Feb 13, 2026

Some people start semaglutide and feel like they have been plugged into a wall outlet. More stamina at the gym. Sharper focus at work. The kind of energy they have not felt in years. Others? They can barely get off the couch for the first three weeks. Same medication. Wildly different experiences. And that contradiction is exactly why this question keeps showing up in forums, doctor offices, and late-night search sessions.
The honest answer is complicated. Semaglutide does not directly boost energy the way caffeine does. It will not light up your central nervous system or flood your brain with stimulants. But it triggers a cascade of metabolic changes, from improved insulin sensitivity to reduced systemic inflammation, that can absolutely transform how energized you feel over weeks and months. The catch is that getting there often means pushing through a temporary fatigue window that derails some people before the benefits kick in.
This guide breaks down every mechanism behind semaglutide and energy. Not the vague "you might feel better" advice. The actual science. We will cover why initial fatigue happens, which metabolic pathways lead to genuine energy improvements, the timeline most people follow, and twelve specific strategies that help you get through the rough patch faster. Whether you are three days into your first dose or three months in wondering why your energy still has not bounced back, the answers are here.
SeekPeptides has tracked thousands of GLP-1 protocol outcomes, and the pattern is clear: energy is not a side effect of semaglutide. It is a downstream result of getting the fundamentals right while the medication does its job.
How semaglutide actually works in your body
Before you can understand the energy question, you need to understand what semaglutide does at a molecular level. It is not a weight loss drug that happens to affect energy. It is a GLP-1 receptor agonist that reshapes how your entire metabolic system processes fuel.
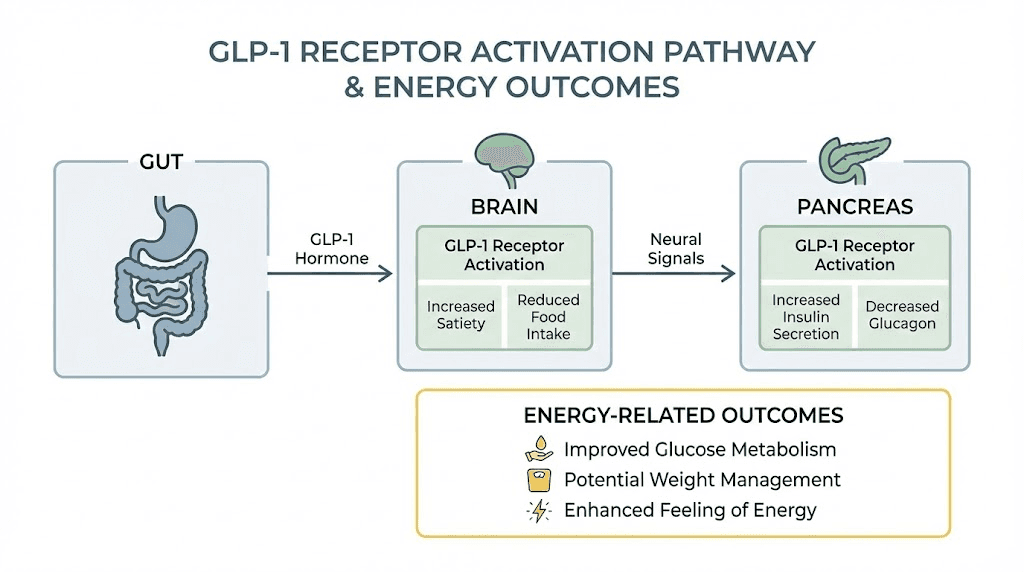
Semaglutide mimics a hormone called glucagon-like peptide-1. Your gut naturally produces GLP-1 after meals. It tells your pancreas to release insulin, signals your liver to slow glucose production, and communicates with your brain that you have eaten enough. The natural version lasts minutes. Semaglutide lasts about a week.
That extended activity creates several downstream effects that all touch energy in different ways. Your blood sugar stabilizes. Your appetite decreases. Your body starts tapping into fat stores more efficiently. And your brain receives consistent satiety signals instead of the chaotic hunger-crash-hunger cycle that drains energy from millions of people daily.
The insulin sensitivity connection
Here is where energy enters the picture. When your cells are insulin resistant, glucose piles up in your bloodstream instead of entering cells where it can be converted to ATP, your body's actual energy currency. You have fuel everywhere. Your cells are starving anyway.
Semaglutide improves insulin sensitivity through two mechanisms. First, it directly enhances pancreatic beta-cell function, improving insulin secretion timing and quantity. Second, the weight loss it produces further reduces insulin resistance. Research from the SUSTAIN trials shows that subjects on semaglutide experienced significant improvements in HOMA-IR scores, a standard measure of insulin resistance, within 12 weeks.
What does that mean for energy? When glucose actually enters your cells efficiently, you stop experiencing the blood sugar rollercoaster. No more 2pm crashes. No more needing sugar hits just to stay awake. Your energy becomes steady, predictable, and sustained throughout the day.
Blood sugar stability and sustained energy
Blood sugar swings are one of the biggest hidden causes of fatigue. A spike after eating floods you with energy briefly. Then insulin overcorrects. Blood sugar drops. You feel exhausted, irritable, foggy. So you eat again. The cycle repeats five or six times a day.
Semaglutide breaks this cycle. By slowing gastric emptying and improving insulin response, it flattens the glucose curve. Food enters your bloodstream more gradually. Insulin responds proportionally instead of overshooting. The result is not a spike of energy. It is a steady baseline that lasts all day.
This is why many people describe their energy on semaglutide not as "more" energy but as "better" energy. The total amount might be similar. The consistency changes everything.
The initial fatigue phase everyone needs to know about
Here is the part most articles bury or skip entirely. Many people feel worse before they feel better on semaglutide. And if nobody warns you, that fatigue can feel like a sign the medication is not working. It is actually a sign that it is.
Clinical trials report that approximately 11% of participants on semaglutide 2.4mg experienced fatigue as a side effect. Some smaller studies put the number closer to 6%. But anecdotal reports from forums and clinical practice suggest the real number is higher, because many people experience mild tiredness they do not formally report.
Why the first 2 to 6 weeks are rough
Several things happen simultaneously when you start semaglutide. Your appetite drops significantly. You eat fewer calories. Your body, accustomed to a certain caloric intake, suddenly receives less fuel than expected. That calorie deficit alone can cause fatigue.
But it goes deeper than simple calorie math. Your body is also adapting to a new metabolic state. Insulin patterns are shifting. Gastric emptying is slowing. Your hypothalamus is recalibrating hunger and satiety signals. All of that metabolic reorganization requires energy itself.
Then there are the gastrointestinal side effects. Nausea affects up to 44% of people in the early weeks. Nausea reduces food intake further. Dehydration from GI symptoms compounds the fatigue. Vomiting and diarrhea deplete electrolytes. Each factor stacks on the others.
Think of it like this. Your body is a factory retooling its entire assembly line. During the retooling, production slows. Once the new system is online, it runs more efficiently than before. But the transition period is genuinely rough.
The fatigue timeline most people experience
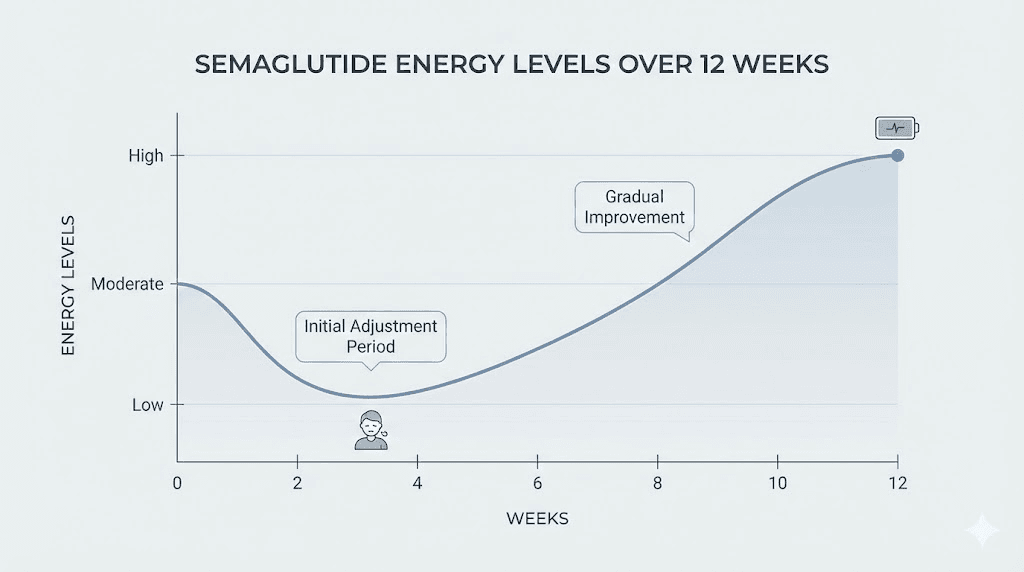
Based on clinical data and thousands of patient reports, the typical energy trajectory on semaglutide looks like this:
Week 1 to 2: Mild to moderate fatigue. Appetite suppression is strongest. Calorie intake drops sharply. GI side effects peak. Energy dips noticeably.
Week 3 to 4: GI symptoms begin stabilizing. Body starts adapting to lower caloric intake. Fatigue remains but starts improving for most people. Some report the first glimpses of improved energy.
Week 5 to 8: The turning point for most users. Weight loss becomes noticeable. Metabolic improvements start compounding. Energy levels begin exceeding baseline for many people.
Month 3 and beyond: Significant weight loss, improved insulin sensitivity, reduced inflammation, and better sleep quality combine to produce noticeably higher energy levels. Most people describe feeling better than they have in years.
Not everyone follows this exact timeline. Some people skip the fatigue phase entirely. Others struggle with it for months, usually because of nutritional issues we will cover later.
Six mechanisms that actually increase energy on semaglutide
Once you get past the adjustment period, semaglutide creates genuine, measurable improvements in energy through multiple pathways. These are not theoretical. They are documented in clinical trials and supported by metabolic research.
1. Improved mitochondrial efficiency
This is the most exciting recent finding. A study published in the journal Obesity found that semaglutide-induced weight loss improves mitochondrial energy efficiency in skeletal muscle. Mitochondria are the actual power plants of your cells, the organelles that convert nutrients into ATP.
The study demonstrated that after weight loss with semaglutide, skeletal muscle mitochondria showed improved oxidative phosphorylation (OXPHOS) efficiency. More efficient mitochondria means more energy produced from the same amount of fuel. Your cells literally become better at generating power.
This finding matters because it suggests the energy improvement is not just about eating less and losing weight. Semaglutide may trigger metabolic adaptations at the cellular level that fundamentally change how your body produces energy. Researchers noted that the AMPK signaling pathway, a master regulator of cellular energy balance, showed enhanced activity in GLP-1 treated subjects.
2. Reduced systemic inflammation
Chronic inflammation is an energy vampire. When your body is fighting low-grade inflammation, which is extremely common in people with excess weight, it diverts resources from normal function to immune activation. You feel tired because your body is literally spending energy on an inflammatory response instead of letting you use it.
Semaglutide has potent anti-inflammatory effects. The SELECT trial showed a 38% reduction in high-sensitivity C-reactive protein (hs-CRP) compared to placebo. Other studies show reductions in pro-inflammatory cytokines including IL-6 and TNF-alpha. These markers directly correlate with fatigue in research.
When inflammation drops, energy becomes available for things you actually want to do. Exercise feels easier. Mental fog lifts. Recovery from workouts improves. The connection between semaglutide and fatigue often reverses once inflammation decreases enough for the benefits to show up.
3. Better sleep quality
Excess weight and obesity significantly increase the risk of obstructive sleep apnea, a condition where your airway partially collapses during sleep, causing repeated micro-awakenings throughout the night. Even mild sleep apnea devastates energy levels because it prevents deep, restorative sleep cycles.
Research shows that GLP-1 receptor agonist users have a 40% lower likelihood of obstructive sleep apnea compared to non-users after adjusting for demographic factors. Weight loss of 10 to 15%, which semaglutide commonly achieves, can significantly reduce sleep apnea severity. The FDA approved tirzepatide specifically for sleep apnea in late 2024, and semaglutide appears to offer similar benefits.
Better sleep means better energy. It is that straightforward. If you have been carrying excess weight and sleeping poorly for years, the improvement in sleep quality alone can transform how you feel during the day. Many users report this is the first improvement they notice, sometimes before significant weight loss even occurs.
4. Reduced physical burden from weight loss
This one is simple physics. Carrying 30, 50, or 100 extra pounds requires enormous energy expenditure just to move through daily life. Walking. Climbing stairs. Standing at a counter. Every activity costs more calories and creates more fatigue when you are heavier.
Semaglutide produces average weight loss of 12 to 15% of body weight in clinical trials. For a 250-pound person, that is 30 to 37 pounds. The reduction in mechanical load on joints, muscles, and the cardiovascular system frees up enormous energy reserves for other activities.
This mechanism is the most intuitive one. When you weigh less, everything requires less effort. Your heart works less hard. Your knees take less impact. You breathe more easily. The compounding effect on daily energy is substantial, and it builds progressively as weight loss continues.
5. Improved cardiovascular efficiency
Semaglutide improves several cardiovascular markers that directly affect how efficiently oxygen reaches your tissues. Blood pressure decreases. Lipid profiles improve. Arterial function improves. The SELECT trial demonstrated a 20% reduction in major adverse cardiovascular events, indicating genuine cardiovascular improvement beyond just weight loss.
When your cardiovascular system works more efficiently, oxygen delivery to muscles and organs improves. This translates directly to energy. Activities that previously left you winded become manageable. Exercise tolerance increases. Recovery between activities speeds up.
6. Fat mobilization as a fuel source
Early in semaglutide treatment, research shows the body shifts toward increased fat oxidation. This means your body becomes more efficient at using stored fat as fuel rather than relying exclusively on dietary glucose.
This metabolic shift is significant for energy. Stored fat represents an enormous energy reserve. A single pound of fat contains approximately 3,500 calories. When your body can access these stores efficiently, you have a virtually unlimited fuel supply compared to the limited glucose available from meals.
The shift does not happen overnight. And during the transition, some people experience fatigue as their body adjusts from primarily burning glucose to incorporating more fat oxidation. But once the metabolic adaptation completes, many people report more stable, sustained energy throughout the day, even when eating significantly less food.
Why some people never get the energy boost
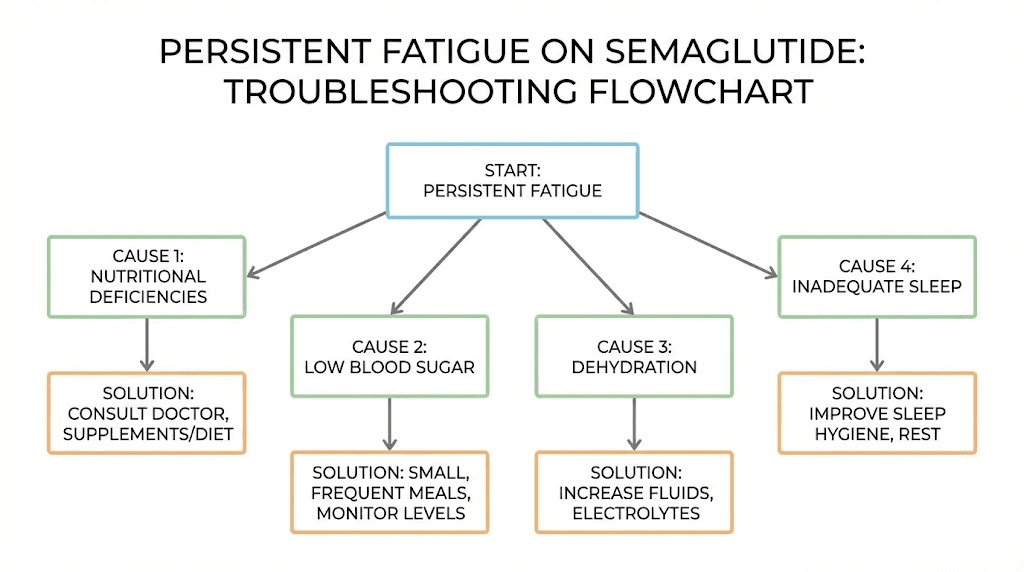
Not everyone on semaglutide experiences improved energy. For some people, the fatigue persists or even worsens over time. Understanding why helps you troubleshoot your own situation and make adjustments before giving up on the medication entirely.
Severe caloric restriction
The most common cause of persistent fatigue on semaglutide is eating too little. When appetite suppression is strong, some people drop to 600 to 800 calories per day without realizing it. That is not sustainable. Your body needs a minimum number of calories to maintain basic metabolic functions, and consistently eating below that threshold triggers conservation mode.
In conservation mode, your body reduces non-essential energy expenditure. You feel tired because your body is deliberately slowing you down to preserve calories for vital organ function. The right diet plan on semaglutide targets a moderate deficit, typically 500 to 750 calories below maintenance, not the extreme restriction that appetite suppression can accidentally create.
Protein deficiency
When you eat less, you almost always eat less protein unless you actively prioritize it. Protein is essential for maintaining muscle mass, neurotransmitter production, enzyme function, and immune response. Without adequate protein, fatigue develops quickly and persists stubbornly.
Research suggests that people on GLP-1 medications should aim for 0.7 to 1.0 grams of protein per pound of body weight per day. For many people, that means protein needs to represent 30 to 40% of their reduced caloric intake. This is substantially higher than most people eat naturally, and it requires deliberate planning.
Dehydration and electrolyte imbalances
GI side effects cause fluid loss. Eating less food means less water intake from food (which normally provides about 20% of daily hydration). And many people simply forget to drink enough water when they are not feeling hungry.
Dehydration of even 2% of body weight causes measurable fatigue, reduced concentration, and decreased physical performance. Electrolyte imbalances, particularly sodium, potassium, and magnesium, amplify these effects significantly.
Nutrient deficiencies
Eating fewer total calories increases the risk of specific nutrient deficiencies that directly cause fatigue. The most common culprits include:
Iron: Reduced meat intake means less heme iron absorption. Iron deficiency is the most common nutritional deficiency worldwide and directly causes fatigue through reduced oxygen-carrying capacity.
Vitamin B12: Essential for energy metabolism and red blood cell production. People taking semaglutide with B12 supplementation often report better energy outcomes than those without.
Vitamin D: Deficiency is associated with fatigue, muscle weakness, and mood changes. People losing weight rapidly may need to adjust vitamin D intake upward.
Magnesium: Involved in over 300 enzymatic reactions including energy production. GI side effects can deplete magnesium quickly.
Inadequate dose titration
Jumping to a higher dose too quickly overwhelms your body's ability to adapt. The standard semaglutide titration schedule starts at 0.25mg weekly for four weeks, increases to 0.5mg for four weeks, then 1.0mg, then 1.7mg, and finally 2.4mg for weight management. Each step gives your body time to adjust.
Skipping steps or accelerating the schedule means more severe side effects, more GI distress, more caloric restriction, and more fatigue. Patience with titration often determines whether someone has a smooth or miserable experience. Check your semaglutide dosage if fatigue seems disproportionate to what others report.
Underlying medical conditions
Semaglutide does not fix thyroid disorders, anemia, chronic fatigue syndrome, or sleep disorders unrelated to weight. If fatigue persists beyond 8 to 12 weeks despite proper nutrition, hydration, and dose management, it warrants investigation into other causes.
Twelve strategies to maximize energy while on semaglutide
If you are experiencing fatigue or want to ensure you get the energy benefits as quickly as possible, these twelve strategies address every known contributing factor. They are ordered by impact, with the most important ones first.
1. Track your actual calorie intake for one week
You cannot fix a problem you cannot see. Most people on semaglutide dramatically underestimate how little they are eating. Use a food tracking app for seven days. Do not change what you eat. Just measure it.
If you are consistently below 1,200 calories for women or 1,500 for men, that is likely a major contributor to your fatigue. The goal is not to eat as little as possible. It is to eat enough to support energy while still maintaining a moderate deficit for weight loss. Your calculator tools can help establish appropriate targets.
2. Front-load protein at every meal
Make protein the first thing you eat at every meal. When appetite is limited, you need to prioritize the most important macronutrient first. Aim for 25 to 40 grams of protein per meal, starting with breakfast.
Good protein sources when appetite is low include Greek yogurt, protein shakes, eggs, cottage cheese, chicken breast, and fish. These are all nutrient-dense without being heavy on the stomach, which matters when semaglutide is causing appetite suppression.
3. Hydrate aggressively, especially in the first month
Aim for 80 to 100 ounces of water daily during the first eight weeks of semaglutide treatment. This is more than the standard recommendation because GI side effects increase fluid losses.
Add electrolytes if you experience nausea, vomiting, or diarrhea. A pinch of salt and a squeeze of lemon in water provides sodium and makes water more palatable. Sugar-free electrolyte packets work well too. Dehydration is the most easily fixable cause of fatigue on semaglutide and the one most people overlook.
4. Eat small, frequent meals instead of large infrequent ones
Semaglutide slows gastric emptying. Large meals sit in your stomach longer, cause more discomfort, and can actually reduce nutrient absorption. Five small meals of 300 to 400 calories beat three meals of 500 to 600 calories for both comfort and energy stability.
This approach also maintains steadier blood sugar levels throughout the day, preventing the energy crashes that some people experience even on semaglutide. Planning meals ahead becomes essential when appetite is unpredictable.
5. Supplement B12, iron, and vitamin D
These three nutrients are the most commonly deficient in people on GLP-1 medications, and all three directly affect energy levels. Consider getting blood work done before starting semaglutide to establish baselines, then recheck at 3 and 6 months.
B12 supplementation is especially important. The combination of semaglutide with B12 is increasingly common in compounded formulations specifically because clinicians recognized the fatigue-B12 connection. If your formulation does not include B12, supplement separately with 1,000 to 2,500mcg of methylcobalamin daily.
6. Maintain or start a movement practice
This sounds counterintuitive when you are tired. But moderate exercise actually increases energy over time by improving mitochondrial function, cardiovascular efficiency, and insulin sensitivity, the same mechanisms semaglutide enhances.
Start small. A 15-minute walk after meals improves blood sugar response and energy more effectively than an hour-long gym session you skip because you are too tired. Build gradually. The combination of semaglutide and consistent moderate exercise produces better energy outcomes than either alone.
Research on GLP-1 receptor agonists and the AMPK signaling pathway in skeletal muscle shows that physical activity amplifies the mitochondrial benefits of the medication. Exercise and semaglutide together enhance endurance more than either intervention independently.
7. Prioritize sleep quality ruthlessly
Seven to nine hours of sleep is non-negotiable during semaglutide treatment. Your body is undergoing significant metabolic changes. Sleep is when the majority of metabolic adaptation and tissue repair occurs.
Practical steps include maintaining a consistent sleep schedule, keeping your bedroom cool and dark, avoiding screens for 30 minutes before bed, and limiting caffeine after noon. If you suspect sleep apnea, get tested. Semaglutide will likely improve it as you lose weight, but in the meantime, untreated sleep apnea will sabotage your energy regardless of what else you do.
8. Follow the proper titration schedule
Do not rush to higher doses. The titration schedule exists specifically to minimize side effects and allow metabolic adaptation. Every dose increase may temporarily increase fatigue as your body readjusts.
If fatigue is severe at your current dose, discuss staying at that dose for an extra four weeks before increasing. The dosage charts provide starting frameworks, but individual adjustment based on tolerance is always appropriate. Slower titration often means better long-term outcomes with fewer side effects.
9. Add magnesium supplementation
Magnesium is involved in over 300 enzymatic reactions in the body, including ATP production, the direct energy currency of your cells. GI side effects from semaglutide can deplete magnesium rapidly, and many people are already deficient before starting the medication.
Magnesium glycinate is the best-tolerated form for people with GI sensitivity. Take 200 to 400mg daily, preferably in the evening since it also supports sleep quality. This single supplement addresses both energy production and sleep improvement simultaneously.
10. Manage stress and cortisol actively
Chronic stress elevates cortisol, which interferes with blood sugar regulation, disrupts sleep, and directly causes fatigue. Semaglutide does not neutralize the effects of chronic stress. If you are stressed, exhausted, and starting a new medication simultaneously, the combined load on your system can be overwhelming.
Daily stress management does not need to be complicated. Ten minutes of deep breathing, a short walk outside, or a brief meditation session can meaningfully reduce cortisol. The goal is consistency rather than intensity.
11. Time your injection strategically
Most people inject semaglutide once weekly. The first 48 to 72 hours after injection tend to have the strongest side effects, including fatigue. Timing your injection for a day when reduced energy is least disruptive, often Friday evening or Saturday morning, allows you to push through the peak side-effect window over the weekend.
This is particularly helpful during the first few months of treatment. As your body adapts, injection timing becomes less critical. Some people find that taking semaglutide at a specific time of day also matters. Evening injections allow you to sleep through the initial peak effects.
12. Consider adjunct supplements for energy support
Several supplements support energy production through mechanisms that complement semaglutide's effects:
CoQ10 (100 to 200mg daily): Supports mitochondrial energy production directly. Particularly important if you take statins, which deplete CoQ10.
Creatine (3 to 5g daily): Supports ATP recycling in muscles and brain. Well-researched, safe, and surprisingly effective for reducing fatigue during caloric restriction.
Alpha-lipoic acid (300 to 600mg daily): Supports glucose uptake into cells and has antioxidant properties that protect mitochondria.
L-carnitine (500 to 1,000mg daily): Helps transport fatty acids into mitochondria for energy production. Particularly relevant since semaglutide increases fat oxidation.

The energy timeline: what to realistically expect
Setting proper expectations prevents frustration and premature discontinuation. Here is what the research and clinical experience show about energy changes over time on semaglutide.
Days 1 to 7: the introduction phase
Most people notice appetite suppression within the first few days. Energy levels are variable. Some feel no change. Others notice mild fatigue, particularly if nausea is present. The key focus during this week is hydration and eating enough despite reduced appetite.
Weeks 2 to 4: the adjustment valley
This is typically the lowest point for energy. Your body is adapting to multiple simultaneous changes. Caloric intake has dropped. GI symptoms may be at their peak. Metabolic recalibration is underway. Many people describe this period as feeling "wiped out" or "foggy."
This is normal. This is temporary. And this is the phase where most people who quit do so. Understanding that it passes makes a significant difference in persistence.
Weeks 5 to 8: the turning point
GI side effects stabilize for most people. The body begins adapting to its new caloric intake. Weight loss becomes visible and motivating. Blood sugar regulation improves measurably. Many people report the first clear improvements in energy during this window.
The improvement often comes gradually rather than suddenly. You might notice you are less tired in the afternoon. Or that you completed a workout that would have been impossible three weeks ago. Or that you are sleeping deeper and waking more refreshed.
Months 3 to 6: compounding benefits
This is where the real energy transformation happens. Weight loss of 8 to 15% reduces physical burden significantly. Inflammation markers drop. Insulin sensitivity improves substantially. Sleep quality improves, often dramatically if you had undiagnosed sleep apnea.
By month three, most people who have followed proper nutrition and hydration protocols report energy levels equal to or better than before starting semaglutide. By month six, many describe it as the best sustained energy they have felt in years.
Month 6 and beyond: the new baseline
Long-term semaglutide users who maintain proper nutrition consistently report improved energy as one of the top benefits, alongside weight loss and reduced appetite. The metabolic improvements become self-reinforcing. Better energy leads to more activity, which leads to better metabolic health, which leads to even better energy.
Clinical data from the STEP trials shows that quality of life measures, including vitality and energy subscales, improve significantly in long-term semaglutide users compared to placebo. The improvement is not just subjective. It is measurable, reproducible, and well-documented.
Semaglutide energy compared to other GLP-1 medications
If energy is a primary concern, you might wonder how semaglutide compares to other options in the GLP-1 class. The answer involves some nuance.
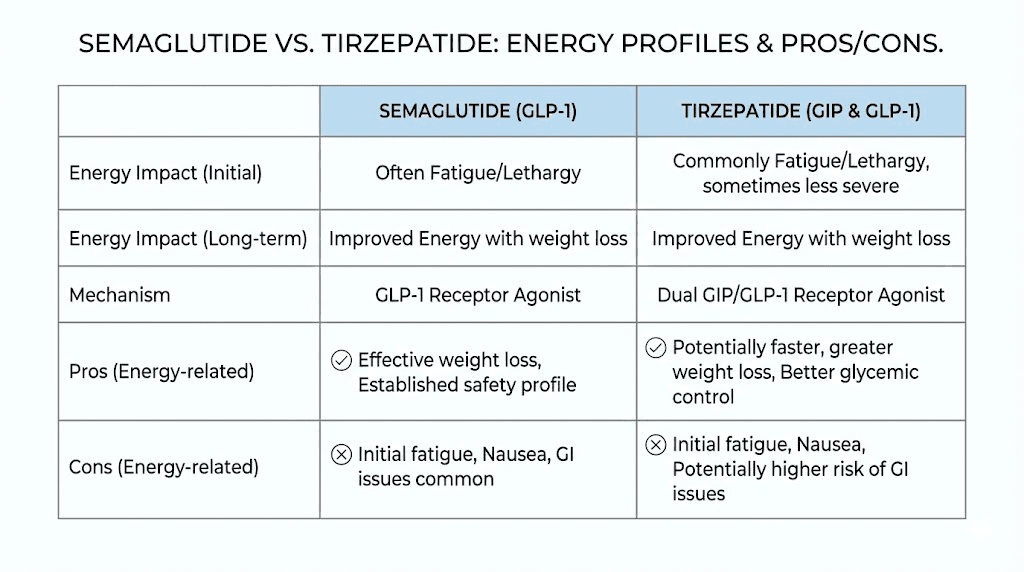
Semaglutide vs tirzepatide for energy
Tirzepatide and semaglutide produce similar fatigue profiles in clinical trials. Tirzepatide, which activates both GLP-1 and GIP receptors, tends to produce slightly more weight loss on average. More weight loss means potentially greater long-term energy improvement from reduced physical burden.
However, tirzepatide can also cause more pronounced GI side effects during titration, which might mean a longer or deeper fatigue valley initially. The semaglutide vs tirzepatide comparison for energy is roughly a wash, with individual variation being the biggest determining factor.
People switching between the two medications sometimes report different energy profiles. This makes sense given the different receptor activation patterns. If fatigue is persistent on one, trying the other is a reasonable conversation to have with your provider.
Oral vs injectable semaglutide
Oral semaglutide achieves lower bioavailability than injectable forms, requiring higher doses to achieve similar effects. The energy profile is broadly comparable, though some users report that oral formulations cause more GI distress initially, which can exacerbate fatigue.
The convenience of oral dosing may improve medication adherence, and consistent dosing produces more consistent metabolic effects, which indirectly supports stable energy levels.
Compounded vs brand-name formulations
Compounded semaglutide formulations sometimes include additional ingredients that may affect energy. B12 is the most common addition, and compounded semaglutide with B12 formulations may provide a slight energy advantage during the early adjustment phase simply because B12 supplementation is built into the dose.
Semaglutide combined with glycine is another compounded variation. Glycine supports neurotransmitter function, sleep quality, and has anti-inflammatory properties that could theoretically support energy, though direct studies on this combination and energy levels are limited.
What the science actually says: key studies on semaglutide and energy
Separating marketing claims from research findings requires looking at the actual studies. Here is what the evidence base shows.
The STEP trials and quality of life
The STEP clinical trial program, which included over 4,500 participants, measured quality of life using the SF-36 questionnaire. This validated instrument includes a "vitality" domain that specifically measures energy and fatigue. Participants on semaglutide 2.4mg showed statistically significant improvements in vitality scores compared to placebo.
Importantly, the improvement in vitality correlated with but was not entirely explained by weight loss. This suggests that semaglutide's effects on energy involve mechanisms beyond just weighing less, likely including the anti-inflammatory and metabolic efficiency improvements discussed earlier.
The SELECT trial and inflammation
The SELECT trial focused on cardiovascular outcomes but provided valuable data on inflammation. The 38% reduction in hs-CRP is one of the most robust findings linking semaglutide to reduced inflammation. Since chronic inflammation is a well-established cause of fatigue, this finding supports an indirect energy benefit from semaglutide.
Mitochondrial efficiency research
The 2025 study on semaglutide-induced weight loss and mitochondrial OXPHOS efficiency represents perhaps the most direct evidence that semaglutide can improve cellular energy production. Published in the journal Obesity, it demonstrated that weight loss from semaglutide specifically, not just caloric restriction, improved how efficiently skeletal muscle mitochondria produce ATP.
This is significant because it means the energy improvement is at least partially medication-specific. Simple caloric restriction without semaglutide would produce some weight loss but might not trigger the same degree of mitochondrial adaptation.
Appetite and energy intake studies
Multiple studies, including work published in Diabetes, Obesity and Metabolism, have shown that semaglutide reduces ad libitum energy intake by approximately 24 to 35%. This reduction in intake is the primary driver of weight loss, which in turn drives most of the energy improvements.
However, total energy expenditure does not appear to increase significantly with semaglutide. The medication does not speed up your metabolism in the traditional sense. Energy improvements come from metabolic efficiency, reduced inflammation, improved sleep, and reduced physical burden rather than from burning more calories at rest.
The prolonged treatment study
A study published in Diabetes in late 2025 examined prolonged semaglutide treatment in mice and found stage-dependent metabolic changes. Early in treatment, fat oxidation increased, consistent with active weight loss. During the maintenance phase, fuel utilization shifted back toward a more balanced glucose and fat mixture.
For energy, this means the body adapts its fuel source selection throughout treatment. Early energy changes might reflect the metabolic stress of shifting to fat oxidation. Later stability in energy often correlates with the body finding a new metabolic equilibrium.
Specific populations and energy considerations
Energy effects can vary significantly based on your starting health status, age, and other factors. Understanding your specific situation helps set appropriate expectations.
People with type 2 diabetes
If you have type 2 diabetes, semaglutide's energy benefits may be more pronounced because the insulin sensitivity improvements address a primary cause of your fatigue. Poorly controlled diabetes causes persistent fatigue through impaired glucose utilization. By improving glycemic control, semaglutide directly addresses this mechanism.
The SUSTAIN trials in diabetic populations showed significant improvements in HbA1c alongside improvements in patient-reported energy levels. For diabetic users, the energy improvement often begins earlier in treatment than for non-diabetic users.
People with significant obesity
If you are starting with a BMI above 35, the initial fatigue phase may be more pronounced because the caloric deficit relative to your previous intake is larger. However, the eventual energy improvement is also often more dramatic because the weight loss produces a larger absolute reduction in physical burden.
A 300-pound person losing 15% of body weight loses 45 pounds. That is 45 fewer pounds to carry up every flight of stairs, during every walk, throughout every waking hour. The energy freed by that reduction is enormous.
Women vs men
Women may experience more fatigue on semaglutide during certain phases of their menstrual cycle. Hormonal fluctuations affect energy independently, and the added metabolic stress of semaglutide can amplify existing cyclical fatigue patterns.
Iron deficiency is also more common in premenopausal women, and the reduced food intake on semaglutide can worsen iron status. Regular monitoring and supplementation are particularly important for women experiencing persistent fatigue on GLP-1 medications. If you are considering GLP-1 therapy during specific life stages, understanding GLP-1 use during breastfeeding and other hormonal considerations is essential.
Older adults
Adults over 60 may experience a longer adjustment period. Metabolic adaptation slows with age, and the body's ability to upregulate mitochondrial efficiency may be reduced. Muscle mass preservation becomes critical, as older adults lose muscle more readily during caloric restriction, and muscle loss directly reduces energy capacity.
Resistance training and adequate protein intake are even more important for older adults on semaglutide. The combination of the medication, progressive resistance exercise, and 1.0 to 1.2 grams of protein per kilogram of body weight per day provides the best energy outcomes in this population.
Combining semaglutide with other approaches for maximum energy
Semaglutide works best as part of a comprehensive approach rather than a standalone solution. These combinations have the strongest evidence for energy optimization.
Semaglutide and structured exercise
The combination of semaglutide and regular exercise produces energy improvements greater than either intervention alone. Exercise directly stimulates mitochondrial biogenesis (the creation of new mitochondria), amplifying the mitochondrial efficiency improvements semaglutide triggers through weight loss.
A practical approach: start with walking 15 to 20 minutes daily during the first month. Add resistance training two to three times per week starting in month two. Gradually increase duration and intensity as energy permits. The goal is consistency, not intensity, especially during the adjustment phase.
Semaglutide and dietary optimization
The right eating plan while on semaglutide focuses on nutrient density rather than calorie restriction. Every calorie you consume needs to work harder when you are eating fewer total calories.
Priority foods for energy include fatty fish (omega-3s reduce inflammation), leafy greens (iron, magnesium, folate), eggs (complete protein, B12, choline), berries (antioxidants protect mitochondria), and nuts and seeds (magnesium, healthy fats, vitamin E).
Foods that tend to worsen fatigue on semaglutide include processed carbohydrates (blood sugar spikes), fried or very fatty foods (worsen GI symptoms and slow digestion further), excessive sugar (energy crashes), and alcohol, since drinking on semaglutide amplifies dehydration and interferes with metabolism.
Semaglutide and sleep optimization
Investing in sleep quality multiplies the energy benefits of semaglutide. Consider a sleep study if you have a history of snoring, obesity, or daytime sleepiness. Even if weight loss eventually resolves sleep apnea, treating it now means better energy during the weight loss process.
Sleep hygiene basics bear repeating because they are so effective: consistent wake time, bedroom temperature between 65 and 68 degrees Fahrenheit, blackout curtains, no screens 30 minutes before bed, and no caffeine after noon.
Semaglutide and stress management
Chronic stress and semaglutide is a difficult combination for energy. Cortisol disrupts blood sugar regulation, counteracting one of semaglutide's primary energy-improving mechanisms. It disrupts sleep, reducing the restorative benefits of better sleep quality. And it promotes inflammation, working against semaglutide's anti-inflammatory effects.
If you are starting semaglutide during a high-stress period, be realistic about energy expectations. The medication will still produce weight loss and metabolic improvements. But the energy benefits may be muted until stress is managed.
When to talk to your doctor about energy on semaglutide
Most fatigue on semaglutide resolves on its own with proper nutrition, hydration, and time. But some situations require medical attention.
See your provider if:
Fatigue persists beyond 12 weeks despite following all recommended strategies
You experience extreme fatigue that prevents normal daily activities
Fatigue worsens rather than improves over time
You develop additional symptoms like hair loss, extreme cold sensitivity, or depression
Your fatigue is accompanied by dizziness, rapid heart rate, or shortness of breath
These patterns may indicate thyroid dysfunction, severe anemia, cardiac issues, or other conditions that need separate evaluation. Semaglutide does not cause these conditions, but it can unmask them by changing metabolic demands, or the fatigue might be entirely unrelated to the medication.
Your provider may check thyroid function (TSH, free T4), complete blood count, iron studies, B12 levels, vitamin D, and basic metabolic panel to rule out treatable causes of persistent fatigue. The relationship between semaglutide and systemic effects means monitoring overall health markers during treatment is always wise.
The bottom line on semaglutide and energy
Does semaglutide give you energy? Not directly. It does not contain a stimulant. It does not speed up your metabolism. It will not make you feel wired or amped up.
What it does is far more valuable. It creates the metabolic conditions for sustained, genuine energy improvement. Better insulin sensitivity means steadier blood sugar. Reduced inflammation means fewer resources diverted to immune activation. Improved mitochondrial efficiency means more ATP from the same fuel. Weight loss means less physical burden on every system in your body. Better sleep means deeper recovery and more restorative rest.
The path to that energy improvement often runs through a valley of initial fatigue. Weeks two through six can be genuinely tough. But the people who maintain proper nutrition, stay hydrated, follow the titration schedule, and give their body time to adapt overwhelmingly report that the energy on the other side was worth the temporary discomfort.
For researchers serious about optimizing their GLP-1 protocols, SeekPeptides provides the most comprehensive resource available. From dosage calculators to diet planning guides, fatigue management protocols, and a community of thousands who have navigated these exact questions, SeekPeptides members access the tools and guidance that turn a good medication into great results.
Frequently asked questions
Does semaglutide give you energy or make you tired?
Both, depending on the timeline. Most people experience mild to moderate fatigue during the first 2 to 6 weeks due to reduced caloric intake, GI side effects, and metabolic adaptation. After this adjustment period, the majority of users report improved, more stable energy from better blood sugar control, reduced inflammation, weight loss, and improved sleep quality.
How long does semaglutide fatigue last?
The most intense fatigue typically lasts 4 to 8 weeks, coinciding with the initial titration period and the body's metabolic adaptation. Most people notice meaningful energy improvement by weeks 8 to 12. Persistent fatigue beyond 12 weeks usually indicates nutritional deficiencies, inadequate caloric intake, or an underlying condition that needs separate evaluation.
Why do I feel so tired on semaglutide?
The most common causes are insufficient caloric intake (eating too little due to appetite suppression), dehydration from GI side effects, protein deficiency, vitamin B12 or iron deficiency, and the body's metabolic adaptation process. Addressing nutrition and hydration first resolves fatigue for the majority of users. Review your semaglutide diet plan to ensure adequate nutrition.
Can I take anything to boost energy while on semaglutide?
Yes. B12 supplementation (1,000 to 2,500mcg methylcobalamin daily) is the most evidence-supported option. Magnesium glycinate (200 to 400mg daily) supports ATP production and sleep. CoQ10 (100 to 200mg) supports mitochondrial function. Creatine (3 to 5g daily) supports cellular energy recycling. Always discuss supplements with your provider. Some people benefit from semaglutide formulations that include B12.
Does semaglutide affect sleep?
Semaglutide can improve sleep quality indirectly through weight loss, which reduces sleep apnea risk and improves breathing during sleep. GLP-1 receptor agonist users show a 40% lower likelihood of obstructive sleep apnea. However, some people experience disrupted sleep during the initial adjustment period, particularly if GI symptoms are active at night.
Is the energy boost from semaglutide permanent?
The energy improvements persist as long as you maintain the underlying benefits: healthy weight, good nutrition, adequate sleep, and regular activity. If you stop semaglutide and regain weight, the energy benefits associated with weight loss would also diminish. The metabolic improvements, including enhanced mitochondrial efficiency, may persist for some time after discontinuation but require ongoing healthy habits to maintain.
Should I take semaglutide in the morning or evening for better energy?
Semaglutide is a once-weekly injection, so time of day matters less than with daily medications. However, many users prefer evening injection because it allows them to sleep through the peak side-effect window (first 24 to 48 hours). This can minimize the perception of fatigue. Learn more about optimal semaglutide timing and how it affects your daily experience.
Will losing weight on semaglutide give me more energy even if the medication itself does not?
Absolutely. Weight loss from any method improves energy through reduced physical burden, improved cardiovascular function, better sleep quality, and decreased inflammation. Semaglutide produces average weight loss of 12 to 15%, which translates to significant improvements in daily energy. The medication adds extra benefits through its direct anti-inflammatory and metabolic effects that pure dietary weight loss may not achieve to the same degree.
External resources
Effects of once-weekly semaglutide on appetite, energy intake, and body weight (PMC)
Semaglutide-induced weight loss improves mitochondrial energy efficiency in skeletal muscle (PMC)
Effects of semaglutide on C-reactive protein in adults with overweight or obesity (The Lancet)
In case I do not see you, good afternoon, good evening, and good night. May your energy stay steady, your metabolism stay efficient, and your protocols stay on track.