Feb 20, 2026

Before you eat another meal on semaglutide, stop. That plate of food sitting in front of you could be the reason your side effects will not go away. The nausea that hits two hours after dinner. The bloating that makes you unbutton your pants. The bathroom issues nobody warned you about. These are not random. They are directly connected to what you are putting in your mouth.
Most people start semaglutide expecting the medication to do all the heavy lifting. Eat less, lose weight, done. But the reality is messier than that. Semaglutide fundamentally changes how your digestive system processes food, slowing gastric emptying by 30 to 40 percent and altering the speed at which nutrients move through your entire GI tract. Foods that caused zero problems before the medication can now trigger hours of misery. And certain food categories become outright enemies of your comfort and your results.
Clinical data backs this up. In a two-year study, 82.2 percent of patients taking semaglutide experienced gastrointestinal adverse events. Nausea alone accounted for over 2,300 reported cases. Vomiting, diarrhea, constipation, and bloating followed close behind. But here is what the studies do not always emphasize: dietary choices dramatically influence the severity of every single one of those side effects.
This guide covers every food category you should avoid or limit while taking semaglutide, explains the specific mechanisms behind why each one causes problems, and provides practical alternatives so you do not have to suffer through your protocol. Whether you are on week one of dose escalation or month six of maintenance, the strategies here will reduce your side effects and help you get the most out of every injection. SeekPeptides members have used these exact dietary frameworks to optimize their semaglutide protocols, and the difference between informed eating and guessing is enormous.
How semaglutide changes your digestive system
Understanding why certain foods become problematic requires knowing what semaglutide actually does inside your body. The medication is not just an appetite suppressant. It is a fundamental modifier of your entire digestive timeline.
Semaglutide mimics the GLP-1 hormone, which activates receptors in the brain, the pancreas, and the gastrointestinal tract simultaneously. At the brain level, it suppresses appetite by signaling fullness to the hypothalamus. At the pancreatic level, it stimulates insulin release and suppresses glucagon. But at the gut level, it does something that directly impacts every food decision you make.
It slows gastric emptying.
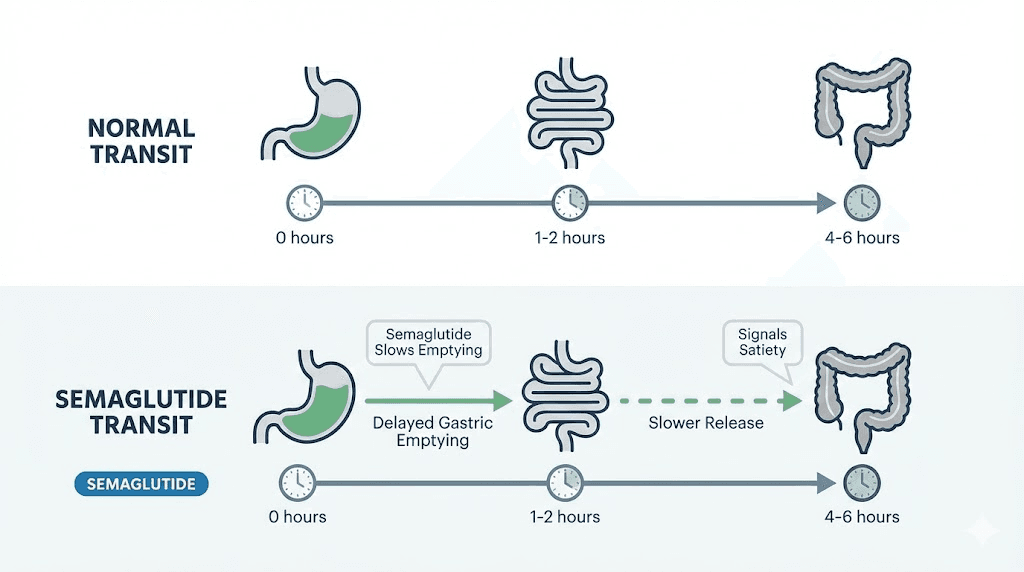
Dramatically. Food that normally moves from your stomach to your small intestine in two to four hours can now take six to eight hours or longer. Your stomach becomes a holding tank where food sits, ferments slightly, and waits. This delayed transit is the mechanism behind the appetite suppression you feel. It is also the mechanism behind nearly every gastrointestinal side effect.
Think of it this way. Your digestive system had a processing speed before semaglutide. Now that speed has been cut in half. Any food that was already slow to digest, heavy, fatty, fibrous, or dense, becomes exponentially slower. And slow digestion in a stomach that is already moving at reduced capacity creates pressure, gas, nausea, and discomfort. The foods on this avoid list are not arbitrary recommendations. They are foods that create the worst bottlenecks in a system that is already deliberately slowed down.
Two mechanisms drive the nausea specifically. First, delayed gastric emptying causes food to sit in the stomach longer, stretching the gastric walls and triggering nausea receptors. Second, semaglutide activates GLP-1 receptors in the brainstem that directly control the vomiting reflex. When you add foods that further slow digestion or irritate the GI lining, you amplify both pathways simultaneously. That is why certain meals feel fine for someone not on the medication but feel terrible for someone on semaglutide therapy.
The complete list of foods to avoid on semaglutide
Not every food on this list will cause problems for every person. Individual tolerance varies. But these categories consistently trigger the worst reactions across thousands of semaglutide users, and the physiological reasons are clear. Start by eliminating the most problematic categories, then test your individual tolerance as your body adjusts to the medication.
High-fat fried foods
This is the number one offender. Fried chicken, French fries, onion rings, mozzarella sticks, fried fish, tempura, doughnuts, and anything that has been submerged in hot oil. These foods create what clinicians call the double-slowing effect. Fat already takes the longest of any macronutrient to digest. It requires bile salts, lipase enzymes, and extended time in the small intestine for absorption. When you layer that onto a stomach that is already moving at half speed from semaglutide, the result is a traffic jam that can last six to ten hours.
The symptoms are predictable and miserable. Nausea that builds slowly after eating and peaks two to three hours later. A heavy, uncomfortable feeling in the upper abdomen that will not go away. In some cases, outright vomiting as the stomach attempts to clear what it cannot process efficiently. Users who track their symptoms consistently report that fried foods produce the most severe and longest-lasting side effects of any food category.
The fat content is only part of the problem. Fried foods also tend to be calorie-dense, meaning you consume a large amount of energy in a small volume. On semaglutide, when your total caloric intake has dropped 25 to 40 percent naturally, wasting those precious calories on nutritionally empty fried food means you miss out on the protein, fiber, and micronutrients your body desperately needs.
Skip the fried foods entirely during the first eight to twelve weeks of semaglutide therapy. After your body has fully adjusted, you can test small amounts, but most long-term users find that their tolerance for fried food never fully returns to pre-medication levels.
Greasy and fatty meats
Bacon, sausage, pepperoni, fatty ground beef, ribeye steaks, lamb chops, pork belly, and processed deli meats with high fat content all fall into this category. The issue is the same as fried foods but in a different package. High fat content plus slow gastric emptying equals prolonged discomfort.
Fatty red meat is particularly problematic because it combines high fat with dense protein that requires extensive mechanical and chemical breakdown. A thick, marbled steak that might have taken four hours to fully digest before semaglutide can now take eight hours or longer. During that entire window, your stomach is working overtime, and the sensation ranges from mild heaviness to active nausea.
This does not mean you need to eliminate meat entirely. Lean proteins like chicken breast, turkey breast, white fish, and shrimp digest much faster and rarely cause problems. The key distinction is fat content, not protein content. A four-ounce chicken breast with 3 grams of fat processes completely differently than a four-ounce sausage link with 22 grams of fat. Choose the lean option every time, especially during the first months of treatment.
Sugary foods and high-sugar snacks
Candy, cookies, cake, ice cream, pastries, chocolate bars, sweetened cereals, granola bars with added sugar, fruit juice concentrates, and anything with high added sugar content. These create problems on two fronts.
First, the blood sugar impact. Semaglutide works partly by regulating blood glucose through enhanced insulin release and glucagon suppression. When you consume a large sugar load, you create a rapid blood glucose spike that the medication then aggressively drives down. The result can be a rollercoaster of energy crashes, intensified nausea, shakiness, and brain fog that feels worse than it would without the medication present.
Second, the caloric waste. When you are eating 1,200 to 1,500 calories per day on semaglutide, every bite matters. A single candy bar at 250 calories represents roughly 15 to 20 percent of your daily intake. That is 250 calories that could have gone toward the protein your muscles need or the fiber your digestive system requires. Sugar provides energy and nothing else. No protein, no fiber, no vitamins, no minerals. It is the definition of empty calories, and on semaglutide, you simply cannot afford empty calories.
The cravings for sugar may decrease naturally as semaglutide alters your reward pathways. Many users report that sweets become less appealing within the first few weeks. Lean into that change. Let the medication work with your diet rather than fighting against it.
Refined carbohydrates and white flour products
White bread, regular pasta, white rice in large quantities, bagels, croissants, crackers made from refined flour, pizza dough, and most commercial baked goods. These foods share a fundamental problem. The refining process strips away fiber, vitamins, and minerals, leaving behind fast-digesting starches that spike blood sugar and provide minimal nutritional value.
On semaglutide, refined carbohydrates create a paradox. They digest quickly in terms of blood sugar impact, causing rapid glucose spikes, but they contribute to constipation because they lack the fiber that keeps the digestive tract moving. Semaglutide already slows gut motility. Adding low-fiber refined carbs on top of that further reduces the mechanical stimulation your intestines need to function properly.
The solution is not eliminating carbohydrates entirely. Complex carbohydrates like brown rice, quinoa, oats, sweet potatoes, and whole grain bread provide sustained energy, B vitamins, and fiber that supports digestive health. The difference between a slice of white bread and a slice of whole grain bread might seem small, but on semaglutide, that fiber content makes a measurable difference in how your digestive system handles the meal.
Swap one for one. Every time you reach for a refined carbohydrate, replace it with a whole grain alternative. The nutritional improvement compounds over time, and your GI tract will thank you.
Carbonated beverages
Soda, sparkling water, beer, champagne, energy drinks, and any beverage that contains dissolved carbon dioxide. The carbon dioxide releases as gas inside your stomach, and on semaglutide, that gas has nowhere to go quickly.
Normal gastric emptying allows gas to dissipate through belching and gradual absorption. Delayed gastric emptying traps that gas in a stomach that is already processing food more slowly. The result is bloating, excessive burping, abdominal distension, and increased nausea. Some users describe the sensation as feeling like their stomach is inflated like a balloon, and the pressure can persist for hours.
Sugary carbonated drinks like regular soda deliver a triple hit: carbonation causing gas, sugar causing blood glucose spikes, and calories wasted on zero nutrition. Diet soda avoids the sugar problem but still delivers the carbonation issue. Neither is a good option on semaglutide.
Still water is always the best choice. If you miss the flavor variety, try adding lemon, lime, cucumber, fresh mint, or berries to still water. Herbal teas, both hot and iced, provide flavor without carbonation. Ginger tea specifically offers anti-nausea benefits that actively help counteract semaglutide side effects rather than making them worse.
Spicy and heavily seasoned foods
Hot peppers, cayenne, habanero sauce, sriracha, wasabi, horseradish, Thai chili dishes, Buffalo wings, curry pastes, and heavily seasoned foods with capsaicin or similar compounds. These irritate the gastric lining, which becomes more sensitive when food is sitting in the stomach for extended periods.
Under normal circumstances, spicy food passes through the stomach in two to four hours, and the irritation is temporary. On semaglutide, that spicy food sits against the stomach lining for six to eight hours. The prolonged contact increases the likelihood of heartburn, acid reflux, stomach pain, and nausea. Users frequently report that meals they previously enjoyed without issues, a favorite Thai curry, a plate of Buffalo wings, suddenly produce hours of burning discomfort.
Mild herbs and seasonings are perfectly fine. Basil, oregano, thyme, rosemary, garlic in moderate amounts, turmeric, and cumin add flavor without the aggressive irritation of hot spices. You do not have to eat bland food on semaglutide. You just need to shift from heat-based flavoring to herb-based flavoring.
If you love spicy food and want to test your tolerance, start with very small amounts after your body has fully adjusted to your current semaglutide dose. Some users find that mild to moderate spice becomes tolerable after the first three months, though tolerance varies significantly between individuals.
Alcohol
Beer, wine, cocktails, spirits, hard seltzer, and all alcoholic beverages. The relationship between alcohol and semaglutide is complicated, and the risks go beyond just feeling nauseous.
There is no direct pharmacological interaction between semaglutide and alcohol according to the FDA label. However, the practical effects of combining them create meaningful problems. Both semaglutide and alcohol lower blood sugar independently. Together, they can push glucose levels low enough to cause hypoglycemia, especially in people taking semaglutide for diabetes alongside other glucose-lowering medications. Symptoms of hypoglycemia, dizziness, confusion, shakiness, and sweating, overlap with symptoms of intoxication, making it difficult to recognize when blood sugar is dangerously low.
Beyond blood sugar, alcohol irritates the GI tract directly. It increases stomach acid production, inflames the gastric lining, and disrupts the balance of gut bacteria. On a stomach that is already processing food more slowly, these effects are amplified. Many semaglutide users report that even one or two drinks produce nausea, flushing, and GI discomfort far more intense than they experienced before starting the medication.
There is also the calorie consideration. A glass of wine contains roughly 125 calories. A craft beer runs 200 to 300. A margarita can hit 400. These are entirely empty calories, providing no protein, no fiber, and no micronutrients, while simultaneously irritating your digestive system and destabilizing your blood sugar. On a reduced-calorie intake, alcohol is one of the worst ways to spend your daily budget.
Many users find that semaglutide naturally reduces their desire to drink. Research suggests that GLP-1 receptor activation may modulate the brain reward pathways associated with alcohol consumption. If you notice this effect, let it work in your favor. If you choose to drink occasionally, keep it minimal, avoid sugary cocktails, never drink on an empty stomach, and monitor your blood sugar carefully.
Heavy dairy products
Full-fat cheese, heavy cream, cream cheese, butter in large amounts, ice cream, alfredo sauce, cheese-heavy dishes like macaroni and cheese, and cream-based soups. High-fat dairy creates the same delayed digestion problems as other fatty foods, with an additional twist.
Semaglutide can mimic or worsen lactose intolerance symptoms. The mechanism is straightforward. By slowing gastric emptying, the medication prolongs the time dairy products remain in the stomach, which increases fermentation. Lactose that would normally reach the small intestine for absorption in a reasonable timeframe instead sits and ferments, producing gas, bloating, cramping, and diarrhea. Some users who had no dairy sensitivity before semaglutide suddenly develop these symptoms.
Research also suggests that changes in gut motility can temporarily affect lactase enzyme activity, reducing the ability to break down lactose efficiently. This does not mean you have become permanently lactose intolerant. It means your digestive system is processing dairy differently while on the medication.
Low-fat and fermented dairy options tend to be tolerable for most users. Plain Greek yogurt, cottage cheese, and small amounts of hard cheese like parmesan or cheddar contain less lactose than soft cheeses and cream. These also provide valuable protein and calcium without the high fat content that compounds digestive issues. If dairy causes problems even in low-fat forms, consider switching to fortified plant-based alternatives for calcium and vitamin D.
Ultra-processed and packaged foods
Fast food meals, frozen dinners, instant noodles, packaged snack cakes, chips, hot dogs, chicken nuggets, processed deli meats, and anything with a lengthy list of artificial ingredients. Ultra-processed foods are engineered for taste and shelf life, not for your body to digest them efficiently.
These foods typically combine high fat, high sodium, refined carbohydrates, and artificial additives in a single product. On semaglutide, that combination creates a perfect storm of digestive problems. The fat slows processing. The sodium causes water retention and bloating. The refined carbs spike blood sugar. And the artificial additives can irritate the GI tract in ways that are difficult to predict.
Beyond the immediate digestive impact, ultra-processed foods waste your limited caloric budget. A frozen pizza at 800 calories provides roughly 15 grams of protein and minimal vitamins. Those same 800 calories from whole foods, grilled chicken, roasted vegetables, and quinoa, could deliver 60 grams of protein and a full spectrum of micronutrients. When every calorie counts, the quality gap between processed and whole foods becomes critical for maintaining muscle mass during weight loss and preventing nutritional deficiencies.
The simplest rule for semaglutide users: if the food comes in a box with a long ingredient list, put it back. If the food comes from the perimeter of the grocery store, produce, proteins, dairy, that is what belongs on your plate.
High-sodium foods
Restaurant meals in general, canned soups, soy sauce, processed meats, pickled foods, salted snacks, frozen meals, and condiments like ketchup, BBQ sauce, and salad dressings. Sodium does not directly interact with semaglutide, but it amplifies several side effects that the medication already promotes.
High sodium intake causes water retention, which worsens the bloated feeling that many semaglutide users already experience from delayed gastric emptying. It also increases thirst, which sounds manageable until you realize that many semaglutide users are already chronically dehydrated because the medication suppresses thirst alongside appetite. Drinking more water to offset sodium while simultaneously experiencing reduced thirst signals creates a hydration challenge that many people do not manage well.
Excess sodium can also raise blood pressure, which counteracts the cardiovascular benefits that semaglutide provides. Studies show that semaglutide improves several cardiovascular markers, but a high-sodium diet can negate some of those gains. For users taking semaglutide with cardiovascular health as a secondary goal, sodium management becomes particularly important.
Aim for under 2,300 milligrams of sodium per day, and ideally closer to 1,500 milligrams. Season food with herbs, spices, lemon juice, and vinegar instead of salt. When buying packaged products, check the nutrition label and choose lower-sodium options. Cooking at home gives you the most control over sodium content, which is another reason to minimize restaurant meals during the adjustment period.
Large portions of any food
This one catches people off guard. Even healthy food can cause problems if you eat too much of it in a single sitting. On semaglutide, your stomach capacity has effectively been reduced. Not physically, but functionally. It processes food so much more slowly that filling it to the same level as before creates excessive pressure and discomfort.
The line between satisfied and uncomfortably full becomes razor-thin. Users describe it as eating three more bites past comfortable and suddenly feeling nauseous for two hours. The margin for error is small, and the consequences of overeating are immediate and unpleasant.
Smaller, more frequent meals are the standard recommendation for a reason. Three moderate meals and one or two snacks distribute your food intake across the day, preventing the stomach from becoming overloaded at any single point. Aim to stop eating at about 70 to 80 percent of perceived fullness. That point where you feel neutral, not hungry but not stuffed, is the sweet spot. It takes practice to recognize, especially early in treatment, but learning to stop before fullness hits is one of the most effective strategies for managing semaglutide side effects.
Using smaller plates, eating more slowly, and putting utensils down between bites all help calibrate portion sizes naturally. These sound like generic diet tips, but on semaglutide, they are functional tools that directly prevent nausea and bloating.
Late-night eating
Eating within two to three hours of bedtime creates specific problems on semaglutide that go beyond general health advice about nighttime snacking. The medication already slows digestion. Lying down after eating removes gravity from the equation, which further slows the movement of food from the stomach into the small intestine.
The result is increased acid reflux, heartburn, and morning nausea. Food that has been sitting in the stomach all night creates a sensation of fullness and queasiness that can persist well into the following day. Some users report that late-night eating the previous evening makes them unable to eat breakfast, which then cascades into missed protein targets and inadequate nutrition for the entire day.
Try to finish your last meal at least three hours before lying down. If you must eat later, choose something small, light, and easily digestible. A few bites of Greek yogurt or a small handful of crackers is manageable. A full dinner at 10 PM is not.
What happens when you eat trigger foods on semaglutide
Understanding the cascade of events helps explain why avoiding certain foods is not just about comfort. It is about the effectiveness of your entire protocol.
The nausea cascade
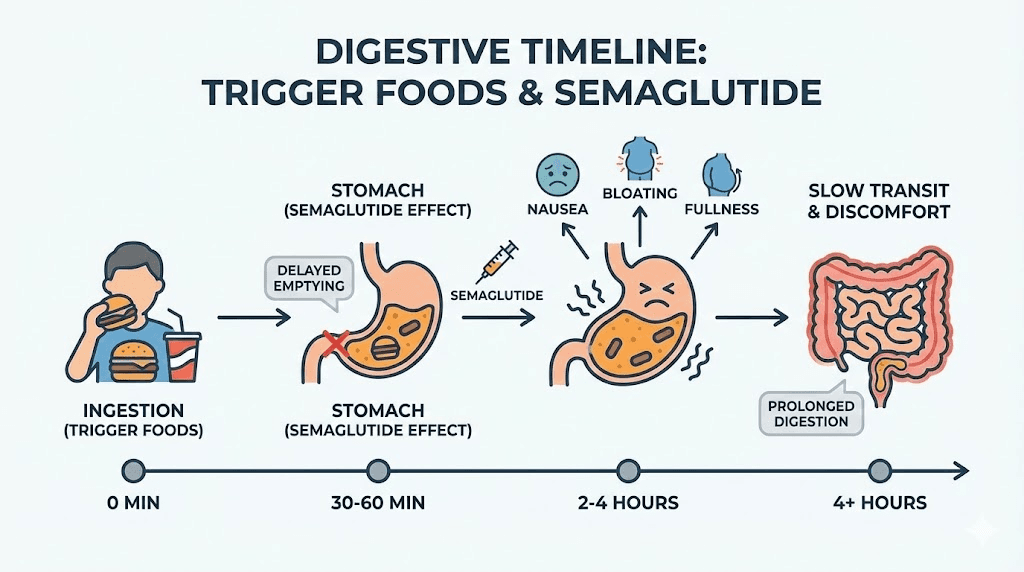
When you eat a high-fat meal on semaglutide, the following sequence unfolds. The food enters your stomach and encounters the drastically slowed gastric emptying. Fat, which already requires the most processing time of any macronutrient, sits in the stomach and begins to interact with gastric acid. The stomach walls stretch beyond comfortable levels because the food is not moving through at its normal rate. Stretch receptors in the stomach wall send signals to the brainstem, which semaglutide has already made more sensitive through direct GLP-1 receptor activation in the area postrema, the brain region that controls nausea and vomiting.
The nausea builds gradually, typically peaking two to three hours after eating. It can persist for four to six hours as the stomach slowly processes the meal. During this window, additional food intake feels impossible, which means your next meal gets skipped or delayed. Skipping meals creates its own problems, including fatigue, blood sugar instability, muscle catabolism, and nutrient deficiencies. One bad meal choice creates a ripple effect that disrupts the entire day.
The bloating mechanism
Bloating on semaglutide results from two overlapping processes. First, delayed gastric emptying causes food to remain in the stomach longer, where bacterial fermentation begins producing gas. Second, reduced gut motility means that gas produced throughout the digestive tract moves more slowly toward exit. The gas accumulates, distending the intestinal walls and creating that uncomfortable, puffy feeling that many users describe as their stomach looking visibly larger after eating.
Carbonated beverages add external gas to this already-compromised system. High-fiber foods, while generally healthy, can also produce excessive gas if introduced too quickly. The key is not eliminating all gas-producing foods but understanding that your baseline gas production is elevated on semaglutide, and anything that adds to it will be felt more acutely.
The constipation pathway
Constipation affects roughly 30 percent of semaglutide users. The mechanism is a direct consequence of slowed gut motility throughout the entire digestive tract, not just the stomach. When food and waste move more slowly through the colon, the body extracts more water from the stool, making it harder, drier, and more difficult to pass.
Refined carbohydrates and low-fiber diets worsen this dramatically. Without adequate fiber to add bulk and draw water into the stool, the constipation becomes chronic. Dehydration, which is common on semaglutide due to suppressed thirst and reduced food-based fluid intake, compounds the problem further. The constipation treatment strategies all center on increasing fiber gradually, maintaining aggressive hydration, and staying physically active.
The blood sugar rollercoaster
Sugary foods and refined carbohydrates create a specific pattern on semaglutide. The rapid glucose spike triggers an aggressive insulin response, partly mediated by the medication itself. Blood sugar drops sharply, often overshooting to the low side. This creates a crash that manifests as fatigue, irritability, shakiness, and intense hunger, the exact opposite of what you want from a medication designed to control appetite and stabilize energy.
Over time, these blood sugar fluctuations can reduce the perceived effectiveness of semaglutide. Users who eat sugar regularly often report that the medication feels like it has stopped working, when in reality their diet is undermining the stable metabolic environment the medication is trying to create. Eliminating sugary foods and refined carbs creates a steadier baseline that allows semaglutide to function at its maximum potential for weight loss and metabolic improvement.
Managing nausea through food avoidance: the strategic approach
Nausea is the most common semaglutide side effect, affecting up to 50 percent of users during dose escalation. But not all nausea is equal, and not all of it is inevitable. Strategic food avoidance can reduce nausea episodes by 40 to 60 percent based on clinician reports and user experiences.
The 48-hour injection window
Nausea peaks in the first 24 to 48 hours after each weekly injection. During this window, your dietary strategy should shift from normal eating to defensive eating. This means avoiding every food category on the avoid list with zero exceptions. Stick to bland, easily digestible foods. Plain crackers. Dry toast. Broth-based soups. Plain rice. Bananas. Applesauce. These BRAT-type foods minimize gastric workload during the period when your body is most sensitive.
Cold foods often work better than hot foods during this window because they produce less aroma. Warm food aromas can trigger nausea in sensitized individuals, and in the hours after injection, that sensitivity is at its peak. Chilled yogurt, cold protein shakes, smoothies, and cold fruit are all better tolerated than hot meals. If the sight or smell of cooking triggers queasiness, prepare meals in advance and eat them cold, or have someone else handle the cooking.
The ginger protocol
Ginger is not just a home remedy suggestion. It contains gingerols and shogaols, compounds with well-documented antiemetic properties that work through 5-HT3 receptor antagonism, the same mechanism used by prescription anti-nausea medications like ondansetron. For semaglutide users, ginger becomes a daily dietary tool rather than an occasional supplement.
Ginger tea throughout the day, especially in the first 48 hours post-injection, provides continuous mild anti-nausea support. Ginger chews before meals prime the stomach and reduce the likelihood of post-meal nausea. Fresh ginger sliced into hot water or added to smoothies delivers the active compounds in a food-based form. Crystallized ginger as a small snack provides quick relief during acute episodes.
The effective dose for anti-nausea benefit is roughly 250 milligrams to 1 gram of ginger four times daily. A standard cup of ginger tea delivers approximately 250 milligrams. Four cups spread across the day reaches the therapeutic range. This is a simple, safe, food-based intervention that meaningfully reduces one of the most disruptive semaglutide side effects.
Peppermint for digestive relief
Peppermint tea contains menthol, which relaxes smooth muscle in the GI tract and reduces the cramping and pressure that contribute to nausea and bloating. A cup after meals can help ease the digestive workload and provide relief within 15 to 20 minutes. Peppermint oil capsules, enteric-coated to reach the intestines, offer a more concentrated option for users with persistent GI discomfort.
The combination of ginger tea before meals and peppermint tea after meals creates a bookend strategy that addresses nausea from both directions. Prevention through ginger. Relief through peppermint. Neither has significant side effects or interactions with semaglutide, making them safe daily additions to your routine.
The dose escalation diet strategy
Your dietary approach should not remain static throughout your semaglutide protocol. Each dose increase resets your body adjustment, and your eating strategy needs to adapt accordingly. Most users follow a standard titration schedule: 0.25 mg for weeks one through four, 0.5 mg for weeks five through eight, 1.0 mg for weeks nine through twelve, and then maintenance at 1.0 to 2.4 mg depending on response.
Weeks one through four (0.25 mg): building the foundation
At this lowest dose, appetite suppression is mild and side effects are minimal for most people. This is not the time to be aggressive with food restriction. It is the time to build habits that will serve you when the dose increases and side effects become more pronounced.
Start eliminating the highest-risk foods now. Remove fried foods, carbonated drinks, and ultra-processed meals from your regular rotation. Begin tracking protein intake and targeting 1.2 to 1.5 grams per kilogram of body weight daily. Increase water intake to 64 to 100 ounces per day. Practice eating slowly, chewing thoroughly, and stopping before feeling full. These habits become critical at higher doses, and building them when the stakes are low makes them automatic when you need them most.
Use a semaglutide dosage calculator to confirm your titration schedule and ensure you are progressing at the right pace. Rushing dose increases without establishing dietary foundations is one of the most common reasons people experience severe side effects and consider discontinuing the medication.
Weeks five through eight (0.5 mg): tightening the approach
Appetite suppression becomes noticeable at this dose. You will start forgetting meals, feeling satisfied with smaller portions, and losing interest in foods that previously appealed to you. This is where the avoid list becomes critical.
Eliminate every food category on the avoid list strictly during the first week at the new dose. Side effects typically peak in the first three to five days after a dose increase, then gradually subside. During those peak days, default to the BRAT-style defensive eating approach. After the initial adjustment, you can cautiously reintroduce moderate amounts of complex carbohydrates, healthy fats, and mildly seasoned foods. But keep fried foods, sugary snacks, and carbonated drinks off the table permanently.
Protein intake becomes harder to maintain as appetite drops. This is when protein shakes and smoothies become essential tools rather than optional supplements. A scoop of protein powder blended with banana, spinach, and almond milk delivers 25 to 30 grams of protein in a form that most users tolerate even when solid food feels impossible. Keep protein powder stocked and accessible at all times.
Weeks nine through twelve (1.0 mg): the intensity peak
For many users, the jump to 1.0 mg produces the strongest side effects of the entire titration. Nausea may return with a vengeance. Appetite suppression can become so intense that eating feels like a chore rather than a pleasure. This is the phase where dietary discipline pays its biggest dividends.
Strictly follow the avoid list. Eat five to six very small meals per day rather than three larger ones. Every meal should start with protein. Keep ginger tea and bland backup foods readily available. If nausea prevents eating, liquid nutrition, protein shakes, broths, smoothies, becomes your primary food source until the side effects subside. Most people adapt within seven to fourteen days at the new dose, but those two weeks can be miserable without proper food management.
This is also the phase where weight loss often accelerates noticeably. The combination of stronger appetite suppression, reduced caloric intake, and improved insulin sensitivity creates rapid changes. Do not let poor food choices undermine this critical window. Every fried meal or sugary snack that triggers a nausea episode means missed nutrition and delayed progress.
Weeks thirteen and beyond: maintenance eating
Once you reach your maintenance dose and your body has fully adjusted, the strict defensive eating phase can relax somewhat. Most long-term semaglutide users develop an intuitive understanding of which foods their body handles well and which ones still cause problems.
The permanent avoid list for most maintenance users includes fried foods, excessive alcohol, sugary drinks, and ultra-processed meals. These categories rarely become well-tolerated even after months on the medication. Moderate amounts of healthy fats, mild spices, and complex carbohydrates typically become manageable again. Some dairy tolerance may return, particularly for fermented products like yogurt and aged cheese.
Continue monitoring portion sizes even on maintenance. The tendency to gradually increase portions as the body adapts is natural, but it undermines the caloric deficit that produces sustained weight loss results. Eat slowly, stop before fullness, and prioritize protein at every meal. These principles do not change regardless of your dose or how long you have been on the medication.
What to eat instead: the semaglutide-friendly food framework
Knowing what to avoid is only half the equation. You need to know what to put on your plate instead. The goal is nutrient density, easy digestibility, and maximum nutritional return per calorie.
Lean proteins that digest easily
Chicken breast, turkey breast, white fish like cod and tilapia, shrimp, eggs, plain Greek yogurt, cottage cheese, tofu, tempeh, and lentils. These provide the protein your body needs without the fat content that triggers nausea. Aim for 25 to 35 grams of protein per meal, and eat protein first before touching anything else on your plate.
White fish deserves special mention because it is the easiest animal protein to digest on semaglutide. Cod, tilapia, sole, and halibut are all extremely low in fat, high in protein, and gentle on the stomach. If meat in general feels difficult, start with white fish and build from there.
Non-starchy vegetables
Spinach, kale, broccoli, cauliflower, zucchini, bell peppers, cucumber, asparagus, green beans, tomatoes, and mushrooms. Cooked vegetables are generally better tolerated than raw on semaglutide because cooking breaks down the cellulose fiber that can cause gas and bloating. Roasting brings out natural sweetness that makes vegetables more appealing when appetite is low.
Start with well-cooked, soft vegetables and gradually introduce raw options as your digestive system adjusts. Raw salads can cause bloating in the early weeks due to the fiber volume and the mechanical work required to break them down. Steamed or roasted vegetables provide the same nutrients with less digestive effort.
Complex carbohydrates in moderate portions
Brown rice, quinoa, oats, sweet potatoes, and whole grain bread. Keep portions moderate, roughly half a cup of cooked grains per meal. Oats are particularly valuable at breakfast because they combine soluble fiber with a gentle texture that most semaglutide users tolerate well. Overnight oats softened in almond milk and mixed with protein powder create a high-protein, high-fiber breakfast that requires zero cooking and minimal stomach effort.
Healthy fats in small amounts
Quarter of an avocado, a tablespoon of olive oil, a small handful of nuts or seeds, or a serving of fatty fish like salmon once or twice per week. These provide essential fatty acids and fat-soluble vitamin absorption without the volume of fat that triggers digestive problems. The key word is small. A quarter avocado is fine. A whole avocado on toast is asking for trouble.
Hydrating foods and beverages
Still water, herbal teas, bone broth, watermelon, cucumber, oranges, and soups. Proper hydration is essential on semaglutide because the medication suppresses thirst alongside appetite. Many symptoms attributed to semaglutide side effects, headaches, fatigue, constipation, dizziness, are actually dehydration symptoms that resolve with adequate fluid intake. Aim for 64 to 100 ounces of total fluid daily.
Eating out on semaglutide: the restaurant survival guide
Restaurants present unique challenges for semaglutide users. Portions are large. Dishes are often high in fat, sodium, and refined carbohydrates. And the social pressure to order what everyone else is eating can override your best intentions. Here is how to navigate eating out without derailing your protocol.
Choose restaurants strategically
Some cuisines are inherently more semaglutide-friendly than others. Japanese restaurants offer grilled fish, steamed vegetables, and miso soup. Mediterranean restaurants feature grilled proteins, salads, and olive oil-based dishes. Poke bowl shops let you build exactly what your body needs. Mexican restaurants offer grilled chicken or fish with beans and vegetables, just skip the fried chips and heavy cheese.
Avoid restaurants where the entire menu revolves around fried food, heavy sauces, or massive portions. Burger joints, fried chicken chains, deep-dish pizza places, and all-you-can-eat buffets are the worst options for semaglutide users. The temptation alone makes disciplined eating difficult, and the available options rarely include anything that meets your nutritional needs.
Order modifications that work
Most restaurants will accommodate simple modifications. Ask for grilled instead of fried. Request sauce on the side. Substitute a side salad for French fries. Ask for steamed vegetables instead of the creamy side dish. These swaps are standard and servers handle them without issue.
Portion control requires more deliberate action. Ask for a to-go container when the meal arrives and immediately box up half. Or share an entree with someone else at the table. Or order an appetizer portion as your main course. On semaglutide, a restaurant appetizer-sized portion is often the right amount for a full meal.
Timing matters
If possible, schedule restaurant meals for days when you are furthest from your injection day. Side effects are typically lowest three to five days after injection, giving you the widest tolerance window for potentially challenging foods. Avoid eating out within 48 hours of your injection when nausea sensitivity is highest.
Eat a small, protein-rich snack before going to the restaurant. Arriving hungry leads to overordering and overeating. A handful of almonds or a few bites of Greek yogurt 30 minutes before takeoff takes the edge off and helps you make rational food choices rather than hunger-driven ones.
Alcohol at restaurants
Social pressure to drink at restaurants is real. If you choose not to drink while on semaglutide, sparkling water with lime in a cocktail glass looks identical to a gin and tonic. Nobody notices. Nobody asks. If you choose to have one drink, make it a glass of dry wine or a spirit with soda water, the lowest-calorie, lowest-sugar options available. Avoid cocktails with sugary mixers, beer with its carbonation and calorie load, and anything sweet.
Common food mistakes semaglutide users make
Even motivated, informed users fall into patterns that undermine their results. These are the mistakes that appear most frequently and the corrections that fix them.
Mistake 1: assuming healthy food cannot cause problems
A giant raw vegetable salad is healthy. But on semaglutide, the massive volume of raw fiber can cause hours of bloating and gas. A smoothie packed with fruits, nuts, seeds, and protein powder is nutrient-dense. But blending everything into a 600-calorie liquid meal can still overwhelm a slowed stomach. Healthy foods still need to follow the portion and preparation rules of semaglutide-friendly eating.
The fix: prepare healthy foods in smaller portions, prefer cooked over raw when digestive symptoms are active, and do not assume that a food being nutritious means it cannot cause GI distress.
Mistake 2: not eating enough on injection day
Some users avoid food entirely on injection day to prevent nausea. This backfires. An empty stomach can actually worsen nausea because gastric acid has nothing to work on and begins irritating the stomach lining directly. The result is a cycle of nausea, food avoidance, worsened nausea, and then either forcing food down while feeling terrible or going an entire day without adequate nutrition.
The fix: eat small amounts of bland, easily digestible food every two to three hours on injection day. Even if the portions are tiny, maintaining some food in the stomach gives the acid something to process and keeps nausea more manageable than total fasting.
Mistake 3: relying on sugar when nauseous
When nausea hits, the natural impulse is to reach for something that settles the stomach. For many people, that means crackers, toast, or ginger ale. The crackers and toast are fine, but reaching for sugary ginger ale, regular soda, or candy introduces sugar that spikes blood glucose and creates the rollercoaster effect described earlier. The nausea might subside temporarily from the ginger in ginger ale, but the sugar creates new problems 30 to 60 minutes later.
The fix: use ginger tea instead of ginger ale. Choose plain crackers or dry toast rather than sweetened options. If you need something beyond bland carbs, a few bites of banana provide gentle carbohydrates with potassium and natural sugars that digest more steadily than processed sugar.
Mistake 4: drinking liquids with meals
Drinking large amounts of liquid during meals adds volume to a stomach that is already processing food slowly. The extra liquid fills space, increases pressure, and can trigger the overfullness sensation that leads to nausea. Many semaglutide users do not realize that the water they are drinking with dinner is contributing to their post-meal discomfort.
The fix: drink water between meals rather than during them. Stop drinking 30 minutes before meals and wait 30 minutes after to resume. Small sips during eating are fine, but chugging a full glass of water alongside your dinner is counterproductive. This habit alone resolves post-meal bloating for many users.
Mistake 5: ignoring individual triggers
The avoid list provides general guidance, but individual tolerance varies significantly. Some users handle moderate spice perfectly well. Others cannot tolerate eggs without nausea. Some find that a specific vegetable, tomatoes, for example, causes problems that other vegetables do not. The general list gets you 80 percent of the way there, but the last 20 percent requires paying attention to your own body.
The fix: keep a simple food diary for the first four to six weeks of treatment. Note what you ate and how you felt one to three hours later. Patterns emerge quickly. Once you identify your personal trigger foods, add them to your personal avoid list regardless of whether they appear on the general recommendations. Your body is the final authority.
The relationship between food avoidance and long-term results
This is not just about comfort. The foods you avoid directly impact how much weight you lose, how much muscle you preserve, and how long you stay on semaglutide successfully.
Users who manage their diet carefully lose more fat and less muscle. Studies from the STEP trials show that roughly 40 percent of weight lost on semaglutide comes from lean body mass when protein intake is inadequate. Users who prioritize protein, eat nutrient-dense foods, and avoid the categories on this list lose predominantly fat. The dietary difference accounts for dramatically different body composition outcomes even at the same scale weight.
Side effect management through food avoidance also affects adherence. The most common reason people discontinue semaglutide is persistent GI side effects. When nausea, bloating, and constipation feel unmanageable, people stop the medication entirely. But these symptoms are highly responsive to dietary intervention. Users who understand and apply the food avoidance strategies described here are significantly more likely to stay on the medication long enough to achieve their goals.
SeekPeptides provides comprehensive nutrition frameworks designed specifically for GLP-1 users, with evidence-based guides that integrate dietary strategy with dosing protocols, supplement recommendations, and side effect management approaches. The combination of smart food avoidance, strategic nutrition, and proper protocol design creates outcomes that neither diet nor medication can achieve alone.
Supplements that help offset food restrictions
When you are avoiding multiple food categories, nutritional gaps can develop. Strategic supplementation fills those gaps without requiring you to eat foods that cause digestive problems.
A daily multivitamin covers baseline micronutrient needs when caloric intake is reduced. Look for one that includes vitamins A, C, D, E, K, B-complex, iron, zinc, and selenium. Take it with food to improve absorption and reduce stomach upset.
Vitamin D at 2,000 to 4,000 IU daily supports bone health, immune function, and mood. Most adults are deficient regardless of diet, and reduced food intake on semaglutide makes the gap wider.
Magnesium citrate at 200 to 400 milligrams before bed addresses constipation and muscle cramps simultaneously. It also supports sleep quality, which many semaglutide users report is disrupted during dose escalation.
Omega-3 fatty acids at 1,000 to 2,000 milligrams of combined EPA and DHA daily support cardiovascular health and reduce inflammation. If you are avoiding fatty fish due to digestive concerns, supplementation becomes essential to maintain adequate omega-3 intake.
Vitamin B12 at 1,000 to 2,500 micrograms daily is particularly important if you are also taking metformin, which depletes B12. Many compounded semaglutide formulations include B12 already, so check your formulation before adding a separate supplement.
Fiber supplements like psyllium husk can help if your reduced food intake makes it difficult to reach 25 to 35 grams of dietary fiber daily. Start with one teaspoon and increase gradually to avoid worsening bloating. Always take fiber supplements with a full glass of water.
When food avoidance is not enough: recognizing serious symptoms
Most semaglutide side effects are manageable through dietary modification. But some symptoms require medical attention rather than a diet adjustment. Know the difference.
Persistent vomiting that prevents keeping any food or water down for more than 24 hours requires medical evaluation. This can lead to dehydration and electrolyte imbalances that become dangerous.
Severe abdominal pain that is sharp, localized, or accompanied by fever could indicate pancreatitis, a rare but serious semaglutide side effect. Do not dismiss significant abdominal pain as a normal GI reaction.
Signs of severe dehydration including dark urine, dizziness upon standing, rapid heartbeat, and confusion need immediate attention, especially if vomiting or diarrhea has been persistent.
Symptoms of hypoglycemia including shakiness, sweating, confusion, and rapid heartbeat, particularly after alcohol consumption or missed meals, require quick action with glucose tablets or juice and may indicate a need to adjust your medication or concurrent diabetes treatment.
The dietary strategies in this guide address the common, mild to moderate side effects that most semaglutide users experience. They are not substitutes for medical evaluation of unusual or severe symptoms. When in doubt, contact your healthcare provider. The line between normal adjustment side effects and concerning symptoms is not always obvious, and it is always better to check than to dismiss something important.
Frequently asked questions
Can I ever eat fried food again on semaglutide?
Most users find that small amounts of fried food become tolerable after three to six months on a stable maintenance dose. However, the tolerance is typically lower than it was before the medication. A few fried items occasionally may be manageable, but a full fried meal is likely to cause problems for as long as you remain on semaglutide.
Is coffee safe on semaglutide?
One to two cups of coffee per day is fine for most users. Avoid adding sugar and heavy cream. Black coffee or coffee with a splash of milk is best. Caffeine has a mild diuretic effect, so compensate with additional water. Some users find that coffee on an empty stomach worsens nausea, so eat something small beforehand or switch to lower-acid coffee options.
Why does food taste different on semaglutide?
Some users report altered taste perception, including foods tasting more bland, overly sweet, or metallic. This appears to result from GLP-1 receptor activation affecting taste bud signaling and altered gut-brain communication. The change is usually temporary and resolves as your body adjusts to the current dose. It may return briefly with each dose increase.
How do I get enough protein when nothing sounds appealing?
Liquid protein is the answer when solid food feels impossible. Protein shakes, smoothies with protein powder, bone broth, and even Greek yogurt-based smoothies deliver high protein in a form that most users tolerate even during peak nausea. Keep protein shake supplies stocked at all times so you always have a backup when solid food is not happening.
Should I eat differently on injection day?
Yes. Keep meals smaller and blander on injection day and for 24 to 48 hours afterward. Focus on easily digestible proteins, plain carbohydrates, and gentle foods. Avoid everything on the high-risk avoid list during this window. Some users find that injecting in the evening allows them to sleep through the initial peak of side effects.
Can I eat fruit on semaglutide?
Most fruits are fine in moderate portions. Berries, apples, bananas, and citrus fruits provide vitamins, fiber, and natural sugars that digest more steadily than processed sugar. Avoid large quantities of high-sugar tropical fruits like mangoes and pineapple, which can spike blood sugar. Dried fruits are calorie-dense and high in sugar concentration, so limit those as well. Fresh, whole fruit in moderate portions is one of the best snack options on semaglutide.
Do the food restrictions change if I am on compounded semaglutide versus brand-name?
The food avoidance guidelines apply equally regardless of whether you are taking compounded semaglutide, Ozempic, Wegovy, or Rybelsus. The active ingredient is the same, and the mechanism of delayed gastric emptying is identical. The only difference may be in formulation additions like B12 in compounded versions, which do not change the dietary recommendations.
How long do dietary restrictions last on semaglutide?
The strictest avoidance is needed during the first eight to twelve weeks of treatment and for one to two weeks after each dose increase. After your body fully adjusts to your maintenance dose, most users can relax restrictions somewhat while keeping the highest-risk categories, fried foods, sugary drinks, excessive alcohol, permanently limited. The core principles of prioritizing protein, eating smaller portions, and choosing whole foods over processed foods should continue for the entire duration of treatment and beyond.
External resources
For researchers serious about optimizing their semaglutide protocols, SeekPeptides offers the most comprehensive resource available, with evidence-based nutrition guides, side effect management strategies, and a community of thousands who have navigated these exact dietary challenges successfully.
In case I do not see you, good afternoon, good evening, and good night. May your meals stay gentle, your nausea stay manageable, and your results stay consistent.