Feb 19, 2026

You are losing muscle. Right now. With every pound that drops on the scale, somewhere between 25% and 40% of that weight is coming from lean tissue, not fat. That is the hidden cost of GLP-1 medications that most guides gloss over, and it is the reason protein shakes have become the single most important dietary tool for anyone on semaglutide or tirzepatide.
Think about what that means in real numbers. Lose 30 pounds on a semaglutide protocol, and between 7.5 and 12 pounds of that could be muscle. That is not cosmetic. Muscle drives your metabolism, protects your joints, keeps your bones dense, and determines whether you maintain your weight loss or regain everything the moment you stop treatment. The STEP 1 trial found that semaglutide users lost an average of 6.92 kg of lean mass, a 13.2% reduction. The SURMOUNT-1 trial showed tirzepatide users lost 5.67 kg of lean mass. These are not small numbers.
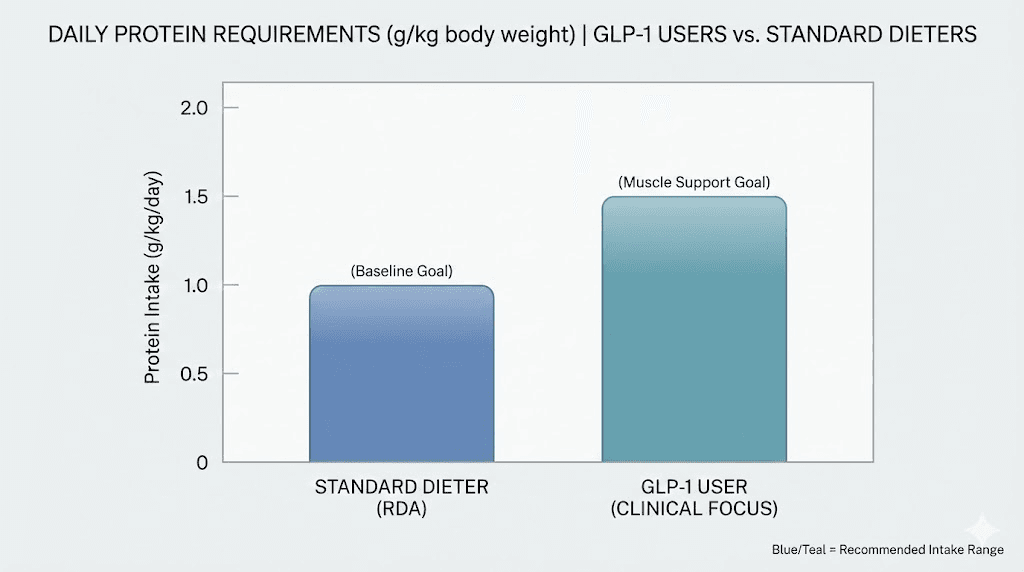
But here is the part nobody talks about enough. You can fight back. Higher protein intake, specifically 1.2 to 1.6 grams per kilogram of body weight per day, has been shown to significantly reduce muscle loss during GLP-1 therapy. And for most people on these medications, protein shakes are the most practical way to hit those targets when your appetite has vanished and the thought of chewing through a chicken breast makes your stomach turn.
This guide covers everything. Which protein shakes work best with GLP-1 medications. How to time them around your injections. What to look for, what to avoid, and how to build a protein strategy that preserves every ounce of muscle while your body sheds fat. SeekPeptides members have been navigating these exact questions, and the protocols that work are more specific than you might expect.
Why protein matters more on GLP-1 medications than any other weight loss approach
GLP-1 receptor agonists create a unique nutritional challenge. They suppress appetite dramatically. They slow gastric emptying. They reduce total caloric intake by 20% to 40% in most users. And while that drives impressive fat loss, it also creates a caloric deficit so severe that your body starts breaking down muscle for energy unless you actively prevent it.
This is not the same as dieting without medication. On a standard calorie-restricted diet, you can usually eat enough protein by simply choosing the right foods. But when semaglutide suppresses your appetite to the point where you struggle to eat 1,000 calories a day, hitting 100 to 130 grams of protein through whole foods alone becomes nearly impossible. The math just does not work.
A joint advisory from the American College of Lifestyle Medicine, the American Society for Nutrition, the Obesity Medicine Association, and the Obesity Society specifically recommends protein intake of 1.2 to 1.6 g/kg/day for people on GLP-1 medications. For a 180-pound person, that translates to roughly 98 to 131 grams of protein daily. For someone who can barely finish half a meal, that number feels enormous.
The muscle loss problem in clinical trials
The data from clinical trials is sobering. In the STEP 1 trial, participants on semaglutide 2.4 mg lost an average of 14.9% of their body weight. But a deeper look at the body composition data reveals that lean mass accounted for 45.2% of the total weight lost. Nearly half. That means for every 10 pounds on the scale, almost 5 were muscle, organ tissue, or bone density.
Tirzepatide performed somewhat better. In SURMOUNT-1, lean mass made up about 25.7% of total weight lost. Still significant, but the dual GIP/GLP-1 mechanism appears to offer some muscle-sparing advantage compared to pure GLP-1 agonists like semaglutide.
Here is the critical nuance though. While absolute lean mass decreased in both trials, the proportion of lean mass relative to total body mass actually increased. In STEP 1, the lean-to-total body mass ratio improved by 3.0 percentage points. Your body was becoming proportionally leaner, even though it was losing some muscle in absolute terms. The goal of protein supplementation is to push that equation further, preserving as much absolute lean mass as possible while maximizing fat loss.
How protein prevents muscle breakdown
Protein does three things that matter during GLP-1 therapy.
First, it provides amino acids for muscle protein synthesis. Your muscles are constantly being broken down and rebuilt. When you are in a calorie deficit, the breakdown accelerates. Adequate protein, particularly leucine-rich protein, signals your body to prioritize muscle rebuilding even during energy restriction. The muscle protein synthesis threshold sits at roughly 25 to 40 grams of high-quality protein per meal.
Second, protein has the highest thermic effect of any macronutrient. Your body burns approximately 20% to 30% of protein calories just digesting and metabolizing them, compared to 5% to 10% for carbohydrates and 0% to 3% for fats. This means protein calories are metabolically more expensive, which supports fat loss while preserving muscle.
Third, protein is the most satiating macronutrient. Even on GLP-1 medications that already suppress appetite, protein helps you feel more satisfied with smaller portions. This matters because it means you are less likely to fill your limited appetite with empty calories from processed carbohydrates or sugars that contribute nothing to muscle preservation.
How much protein you actually need on GLP-1 medications
The numbers vary depending on your body weight, activity level, and which medication you are using. But the research points to a clear range.
Minimum for muscle preservation: 1.2 g/kg of body weight per day. This is the floor. Below this, you are almost certainly losing more muscle than necessary.
Optimal for active individuals: 1.6 g/kg of body weight per day. If you are doing any form of resistance training or exercise, this is your target.
For serious athletes or heavy resistance trainers: 1.6 to 2.2 g/kg of body weight per day. The higher end applies to those doing intense strength training 3 or more times per week.
Let me put that in practical terms.
A 150-pound (68 kg) person needs 82 to 109 grams of protein daily at the standard range. A 200-pound (91 kg) person needs 109 to 146 grams. A 250-pound (113 kg) person needs 136 to 181 grams.
Those numbers are achievable with whole foods when your appetite is normal. But on semaglutide or tirzepatide, where most people struggle to eat more than two small meals per day? That is where protein shakes become essential, not optional.
The 25-40 gram per meal rule
Research on muscle protein synthesis shows that your body can only effectively use about 25 to 40 grams of protein at once for muscle building. Eating 80 grams in one sitting does not produce twice the muscle-preserving effect of 40 grams. It simply gets oxidized for energy or converted to glucose.
This means distribution matters. Three to four protein-rich meals or snacks spread throughout the day, each containing 25 to 40 grams, is far more effective than trying to cram all your protein into one massive meal. For GLP-1 users who can barely manage two meals, adding one or two protein shakes between meals solves the distribution problem elegantly.
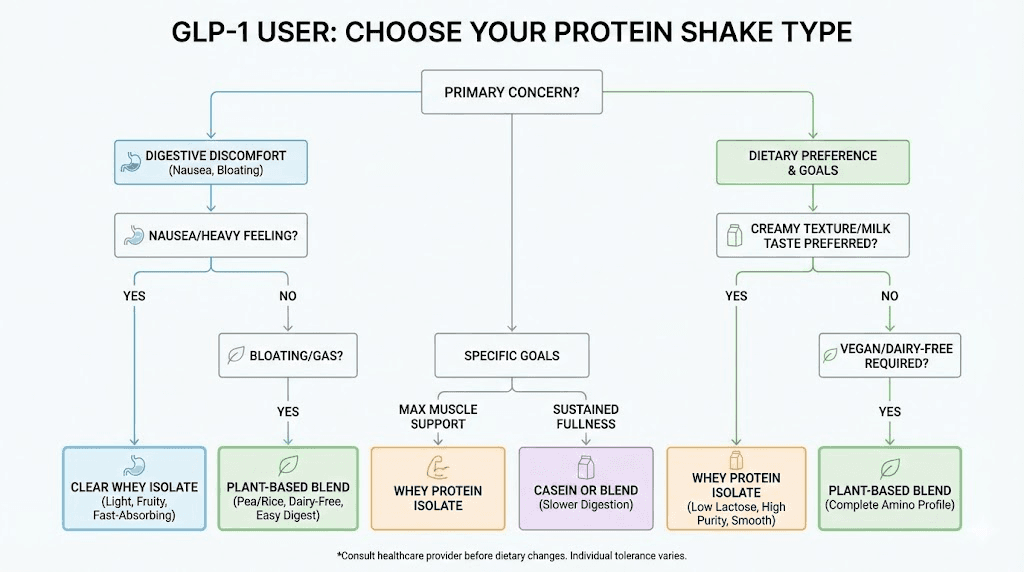
Choosing the right protein shake for GLP-1 users
Not all protein shakes are created equal, and this matters more for GLP-1 users than for anyone else. The medication slows gastric emptying, which means anything heavy, fatty, or fiber-dense will sit in your stomach longer than usual. The wrong protein shake can trigger nausea, bloating, and gastrointestinal discomfort that makes you avoid protein altogether.
Whey protein isolate: the gold standard
Whey protein isolate is the most recommended option for GLP-1 users, and for good reason. It has the highest bioavailability of any protein source, meaning your body absorbs and uses a higher percentage of the protein compared to other sources. It is rich in leucine, the amino acid most critical for triggering muscle protein synthesis. And it digests relatively quickly, which is important when your stomach is already emptying slowly from the medication.
Look for whey isolate specifically, not whey concentrate. Isolate has been filtered to remove most of the lactose and fat, making it easier on the digestive system. This distinction matters because GLP-1 medications amplify digestive sensitivity. What you tolerated fine before starting semaglutide might now cause bloating, cramping, or nausea.
Hydrolyzed whey isolate takes this one step further. The protein has been partially broken down (pre-digested), which means your body has to do less work to absorb it. For anyone experiencing significant gastrointestinal side effects, hydrolyzed whey is often the best-tolerated option.
Plant-based protein: when dairy is not an option
If you cannot tolerate dairy, or if you follow a plant-based diet, you have solid alternatives. But you need to be strategic about which ones you choose.
Pea protein is the most popular plant-based option for GLP-1 users. It has a complete amino acid profile, decent leucine content, and is generally well-tolerated. Soy protein isolate is another strong choice, with research showing comparable GLP-1 secretion responses to whey and casein when stomach emptying rates are similar.
Rice protein on its own has a lower leucine content, but blended rice-pea protein powders address this limitation. The combination provides a more complete amino acid profile that approaches whey in terms of muscle-building potential.
The key difference between plant and animal proteins for GLP-1 users comes down to leucine. Whey protein delivers approximately 2.5 grams of leucine per 25-gram serving. Most plant proteins deliver 1.5 to 2 grams per equivalent serving. Since leucine is the primary trigger for muscle protein synthesis, plant-based protein users may need slightly higher total protein intake to compensate, roughly 10% to 15% more.
Clear whey isolate: the nausea-friendly option
Clear whey isolate has become increasingly popular among semaglutide and tirzepatide users specifically because it does not look, taste, or feel like a traditional milkshake-style protein shake. It mixes with water to create a juice-like drink that is significantly easier to consume when nausea is present.
The advantages are real. No thick, creamy texture that triggers gag reflexes during peak nausea days. No dairy taste that many GLP-1 users report becoming aversive. And because it is a whey isolate, the protein quality and amino acid profile remain excellent.
The downside? Clear whey isolates tend to contain more artificial sweeteners and flavoring to achieve that juice-like taste. If you are sensitive to artificial sweeteners (which some GLP-1 users report), look for brands that use stevia or monk fruit instead of sucralose or aspartame.

Collagen peptides: useful but not a replacement
Collagen peptides have gained popularity in the GLP-1 community because they dissolve easily, have almost no taste, and can be mixed into nearly anything, coffee, soups, smoothies, even water. For people who cannot stomach a full protein shake, collagen seems like an easy solution.
But there is a significant limitation. Collagen peptides are not a complete protein. They lack tryptophan entirely and are low in several other essential amino acids, including leucine. This makes them poor drivers of muscle protein synthesis compared to whey, casein, or even soy.
Use collagen peptides as a supplement to your primary protein strategy, not a replacement. Adding 10 to 15 grams of collagen to your morning coffee gives you extra protein grams toward your daily target and supports joint, skin, and bone health, all of which matter during rapid weight loss. But your core protein intake should come from complete protein sources.
Casein protein: the slow-release option
Casein digests slowly, forming a gel in your stomach that releases amino acids over several hours. This sounds ideal for overnight muscle preservation, but for GLP-1 users, the slow digestion is a double-edged sword.
Because GLP-1 medications already slow gastric emptying, adding a slow-digesting protein can compound the feeling of fullness and potentially worsen nausea. Some users tolerate casein well, particularly as a nighttime shake consumed several days after their weekly injection when GI side effects are minimal. Others find it sits like a brick in their stomach.
If you want to try casein, start with half a serving mixed in a large volume of water. Sip it slowly over 30 to 45 minutes. If you tolerate it, a casein shake before bed can provide a steady stream of amino acids during your overnight fasting period, which is when muscle breakdown peaks.
What to look for in a GLP-1-friendly protein shake
The ideal protein shake for someone on semaglutide or tirzepatide looks very different from what a typical gym-goer might choose. Here is what to prioritize.
Protein content: 20-30 grams per serving
You want enough protein per serving to trigger muscle protein synthesis (minimum 20 grams) without so much total volume or calories that it overwhelms your suppressed appetite. Shakes with 20 to 30 grams per serving hit this sweet spot. Anything higher per single serving risks sitting too heavy, especially on injection days.
Low fat: 5 grams or less per serving
Fat slows digestion. Your medication is already slowing digestion. Combining the two can cause significant discomfort. Look for protein shakes with 5 grams of fat or less per serving. This rules out many mass-gainer shakes, meal replacement shakes, and protein blends designed for bulking.
Low sugar: 5 grams or less per serving
Many GLP-1 users, particularly those with prediabetes or type 2 diabetes, need to monitor their blood sugar carefully. Lower-sugar formulations, generally around 5 grams per serving or less, help maintain glycemic control. This is especially important because semaglutide itself affects blood glucose levels, and adding a sugar-heavy shake can cause unpredictable blood sugar spikes.
Calorie count: under 200 calories per serving
When your total daily intake might be 800 to 1,200 calories, you cannot afford to spend 300 to 400 of them on a single shake. Look for shakes in the 100 to 200 calorie range per serving. This gives you the protein you need without consuming a huge proportion of your limited daily calories.
Fiber content: moderate (3-6 grams)
Some fiber is beneficial. It feeds your gut microbiome, supports regular bowel movements (important since constipation is a common GLP-1 side effect), and adds minimal bulk. But too much fiber in a protein shake can worsen the bloating and fullness that GLP-1 medications already cause. Aim for 3 to 6 grams per serving, not the 10 to 15 grams found in some high-fiber meal replacement shakes.
Minimal artificial additives
GLP-1 medications change how your body responds to various food additives. Some users report increased sensitivity to artificial sweeteners, sugar alcohols, and certain thickeners. If you notice that protein shakes cause more GI distress than expected, try switching to a simpler formula with fewer additives. Unflavored protein powder mixed with your own ingredients gives you the most control.
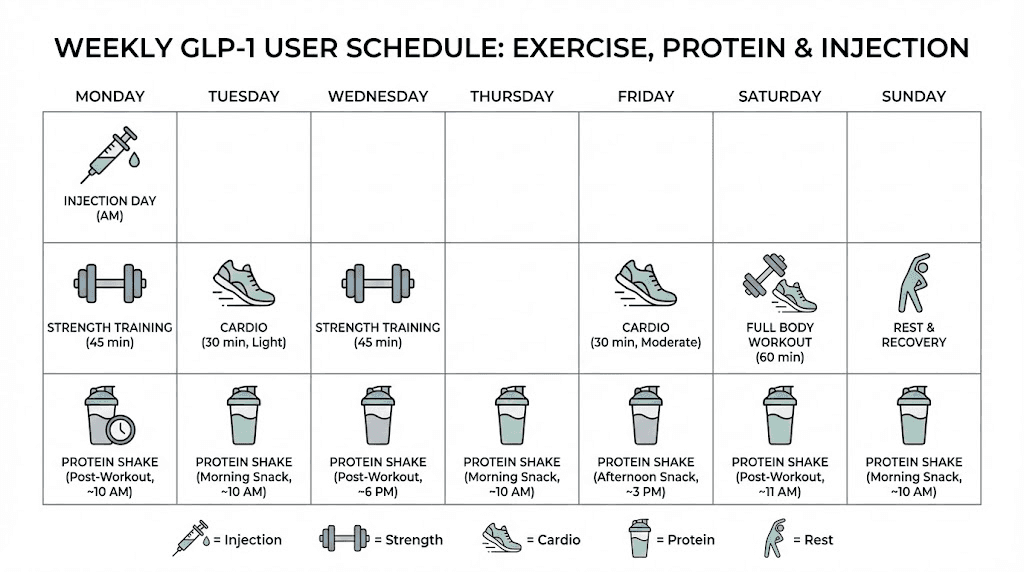
Timing your protein shakes around GLP-1 injections
Timing matters more than most people realize. The nausea, reduced appetite, and slowed gastric emptying from GLP-1 medications follow a predictable pattern throughout the week, and smart protein timing can work with these fluctuations rather than against them.
The weekly tolerance cycle
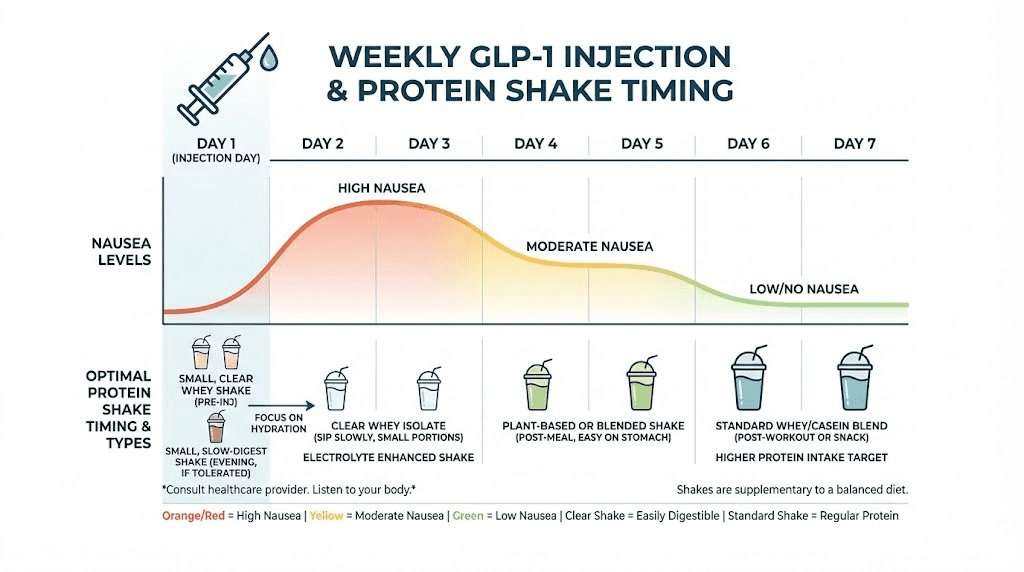
Most GLP-1 users experience a predictable pattern of side effects throughout their dosing week.
Days 1-2 post-injection: Peak medication levels. Strongest appetite suppression. Highest nausea risk. This is when protein shakes are most important because whole food intake is often at its lowest, but also when tolerance is worst.
Days 3-5 post-injection: Medication still active but side effects moderating. Most users find this is when protein shakes are easiest to consume. This is your window to maximize protein intake.
Days 6-7 post-injection: Medication waning. Appetite starts returning. Some users can eat more whole food protein during this period, reducing their reliance on shakes.
Injection day strategy
On the day of your GLP-1 injection, consume your protein shake before your injection if possible. Many users inject in the evening, so having a shake in the morning or early afternoon gives you a protein dose before nausea peaks. If you inject in the morning, try to have a small protein shake 30 to 60 minutes before the injection.
After the injection, stick to clear liquids if nausea is present. Clear whey isolate mixed with water is often tolerated better than creamy shakes during this period.
Peak nausea days strategy
During your worst nausea days (typically 24 to 48 hours post-injection), consider these approaches.
Sip a diluted protein shake slowly over 30 to 60 minutes instead of drinking it all at once. Use half the powder in twice the liquid volume. Choose clear whey isolate or unflavored collagen mixed into broth or ginger tea. Or try frozen protein shake popsicles, which are often better tolerated than liquid shakes because cold temperatures can help manage nausea.
Some tirzepatide users find that eating a few plain crackers or a small piece of fruit 10 to 15 minutes before their protein shake reduces nausea significantly. The small amount of simple carbohydrate seems to settle the stomach enough to tolerate the protein.
The 30-60 minute liquid-meal buffer
If you are consuming protein shakes alongside solid food meals, leave a 30 to 60 minute buffer between liquids and meals. Drinking a protein shake immediately before or during a solid food meal can amplify the feeling of excessive fullness and slow down digestion further. Have your shake as a separate mini-meal between your main meals.
Building a daily protein shake protocol for GLP-1 users
Theory is useful. Protocols are actionable. Here are specific approaches based on your daily calorie and protein targets.
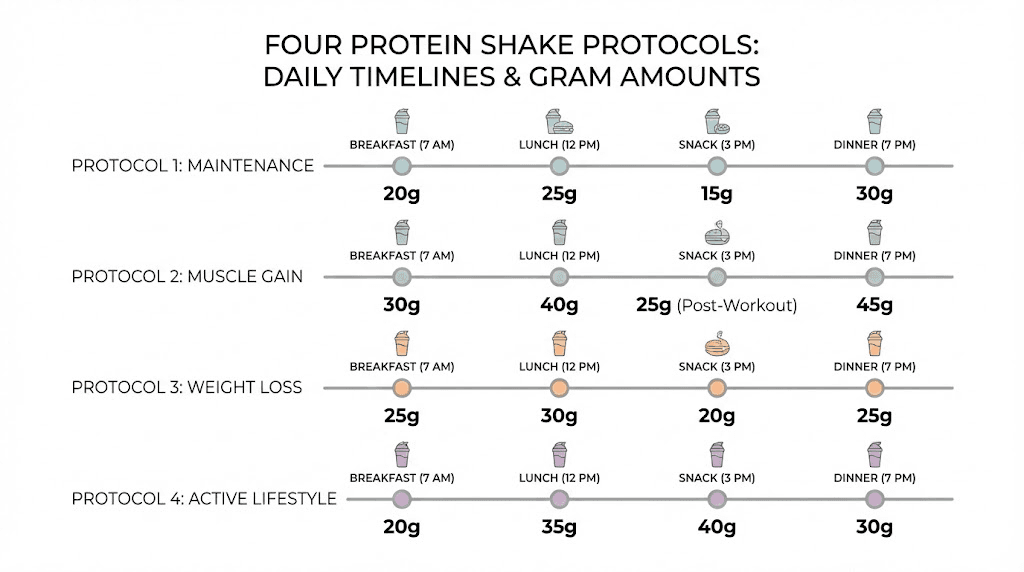
Protocol 1: the minimum effective approach (for severe appetite suppression)
Goal: Hit 80-100 grams of protein daily when whole food intake is extremely limited.
Daily protein shake schedule:
Morning (8-9 AM): 1 scoop whey isolate (25g protein) in 10-12 oz water. Sip over 20-30 minutes.
Afternoon (2-3 PM): 1 scoop whey isolate or plant protein (25g protein) in 10-12 oz water or almond milk.
With meals: 30-50g protein from whatever whole food you can manage (eggs, Greek yogurt, chicken, fish).
Total daily protein: 80-100 grams from shakes plus food. Total shake calories: approximately 200-260. Best for: First 4-8 weeks on medication when appetite suppression is most severe. Also works for dose escalation periods when side effects intensify.
Protocol 2: the balanced approach (moderate appetite suppression)
Goal: Hit 100-130 grams of protein daily with a mix of shakes and whole foods.
Daily protein shake schedule:
Morning (7-8 AM): 1 scoop whey isolate (25g protein) blended with 1/2 banana, ice, and 8 oz almond milk. Sip over 15-20 minutes.
Post-workout or afternoon (2-4 PM): 1 scoop clear whey isolate (22-25g protein) in 12 oz cold water.
Meals (lunch and dinner): 25-40g protein each from whole food sources.
Total daily protein: 100-130 grams. Total shake calories: approximately 250-350. Best for: Weeks 8-16 on medication when appetite has stabilized somewhat. Works well for users doing light to moderate exercise.
Protocol 3: the active approach (for resistance trainers)
Goal: Hit 130-160 grams of protein daily to support muscle building during weight loss.
Daily protein shake schedule:
Morning (7 AM): 1.5 scoops whey isolate (37g protein) with water or almond milk.
Post-workout (within 1 hour of training): 1 scoop whey isolate (25g protein) in water. Fast-digesting post-training.
Evening (8-9 PM): 1 scoop casein protein (25g protein) in 10 oz water. Slow release overnight. Only on days when GI tolerance is good (days 4-7 of dosing cycle).
Meals: 25-40g protein each from lean whole food sources, 2-3 meals daily.
Total daily protein: 130-160 grams. Total shake calories: approximately 350-450. Best for: Experienced GLP-1 users who have adapted to side effects and are doing regular strength training to maximize body recomposition.
Protocol 4: the plant-based approach
Goal: Hit 100-140 grams of protein daily without any animal products.
Daily protein shake schedule:
Morning: 1.5 scoops pea-rice blend protein (35g protein) in oat milk with a tablespoon of nut butter.
Afternoon: 1 scoop soy protein isolate (25g protein) in water with half a banana.
Evening: 15g collagen peptides in herbal tea or broth (joint and skin support, not complete protein).
Meals: Tofu, tempeh, edamame, lentils targeting 25-40g per meal.
Total daily protein: 100-140 grams. Best for: Vegans and vegetarians on GLP-1 therapy who need a comprehensive protein strategy. Note: aim for 10-15% higher total protein than omnivore targets to compensate for lower leucine content in plant proteins.
Managing common problems with protein shakes on GLP-1 medications
Even the best protein shake strategy runs into practical challenges when combined with GLP-1 medications. Here is how to handle the most common ones.
Problem: protein shakes trigger nausea
This is the most common complaint, especially during the first few weeks or after dose increases. Nausea affects 17% to 25% of GLP-1 users, and thick, creamy protein shakes can make it worse.
Solutions:
Switch to clear whey isolate. The juice-like consistency is dramatically easier to tolerate than milkshake-style shakes.
Dilute your shake. Use double the recommended liquid for a thinner consistency. You are getting the same protein in a less concentrated form.
Serve it cold. Cold temperatures suppress the gag reflex and reduce nausea perception. Blend your shake with ice or freeze it into popsicles.
Sip slowly. Drink your shake over 30 to 60 minutes instead of gulping it down. Your slowed gastric emptying needs time to process each sip.
Try unflavored protein in savory applications. Mix unflavored whey isolate into chicken broth, miso soup, or tomato soup. The savory flavors can be more tolerable than sweet when nausea is present.
Problem: protein shakes cause bloating
Bloating is common on GLP-1 medications regardless of protein shake use. But certain shake ingredients make it worse.
Solutions:
Avoid sugar alcohols (erythritol, sorbitol, xylitol, maltitol). These are common in low-calorie protein shakes and powders, and they cause significant gas and bloating, especially with already-slowed digestion.
Choose whey isolate over concentrate. Concentrate contains lactose that many people do not digest efficiently. Isolate removes most of the lactose.
Skip high-fiber protein shake formulas. While fiber is generally healthy, the combination of fiber, protein, and GLP-1-induced slow gastric emptying creates a bloating perfect storm.
Take a digestive enzyme with your shake. A broad-spectrum digestive enzyme containing protease (for protein), lactase (if using dairy), and lipase (for any fats) can significantly reduce bloating.
Problem: you cannot finish a full serving
This is incredibly common. The appetite suppression from semaglutide can be so profound that even a 10-ounce protein shake feels like a Thanksgiving dinner.
Solutions:
Split one serving into two half-servings consumed 2 to 3 hours apart. You get the same total protein, just in smaller doses that your stomach can handle.
Use higher-protein-per-ounce formulas. Some protein powders pack 25 to 30 grams of protein into just 6 to 8 ounces of liquid when mixed. Less volume, same protein.
Make protein-enriched foods instead of drinks. Mix unflavored protein powder into oatmeal, yogurt, pudding, or mashed potatoes. You get the protein without the liquid volume that triggers fullness.
Problem: taste aversion to protein shakes
GLP-1 medications can change how things taste. Foods and drinks you loved before may now taste too sweet, too rich, or just plain wrong. Many users develop specific aversions to chocolate or vanilla protein shakes they previously enjoyed.
Solutions:
Rotate flavors weekly. Do not commit to one flavor in bulk. Buy sample packs or smaller containers until you know what your medication-altered palate prefers.
Try fruit-flavored clear whey. Berry, citrus, and tropical flavors often work better than traditional dessert flavors when taste perception has changed.
Go unflavored. Unflavored whey isolate has almost no taste and can be mixed into any food or drink without altering the flavor significantly.
Consider the temperature. Some users find that flavors they dislike cold taste fine when mixed warm (like vanilla in coffee) or frozen (like a chocolate protein popsicle).
Protein shakes versus whole food protein: when to use each
Protein shakes are not a replacement for whole food protein. They are a supplement, a tool to fill the gap between what you eat and what your muscles need. Understanding when to rely on shakes versus whole food helps you build the most effective strategy.
When protein shakes are the better choice
Use protein shakes when your appetite is severely suppressed, typically days 1-3 of your dosing cycle. Use them when nausea prevents you from eating solid food. Use them as a post-workout recovery tool when solid food would sit too heavy. Use them when you are traveling and access to high-quality protein sources is limited. And use them anytime you have fallen short on protein for the day and need a quick, efficient way to catch up.
When whole food protein is better
Whenever you can tolerate solid food, prioritize it. Whole food protein comes packaged with other nutrients that shakes lack: iron from red meat, omega-3s from fish, calcium from dairy, fiber from legumes. These micronutrients matter more during GLP-1 therapy because your total food intake is so reduced that every calorie needs to deliver maximum nutritional value.
Whole food protein also requires chewing, which triggers digestive enzyme release and improves nutrient absorption. The mechanical act of eating sends satiety signals to your brain that liquid calories do not produce as effectively.
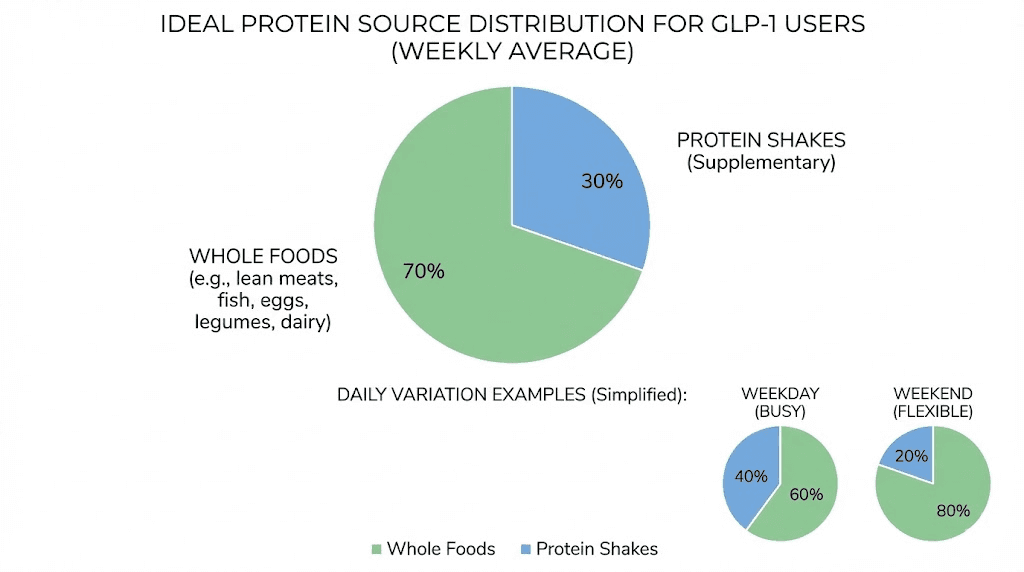
The ideal ratio
For most GLP-1 users, aim for approximately 60% to 70% of daily protein from whole foods and 30% to 40% from protein shakes. On severe nausea days, that ratio might flip to 30% whole food and 70% shakes. On your best tolerance days, you might manage 80% whole food and 20% shakes.
The point is flexibility. Listen to your body. On days when you can eat, eat real food. On days when you cannot, do not let your protein intake crash to zero. That is exactly when shakes prove their worth.
The best whole food protein sources to combine with your shakes
Your protein shakes work best as part of a comprehensive nutrition strategy. Here are the whole food sources that pair best with GLP-1 medications, ranked by tolerance and protein density.
High tolerance, high protein
Greek yogurt (15-20g per serving): Smooth, cold, and easy to eat even with mild nausea. The probiotics also support gut health, which is important since GLP-1 medications affect the digestive system. Choose plain varieties and add your own flavoring to control sugar content.
Eggs (6-7g each): Versatile, easy to prepare in small portions, and well-tolerated by most GLP-1 users. Scrambled, hard-boiled, or poached all work. Two to three eggs provide 12 to 21 grams of complete protein in a small, manageable volume.
Cottage cheese (14g per half cup): High protein density in a small volume. The soft texture makes it easy to eat. Mix with fruit for palatability.
Moderate tolerance, high protein
Chicken breast (31g per 4 oz): The classic high-protein food. But for GLP-1 users, dry chicken can be difficult to eat and sits heavy. Shred it, use it in soups, or marinate it to improve tolerance. Rotisserie chicken tends to be better tolerated than grilled breast.
Fish and seafood (20-25g per 4 oz): White fish like cod, tilapia, and sole are extremely well-tolerated. They are light, flaky, and digest relatively easily. Salmon provides healthy omega-3 fats but is richer, so portions may need to be smaller. Shrimp is another excellent option with 20 grams of protein in just 4 ounces.
Turkey deli meat (10-12g per 2 oz): Convenient, no preparation needed, and easy to eat in small amounts. Look for low-sodium, nitrate-free options. Roll it up with a slice of cheese for an easy high-protein snack.
Variable tolerance, good protein
Lean beef (26g per 4 oz): Excellent protein and iron content, but many GLP-1 users develop an aversion to red meat during treatment. If you tolerate it, ground beef in small portions is usually easier than steak.
Tofu (10g per half cup, firm): A solid plant-based option that is easy on the stomach. The soft texture works well when chewing feels like a chore. Press it, cube it, and add it to soups or stir-fries.
Lentils and beans (8-9g per half cup cooked): Good protein and fiber, but the fiber content can worsen bloating for some GLP-1 users. Start with small portions and see how you tolerate them.
Protein shake recipes optimized for GLP-1 users
Generic protein shake recipes rarely account for the unique digestive challenges of GLP-1 therapy. These recipes are designed specifically for semaglutide and tirzepatide users.
The gentle morning shake (for injection days and high-nausea periods)
Ingredients: 1 scoop unflavored whey isolate (25g protein), 12 oz cold water, 1 tablespoon fresh ginger (grated), squeeze of lemon juice, 4-5 ice cubes.
Calories: approximately 110. Protein: 25g. Why it works: Ginger is a natural anti-nausea agent. The thin, cold consistency is easy to sip slowly. No dairy, minimal flavor compounds that might trigger aversion.
The muscle-preservation smoothie (for good tolerance days)
Ingredients: 1 scoop vanilla whey isolate (25g protein), 1/2 frozen banana, 1/2 cup frozen berries, 8 oz unsweetened almond milk, 1 tablespoon ground flaxseed, 4-5 ice cubes.
Calories: approximately 230. Protein: 27g. Why it works: Fruit provides potassium (important for muscle function and often depleted during rapid weight loss). Flaxseed adds omega-3s without significant bulk. The frozen fruits create a thick, satisfying texture that feels like a treat.
The savory protein broth (when sweet flavors are intolerable)
Ingredients: 1 scoop unflavored whey isolate (25g protein), 10 oz warm (not boiling) bone broth or chicken broth, pinch of salt, splash of hot sauce (optional).
Calories: approximately 140. Protein: 30-35g (broth adds protein). Why it works: Many GLP-1 users find that sweet flavors become intolerable, especially during dose escalation. This savory option tastes like a light soup. The warm temperature is soothing on the stomach. And bone broth adds its own protein plus collagen, glycine, and gelatin for gut support.
The protein popsicle (for severe nausea days)
Ingredients: 1 scoop berry-flavored clear whey isolate (22g protein), 8 oz cold water, 1/4 cup fresh berries blended smooth. Pour into popsicle molds and freeze for 4+ hours.
Calories: approximately 120. Protein: 22g. Why it works: Frozen food is one of the best-tolerated formats during severe nausea. You consume the protein slowly as the popsicle melts, which prevents the stomach from being overwhelmed. Keep a batch in the freezer for your worst days.
The overnight protein pudding (for people who hate drinking shakes)
Ingredients: 1 scoop chocolate or vanilla casein protein (25g protein), 1/2 cup plain Greek yogurt (10g protein), 4 oz unsweetened almond milk. Mix together, refrigerate overnight.
Calories: approximately 220. Protein: 35g. Why it works: The casein and yogurt create a thick, pudding-like texture overnight. For people who find drinking protein intolerable, eating it with a spoon can be a game-changer. Best consumed on days 4-7 of the dosing cycle when GI tolerance is highest.
Resistance training: the other half of the muscle preservation equation
Protein shakes alone will not save your muscle mass. They provide the raw materials. But without the mechanical signal of resistance training, your body has no reason to prioritize keeping muscle during a calorie deficit.
A study from the Endocrine Society showed that combining higher protein intake with resistance training 2 to 3 times per week can prevent, and in some cases even reverse, the lean mass loss typically seen with GLP-1 medications. This is not optional if you care about body composition.
The minimum effective resistance training protocol for GLP-1 users
You do not need to become a powerlifter. The minimum effective dose for muscle preservation during GLP-1 therapy is:
Frequency: 2-3 sessions per week. Duration: 30-45 minutes per session. Exercises: Compound movements that work multiple muscle groups. Squats, deadlifts, rows, presses, and lunges. Intensity: Moderate. You should be able to complete 8-12 repetitions with a weight that feels challenging by the last 2-3 reps. Progression: Gradually increase weight or reps over time. Your body adapts, so the stimulus must increase.
The timing of your post-workout protein shake matters here. Consuming 25 to 30 grams of protein within 60 minutes of finishing your resistance training session maximizes muscle protein synthesis during the recovery window. This is when your muscles are most receptive to amino acids and most actively repairing the micro-damage from training.
Adjusting training for GLP-1 side effects
Exercise on GLP-1 medications requires some modifications. If you experience fatigue, schedule your workouts on your best-feeling days (typically days 4-6 of your dosing cycle). If nausea is an issue, avoid heavy compound movements that increase intra-abdominal pressure (like heavy squats or deadlifts) and substitute machines or lighter free weights.
Stay hydrated. GLP-1 medications reduce thirst along with hunger, and exercising while dehydrated increases muscle breakdown and reduces performance. Aim for at least 16 ounces of water in the hour before training and sip water throughout your session.
Common mistakes GLP-1 users make with protein shakes
After reviewing thousands of protocols and community discussions, certain mistakes come up repeatedly. Avoid these.
Mistake 1: counting collagen as complete protein
Collagen peptides count toward your total protein grams, but they should not be counted as complete protein for muscle-building purposes. If you are getting 40 grams of your daily protein from collagen and 60 grams from whey, your effective muscle-building protein is closer to 60 grams, not 100. Use collagen as a bonus, not a foundation. Your primary protein should come from complete sources.
Mistake 2: drinking protein shakes too fast
On GLP-1 medications, chugging a protein shake in 2 minutes like you might at the gym is a recipe for nausea, bloating, and potentially vomiting. Your stomach empties 30% to 50% slower than normal. Treat every protein shake like a slow-sipping cocktail. Twenty to thirty minutes minimum.
Mistake 3: choosing mass-gainer shakes
Mass-gainer protein shakes contain 500 to 1,200 calories per serving, loaded with maltodextrin, fats, and sugars designed to help underweight people gain weight. They are the exact opposite of what GLP-1 users need. You want maximum protein per calorie, not maximum calories per serving. Always check the nutrition label. If the calorie count is over 200 per serving or the sugar content is over 10 grams, it is probably not formulated for your situation.
Mistake 4: only drinking protein on workout days
Muscle protein synthesis does not stop on rest days. Your muscles are recovering and rebuilding 24/7, not just in the hours after exercise. Your protein needs are the same every day, regardless of whether you trained. In fact, recovery days are when your muscles are doing the most rebuilding. Skipping protein on rest days undermines the work you did in the gym.
Mistake 5: ignoring micronutrients
When your total caloric intake drops to 800 to 1,200 calories per day, micronutrient deficiencies become a serious concern. Protein shakes provide protein but usually lack adequate amounts of iron, calcium, vitamin D, vitamin B12, and magnesium. These nutrients are critical for muscle function, bone density, and energy metabolism.
Consider pairing your protein shake strategy with a high-quality multivitamin. Supplements to take with GLP-1 medications should include vitamin D (2,000 to 4,000 IU daily), calcium (600 to 1,200 mg daily), magnesium (200 to 400 mg daily), and a B-complex vitamin. Your protein shakes handle the macronutrient side. Your supplements handle the micronutrient side.
Mistake 6: stopping protein shakes when appetite returns
As your body adapts to GLP-1 medications, appetite suppression often moderates. Some users take this as a signal to stop their protein shake regimen. Do not. Even when you can eat more whole food, maintaining at least one daily protein shake ensures you consistently hit your protein targets. It is insurance against the days when your appetite fluctuates unpredictably.
Special considerations for different GLP-1 medications
While the core protein strategy is the same across all GLP-1 medications, there are specific nuances worth noting for each one.
Semaglutide (Ozempic, Wegovy) protein considerations
Semaglutide produces the strongest appetite suppression of the pure GLP-1 agonists, particularly at the 2.4 mg dose used for weight management. This means protein shake tolerance can be especially challenging during the first 8 to 12 weeks.
Start with half servings. Seriously. Use half a scoop of protein powder in a full serving of liquid for the first two weeks at each new dose level. Once you confirm tolerance, increase to a full scoop.
Semaglutide users also report more taste changes than tirzepatide users. Be prepared to experiment with multiple flavors and formats. What works at the 0.5 mg dose might become intolerable at 1.0 mg or 2.4 mg.
Semaglutide with B12 compounds may offer additional benefits for energy and metabolism. The B12 can help offset the fatigue that makes maintaining exercise and nutrition routines challenging during treatment.
Tirzepatide (Mounjaro, Zepbound) protein considerations
Tirzepatide works on both GLP-1 and GIP receptors, which creates a slightly different side effect profile. GI side effects can be just as intense, but many users report that nausea peaks more sharply and resolves more quickly compared to semaglutide. This means you might have a wider window for comfortable protein shake consumption during the week.
The body composition data also suggests that tirzepatide may be slightly more muscle-sparing than semaglutide, with lean mass accounting for roughly 25.7% of weight lost versus 45.2% with semaglutide. This does not mean you need less protein. It means the protein you consume may be even more effective at preserving muscle when combined with tirzepatide.
Some tirzepatide compounds that include glycine offer additional support for digestive comfort. Glycine is an amino acid that supports gut lining integrity and can reduce GI side effects, making protein shakes easier to tolerate.
Retatrutide and newer triple-agonist considerations
For users exploring retatrutide or other triple-agonist medications (GLP-1/GIP/glucagon), the protein requirements are likely even higher. The glucagon component increases the metabolic rate, which means more calories are being burned at rest, but it also means muscle tissue is at greater risk of breakdown without adequate protein.
Triple-agonist users should aim for the higher end of protein targets, 1.6 to 2.0 g/kg/day, and consider three protein shakes per day rather than two during the initial dose escalation phase. The appetite suppression from triple agonists tends to be even more pronounced than with semaglutide or tirzepatide alone.
Protein shake ingredients to avoid on GLP-1 medications
What you leave out of your protein shake matters as much as what you put in. These ingredients are common in protein powders but problematic for GLP-1 users.
Sugar alcohols (erythritol, sorbitol, xylitol, maltitol)
Sugar alcohols are used as low-calorie sweeteners in many protein powders and pre-made shakes. They cause gas, bloating, and diarrhea in many people even without GLP-1 medications. With the slowed gastric emptying from semaglutide, these effects are amplified significantly. Check labels carefully. If any sugar alcohol is listed in the first five ingredients, look for a different product.
Carrageenan
This common thickener derived from seaweed is used in many pre-made protein shakes. Research suggests it can trigger intestinal inflammation in sensitive individuals. On GLP-1 medications, where your gut is already under stress from altered motility, carrageenan can worsen bloating, cramping, and general GI discomfort.
Inulin and chicory root fiber
These prebiotic fibers are added to many protein powders for their supposed gut health benefits. While they can be beneficial in normal circumstances, they ferment rapidly in the gut, producing gas. With GLP-1-slowed transit time, that gas has nowhere to go quickly, leading to painful bloating and distension.
MCT oil or coconut oil powder
Some protein powders add MCT oil for purported fat-burning benefits. For GLP-1 users, the added fat further slows already-impaired gastric emptying. The result is prolonged fullness, nausea, and a feeling of the shake sitting like lead in your stomach.
Heavy metals contamination
This is not specific to GLP-1 users, but it matters. Many protein powders, particularly plant-based ones, contain concerning levels of lead, cadmium, arsenic, and mercury. When you are consuming protein powder daily as a medical necessity, long-term heavy metal exposure becomes a legitimate concern. Look for brands that provide third-party testing results for heavy metals. NSF Certified for Sport or Informed Sport certifications indicate testing has been done.
How protein shakes fit into the bigger GLP-1 nutrition picture
Protein is the priority, but it is not the only nutritional consideration during GLP-1 therapy. Your protein shake strategy should fit into a comprehensive nutrition plan that addresses all the challenges these medications create.
Hydration: the overlooked foundation
GLP-1 medications reduce not just hunger but thirst. Many users become chronically mildly dehydrated without realizing it, which worsens constipation, headaches, and fatigue. Since protein metabolism produces nitrogen waste that the kidneys must flush out, adequate hydration is even more important on a high-protein diet.
Aim for at least 64 ounces of water daily, more if you are exercising. Your protein shakes contribute to total fluid intake, which is another advantage they offer over whole food protein sources.
Fiber and gut health
Constipation is one of the most common side effects of GLP-1 medications, affecting 20% to 30% of users. While your protein shakes should be low in fiber to prevent bloating, you need to get adequate fiber from other sources. Fruits, vegetables, and whole grains consumed during your higher-tolerance days provide the fiber your gut needs.
Probiotic-rich foods like yogurt, kefir, and fermented vegetables support the gut microbiome, which GLP-1 medications can disrupt. Including Greek yogurt as one of your protein sources does double duty, providing both protein and probiotics.
Electrolytes and minerals
Rapid weight loss depletes electrolytes. Combined with reduced food intake and potential GI side effects like diarrhea or vomiting, electrolyte imbalances can cause muscle cramps, fatigue, irregular heartbeat, and dizziness. Ensure adequate intake of sodium, potassium, and magnesium either through food, supplements, or electrolyte-enhanced protein shakes.
Healthy fats
While your protein shakes should be low-fat, your overall diet should not be fat-free. Essential fatty acids (omega-3s and omega-6s) support hormone production, brain function, and nutrient absorption. Get them from small portions of fatty fish, avocado, nuts, seeds, and olive oil during your higher-tolerance days. Just keep them separate from your protein shakes to prevent the digestion issues discussed earlier.
Tracking your protein intake on GLP-1 medications
What gets measured gets managed. Tracking your daily protein intake during GLP-1 therapy is not obsessive. It is necessary. The margin for error is slim when your total food intake is so reduced.
Simple tracking methods
You do not need a complicated app or a food scale at every meal. A simple tracking approach works for most people:
Know your protein shake numbers. If you use the same powder daily, memorize the protein per scoop. One scoop equals 25 grams. Two shakes a day equals 50 grams from shakes. Now you just need to track your food protein.
Use the palm method for whole foods. A palm-sized portion of meat, fish, or poultry contains approximately 25 to 30 grams of protein. One palm at lunch, one at dinner, plus your two shakes puts you at 100 to 110 grams. Quick mental math, no apps required.
Track weekly averages, not daily totals. Some days on GLP-1 medications, you simply cannot eat enough. Other days are better. What matters is that your weekly average protein intake stays in the target range. One bad day does not undo a good week.
When to adjust your protein targets
Increase protein targets when you increase your GLP-1 dose (each dose escalation increases muscle loss risk). Increase when you start or intensify a resistance training program. And increase when you notice signs of muscle loss, such as weakness that is disproportionate to weight loss, difficulty with everyday tasks, or your body composition metrics showing a declining lean mass percentage.
Decrease protein targets if you are experiencing kidney issues (consult your doctor first) or if GI side effects are so severe that forcing protein is causing more harm than good. In the latter case, focus on getting whatever protein you can tolerate and work with your prescriber on managing the GI symptoms.
The role of protein shakes in long-term GLP-1 maintenance
Most people think of protein shakes as a temporary measure during the active weight loss phase of GLP-1 therapy. But the research suggests protein supplementation remains important even after you reach your goal weight.
Transitioning from weight loss to maintenance
When you transition from weight loss to maintenance on GLP-1 medications, your caloric intake increases but your protein needs remain high. Your body is still adapting to its new weight, still rebuilding some of the lean mass that was lost, and still requires elevated protein to support metabolic health.
During maintenance, many users can reduce from two or three daily protein shakes to one, using it as insurance to hit their targets on days when whole food intake falls short. The shake transitions from a primary protein source to a backup.
What happens if you stop GLP-1 medications
Weight regain after stopping GLP-1 medications is common, with studies showing 50% to 70% of lost weight returning within a year. The users who maintain the best outcomes are those who built sustainable habits during treatment, including adequate protein intake and regular resistance training.
If you stop your medication, your appetite will return to normal, making whole food protein easier to consume. But maintaining at least one daily protein shake can help prevent the gradual slide back into old eating patterns. Think of it as a nutritional anchor, a daily habit that keeps protein front and center in your diet.
Protein shakes and specific health conditions on GLP-1 therapy
Certain health conditions require modifications to the standard protein shake approach.
Type 2 diabetes
If you are using semaglutide or tirzepatide for type 2 diabetes management alongside weight loss, blood sugar control adds another layer of complexity. Choose protein shakes with less than 5 grams of sugar per serving. Avoid shakes with maltodextrin or dextrose, which spike blood sugar rapidly. And time your protein shake 30 to 60 minutes before meals, which can help blunt the blood sugar response to the subsequent meal.
A whey protein shake consumed before a carbohydrate-containing meal has been shown to improve postprandial glucose control by stimulating additional GLP-1 secretion and slowing gastric emptying of the meal. This is one of the few cases where protein timing has a direct, measurable health benefit beyond muscle preservation.
Kidney disease
High protein intake can stress compromised kidneys. If you have chronic kidney disease (any stage), talk to your nephrologist before increasing protein intake or starting protein shakes. Your protein target may need to be lower than the standard 1.2 to 1.6 g/kg recommendation, and specific types of protein may be more appropriate.
Pregnancy and breastfeeding
GLP-1 medications are not recommended during pregnancy or breastfeeding. If you become pregnant while on treatment, work with your healthcare provider immediately. Protein needs during pregnancy are different from those during weight loss.
Over 65
Older adults on GLP-1 medications face the highest risk of muscle loss because they are already experiencing age-related muscle decline (sarcopenia). Protein needs are at the higher end of the range, 1.6 to 2.0 g/kg/day, and resistance training is even more critical. Protein shakes enriched with leucine (look for at least 3 grams per serving) are particularly beneficial for older adults because the leucine threshold for muscle protein synthesis increases with age.
Frequently asked questions
Can I replace all my meals with protein shakes on GLP-1 medications?
No. While protein shakes are essential for meeting protein targets, they should not replace all meals. Whole foods provide micronutrients, fiber, phytonutrients, and the mechanical stimulation of chewing that liquid meals cannot replicate. Aim for at least one whole food meal per day, even if it is small. Use meal planning strategies to make those meals as nutrient-dense as possible.
Will protein shakes slow my weight loss on semaglutide or tirzepatide?
Protein shakes will not slow fat loss if your total caloric intake remains in a deficit, which it almost certainly will on GLP-1 medications. What they may do is slow the number on the scale slightly because you are preserving muscle mass, which weighs more than fat. This is a good thing. Your body composition is improving even if the scale moves more slowly. Focus on how your clothes fit, how you feel, and your body measurements rather than just the number on the scale.
How soon after starting GLP-1 medication should I begin protein shakes?
Start immediately. Muscle loss begins from the first day of caloric restriction. Do not wait until you notice weakness or your doctor tells you that you have lost muscle. By then, you have already lost lean mass that is difficult to regain. Start with one shake per day at your initial dose and increase to two as appetite suppression intensifies with dose escalation.
Can I drink protein shakes on an empty stomach with GLP-1 medications?
You can, but many users find it triggers nausea, especially on high-nausea days. Eating a few plain crackers, a small piece of fruit, or a few bites of toast 10 to 15 minutes before your protein shake can help settle your stomach. If you tolerate shakes on an empty stomach, there is no medical reason to avoid it.
What if I cannot tolerate any protein shakes?
If traditional protein shakes are completely intolerable, try these alternatives. Mix unflavored protein powder into foods like oatmeal, yogurt, soup, or mashed sweet potatoes. Try collagen peptides in coffee or tea (not a complete protein but contributes to total protein grams). Use clear whey protein that dissolves like a juice. Try protein-enriched waters or protein-enhanced broths. If all liquid and powder forms fail, focus entirely on high-protein whole foods in the smallest tolerable portions.
Should I use protein shakes with creatine on GLP-1 medications?
Creatine is safe to combine with GLP-1 medications and may offer additional muscle preservation benefits. It helps maintain intramuscular water content (which supports muscle function and appearance) and has been shown to enhance the muscle-building response to resistance training. Adding 3 to 5 grams of creatine monohydrate to your daily protein shake is a reasonable strategy for GLP-1 users concerned about muscle loss.
Do protein shakes interact with semaglutide or tirzepatide?
There are no known drug interactions between protein shakes and any GLP-1 receptor agonist. Protein shakes are food, and the medication works regardless of what you eat. The only consideration is timing. Taking your protein shake immediately around injection time is fine pharmacologically, but it may not be practical if nausea is present.
How much protein is too much on GLP-1 medications?
For healthy individuals, protein intake up to 2.2 g/kg/day is well-supported by research and generally safe. Going above this level provides no additional muscle-preserving benefit and simply wastes calories on excess protein your body cannot use for muscle building. Unless you are an elite athlete doing intense daily training, staying in the 1.2 to 1.6 g/kg/day range is optimal for most GLP-1 users.
External resources
Impact of Semaglutide on Body Composition: STEP 1 Study (PubMed Central)
Higher Protein Intake May Protect Against Muscle Loss on Anti-Obesity Drugs (Endocrine Society)
For researchers serious about optimizing their protocols during GLP-1 therapy, SeekPeptides provides the most comprehensive resource available. Members access evidence-based nutrition guides, body composition tracking tools, and a community of thousands who have navigated these exact protein and muscle preservation questions successfully.
In case I do not see you, good afternoon, good evening, and good night. May your protein stay complete, your muscle stay preserved, and your progress stay consistent.