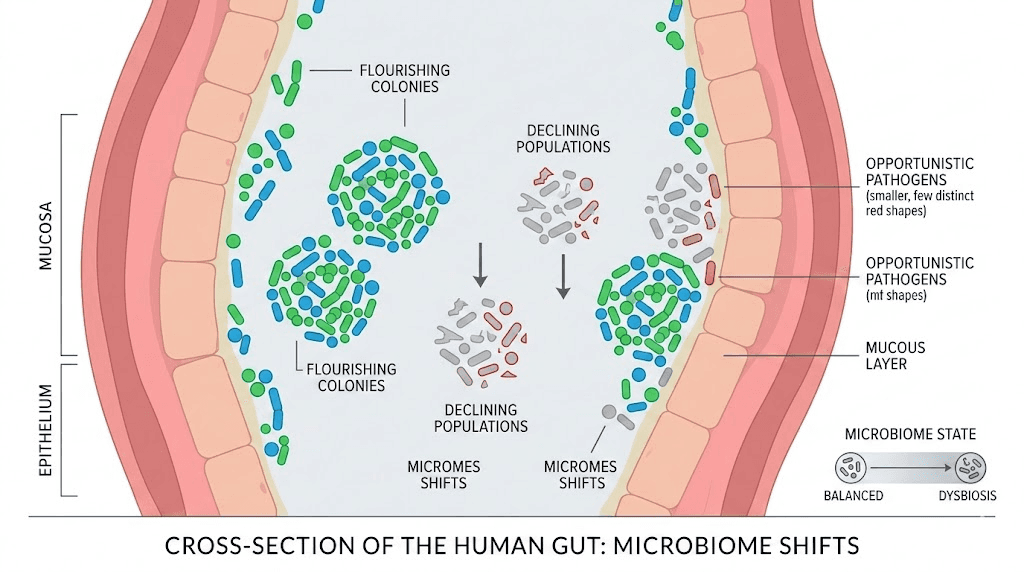
The primary mechanism is gastric emptying delay. Semaglutide activates GLP-1 receptors in the brain and gut, which slows the rate at which food moves from the stomach into the small intestine. This is partly how the drug reduces appetite and helps with weight loss. But slower transit time means food sits in the stomach and upper intestines longer than usual. Bacteria that thrive in these extended fermentation conditions begin to flourish. Others that depend on regular motility decline.
Research on GLP-1 receptor agonists and the gut microbiome reveals several consistent patterns. Akkermansia muciniphila, a beneficial bacterium that strengthens the gut lining, tends to increase during semaglutide treatment. This is actually a positive shift. However, overall bacterial diversity often decreases, which can leave the gut more vulnerable to opportunistic organisms and less resilient to dietary changes.
One study on Chinese patients with type 2 diabetes found that semaglutide treatment shifted Bifidobacterium abundance from 10.38% to 17.98%, a significant increase in a genus known for supporting digestive health. But these shifts do not happen uniformly. Your individual response depends on your baseline microbiome composition, your diet, your dosage, and how quickly you titrated up. Proper titration is important, and our semaglutide dosage chart in units provides the standard schedules.
The GI side effects that plague so many semaglutide users, the nausea, the bloating, the constipation, the diarrhea, are not random bad luck. They are downstream consequences of these microbiome shifts combined with delayed gastric motility. When the bacterial balance tips in the wrong direction, gas production increases, gut barrier function weakens, and inflammatory signaling ramps up. That is why a targeted probiotic approach can make such a meaningful difference. You are not just masking symptoms. You are addressing the underlying microbial disruption that causes them.
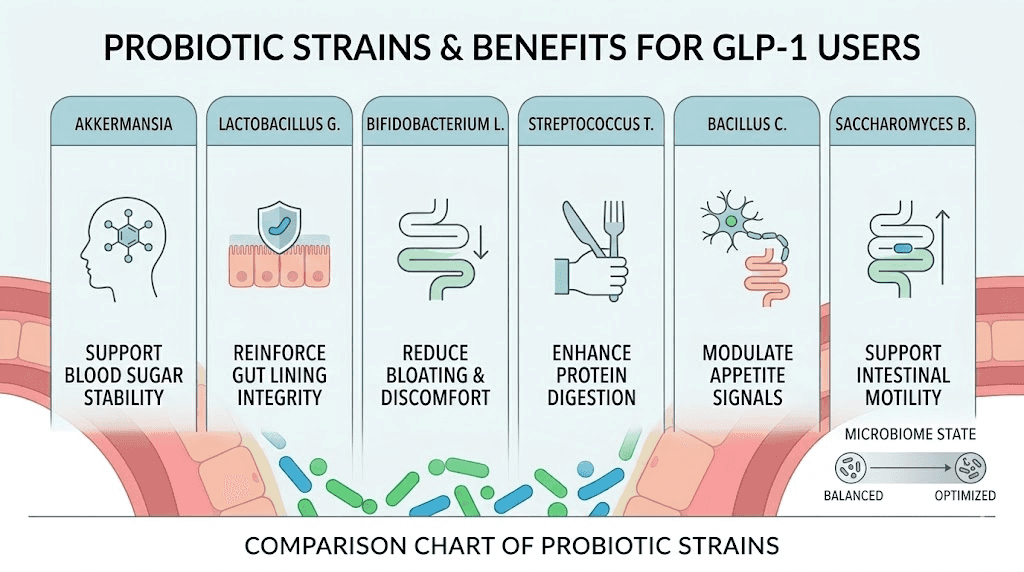
The six best probiotic strains for semaglutide users
Not every probiotic strain addresses the specific disruptions semaglutide causes. The six strains below have the strongest evidence base for supporting gut health during GLP-1 therapy. Some directly enhance GLP-1 signaling. Others target the exact side effects that drive people to quit their medication. Understanding what each strain does, and at what dose, allows you to build a targeted protocol rather than guessing with a generic blend.
Lactobacillus reuteri
This is the single most relevant probiotic strain for semaglutide users, and the research explains why. A study by Simon et al. published in Diabetes Care examined 21 participants who supplemented with Lactobacillus reuteri SD5865 for four weeks. The results were striking. Participants showed 76% higher GLP-1 release and 49% higher insulin secretion compared to placebo.
Think about what that means in practice. Semaglutide works by mimicking GLP-1. A probiotic that naturally amplifies your own GLP-1 production could enhance the effects of the medication you are already taking. This is not a replacement for semaglutide. For those tracking their before and after semaglutide results, it is a complement that may help you achieve better results at the same dose, or maintain results as you eventually taper down.
L. reuteri also produces antimicrobial compounds called reuterin that help keep pathogenic bacteria in check. For semaglutide users whose slowed gut motility creates favorable conditions for harmful organisms, this protective effect matters. The recommended dose is 10 billion CFU daily, taken consistently for at least four weeks to see measurable changes. You can find L. reuteri in fermented foods like certain yogurts, but supplemental forms deliver more reliable and therapeutic doses. Understanding the fundamentals of peptide and supplement protocols helps frame why consistency matters so much.
If you are using our semaglutide dosage calculator to optimize your medication dose, consider L. reuteri the probiotic equivalent of fine-tuning. It works with your GLP-1 therapy rather than around it.
Akkermansia muciniphila
Akkermansia is having a moment, and the science backs the hype. This bacterium lives in the mucus layer of your intestinal lining, where it performs a critical job: maintaining gut barrier integrity. When Akkermansia populations are healthy, the gut wall stays strong. When they decline, intestinal permeability increases, leading to inflammation, immune dysregulation, and worsened GI symptoms.
Here is where it gets interesting for semaglutide users. Akkermansia muciniphila secretes a protein called P9 that directly stimulates GLP-1 production from intestinal L-cells. This creates a positive feedback loop. More Akkermansia means more P9 protein, which means more natural GLP-1 signaling, which supports the very mechanism your medication relies on.
Animal studies show that semaglutide itself tends to increase Akkermansia populations. So you might wonder why supplementation matters. The answer is timing and magnitude. Supplementing with Akkermansia from the start of your semaglutide journey may help establish robust populations faster than waiting for the drug to shift your microbiome gradually. For people who experience significant early side effects, that head start can mean fewer weeks of discomfort.
Akkermansia is notoriously difficult to deliver in supplement form because it is an anaerobic organism that dies on exposure to oxygen. Pasteurized (heat-killed) forms have shown benefits in human trials, and products like the Pendulum GLP-1 Probiotic use proprietary encapsulation to deliver viable organisms. This is one strain where product quality makes an enormous difference.
Bifidobacterium lactis
Constipation is the most common GI complaint among semaglutide users, and Bifidobacterium lactis is the most studied probiotic strain for addressing it. Two specific sub-strains stand out: BB-12 and HN019.
Multiple clinical trials demonstrate that B. lactis BB-12 improves stool frequency and consistency in constipated adults. The mechanism involves several pathways. B. lactis produces short-chain fatty acids that stimulate intestinal motility, lowers colonic pH to create a more favorable environment for beneficial bacteria, and enhances mucus production that lubricates the intestinal tract.
For semaglutide users specifically, the constipation problem is compounded by delayed gastric emptying. Food moves more slowly through the entire GI tract, and the colon absorbs more water from stool as it sits there longer. B. lactis helps counteract both issues. It promotes the peristaltic contractions that move material through the intestines while simultaneously improving stool hydration.
The effective dose in most studies ranges from 1 to 10 billion CFU daily. Higher doses are not necessarily better, especially when starting out. If you are already experiencing constipation on semaglutide, begin with a moderate dose and increase gradually over two weeks. Sudden high-dose probiotic introduction can temporarily worsen bloating and gas as your gut flora adjusts. Users managing their semaglutide diet plan should pair this strain with adequate fiber and hydration for best results.
Saccharomyces boulardii
This one is different. Saccharomyces boulardii is not a bacterium at all. It is a yeast.
That distinction matters enormously for semaglutide users, because S. boulardii is uniquely resistant to antibiotics and does not compete with bacterial probiotics for the same ecological niches. It works through entirely different mechanisms, which means you can take it alongside bacterial strains without interference.
S. boulardii is the most evidence-backed probiotic for diarrhea management, period. Meta-analyses covering thousands of patients show significant reductions in both the duration and severity of diarrhea across multiple causes: antibiotic-associated, infectious, and medication-induced. For the subset of semaglutide users who experience diarrhea rather than constipation, especially during the first week on semaglutide or after dose increases, S. boulardii offers rapid relief. Users wondering why they are not losing weight on semaglutide should also consider that persistent diarrhea can impair nutrient absorption and metabolic efficiency.
The yeast also produces enzymes that break down bacterial toxins in the gut, strengthens tight junctions between intestinal cells, and modulates the immune response in the gut wall. These anti-inflammatory effects can help with the generalized GI irritation that many semaglutide users describe as a vague, persistent abdominal discomfort that does not fit neatly into the categories of nausea, bloating, or diarrhea.
Standard dosing is 250 to 500 mg daily, typically containing 5 to 10 billion CFU. Because it is a yeast, it survives stomach acid well and does not require refrigeration, making it one of the most convenient probiotics to add to your routine. For more on supplements to take with GLP-1 medications, our tirzepatide supplement guide covers overlapping recommendations.
Lactobacillus rhamnosus GG
LGG, as it is commonly known, is one of the most extensively studied probiotic strains in existence, with over 1,000 published studies to its name. Its primary strengths lie in immune support and diarrhea management, but it offers broader benefits that are relevant to the semaglutide experience.
LGG adheres strongly to the intestinal wall, forming a protective barrier that prevents pathogenic bacteria from attaching. This colonization resistance is particularly valuable when semaglutide-induced changes in gut motility create opportunities for less desirable organisms to gain a foothold. By occupying attachment sites along the intestinal lining, LGG essentially blocks the competition.
For diarrhea specifically, LGG has shown efficacy in both prevention and treatment across dozens of clinical trials. It reduces intestinal inflammation, modulates water and electrolyte transport in the gut, and helps normalize stool consistency. Semaglutide users who alternate between constipation and diarrhea, a surprisingly common pattern, may find LGG helpful for stabilizing bowel function in either direction.
The immune support aspect should not be overlooked either. Semaglutide has been shown to have immunomodulatory effects, and some users report increased susceptibility to minor infections during treatment, possibly related to microbiome disruption. LGG stimulates the production of secretory IgA, an antibody that plays a frontline defense role in the gut and respiratory tract. This support becomes especially relevant for users who are also experiencing fatigue on semaglutide, which can sometimes indicate immune system strain. Typical dosing is 10 billion CFU daily, and it pairs well with Bifidobacterium strains in combination formulas. For users also experiencing GLP-1 headaches, immune support from LGG may help address the systemic inflammation that sometimes contributes to headache frequency.
Bifidobacterium longum
Gas. Bloating. That uncomfortable fullness that lingers for hours after eating even a small meal. These are the complaints that Bifidobacterium longum addresses most directly.
B. longum is one of the first bacterial species to colonize the human gut at birth, and it remains one of the most important throughout life. It ferments complex carbohydrates into short-chain fatty acids, particularly acetate and lactate, which serve as fuel for other beneficial bacteria and for the cells lining the colon. This cross-feeding network is essential for a balanced microbiome.
What makes B. longum particularly relevant for semaglutide users is its ability to reduce gas production. When semaglutide slows gut transit, undigested food spends more time being fermented by gut bacteria. Some bacteria produce excessive hydrogen and methane gas during this process. B. longum helps shift the fermentation profile toward less gas-producing pathways, which directly reduces the bloating and distension that so many GLP-1 users experience.
Clinical studies show that B. longum supplementation reduces both subjective bloating scores and objective measures of abdominal distension. For semaglutide users who list bloating as their primary complaint, this strain deserves priority. It also produces B vitamins and helps with the absorption of minerals like calcium, iron, and magnesium, nutrients that can become depleted when appetite suppression leads to reduced food intake. Users concerned about energy levels during caloric restriction should also review the semaglutide and energy guide.
Effective doses range from 1 to 10 billion CFU daily. B. longum is widely available in multi-strain formulas and as a standalone supplement. It is stable in both refrigerated and shelf-stable formulations, though refrigerated products generally deliver higher viable counts.
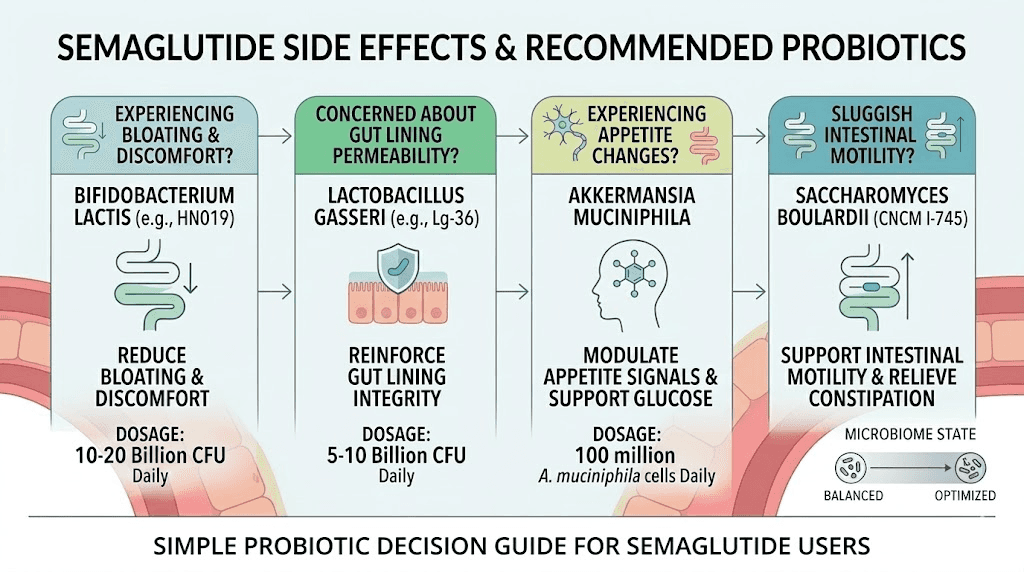
Matching probiotics to your specific side effects
Knowing the six best strains is useful. Knowing which ones to take for your specific situation is what actually solves the problem. Semaglutide side effects vary widely from person to person, and the probiotic approach should be just as personalized. Here is how to match strains to symptoms.
Probiotics for semaglutide constipation
Constipation affects roughly 20 to 25% of semaglutide users, making it the most reported GI side effect. The cause is straightforward: delayed gastric emptying extends transit time throughout the entire digestive tract, and the longer stool sits in the colon, the more water gets absorbed, making it harder and more difficult to pass.
Your primary strain here is Bifidobacterium lactis, specifically the BB-12 or HN019 sub-strains. Start with 5 billion CFU daily and increase to 10 billion after one week if needed. Pair it with Bifidobacterium longum at 5 billion CFU for its motility-enhancing effects.
Timing matters. Take your constipation-targeted probiotics with your largest meal of the day. The food provides a buffering effect that helps more organisms survive stomach acid, and the meal itself stimulates the gastrocolic reflex, a natural wave of intestinal contractions that promotes bowel movements. For detailed dietary strategies that complement probiotic use, explore our guide on the best foods to eat on semaglutide.
If probiotics alone are not resolving constipation after two to three weeks, you may need to add a prebiotic fiber supplement, increase water intake to at least 80 ounces daily, review the complete semaglutide diet plan, or discuss additional treatment options with your provider. Some users find that splitting their semaglutide dose reduces constipation severity as well.
Probiotics for semaglutide diarrhea
Diarrhea is less common than constipation with semaglutide, but it can be more disruptive to daily life. It tends to occur most frequently during the first few weeks of treatment or immediately after dose increases, as the gut adjusts to the new GLP-1 signaling levels.
Saccharomyces boulardii is your first-line probiotic for diarrhea. Take 250 to 500 mg daily at the first sign of loose stools. Because it is a yeast and not a bacterium, it works through different pathways than bacterial probiotics and produces results quickly, often within 48 to 72 hours.
Add Lactobacillus rhamnosus GG at 10 billion CFU daily for additional diarrhea management and immune support. The combination of S. boulardii and LGG covers multiple mechanisms: toxin neutralization, intestinal barrier strengthening, fluid balance normalization, and immune modulation.
Critical note: if diarrhea persists beyond two weeks or is accompanied by fever, blood in stool, or severe dehydration, contact your healthcare provider immediately. Probiotics support normal GI function, but they are not a treatment for serious infections or inflammatory conditions. For more guidance on managing the adjustment period, read about how semaglutide makes you feel during the early weeks. Users who stop semaglutide abruptly may also experience a rebound in GI symptoms as the gut adjusts to the absence of GLP-1 stimulation.
Probiotics for nausea and bloating
Nausea is the side effect most semaglutide users fear, and it is the one with the weakest direct probiotic evidence. No robust clinical trials demonstrate that any probiotic strain prevents GLP-1-related nausea specifically. That is the honest truth, and any product claiming otherwise is overstating the science.
However, there is an indirect pathway that matters. Much of semaglutide-associated nausea stems from delayed gastric emptying, food sitting in the stomach longer than normal, leading to a sensation of fullness and queasiness. Probiotics that improve overall gut motility and reduce bacterial fermentation may help by addressing contributing factors rather than the nausea directly.
Bifidobacterium longum is the priority strain for this combination of symptoms. Its gas-reducing properties ease the bloating that often accompanies and worsens nausea. Lactobacillus reuteri adds value by normalizing gastric motility signals. Together, these strains create a less hostile gut environment that may reduce the intensity and duration of nausea episodes.
Practical tips: take these probiotics at least two hours before or after your meal, as nausea-prone users often do better with probiotics on a relatively empty stomach. Avoid probiotics that contain prebiotics like inulin or FOS during active nausea episodes, as these fermentable fibers can temporarily increase gas production and worsen symptoms. The foods to avoid on semaglutide guide covers dietary triggers that compound nausea.
Probiotics for sulfur burps on semaglutide
Sulfur burps. The rotten-egg-smelling belches that have spawned countless threads in GLP-1 support groups. They are one of the most distinctive and socially distressing side effects of semaglutide, and they have a specific microbial cause that probiotics can help address.
Sulfur burps occur when hydrogen sulfide-producing bacteria overgrow in the upper GI tract. Semaglutide delayed gastric emptying creates a warm, food-rich environment where sulfur-reducing bacteria like Desulfovibrio can thrive. These organisms break down sulfur-containing amino acids from protein-rich foods and release hydrogen sulfide gas, which rises through the esophagus as those unmistakable burps.
The probiotic strategy for sulfur burps is about competitive exclusion: flooding the gut with beneficial organisms that outcompete sulfur-producing bacteria for resources and attachment sites. Lactobacillus reuteri and Lactobacillus rhamnosus GG are the most effective strains for this purpose. Both produce antimicrobial compounds that inhibit sulfur-reducing bacteria, and both compete for the same ecological niche in the upper GI tract.
Take these strains first thing in the morning on an empty stomach, at least 30 minutes before eating. This gives the probiotics time to reach the upper intestine before food arrives. Simultaneously, reduce your intake of high-sulfur foods like eggs, cruciferous vegetables, and red meat during flare-ups. Our comprehensive guide on sulfur burps and GLP-1 medications provides additional dietary and lifestyle strategies for managing this specific side effect.
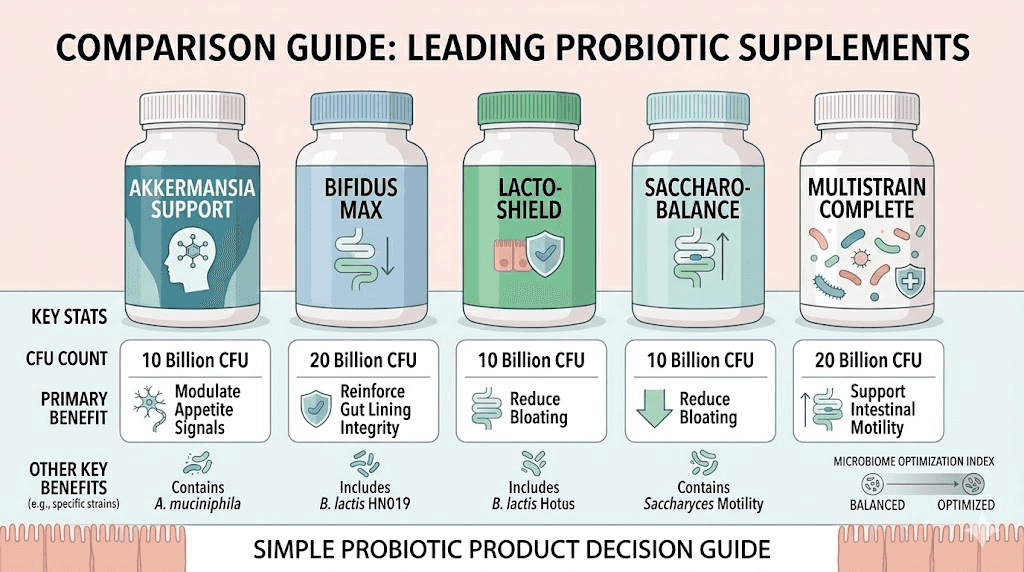
Best probiotic products for semaglutide users
Knowing which strains to target is half the equation. The other half is finding products that deliver those strains in therapeutic doses with reliable quality. The probiotic supplement market is notoriously inconsistent, with some products containing far fewer viable organisms than their labels claim. These five products have the strongest combination of relevant strains, third-party testing, and real-world results among semaglutide users. You can use our peptide cost calculator to budget supplement spending alongside your medication costs.
Pendulum GLP-1 Probiotic
This is the only probiotic product specifically formulated for GLP-1 support, and it contains the strain that matters most: Akkermansia muciniphila. The formula also includes Clostridium butyricum, which produces butyrate, a short-chain fatty acid that directly stimulates GLP-1 secretion from intestinal L-cells, and Bifidobacterium infantis for general digestive support.
Pendulum consumer research shows that 91% of users reported reduced food cravings after six weeks of use. While this is company-funded data and should be interpreted with appropriate skepticism, the mechanistic rationale is sound. Akkermansia P9 protein and Clostridium butyricum butyrate both stimulate pathways that enhance GLP-1 signaling, which should complement semaglutide effects.
The downside is cost. Pendulum GLP-1 Probiotic runs significantly more than generic probiotic blends, reflecting the difficulty and expense of manufacturing Akkermansia in viable form. For a detailed analysis, read our full Pendulum GLP-1 Probiotic review. If budget allows, this is the most targeted option for semaglutide users who want to enhance their GLP-1 response.
Seed DS-01 Daily Synbiotic
Seed takes a different approach. Rather than targeting GLP-1 specifically, DS-01 delivers 24 clinically studied strains across multiple categories: gastrointestinal health, gut barrier integrity, gut immune function, dermatological health, cardiovascular health, and micronutrient synthesis. The total count is 53.6 billion AFU (active fluorescent units, their preferred metric over CFU).
For semaglutide users, the relevant strains include Bifidobacterium longum, Lactobacillus rhamnosus, and several other Bifidobacterium and Lactobacillus species that support motility and reduce gas production. The product uses a patented two-capsule-in-one design where the outer capsule acts as a prebiotic and the inner capsule protects the probiotic strains from stomach acid.
Seed does not contain Akkermansia or L. reuteri, which means it misses the GLP-1-enhancing strains. However, its broad-spectrum approach covers multiple GI symptoms simultaneously, making it a strong choice for users experiencing a mix of constipation, bloating, and irregular bowel function. The quality control standards are among the highest in the industry, with genomic verification of every strain and third-party testing for potency through shelf life.
VSL#3
VSL#3 is the heavyweight of the probiotic world, delivering 450 billion CFU per sachet across eight bacterial strains. Originally developed for managing inflammatory bowel conditions, it has the most clinical evidence behind it for serious gastrointestinal issues.
The formula includes multiple strains of Lactobacillus, Bifidobacterium, and Streptococcus thermophilus. The sheer microbial load makes it particularly effective for resetting a disrupted gut microbiome, which is exactly what happens during semaglutide initiation. Multiple randomized controlled trials show improvements in bloating, abdominal pain, and stool consistency.
The caveat: VSL#3 requires refrigeration, comes in powder sachets that need to be mixed into cold food or liquid, and is more expensive than standard capsule probiotics. It is also more than most semaglutide users need. Users interested in understanding the broader landscape of peptides for gut health can explore additional compounds that support intestinal repair. Consider VSL#3 if you have a history of GI issues predating semaglutide, if standard probiotics have not resolved your symptoms after four to six weeks, or if your provider recommends a high-potency formulation. For people whose semaglutide protocol includes B12 or other compounded additions, VSL#3 offers robust gut support during complex regimens.
Culturelle Digestive Daily
Sometimes the simplest approach works best. Culturelle Digestive Daily contains a single strain, Lactobacillus rhamnosus GG, at 10 billion CFU per capsule. No fillers, no unnecessary additions, just the most studied probiotic strain in the world in a clinically validated dose.
For semaglutide users who want a no-frills, evidence-based probiotic that targets diarrhea and immune support, Culturelle is hard to beat on a value basis. It is widely available at every pharmacy, does not require refrigeration, and costs a fraction of premium products. The trade-off is that you are getting one strain instead of a targeted blend, so if constipation or bloating are your primary concerns, you may need to supplement with additional strains.
Culturelle works well as a starting point for semaglutide users who are new to probiotics and want to test their tolerance before investing in more complex (and expensive) formulations.
Align Probiotic
Align contains Bifidobacterium longum 35624, a proprietary strain specifically studied for abdominal discomfort, bloating, and gas. Originally marketed for IBS sufferers, it has found a growing audience among GLP-1 users whose primary complaints center on these symptoms.
The dose is relatively modest at 1 billion CFU per capsule, but B. longum 35624 has been shown to be effective at this count in multiple clinical trials. The strain was isolated and developed by gastroenterologists, and it is the only Bifidobacterium strain with FDA-recognized structure/function claims for digestive health.
Align is a targeted choice for semaglutide users whose bloating and gas are more problematic than constipation or diarrhea. Those dealing with persistent semaglutide burping may also find B. longum 35624 helpful for reducing upper GI gas. It pairs well with Culturelle (LGG) for a simple two-product protocol that covers bloating, gas, diarrhea, and immune support without overcomplicating things. Those using starting doses of semaglutide may find this combination sufficient, while users at higher doses like 1.7 mg may need a more comprehensive approach.
Product comparison
Product | Key strains | CFU count | Best for | Rating |
|---|---|---|---|---|
Pendulum GLP-1 | Akkermansia, C. butyricum, B. infantis | Not disclosed | GLP-1 enhancement, cravings | 9/10 |
Seed DS-01 | 24 strains including B. longum, L. rhamnosus | 53.6 billion AFU | Broad GI support, gut barrier | 8/10 |
VSL#3 | 8 strains, Lactobacillus, Bifidobacterium, Streptococcus | 450 billion CFU | Severe GI issues, microbiome reset | 8/10 |
Culturelle | L. rhamnosus GG | 10 billion CFU | Diarrhea, immune support, simplicity | 7/10 |
Align | B. longum 35624 | 1 billion CFU | Bloating, gas, abdominal comfort | 7/10 |
The best product depends on your priorities. If maximizing GLP-1 response is the goal, Pendulum wins. If broad-spectrum gut support at a reasonable price point matters more, Seed or VSL#3 deliver. For targeted single-symptom management on a budget, Culturelle or Align get the job done. Many experienced semaglutide users combine two products, often Pendulum plus either Culturelle or Align, to cover both GLP-1 enhancement and symptom-specific relief.
When and how to take probiotics with semaglutide
Timing is not everything. But it is a lot.
The most common mistake semaglutide users make with probiotics is treating timing as an afterthought, popping capsules whenever they remember without considering how the probiotic interacts with their injection schedule, meals, and other supplements. A strategic approach to timing can significantly improve both probiotic survival and effectiveness.
Timing relative to injection day
Semaglutide injections trigger a cascade of physiological changes that peak in the 24 to 48 hours after injection. GLP-1 receptor activation intensifies, gastric emptying slows further, and GI symptoms like nausea and bloating are most likely during this window. For users who select their injection timing carefully, probiotic timing should follow suit.
Take your probiotics consistently every day, not just on injection days. Consistency matters far more than any single-day timing trick. However, if you experience intensified GI symptoms on injection day and the day after, consider doubling your probiotic dose on those two days to provide extra microbial support during peak medication activity. This is especially relevant for users navigating the early titration phase described in our semaglutide dosage chart.
Morning vs evening dosing
Research on probiotic timing is limited but suggestive. A small study found that probiotics taken 30 minutes before breakfast showed higher gut colonization rates than those taken at other times. The theory is that overnight fasting reduces stomach acid production, creating a less hostile environment for probiotic organisms to survive the journey to the intestines.
For most semaglutide users, morning dosing before breakfast works well. However, if you take your semaglutide injection in the morning and experience peak nausea within a few hours, taking probiotics on an already-queasy stomach may worsen discomfort. In that case, shift probiotics to the evening, at least two hours after dinner.
The exception is Saccharomyces boulardii for active diarrhea. Take it as soon as symptoms appear, regardless of time of day or meal timing.
With food or on empty stomach
This depends on the specific probiotic and your symptoms. General guidelines that serve most semaglutide users well:
Lactobacillus and Bifidobacterium strains: take with a meal containing some fat, which buffers stomach acid and improves survival rates
Saccharomyces boulardii: take on an empty stomach or with food, as it survives stomach acid regardless
Akkermansia-containing products (Pendulum): follow the manufacturer directions, as encapsulation technology varies
Multi-strain blends (Seed, VSL#3): take according to product instructions, as delivery systems differ
If nausea is a concern, avoid taking probiotics with your largest meal. Opt for a lighter meal or snack instead. Users following a structured semaglutide diet plan can integrate probiotic timing into their meal schedule for consistency. The GLP-1 oral liquid dosing guide covers timing considerations for those using non-injectable formulations.
Starting before vs after beginning semaglutide
This is a question that does not get asked often enough. The ideal approach is to start probiotics two to four weeks before your first semaglutide injection. This gives beneficial bacteria time to establish populations in your gut before the medication begins altering the microbial landscape.
Think of it as preparing the soil before planting. A gut that already has robust Lactobacillus, Bifidobacterium, and Akkermansia populations will be more resilient to the disruptions semaglutide causes. Users who start probiotics proactively report fewer and milder GI side effects during the critical first four to six weeks of semaglutide treatment.
If you have already started semaglutide without probiotics, it is not too late. Begin supplementation immediately and expect two to four weeks before you notice meaningful changes. The gut microbiome does not shift overnight, regardless of when you start. For users who are still in the early stages, our guide on when weight loss begins on semaglutide provides helpful timeline expectations.
How semaglutide reshapes your gut bacteria
We touched on this earlier, but the specifics matter. Understanding exactly how semaglutide changes your microbiome helps explain why certain probiotics work and others do not, and it informs a more strategic supplementation approach.
Akkermansia increases
Multiple animal studies demonstrate that GLP-1 receptor agonists like semaglutide increase Akkermansia muciniphila populations in the gut. This is one of the few microbiome changes that is unambiguously positive. Higher Akkermansia levels correlate with better metabolic health markers, stronger gut barrier function, and improved insulin sensitivity.
The mechanism involves GLP-1 signaling promoting mucus production in the intestinal lining. Since Akkermansia feeds on mucus, more mucus means more Akkermansia. This creates a virtuous cycle where the bacterium strengthens the mucus layer it feeds on, maintaining gut barrier integrity while producing the P9 protein that stimulates additional GLP-1 production.
For probiotic strategy, this means Akkermansia supplementation is especially valuable in the early weeks before semaglutide has had time to naturally boost these populations.
Bifidobacterium shifts
The study on Chinese type 2 diabetes patients showed Bifidobacterium abundance nearly doubling from 10.38% to 17.98% after semaglutide treatment. Bifidobacterium species are generally beneficial, producing short-chain fatty acids, supporting immune function, and helping with nutrient absorption.
However, this rapid expansion of one genus can come at the expense of others. Microbial ecology operates on competition. When Bifidobacterium populations surge, they consume more of the available resources, potentially crowding out other beneficial organisms. This is one reason why overall diversity can decrease even as certain beneficial species increase.
Supplementing with diverse Lactobacillus strains alongside the natural Bifidobacterium increase helps maintain broader bacterial diversity while supporting the positive shifts semaglutide initiates. Users who have been on the medication for extended periods, as discussed in the long-term semaglutide guide, should be particularly attentive to diversity maintenance.
Diversity concerns
Reduced microbial diversity is the most concerning microbiome change associated with semaglutide. A diverse gut microbiome is a resilient one. It can adapt to dietary changes, resist pathogen invasion, and maintain stable metabolic function. When diversity drops, the ecosystem becomes more fragile and more susceptible to disruption from stress, dietary changes, antibiotics, or illness.
Animal studies show that semaglutide reduces alpha diversity, a measure of how many different species coexist in the gut. While human data is more limited, the clinical picture is consistent: semaglutide users who experience persistent GI issues often show lower microbiome diversity on stool testing than those who tolerate the medication well.
This is where broad-spectrum probiotics like Seed DS-01 or VSL#3 earn their value. By introducing multiple species simultaneously, they help counteract the diversity-reducing effects of semaglutide. A multi-strain approach is particularly important for long-term users who plan to continue semaglutide for extended periods.
What this means long-term
The long-term microbiome effects of semaglutide remain an active area of research. We do not yet have comprehensive human data spanning years of continuous use. What we know from shorter-term studies and animal models suggests that the beneficial changes (increased Akkermansia, increased Bifidobacterium) likely persist as long as the medication continues, while the diversity reduction may stabilize or partially reverse as the gut adapts.
Users who want to understand how their medication is processed can check the semaglutide shelf life and storage duration guides to ensure medication potency is not a confounding factor. For practical purposes, this means probiotic supplementation is not just a short-term fix for initial side effects. It is an ongoing component of a thoughtful semaglutide protocol. Users who maintain consistent probiotic intake throughout their treatment are investing in long-term gut resilience. Those considering discontinuing semaglutide should continue probiotics through the transition period, as the microbiome will shift again when GLP-1 signaling returns to baseline levels.
Building a complete gut health protocol on semaglutide
Probiotics are powerful. But they are most effective as part of a comprehensive gut health strategy rather than a standalone intervention. The semaglutide users who report the fewest side effects and the best overall outcomes are typically the ones who address gut health from multiple angles simultaneously.
Prebiotics: feeding your good bacteria
Prebiotics are non-digestible fibers that serve as food for beneficial gut bacteria. Without adequate prebiotic intake, even the best probiotic supplement will struggle to establish lasting colonies. The organisms need fuel to multiply and compete effectively against less desirable species.
The most effective prebiotics for semaglutide users include partially hydrolyzed guar gum (PHGG), which improves stool consistency without excessive gas production, acacia fiber, which is gentle on sensitive stomachs and feeds Bifidobacterium species, and resistant starch from cooled potatoes, green bananas, or supplements, which selectively promotes butyrate-producing bacteria.
Start with small doses. Semaglutide users are often more sensitive to fermentable fibers than the general population because delayed gastric emptying gives bacteria more time to ferment these substrates. Begin with 3 to 5 grams of prebiotic fiber daily and increase by 2 to 3 grams per week as tolerated. If bloating worsens, reduce the dose and increase more gradually.
Fermented foods
Fermented foods deliver live cultures in a food matrix that may enhance survival through the digestive tract. They also provide nutrients, enzymes, and organic acids that support overall gut health beyond what isolated probiotic strains offer.
The most beneficial fermented foods for semaglutide users include plain yogurt with live active cultures (check the label for specific strains), kefir (contains a broader range of organisms than yogurt), sauerkraut and kimchi (provide Lactobacillus species plus fiber), and miso soup (gentle on the stomach and provides glutamate that supports gut lining repair).
A practical goal is one to two servings of fermented foods daily. For semaglutide users with reduced appetite, small portions count. Even a few tablespoons of sauerkraut or a small cup of yogurt provide meaningful microbial diversity. Integrate these into the foods you eat while on semaglutide for dual nutritional and probiotic benefits.
Hydration strategies
Water is the most overlooked component of gut health on semaglutide. Dehydration worsens every GI side effect. It makes constipation harder to resolve, increases the concentration of bile acids that irritate the gut lining, reduces the volume of protective mucus, and impairs the motility that probiotics are trying to support.
Aim for a minimum of 64 ounces of water daily, and closer to 80 to 100 ounces if you are active or live in a warm climate. Semaglutide can reduce thirst cues alongside appetite, so many users need to set reminders or use marked water bottles to ensure adequate intake. Electrolyte-enhanced water can be helpful, especially for users experiencing diarrhea. Some users experiencing dizziness on semaglutide find that improved hydration resolves the issue entirely.
Diet considerations
What you eat shapes your microbiome more powerfully than any supplement. A diet rich in diverse plant foods provides the range of fibers and polyphenols that feed different bacterial species and maintain diversity. Research consistently shows that people who eat 30 or more different plant foods per week have significantly more diverse gut microbiomes than those who eat fewer than 10.
For semaglutide users with reduced appetite, quality over quantity matters even more. Every bite should count. Prioritize colorful vegetables, berries, legumes, nuts, seeds, and whole grains when your appetite allows. Avoid highly processed foods that feed inflammatory bacteria and contain emulsifiers that disrupt the gut lining. Our detailed guide on foods to avoid on semaglutide covers specific items that undermine gut health.
Protein intake deserves special attention. Semaglutide users often eat less protein than they need, which can accelerate muscle loss during weight reduction. High-quality protein sources like fish, poultry, eggs, and legumes also provide amino acids that support gut lining repair. For meal planning guidance, the GLP-1 breakfast ideas article and protein shake recipes for GLP-1 users offer practical starting points.
Supplements that complement probiotics
Several supplements work synergistically with probiotics to support gut health during semaglutide treatment.
L-glutamine, the most abundant amino acid in the body, is the primary fuel source for intestinal cells. Supplementing with 5 to 10 grams daily can support gut lining repair and reduce intestinal permeability. This is especially relevant for semaglutide users whose microbiome shifts have compromised barrier function.
Digestive enzymes can help compensate for the disrupted digestion that delayed gastric emptying causes. A broad-spectrum enzyme blend taken with meals helps break down proteins, fats, and carbohydrates more completely, reducing the amount of undigested material available for bacterial fermentation and gas production.
Zinc carnosine has specific evidence for gastric mucosal healing and may help with the stomach irritation some semaglutide users experience. B vitamins, particularly B12, can become depleted during semaglutide treatment due to reduced food intake and altered absorption. Many users benefit from a semaglutide and B12 combination approach. Berberine is another supplement some users combine with semaglutide for additional metabolic support, though it should be introduced carefully due to its own effects on the gut microbiome. Users who drink alcohol on semaglutide should be especially attentive to zinc and B vitamin status, as alcohol further depletes these nutrients.

What the research actually shows
Claims about probiotics and semaglutide range from well-supported to wildly speculative. Separating evidence from hype requires looking at the actual studies, their limitations, and what they do and do not prove.
The L. reuteri GLP-1 study
The Simon et al. study is the most frequently cited evidence for probiotic-GLP-1 synergy, and understanding its details matters. Twenty-one participants with stable glucose tolerance received either Lactobacillus reuteri SD5865 or placebo for four weeks. After a standardized meal test, the L. reuteri group showed 76% higher GLP-1 release and 49% higher insulin secretion.
These results are genuinely impressive. But context is essential. The study was small (21 participants), short-term (four weeks), and conducted in metabolically healthy individuals, not in people taking GLP-1 receptor agonists. We are extrapolating when we suggest these results apply to semaglutide users. The biological plausibility is strong. L. reuteri enhancing natural GLP-1 production while semaglutide provides exogenous GLP-1 receptor activation makes mechanistic sense. But we do not yet have a randomized controlled trial specifically testing L. reuteri supplementation in semaglutide users.
What the study tells us: L. reuteri can significantly increase natural GLP-1 production. What it does not tell us: whether this enhancement produces measurably better outcomes when combined with semaglutide.
Systematic reviews on GLP-1 and gut microbiota
Several systematic reviews have examined the relationship between GLP-1 receptor agonists and the gut microbiome. The consistent finding is that these medications produce measurable shifts in bacterial composition, with increases in Akkermansia and Bifidobacterium being the most replicated results.
However, most of the primary studies underlying these reviews are animal studies, often conducted in mice or rats. The human data is sparser and more variable. Some human studies show the same patterns seen in animals. Others show different shifts depending on the population studied, the specific GLP-1 agonist used, and the duration of treatment.
The reviews generally conclude that gut microbiome modulation may contribute to the metabolic benefits of GLP-1 receptor agonists, and that probiotics may complement these effects. But the language is appropriately cautious: "may," "suggest," "warrant further investigation." We are in the early stages of understanding this interaction, not at the point of definitive clinical recommendations.
Animal vs human study limitations
Much of the microbiome research on semaglutide comes from rodent models. While animal studies are valuable for understanding mechanisms, they have significant limitations when applied to human probiotic recommendations.
Mice have fundamentally different gut microbiome compositions than humans. They eat different diets, have different gut transit times, and harbor different bacterial species. A probiotic effect observed in mice may not translate to humans, and the doses used in animal studies often do not scale linearly to human equivalents.
Additionally, laboratory mice live in controlled environments with standardized diets, which removes the enormous variability in diet, lifestyle, stress, and medication use that characterizes real human gut microbiomes. The pristine conditions of a mouse study do not replicate the complexity of a human taking semaglutide while also managing work stress, variable sleep, multiple medications, and a real-world diet.
An honest assessment of the evidence
Here is the straight truth about probiotics and semaglutide.
Strong evidence exists for individual probiotic strains addressing specific GI symptoms (constipation, diarrhea, bloating) regardless of cause. These benefits likely extend to semaglutide-induced symptoms, though direct studies are limited.
Moderate evidence exists for L. reuteri enhancing GLP-1 production and for Akkermansia supporting gut barrier function during GLP-1 therapy. The mechanistic rationale is sound, and preliminary data is encouraging.
Weak evidence exists for probiotics preventing semaglutide nausea specifically, for specific probiotic products outperforming others in GLP-1 populations, and for optimal probiotic timing relative to semaglutide injections.
No evidence exists for probiotics replacing semaglutide, for specific CFU counts being necessary for semaglutide users (as opposed to general probiotic dosing), or for probiotics eliminating all GI side effects.
This honest assessment should not discourage probiotic use. The general evidence for probiotic benefits in GI health is substantial, and the specific mechanistic connections to GLP-1 therapy are promising. But it should calibrate expectations. Probiotics are a supportive measure, not a magic bullet. Users tracking their semaglutide results week by week should give probiotics at least four weeks before judging their impact.
Common mistakes when combining probiotics and semaglutide
Even informed users make errors that reduce the effectiveness of their probiotic strategy. These are the mistakes that come up most frequently in GLP-1 communities and clinical discussions.
Taking probiotics too close to injection
Some users take their probiotic immediately before or after their semaglutide injection, thinking the two should be administered together. This is not harmful, but it is suboptimal. The nausea and GI disruption that often follow injection can reduce probiotic absorption and increase the likelihood of vomiting the dose before it reaches the intestines.
Better approach: maintain your normal daily probiotic schedule regardless of injection timing. Users wondering about accidental intramuscular injection should know that injection technique does not affect probiotic strategy, though it may influence how the medication absorbs. If your injection causes significant nausea, skip the probiotic dose for that session and resume at the next regular time. Consistency over weeks matters far more than any single dose. Users who inject at a specific time can find guidance in the best injection site article to minimize injection-related discomfort.
Choosing wrong strains for wrong symptoms
A semaglutide user with constipation takes a probiotic heavy in Saccharomyces boulardii, which is primarily an anti-diarrheal agent. A user with diarrhea takes a product loaded with Bifidobacterium lactis, which can increase stool frequency. The mismatch is common and can actually worsen symptoms.
Refer to the side effect matching section above. Identify your primary symptom first, then select the strain or product that targets it. If you have multiple symptoms, prioritize the most disruptive one and add secondary strains after two weeks once the primary issue has stabilized.
Expecting too much too fast
Probiotics are not antibiotics. They do not produce dramatic overnight results. The gut microbiome shifts gradually, and meaningful changes in symptoms typically require two to four weeks of consistent supplementation. Users who try a probiotic for three days, notice no difference, and switch to a different product are never giving any single approach enough time to work.
Set realistic expectations. This mirrors the patience required for the medication itself, as many users ask how long semaglutide takes to suppress appetite. Commit to one probiotic strategy for a minimum of four weeks before evaluating its effectiveness. Keep a simple symptom diary noting your primary complaints on a 1-to-10 scale daily. After four weeks, compare your average scores to baseline. Small improvements (2 to 3 points on a 10-point scale) are clinically meaningful, even if they do not feel transformative on any given day. This patience applies equally to the medication itself, as our guide on how long semaglutide takes to work explains.
Buying low-quality or low-CFU products
The probiotic supplement market has minimal regulation compared to pharmaceuticals. Independent testing by organizations like ConsumerLab and LabDoor has repeatedly found products that contain far fewer viable organisms than their labels claim. Some products contain different species entirely than what is listed.
Quality markers to look for include third-party testing certifications (USP, NSF, or independent lab verification), guaranteed CFU counts at expiration (not just at time of manufacture), specific strain identification (e.g., Lactobacillus rhamnosus GG, not just "Lactobacillus rhamnosus"), appropriate storage requirements clearly stated, and a company that publishes its clinical research or references specific studies.
Price is not a perfect indicator of quality, but extremely cheap probiotics (under a few dollars for a month supply) are almost certainly underdelivering on their label claims.
Stopping too early
Many semaglutide users start probiotics when side effects are at their worst during initial titration, experience improvement as their body adjusts to the medication, and then stop taking probiotics, attributing the improvement entirely to adaptation rather than microbial support.
The problem is that stopping probiotics can cause a rebound in symptoms, especially when you increase your semaglutide dose. Each dose increase is essentially another disruption to the gut microbiome, and the probiotic support that helped you through the previous adjustment is no longer there.
A smarter approach is to continue probiotics throughout your semaglutide treatment, including through all dose titrations. You can potentially reduce the dose or simplify from a multi-strain approach to a single maintenance strain once your symptoms have been stable for two to three months. But complete discontinuation during active semaglutide treatment is premature for most users, whether they are in their first month or well past the post-surgery resumption phase. This is particularly important during the challenging phases described in our four weeks on semaglutide guide and when users face a semaglutide plateau.
Advanced considerations for long-term semaglutide users
Users who have been on semaglutide for months face different gut health challenges than those just starting out. Initial side effects typically subside, but longer-term microbiome changes continue evolving. Probiotic strategy should adapt accordingly.
Nutrient absorption and probiotic support
Prolonged reduced food intake on semaglutide can lead to deficiencies in key nutrients that the gut microbiome needs to function optimally. B vitamins, zinc, magnesium, and iron are commonly affected. Certain Bifidobacterium strains help synthesize B vitamins and improve mineral absorption, making them particularly valuable for long-term users who may not be eating enough to meet their nutritional needs through diet alone.
Consider pairing your probiotic with a high-quality multivitamin or specific nutrient supplements based on bloodwork. Many semaglutide users benefit from methylcobalamin supplementation alongside their probiotic, as B12 absorption depends partly on healthy gut flora. The GLP-1 vitamin guide covers nutritional considerations in detail.
Transitioning off semaglutide
When users eventually discontinue semaglutide, the gut microbiome shifts again as gastric motility returns to normal and GLP-1 receptor activation from the medication ceases. This transition period can bring its own wave of GI symptoms, including changes in bowel habits, appetite fluctuations, and digestive discomfort.
Continue probiotic supplementation for at least four to eight weeks after your last semaglutide dose. The gut microbiome needs time to re-establish equilibrium without the medication influence. L. reuteri is especially valuable during this period because it supports natural GLP-1 production, potentially helping maintain some metabolic benefits as the exogenous GLP-1 analog clears your system. Our guide on semaglutide withdrawal symptoms covers what to expect during discontinuation, and the article on restarting semaglutide after a break addresses how to approach re-initiation if needed. Users storing medication should also review compounded semaglutide fridge storage timelines and whether expired semaglutide is safe to use.
Combining with other GLP-1 support supplements
Many semaglutide users take additional supplements beyond probiotics. Understanding interactions is important. Glycine supplementation is increasingly popular among semaglutide users for its role in collagen synthesis and sleep quality. Glycine does not interfere with probiotics and may actually support gut lining repair.
L-carnitine is another common addition for energy support and fat metabolism. It does not interact with probiotics directly, but users should space them apart if taking multiple supplements to reduce GI burden. Niacinamide and pyridoxine are also compatible with probiotic supplementation.
For users considering combining phentermine with semaglutide, be aware that stimulant medications can affect gut motility in opposite ways to GLP-1 agonists, creating a more complex microbiome environment where probiotic support becomes even more important. Semaglutide users also dealing with blood clot concerns or kidney stone risk should discuss all supplements, including probiotics, with their provider. The GLP-1 hair loss guide covers another common concern where nutritional status, supported by healthy gut absorption, plays a key role.
Probiotic considerations for different semaglutide formulations
The route of semaglutide administration may influence gut health in different ways. Injectable semaglutide affects the gut primarily through systemic GLP-1 receptor activation, while sublingual semaglutide and oral semaglutide drops also involve direct contact with the GI mucosa.
The GLP-1 oral liquid formulation is one example of a non-injectable approach. Oral formulations may have more direct effects on the upper GI microbiome, making probiotics that colonize the upper intestinal tract (like L. reuteri) potentially more relevant. Users of compounded semaglutide should apply the same probiotic principles regardless of the compounding pharmacy or formulation used. The active ingredient works the same way, whether injectable or oral, and the microbiome effects are comparable across formulations. Information on proper semaglutide reconstitution and injection technique ensures you are getting the full dose that your probiotic protocol is designed to complement.
Comparing probiotic approaches for GLP-1 users
Semaglutide is not the only GLP-1 medication on the market, and users considering or switching between options should understand how probiotic needs may differ. The core microbiome effects are similar across GLP-1 receptor agonists, but there are nuances worth noting.
Tirzepatide, which activates both GLP-1 and GIP receptors, may produce somewhat different microbiome shifts due to its dual mechanism. Users dealing with tirzepatide constipation or tirzepatide bloating should apply the same strain-matching principles outlined in this guide. The semaglutide vs tirzepatide side effect comparison reveals that tirzepatide users may experience slightly different GI symptom profiles, with tirzepatide diarrhea being somewhat more common in clinical trials.
Users who are switching from tirzepatide to semaglutide or considering whether tirzepatide might work better for them should maintain probiotic supplementation through the transition. Changing GLP-1 medications creates an additional microbiome disruption that probiotic support can help smooth.
For a broader comparison of these medications, including their metabolic effects and side effect profiles, the semaglutide vs tirzepatide comparison page and the phentermine vs semaglutide analysis, and the semaglutide glycine B12 blend guide provide detailed breakdowns. Users interested in GLP-1 therapy more broadly can explore the GLP-1 fat loss treatment overview and find the best GLP-1 injection site for weight loss.
Gut health beyond probiotics: the bigger picture
Probiotics are one tool in a larger toolkit. For semaglutide users serious about optimizing gut health, several additional factors deserve attention.
Stress and the gut-brain axis
Chronic stress directly impairs gut barrier function, shifts microbiome composition toward inflammatory species, and reduces the effectiveness of probiotic supplementation. The gut-brain axis is bidirectional, meaning gut dysfunction also worsens mood and stress responses, creating a negative feedback loop.
Semaglutide itself interacts with the gut-brain axis through central GLP-1 receptors in the brain. Some users report mood changes, anxiety, or insomnia during treatment. These neurological effects may partly reflect microbiome-mediated changes in neurotransmitter production. Users dealing with persistent fatigue or sleep disruption should consider that the gut produces approximately 95% of the body serotonin supply, and microbiome disruptions can alter serotonin synthesis.
Stress management practices, whether meditation, exercise, adequate sleep, or simply reducing unnecessary stressors, amplify the benefits of probiotic supplementation by creating a more hospitable gut environment for beneficial bacteria to thrive in.
Exercise and microbiome diversity
Regular physical activity is one of the most powerful ways to increase gut microbiome diversity, independent of diet or supplementation. Studies show that active individuals have significantly more diverse gut bacteria than sedentary individuals, and that starting an exercise program can shift the microbiome toward a healthier composition within weeks.
For semaglutide users, exercise serves double duty. It supports microbiome health while also enhancing the weight loss and metabolic improvements the medication provides. Even users who are trying to lose weight without exercise or those experiencing GLP-1 fatigue should consider moderate activity specifically for its gut health benefits. Walking 30 minutes daily is enough to produce measurable microbiome improvements.
Sleep and microbial rhythms
The gut microbiome follows circadian rhythms, with different bacterial species being more or less active at different times of day. Disrupted sleep throws off these microbial rhythms, reducing the effectiveness of time-sensitive probiotic dosing and impairing gut barrier function overnight when repair processes normally peak.
Prioritize seven to eight hours of quality sleep. If semaglutide affects your sleep, address this actively rather than accepting it as an unavoidable side effect. Users experiencing sleep disruption can find strategies in the semaglutide and insomnia guide.
The role of peptides in gut health
Beyond probiotics, certain peptides have shown promise for supporting gut health and reducing inflammation. The peptides for gut health resource page covers compounds that have been studied for gastrointestinal support. Inflammation-targeting peptides may complement probiotic therapy by addressing the inflammatory component of gut dysfunction, while KPV peptide has shown specific promise for intestinal inflammation in preclinical research.
Understanding how peptides work at the cellular level helps contextualize why gut health optimization matters for anyone pursuing peptide-based protocols. The introduction to peptides provides foundational knowledge for those new to the field, while the peptide safety guide covers important risk considerations. Users exploring gut-supportive peptides may also benefit from the peptide stack calculator for planning multi-compound protocols, and those curious about injection methods can reference the GLP-1 injection guide and injection site guide.
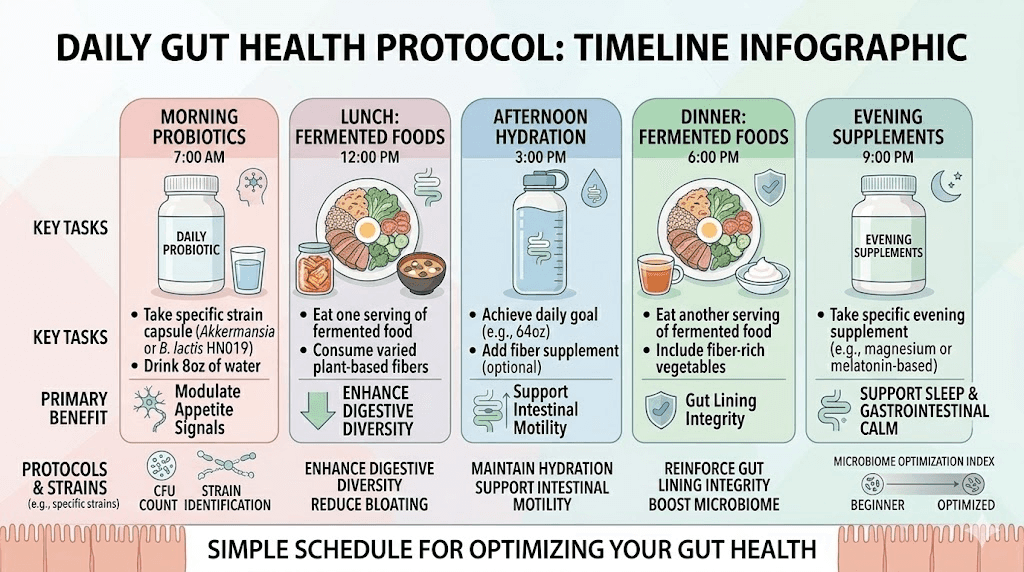
Practical protocol: putting it all together
Theory is useful. Execution is what changes outcomes. Here is a practical protocol that integrates everything covered in this guide into a manageable daily routine for semaglutide users.
Starter protocol (first four weeks)
Goal: establish baseline probiotic support and identify which strains work for your body.
Morning (30 minutes before breakfast):
Lactobacillus reuteri, 10 billion CFU
16 ounces of water
With breakfast:
Bifidobacterium lactis, 5 billion CFU (increase to 10 billion in week two if tolerated)
One serving of fermented food (yogurt, kefir, or sauerkraut)
Evening (with dinner):
Bifidobacterium longum, 5 billion CFU
3 to 5 grams prebiotic fiber (PHGG or acacia)
If experiencing diarrhea, add: Saccharomyces boulardii, 250 mg twice daily
Hydration target: 80 ounces minimum daily
Track your primary GI symptoms daily on a 1 to 10 scale. After four weeks, evaluate whether symptoms have improved. Use the semaglutide dosage calculator to ensure your medication dose is optimized alongside your probiotic protocol. Our general peptide calculator and reconstitution calculator are also available for those managing multiple compounds.
Enhanced protocol (after four weeks)
If the starter protocol helps but you want additional GLP-1 support, add Pendulum GLP-1 Probiotic according to product directions. If constipation remains an issue, increase Bifidobacterium lactis to 10 billion CFU and add 5 to 10 grams additional prebiotic fiber. If bloating persists, switch to Align (B. longum 35624) which has more specific evidence for bloating than generic B. longum supplements.
Maintenance protocol (after three months)
Once symptoms have been stable for two to three months, you can simplify. Continue L. reuteri daily for ongoing GLP-1 support. Rotate between a multi-strain product (Seed or VSL#3) and targeted single-strain products on a monthly basis to maintain diversity. Continue fermented foods and prebiotic fiber indefinitely. These dietary habits provide ongoing microbiome support that supplements alone cannot replicate.
SeekPeptides members access detailed protocols for optimizing every aspect of their semaglutide experience, from dosing strategies and injection techniques to side effect management and supplement stacking. The combination of personalized guidance and community support helps members navigate the complexities of GLP-1 therapy with confidence.
Special populations and considerations
Not every semaglutide user falls into the same category. Certain groups may need modified probiotic approaches.
Women using semaglutide should be aware that the medication can affect menstrual cycles, and hormonal fluctuations influence the gut microbiome independently. Probiotic support during the luteal phase (the two weeks before menstruation) may need to be more robust, as this is when GI symptoms tend to be most pronounced for women on GLP-1 medications. The interplay between semaglutide and hormonal health in women deserves attention when designing a complete protocol.
Users with autoimmune conditions should discuss probiotic supplementation with their healthcare provider, as certain strains can stimulate immune activity that may not be desirable in autoimmune contexts. The Hashimoto and GLP-1 guide addresses considerations for thyroid autoimmunity specifically, while the microdosing GLP-1 for autoimmune article explores conservative approaches. The tirzepatide with B12 and tirzepatide glycine guides offer parallel nutrient support information for dual-agonist users.
Users taking antibiotics concurrently with semaglutide face compounded microbiome disruption. Continue probiotics during and for at least four weeks after completing antibiotic courses. Saccharomyces boulardii is particularly valuable during antibiotic treatment because, as a yeast, it is not killed by antibacterial antibiotics.
Travelers taking semaglutide need to plan probiotic storage and access. Our travel with semaglutide guide covers medication logistics, and the same principles apply to probiotic supplements. Heat-stable products like Saccharomyces boulardii and certain shelf-stable multi-strain formulas are more practical for travel than refrigeration-dependent products. Understanding what your semaglutide should look like also helps catch storage issues while traveling. Users concerned about semaglutide arriving hot during shipping face analogous concerns with heat-sensitive probiotics. Those dealing with allodynia on semaglutide or GLP-1 injection site reactions should note that gut inflammation from poor microbiome health can amplify systemic inflammatory symptoms, making probiotic support even more relevant.
Users monitoring their labs should note that semaglutide can affect blood work results, and some probiotic effects may also influence lab values like inflammatory markers and liver enzymes. Share your complete supplement list with your healthcare provider for accurate interpretation. Information about qualifying for semaglutide and payment options like Afterpay can help with access considerations.
Understanding product labels and marketing claims
The probiotic industry spends billions on marketing, and much of it is misleading. Semaglutide users navigating this landscape need to separate genuine quality indicators from marketing noise.
CFU count alone means nothing without strain specificity. A product claiming 100 billion CFU of unspecified "probiotic blend" is likely less effective than a product delivering 10 billion CFU of a clinically studied strain. Always look for specific strain designations (the letters and numbers after the species name, like "GG" in Lactobacillus rhamnosus GG or "BB-12" in Bifidobacterium lactis BB-12).
"Clinically studied" on a label may refer to studies on the individual strains, not the specific product or combination. Check whether the company references actual published research and whether those studies used the same strains at similar doses as the product contains.
Delivery technology matters. Many probiotic organisms die in stomach acid before reaching the intestines. Enteric coating, delayed-release capsules, and microencapsulation can significantly improve survival rates. Products that invest in these technologies typically cost more but deliver more viable organisms to where they need to go.
Expiration dating should guarantee CFU count at expiration, not at time of manufacture. Probiotics naturally lose viability over time, and a product that only guarantees potency at manufacture may contain significantly fewer viable organisms by the time you use it. Reputable brands state "X billion CFU guaranteed at expiration" clearly on the label. This attention to expiration and storage parallels the importance of checking whether your compounded semaglutide has expired or whether it needs refrigeration.
Frequently asked questions
Can I take probiotics on the same day as my semaglutide injection?
Yes. There is no interaction between probiotics and semaglutide that requires separating them to different days. Take your probiotic at its normal time. If injection-day nausea makes you feel too unwell to take supplements, skip that dose and resume the next day. Consistency over weeks matters more than any single day. Review the best time of day to take semaglutide to optimize your schedule.
How long does it take for probiotics to help with semaglutide side effects?
Most users notice initial improvements in two to four weeks. Some symptoms like diarrhea may respond faster (within days) when using targeted strains like Saccharomyces boulardii. Constipation typically takes longer to resolve, often three to four weeks. Commit to a full four-week trial before judging effectiveness. For a broader timeline perspective, explore how long GLP-1 medications take to work.
Should I take probiotics before starting semaglutide?
Ideally, yes. Starting probiotics two to four weeks before your first semaglutide injection allows beneficial bacteria to establish populations before the medication disrupts the gut microbiome. This proactive approach can reduce the severity of initial side effects. Our first week on semaglutide guide covers what to expect during the early days.
Do I need to refrigerate my probiotics?
It depends on the product. Some probiotics (VSL#3, certain Akkermansia products) require refrigeration to maintain viability. Others (Saccharomyces boulardii, many shelf-stable blends) are designed to remain potent at room temperature. Check the product label. When in doubt, refrigerate. Cold storage never harms probiotics, but heat can kill them, similar to how semaglutide degrades when it gets warm.
Can probiotics replace semaglutide for weight loss?
No. Probiotics support gut health and may modestly enhance GLP-1 signaling, but they do not produce the dramatic appetite suppression and metabolic effects of semaglutide. Think of probiotics as a supporting player, not a substitute. The appetite suppression effects of semaglutide operate through different pathways than probiotics can replicate.
Is it safe to take multiple probiotic products at the same time?
Generally, yes. Different probiotic strains occupy different ecological niches in the gut and do not typically compete with each other. Many people take two or three different products simultaneously. The main risk is temporary digestive discomfort (gas, bloating) when introducing multiple new organisms at once. Start one product at a time, spacing new additions two weeks apart to identify which strains work best for your body.
Should I take probiotics with semaglutide if I have no side effects?
Even without noticeable side effects, semaglutide is changing your gut microbiome. Proactive probiotic support helps maintain microbial diversity and gut barrier function, potentially preventing problems before they develop. It is not mandatory if you feel fine, but it is a reasonable preventive measure, especially during dose increases when new symptoms can emerge. Monitor your monthly results and adjust accordingly.
What about probiotic-rich drinks and postbiotics for GLP-1 support?
Products like the reSM GLP-1 postbiotic, Replenza GLP-1, Tranont GLP-1, and the Advanced Bionutritionals GLP-1 Plus take different approaches to GLP-1 support, including postbiotics (metabolites produced by bacteria rather than live organisms). These can complement traditional probiotics but should not replace them for semaglutide side effect management. The Gentle Patches GLP-1 product takes yet another approach with transdermal delivery. For users interested in tracking their overall GLP-1 protocol, the GLP-1 plotter can help visualize progress over time. The relationship between GLP-1 and Ozempic is another common question worth understanding.
External resources
PubMed - National Library of Medicine (search "probiotics GLP-1" or "semaglutide microbiome" for primary research)
National Institute of Diabetes and Digestive and Kidney Diseases - Digestive Diseases
International Scientific Association for Probiotics and Prebiotics (ISAPP)
World Gastroenterology Organisation - Probiotics and Prebiotics
Navigating semaglutide side effects does not have to be a guessing game. The right probiotic strains, taken at the right doses and the right times, can transform your experience with GLP-1 therapy from barely tolerable to genuinely comfortable. The research is still evolving, the perfect protocol does not exist yet, and individual responses will always vary. But the tools and knowledge are here, right now, to make meaningful improvements.
SeekPeptides members access comprehensive protocols for every aspect of peptide and GLP-1 therapy, including gut health optimization, supplement stacking guides, and a community of experienced users who have navigated these exact challenges. For anyone serious about getting the most from their semaglutide treatment while protecting long-term gut health, personalized guidance makes the difference between adequate results and exceptional ones.
In case I do not see you, good afternoon, good evening, and good night. May your gut bacteria stay balanced, your side effects stay minimal, and your semaglutide results stay consistent.