Feb 19, 2026

Before you draw another dose of semaglutide, consider this. The FDA has documented cases where patients injected five to twenty times their intended dose because they confused units with milligrams. That is not a typo. Five to twenty times too much, all from a simple math error on a syringe they thought they understood.
The problem is deceptively simple. Your healthcare provider prescribes a dose in milligrams. Your syringe measures in units. And the relationship between those two numbers changes depending on the concentration of your specific vial. Get the conversion right and you are on track. Get it wrong and you are either wasting medication or flooding your system with far more than intended.
This guide breaks down the complete process for converting semaglutide units to milligrams. Every concentration. Every formula. Every common mistake. Whether you are working with a 5 mg/mL vial, a 10 mg formulation, or something in between, by the end of this article the math will feel second nature. And more importantly, you will never second-guess your dose again.
SeekPeptides has put together this resource because dosing accuracy is not optional. It is the foundation of safe, effective research with GLP-1 receptor agonists. And the conversion from units to milligrams is where most errors begin.
Why semaglutide units and milligrams are not the same thing
This is where the confusion starts for nearly everyone. Units and milligrams measure two completely different things. Milligrams measure the weight of the active ingredient, the actual amount of semaglutide in your dose. Units measure the volume of liquid you draw into a syringe. These are not interchangeable. They are not even close to the same measurement.
Think of it this way.
A standard insulin syringe holds 1 mL of liquid, divided into 100 units. Each unit represents 0.01 mL of volume. That is all a unit tells you, how much liquid you are drawing. It tells you nothing about how many milligrams of semaglutide that liquid contains.
The amount of semaglutide in those units depends entirely on concentration. A vial labeled 5 mg/mL contains 5 milligrams of semaglutide dissolved in every milliliter of liquid. A vial labeled 2.5 mg/mL contains half that amount in the same volume. So 20 units drawn from a 5 mg/mL vial delivers 1 mg of semaglutide. But 20 units from a 2.5 mg/mL vial delivers only 0.5 mg.
Same number on the syringe. Completely different dose.
This distinction matters more than most people realize. A compounded semaglutide vial from one pharmacy might come as 2.5 mg/mL while another pharmacy sends 5 mg/mL. If you switch pharmacies and keep drawing the same number of units, you could double your dose overnight without realizing it.
The relationship between units, milliliters, and milligrams is straightforward once you understand the underlying logic. One milliliter always equals 100 units on an insulin syringe. That never changes. The variable is always the concentration, how much semaglutide is packed into each milliliter. Once you know your concentration, the conversion becomes basic arithmetic. Without it, you are guessing.

The core formula for converting semaglutide units to mg
Every semaglutide conversion uses one formula. Learn this and you can calculate any dose from any concentration.
mg = (Units x Concentration in mg/mL) / 100
That is it. Three numbers. One multiplication. One division. The reason this works is simple. There are 100 units in 1 mL. So dividing by 100 converts your units into milliliters first, then multiplying by concentration converts milliliters into milligrams.
Here is a practical example. You have a 5 mg/mL vial and you draw 10 units.
mg = (10 x 5) / 100 = 50 / 100 = 0.5 mg
You just drew 0.5 mg of semaglutide. Simple.
Now reverse it. Your provider prescribed 1.0 mg and you need to know how many units to draw from a 5 mg/mL vial.
Units = (mg x 100) / Concentration in mg/mL
Units = (1.0 x 100) / 5 = 100 / 5 = 20 units
Both formulas are two sides of the same coin. You will use the first when you know the units and need the mg. You will use the second when you know the mg and need the units. For detailed peptide dosage calculations, this same logic applies to virtually every injectable medication.
Why concentration is the critical variable
The concentration on your vial label determines everything. It is the bridge between volume (what your syringe measures) and dose (what your body receives). Without knowing your exact concentration, the formula is useless.
Compounding pharmacies produce semaglutide in a range of concentrations. The most common ones you will encounter include 1 mg/mL, 2 mg/mL, 2.5 mg/mL, 3 mg/mL, 5 mg/mL, and sometimes even 10 mg/mL. Each concentration requires a different number of units for the same milligram dose.
Brand-name products like Ozempic use pre-filled pens with fixed concentrations, which eliminates the math entirely. The pen dials to specific milligram doses and delivers the correct volume automatically. But compounded semaglutide comes in multi-dose vials that require manual measurement with an insulin syringe. This is where the conversion formula becomes essential.
Always check your vial label before every dose. Even if you have been using the same pharmacy for months, concentrations can change between refills. A quick label check takes two seconds. A dosing error can take weeks to recover from.
The quick reference shortcut
If memorizing formulas is not your style, here is a shortcut that works for any concentration. Divide 100 by your concentration to find out how many units equal 1 mg.
For 5 mg/mL: 100 / 5 = 20 units per mg
For 2.5 mg/mL: 100 / 2.5 = 40 units per mg
For 10 mg/mL: 100 / 10 = 10 units per mg
Once you know your "units per mg" number, multiply by your prescribed dose. Need 0.5 mg from a 5 mg/mL vial? That is 20 x 0.5 = 10 units. Need 1.7 mg from a 2.5 mg/mL vial? That is 40 x 1.7 = 68 units. This mental math approach is faster than the full formula and works perfectly for on-the-spot calculations. Use our semaglutide dosage calculator to verify your math every time.
Complete conversion tables for every semaglutide concentration
Below you will find conversion tables for every standard semaglutide concentration. These cover the full range of doses used in clinical practice and research. Bookmark this section, because you will come back to it.
Each table shows the milligram dose, the equivalent in units on an insulin syringe, and the corresponding volume in milliliters. All three numbers represent the same dose expressed in different measurement systems. Understanding how they relate is the foundation of accurate semaglutide dosing.
1 mg/mL concentration
This is the lowest common concentration, typically found in early-stage prescriptions or diluted formulations. Because the concentration is low, you need more volume (more units) for each milligram.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.125 mg | 12.5 units | 0.125 mL |
0.25 mg | 25 units | 0.25 mL |
0.5 mg | 50 units | 0.50 mL |
0.75 mg | 75 units | 0.75 mL |
1.0 mg | 100 units | 1.00 mL |
At 1 mg/mL, you need 100 units to deliver just 1 mg. That fills an entire 1 mL syringe. Higher doses are not practical at this concentration because they would require more volume than a standard syringe holds. If your prescribed dose exceeds 1 mg and your vial is 1 mg/mL, you likely need a higher concentration formulation.
2 mg/mL concentration
A step up in concentration. Common in some compounded formulations combined with B12.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.25 mg | 12.5 units | 0.125 mL |
0.5 mg | 25 units | 0.25 mL |
1.0 mg | 50 units | 0.50 mL |
1.5 mg | 75 units | 0.75 mL |
2.0 mg | 100 units | 1.00 mL |
Notice the pattern. At 2 mg/mL, every dose requires exactly half the units compared to 1 mg/mL. If you previously used a 1 mg/mL vial and switch to 2 mg/mL, you must cut your units in half to maintain the same milligram dose. This is one of the most common sources of dosing errors when patients switch between concentrations.
2.5 mg/mL concentration
One of the most widely used concentrations for compounded semaglutide. Many compounding pharmacies default to this formulation, particularly for semaglutide combined with cyanocobalamin.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.25 mg | 10 units | 0.10 mL |
0.5 mg | 20 units | 0.20 mL |
0.75 mg | 30 units | 0.30 mL |
1.0 mg | 40 units | 0.40 mL |
1.25 mg | 50 units | 0.50 mL |
1.5 mg | 60 units | 0.60 mL |
1.7 mg | 68 units | 0.68 mL |
2.0 mg | 80 units | 0.80 mL |
2.4 mg | 96 units | 0.96 mL |
2.5 mg | 100 units | 1.00 mL |
At 2.5 mg/mL, 40 units equals 1 mg. This is an easy number to remember. If you are titrating through the standard semaglutide dosing schedule, you start at 10 units (0.25 mg) and increase by 10 units every four weeks. Clean, simple increments.
3 mg/mL concentration
Less common than 2.5 mg/mL or 5 mg/mL, but some pharmacies use this formulation. The math is slightly less intuitive.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.25 mg | 8.3 units | 0.083 mL |
0.5 mg | 16.7 units | 0.167 mL |
0.75 mg | 25 units | 0.25 mL |
1.0 mg | 33.3 units | 0.333 mL |
1.5 mg | 50 units | 0.50 mL |
2.0 mg | 66.7 units | 0.667 mL |
2.4 mg | 80 units | 0.80 mL |
3.0 mg | 100 units | 1.00 mL |
Notice the fractional units. When your calculation produces a number like 8.3 or 16.7 units, round to the nearest whole unit marking on your syringe. Most insulin syringes have markings at every 1 or 2 units, so rounding by half a unit introduces minimal error. Your semaglutide syringe dosage chart should account for these rounding adjustments.
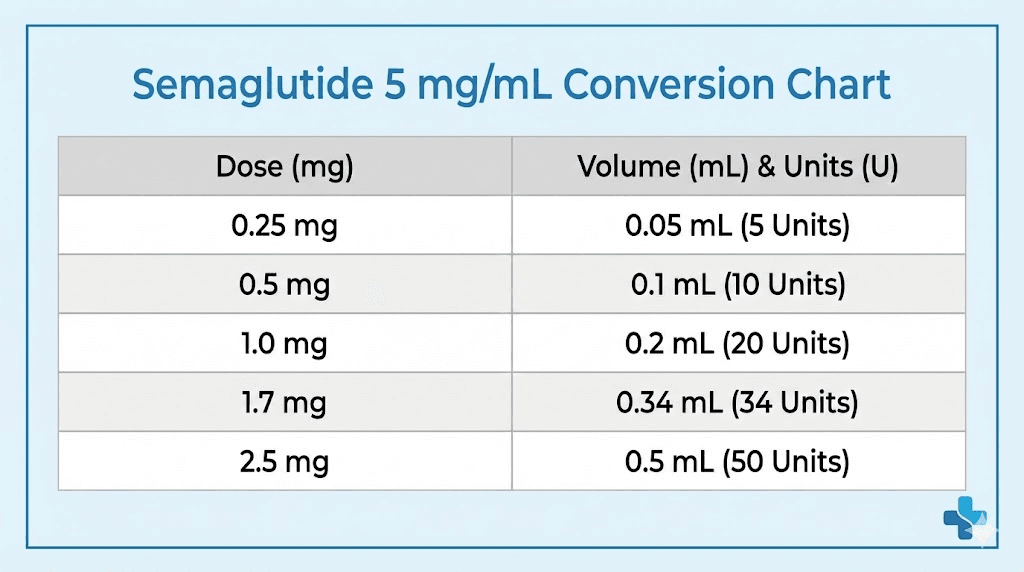
5 mg/mL concentration
This is the most common concentration for compounded semaglutide vials. It offers a good balance between injection volume and dosing precision. If you are using compounded semaglutide, there is a strong chance your vial is 5 mg/mL.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.25 mg | 5 units | 0.05 mL |
0.5 mg | 10 units | 0.10 mL |
0.75 mg | 15 units | 0.15 mL |
1.0 mg | 20 units | 0.20 mL |
1.25 mg | 25 units | 0.25 mL |
1.5 mg | 30 units | 0.30 mL |
1.7 mg | 34 units | 0.34 mL |
2.0 mg | 40 units | 0.40 mL |
2.4 mg | 48 units | 0.48 mL |
2.5 mg | 50 units | 0.50 mL |
The 5 mg/mL concentration is elegant. Twenty units per milligram. Small injection volumes across the entire dosing range. Even the maximum clinical dose of 2.4 mg requires only 48 units, well within what a standard syringe can deliver comfortably. This is why most guides, including our semaglutide 5 mg dosage chart, focus on this concentration first.
If your vial says 5 mg/mL and your provider says to take 0.25 mg, draw exactly 5 units. If your provider increases you to 0.5 mg, draw 10 units. Each step up in the titration schedule adds just 5 units. Clean. Predictable. Hard to mess up.
10 mg/mL concentration
The highest concentration you are likely to encounter. This formulation packs twice the semaglutide into each milliliter compared to 5 mg/mL, which means smaller injection volumes but less room for measurement error.
Dose (mg) | Units | Volume (mL) |
|---|---|---|
0.25 mg | 2.5 units | 0.025 mL |
0.5 mg | 5 units | 0.05 mL |
1.0 mg | 10 units | 0.10 mL |
1.5 mg | 15 units | 0.15 mL |
2.0 mg | 20 units | 0.20 mL |
2.4 mg | 24 units | 0.24 mL |
2.5 mg | 25 units | 0.25 mL |
5.0 mg | 50 units | 0.50 mL |
10.0 mg | 100 units | 1.00 mL |
At 10 mg/mL, a single unit error on your syringe equals 0.1 mg of semaglutide. That might not sound like much, but at the starting dose of 0.25 mg, drawing 3 units instead of 2.5 means you are taking 0.3 mg, a 20% overdose. For the 10 mg/mL concentration, precision matters more than at any other concentration.
This is one reason why many providers and pharmacists recommend 5 mg/mL as the default, especially for patients doing their own injections. The slightly larger volume gives more room for minor measurement variations without dramatically changing the actual dose received.
How to use an insulin syringe for semaglutide dosing
If you have never used an insulin syringe before, the markings can look intimidating. They should not be. Once you understand the basics, reading a syringe is as simple as reading a ruler.
A standard U-100 insulin syringe comes in three common sizes. The 0.3 mL syringe holds 30 units. The 0.5 mL syringe holds 50 units. The 1 mL syringe holds 100 units. The size you need depends on your dose volume. For most semaglutide doses measured in mL, a 0.5 mL or 1 mL syringe works perfectly.
Reading the markings
On a 1 mL (100-unit) syringe, each small line represents 1 unit. On a 0.5 mL (50-unit) syringe, each small line represents 1 unit as well, but the markings are more spread out and easier to read at low volumes. On a 0.3 mL (30-unit) syringe, each line represents 0.5 units, giving you the finest precision.
Always read the syringe at the top of the plunger seal, where the rubber meets the barrel. Do not read at the bottom of the seal, the halfway point, or the tip of the plunger. The top of the seal, closest to the needle, is your measurement line.
For anyone learning proper injection technique, our guide on how to inject GLP-1 medications covers the full process from preparation to administration.
Choosing the right syringe size
Match your syringe to your dose volume. If your calculated dose is 10 units (0.1 mL), a 0.3 mL syringe gives the best precision. If your dose is 50 units (0.5 mL), use a 0.5 mL or 1 mL syringe. Never use a syringe where your dose falls in the bottom 10% of its capacity, because the markings become too compressed to read accurately.
Some researchers prefer peptide injection pens for even greater precision. These dial-a-dose devices eliminate syringe reading entirely. But for standard vial-and-syringe protocols, the right syringe size paired with careful measurement delivers excellent accuracy.
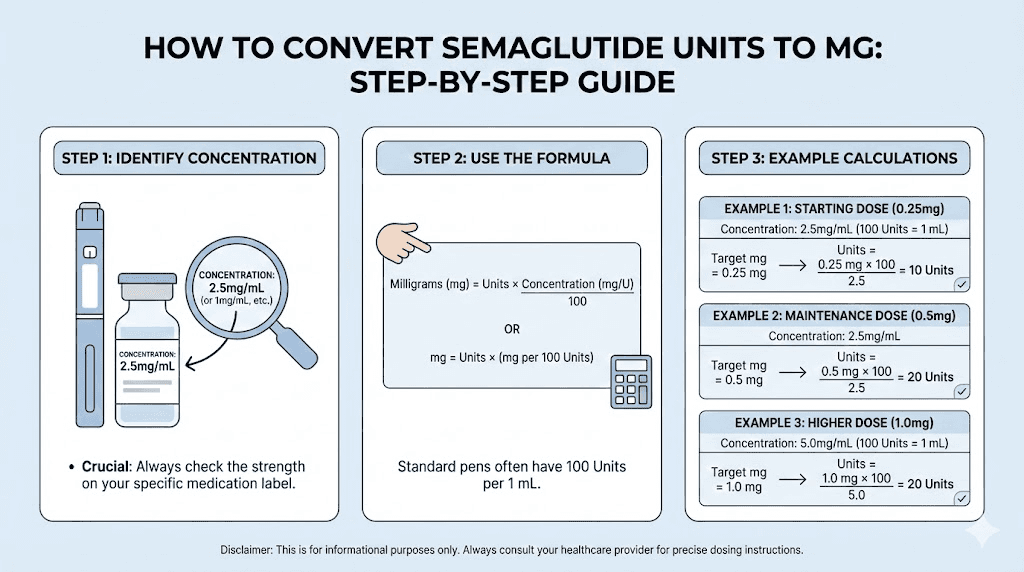
Step-by-step conversion examples
Theory is useful. Practice is better. Here are real-world conversion scenarios you are likely to encounter, worked through from start to finish.
Example 1: Starting dose from a 5 mg/mL vial
Your provider prescribes 0.25 mg weekly. Your vial label reads 5 mg/mL.
Step 1: Identify your concentration. 5 mg/mL.
Step 2: Apply the formula. Units = (0.25 x 100) / 5 = 25 / 5 = 5 units.
Step 3: Draw 5 units on your insulin syringe.
Step 4: Verify. 5 units from a 5 mg/mL vial = (5 x 5) / 100 = 0.25 mg. Confirmed.
This is the standard starting dose in most semaglutide conversion charts. If you can do this one, you can do any of them.
Example 2: Mid-titration dose from a 2.5 mg/mL vial
Your provider increases you to 1.0 mg weekly. Your vial is 2.5 mg/mL.
Step 1: Concentration is 2.5 mg/mL.
Step 2: Units = (1.0 x 100) / 2.5 = 100 / 2.5 = 40 units.
Step 3: Draw 40 units.
Step 4: Verify. (40 x 2.5) / 100 = 1.0 mg. Correct.
At the 2.5 mg/mL concentration, reaching the 1.0 mg dose requires 40 units, nearly half a standard syringe. Compare that to just 20 units at 5 mg/mL. Same milligram dose, double the volume.
Example 3: Maximum dose from a 10 mg/mL vial
Your provider prescribes the maximum clinical dose: 2.4 mg weekly. Your vial is 10 mg/mL.
Step 1: Concentration is 10 mg/mL.
Step 2: Units = (2.4 x 100) / 10 = 240 / 10 = 24 units.
Step 3: Draw 24 units.
Step 4: Verify. (24 x 10) / 100 = 2.4 mg. Confirmed.
At 10 mg/mL, even the maximum dose requires only 24 units. That is a tiny injection volume of 0.24 mL. Comfortable, quick, and precise, assuming you read the syringe carefully. Our semaglutide syringe dosage conversion chart provides a visual reference for scenarios exactly like this.
Example 4: Switching concentrations mid-protocol
You have been drawing 20 units from a 5 mg/mL vial (1.0 mg). Your pharmacy sends a new vial at 2.5 mg/mL. How many units do you need now?
Step 1: Your dose is 1.0 mg (unchanged).
Step 2: New concentration is 2.5 mg/mL.
Step 3: Units = (1.0 x 100) / 2.5 = 40 units.
You now need to draw 40 units instead of 20 to get the same 1.0 mg dose. If you kept drawing 20 units from the 2.5 mg/mL vial, you would only get 0.5 mg, half your intended dose. This is exactly the type of scenario that causes problems when people follow their routine on autopilot without checking the vial label.
For anyone navigating concentration changes, pharmacy-specific dosage charts can help ensure accuracy during transitions.
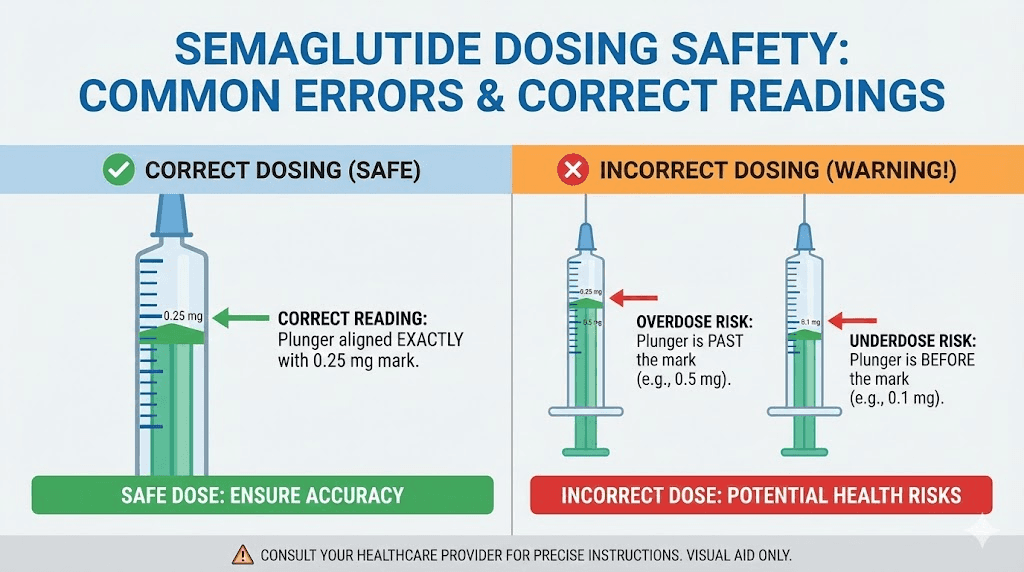
Common mistakes that lead to wrong semaglutide doses
Dosing errors with semaglutide are not rare. They happen to smart, careful people who simply misunderstand one piece of the equation. Here are the most common mistakes and exactly how to avoid each one.
Mistake 1: Assuming units equal milligrams
This is the single most dangerous mistake. A patient prescribed 0.5 mg draws 50 units, thinking units and milligrams are the same thing. From a 5 mg/mL vial, 50 units actually delivers 2.5 mg, five times the intended dose.
The fix: Always convert. Never assume. If your prescribed dose is in milligrams and your syringe measures in units, you must do the math. There is no shortcut around this step. Use the semaglutide dosage calculator on SeekPeptides to double-check your work every single time.
Mistake 2: Using the wrong concentration in your calculation
You calculate your dose using 2.5 mg/mL, but your actual vial is 5 mg/mL. Now you are drawing double the units you need. This happens most often when someone refills a prescription and the pharmacy changes the concentration without making it obvious.
The fix: Read your vial label before every injection. Not just the first time. Every time. Concentration can change between refills, between pharmacies, and even between batches from the same pharmacy.
Mistake 3: Confusing mL with units
Someone told to inject 0.5 mL draws 50 units instead of 0.5 mL. On a 1 mL (100-unit) syringe, 0.5 mL and 50 units are actually the same thing, so this works out. But on a 0.3 mL (30-unit) syringe, the scales are different, and drawing to the "50" line is impossible because the syringe only goes to 30. Confusion sets in, and people start guessing.
The fix: Always work in units. Convert your milligram dose to units using the formula, then draw that many units. Ignore the mL scale on the syringe entirely. Units are universal across all insulin syringes.
Mistake 4: Rounding errors at high concentrations
At 10 mg/mL, each unit on the syringe represents 0.1 mg. Drawing one unit too many or too few changes your dose by 0.1 mg. At the starting dose of 0.25 mg, that is a 40% swing. These small rounding errors compound over time, potentially leading to inconsistent semaglutide results.
The fix: Use the smallest syringe that fits your dose. For doses under 15 units, a 0.3 mL syringe provides the finest gradations and most readable markings. For understanding when results typically appear, see our guide on how long semaglutide takes to work.
Mistake 5: Not accounting for dead space
Every syringe has a small amount of "dead space" in the hub where the needle attaches. This is liquid that gets drawn into the syringe but never gets injected. At very small volumes (under 5 units), dead space can represent a meaningful percentage of the total dose.
The fix: Use low dead-space syringes designed for precise small-volume injections. These syringes minimize waste and improve accuracy at tiny volumes. Most pharmacy-grade insulin syringes sold in the US are already low dead-space, but check the packaging if you are unsure.
Mistake 6: Mixing up vials
If you use multiple medications, accidentally drawing from the wrong vial delivers the wrong medication entirely. This is not specific to semaglutide, but it happens more than people admit.
The fix: Store vials separately. Label them clearly. Always read the vial label twice before drawing. If you are managing multiple peptide storage protocols, dedicated storage containers for each medication reduce the risk of mix-ups.
FDA safety warnings about semaglutide dosing errors
This is not theoretical. The FDA has issued explicit warnings about dosing errors with compounded semaglutide, and the data is alarming.
Healthcare providers have incorrectly calculated intended doses when converting from milligrams to either units or milliliters. In documented cases, patients administered five to twenty times more than their intended dose. That is not a minor overshoot. At the starting dose of 0.25 mg, a 20x error means receiving 5 mg in a single injection, the equivalent of 20 weeks of starting doses delivered all at once.
The consequences are severe. Patients have experienced extreme nausea, uncontrollable vomiting, dangerous drops in blood sugar, and in some cases required emergency medical intervention. One documented case involved a provider who intended to prescribe 0.25 mg (5 units from a 5 mg/mL vial) but instead prescribed 25 units, delivering 1.25 mg, five times the intended dose. The patient experienced severe vomiting for days.
Another common scenario involves the decimal point. A patient meant to draw 5 units (0.05 mL) but drew to the 50-unit line instead (0.5 mL), receiving ten times their intended dose. On a 1 mL syringe, the difference between 5 and 50 is the difference between a tiny mark near the bottom and the halfway point of the barrel. Easy to confuse if you are not paying close attention.
These warnings apply specifically to compounded semaglutide products used with standard insulin syringes. Brand-name products like Ozempic and Wegovy use pre-filled pens that prevent this type of error entirely, since patients never need to calculate or measure doses manually.
The lesson is clear. Double-check every calculation. Verify your concentration. Use a calculator if you have any doubt. The two minutes spent verifying could prevent days of adverse effects. For comprehensive safety information, see our peptide safety guide.
How reconstitution affects your semaglutide conversion
If you are working with lyophilized (freeze-dried) semaglutide that requires reconstitution before use, the amount of bacteriostatic water you add directly determines the concentration, and therefore your units-to-mg conversion.
This is critical to understand. The concentration on a reconstituted vial is not fixed by the manufacturer. You create it based on how much water you add.
The reconstitution formula
Concentration (mg/mL) = Total mg in vial / Total mL of water added
A 5 mg vial reconstituted with 1 mL of bacteriostatic water produces a 5 mg/mL solution. The same 5 mg vial reconstituted with 2 mL produces 2.5 mg/mL. Add 5 mL and you get 1 mg/mL.
Same vial. Same peptide. Three completely different concentrations. Three completely different unit-to-mg conversions.
For 5 mg semaglutide reconstitution, the most common approach uses 1 mL of bacteriostatic water to create a 5 mg/mL solution. This matches the standard conversion tables above. But if your protocol calls for a different dilution, you need to recalculate everything.
Detailed guides for specific reconstitution volumes include our 5 mg reconstitution chart and 10 mg reconstitution chart. If you are mixing for the first time, our semaglutide mixing chart walks through the entire process.
Bacteriostatic water volume matters
The amount of bacteriostatic water you use is not arbitrary. Using too little creates a highly concentrated solution where small syringe errors become magnified. Using too much creates a dilute solution that requires large injection volumes.
For a 5 mg vial mixed with the right amount of bac water, the sweet spot is usually 1 mL, creating a 5 mg/mL concentration. For a 10 mg vial, using 2 mL of water also produces 5 mg/mL. Both approaches give you the same working concentration and the same conversion math.
Our peptide reconstitution calculator automates this entire process. Enter your vial size, the amount of water added, and your desired dose, and it calculates the exact number of units to draw. No manual math required.
Always document your reconstitution
Write the concentration directly on the vial using a permanent marker after reconstitution. Include the date you mixed it and the concentration in mg/mL. Six days from now, when you are drawing your weekly dose, you do not want to rely on memory for a number that determines your dosing accuracy.
Proper peptide storage after reconstitution is equally important. Reconstituted semaglutide should be refrigerated at 2-8 degrees Celsius. Understanding how long compounded semaglutide lasts in the fridge ensures you are not using degraded medication, which could lead to underdosing even with perfect unit-to-mg conversion.
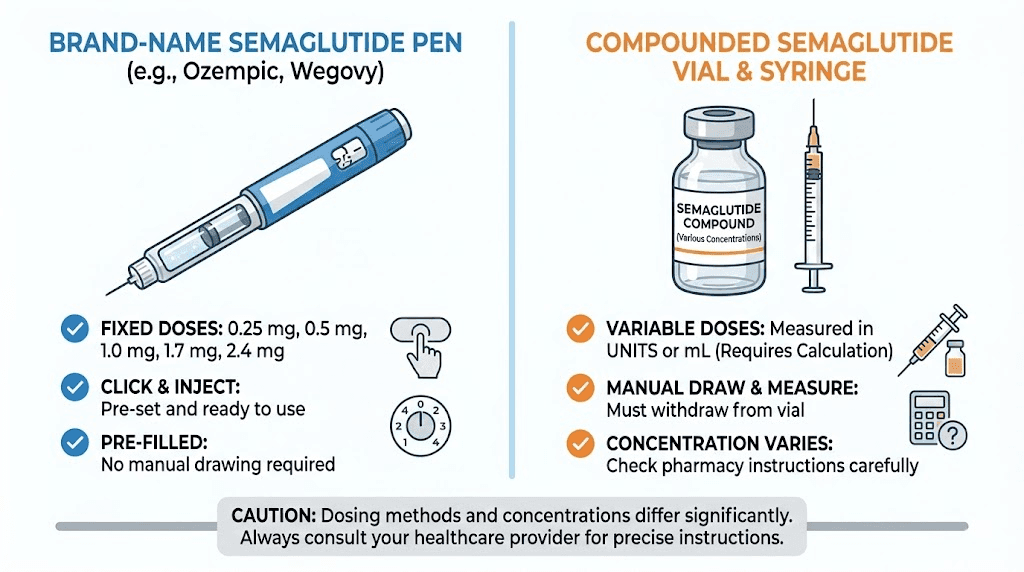
Brand-name semaglutide vs compounded semaglutide conversions
The conversion challenge primarily affects people using compounded semaglutide from vials. Brand-name products handle dosing differently, and understanding these differences helps explain why the conversion topic matters so much for certain groups of users.
Brand-name products (Ozempic, Wegovy)
Ozempic and Wegovy come in pre-filled injection pens. These pens have dose selectors that click to specific milligram amounts. You never see units, milliliters, or concentration numbers. You simply dial to 0.25 mg, 0.5 mg, 1.0 mg, or whatever your prescribed dose is, and inject. The pen delivers the exact volume needed automatically.
This design eliminates conversion errors entirely. It is also why brand-name products have a lower rate of dosing mistakes compared to compounded versions. The trade-off is cost and availability.
Compounded semaglutide from pharmacies
Compounded semaglutide comes in multi-dose vials with a stated concentration (typically 2.5 mg/mL or 5 mg/mL). You draw your dose manually using an insulin syringe. This requires you to convert your milligram prescription into units on the syringe, which is the entire reason this guide exists.
Different compounding pharmacies use different concentrations, different vial sizes, and sometimes even different salt forms of semaglutide. Empower Pharmacy, Olympia Pharmacy, and Direct Meds each have their own formulations. Always use the concentration printed on your specific vial, not a number from a generic chart online.
Compounded semaglutide with additives
Many compounding pharmacies add ingredients like B12 (cyanocobalamin), methylcobalamin, or glycine to their semaglutide formulations. These additives change the total volume of the solution but do not change the semaglutide concentration listed on the label.
The conversion formula still works exactly the same way. The semaglutide concentration (mg/mL) on the label already accounts for the total solution volume including any additives. You do not need to adjust your calculations for B12 or other ingredients.
Standard semaglutide titration schedule in units
Most semaglutide protocols follow a gradual titration, starting at the lowest dose and increasing every four weeks until reaching the target dose. Understanding this schedule in units for your specific concentration eliminates the need to recalculate every time your dose changes.
Titration schedule for 5 mg/mL concentration
Weeks | Dose (mg) | Units | Frequency |
|---|---|---|---|
Weeks 1-4 | 0.25 mg | 5 units | Once weekly |
Weeks 5-8 | 0.5 mg | 10 units | Once weekly |
Weeks 9-12 | 1.0 mg | 20 units | Once weekly |
Weeks 13-16 | 1.7 mg | 34 units | Once weekly |
Week 17+ | 2.4 mg | 48 units | Once weekly |
Each step in the titration adds a predictable number of units. From 0.25 mg to 0.5 mg, you go from 5 to 10 units. From 0.5 mg to 1.0 mg, you go from 10 to 20 units. The increments make sense mathematically, and your syringe makes them easy to measure.
Titration schedule for 2.5 mg/mL concentration
Weeks | Dose (mg) | Units | Frequency |
|---|---|---|---|
Weeks 1-4 | 0.25 mg | 10 units | Once weekly |
Weeks 5-8 | 0.5 mg | 20 units | Once weekly |
Weeks 9-12 | 1.0 mg | 40 units | Once weekly |
Weeks 13-16 | 1.7 mg | 68 units | Once weekly |
Week 17+ | 2.4 mg | 96 units | Once weekly |
Notice that at 2.5 mg/mL, the maximum dose of 2.4 mg requires 96 units, nearly filling an entire 1 mL syringe. This is approaching the practical limit for this concentration. If your provider prescribes doses above 2.4 mg for any reason, you may need a higher concentration vial.
The titration approach helps manage semaglutide side effects like constipation and fatigue by giving the body time to adjust at each dose level. If side effects become problematic at any point, providers often recommend staying at the current dose for an additional four weeks before increasing. For detailed information about what to expect, see semaglutide one month results.
Many people wonder about the best time of day to inject semaglutide. The answer depends on individual tolerance, but consistency matters more than timing. Pick a day and a time, then stick to it. That consistency makes the weekly routine automatic and reduces the chance of missed or double doses.
Quick-reference master table: all concentrations side by side
This single table shows how the same milligram dose requires different numbers of units depending on concentration. Print this out, save a screenshot, or bookmark it. This is the most useful reference in this entire guide.
Dose (mg) | 1 mg/mL | 2 mg/mL | 2.5 mg/mL | 3 mg/mL | 5 mg/mL | 10 mg/mL |
|---|---|---|---|---|---|---|
0.25 mg | 25 units | 12.5 units | 10 units | 8.3 units | 5 units | 2.5 units |
0.5 mg | 50 units | 25 units | 20 units | 16.7 units | 10 units | 5 units |
1.0 mg | 100 units | 50 units | 40 units | 33.3 units | 20 units | 10 units |
1.7 mg | - | 85 units | 68 units | 56.7 units | 34 units | 17 units |
2.0 mg | - | 100 units | 80 units | 66.7 units | 40 units | 20 units |
2.4 mg | - | - | 96 units | 80 units | 48 units | 24 units |
Dashes indicate doses that exceed the 100-unit capacity of a standard 1 mL syringe at that concentration. For those doses, you need a higher concentration formulation. For even more specific dosage references, check our articles on how many mg is 40 units of semaglutide and how many mg is 50 units.
Understanding what your syringe numbers actually mean
Let us address a point of confusion that trips up even experienced users. The numbers on an insulin syringe are unit markings, not milligram markings and not milliliter markings. They represent volume divisions of the total syringe capacity.
On a 100-unit (1 mL) syringe:
10 on the syringe = 10 units = 0.10 mL
25 on the syringe = 25 units = 0.25 mL
50 on the syringe = 50 units = 0.50 mL
100 on the syringe = 100 units = 1.00 mL
The milligram value of each number depends entirely on what medication is in the syringe and at what concentration. Ten units of semaglutide could be 0.1 mg (from a 1 mg/mL vial), 0.5 mg (from a 5 mg/mL vial), or 1.0 mg (from a 10 mg/mL vial). The syringe does not know what is inside it. That is your job.
This is why the phrase "units to mg" exists as a search query. People see a number on their syringe and want to know what it means in milligrams. The answer is always: it depends on your concentration. Our dedicated article on 100 units of semaglutide in milligrams explores the high-volume end of this spectrum.
Tools and calculators for accurate semaglutide dosing
Manual math works. But calculators are faster and eliminate human error. Several tools exist to make semaglutide unit-to-mg conversion automatic.
Online dosage calculators
The SeekPeptides semaglutide dosage calculator handles the conversion instantly. Enter your vial concentration and desired dose in milligrams, and it returns the exact number of units to draw. No formulas to remember. No mental math. Just accurate results.
For broader peptide calculations beyond semaglutide, the general peptide calculator supports multiple compounds and concentration formats. The reconstitution calculator is particularly useful if you are mixing your own vials and need to determine the resulting concentration before calculating units.
Dosage tracking tools
Beyond one-time calculations, tracking your doses over time helps identify patterns and ensures consistency. Tools like the GLP-1 plotter and GLP-1 companion apps let you log each injection, track your titration progress, and monitor for dose-dependent side effects.
The peptide cost calculator adds another dimension by calculating the per-dose cost at different concentrations. Higher concentration vials often cost more upfront but deliver more doses per vial, reducing the per-injection price. Understanding your cost-per-mg helps inform purchasing decisions.
Printable reference charts
For those who prefer physical references, printable dosage charts for each concentration can be laminated and stored with your supplies. Our 5 mg/2 mL dosage chart, semaglutide B12 dosage chart, and IVIM dosing chart are formatted for quick reference during preparation.
SeekPeptides members get access to all of these tools plus personalized protocol guidance that accounts for individual factors like body weight, prior GLP-1 experience, and specific health goals. Accurate dosing is just the starting point. Optimizing your entire protocol is where real results happen.
What to do if you think you drew the wrong dose
Mistakes happen. Even with perfect knowledge of the conversion formula, a moment of distraction can lead to drawing the wrong number of units. Here is what to do in different scenarios.
If you have not injected yet
Simply empty the syringe back into the vial (or discard the contents into a sharps container if sterility is a concern), get a fresh syringe, and start over. There is no harm in wasting one syringe load of medication to ensure accuracy. The cost of a new syringe is trivial compared to the consequences of an incorrect dose.
If you already injected too much
Do not panic, but do take it seriously. Contact your healthcare provider or pharmacist to report the overdose amount. Common symptoms of semaglutide overdose include severe nausea, vomiting, and potential hypoglycemia. Have a source of glucose available (juice, candy, glucose tablets) in case blood sugar drops. Monitor symptoms for 24-48 hours, as semaglutide effects can take time to develop.
If you experience severe vomiting that prevents keeping fluids down, or if you feel faint or confused, seek emergency medical attention. These symptoms could indicate significant hypoglycemia or dehydration.
If you already injected too little
An underdose is far less concerning than an overdose. You simply received less medication than intended. Do not inject a second time to "make up" the difference, as this creates the risk of double-dosing if your initial measurement was actually correct. Instead, note the error and ensure accuracy on your next scheduled dose. One week of lower-than-intended dosing will not significantly impact your overall protocol.
For ongoing support with dose management, many people find that understanding common peptide mistakes helps them establish better habits from the start. And if you are concerned about not seeing results on semaglutide, inaccurate dosing is often the first thing to investigate.
Special conversion scenarios
Not every situation fits neatly into the standard tables. Here are some less common but important conversion scenarios.
Microdosing semaglutide
Some protocols call for doses below the standard 0.25 mg starting dose. At 5 mg/mL, a 0.125 mg dose requires just 2.5 units. That is a tiny volume that pushes the limits of syringe accuracy. For microdosing, consider using a 0.3 mL (30-unit) syringe where the markings are spaced further apart, making small volumes easier to measure precisely.
Alternatively, reconstituting to a lower concentration (like 2.5 mg/mL) doubles the volume needed for the same dose, making it easier to measure. A 0.125 mg dose from a 2.5 mg/mL vial requires 5 units, a much more manageable measurement. Our semaglutide appetite suppression guide explores how even low doses can produce meaningful effects.
Converting between semaglutide and tirzepatide
If your provider switches you from semaglutide to tirzepatide, the unit-to-mg conversion follows the same formula but with tirzepatide concentrations instead. The two medications are not dose-equivalent, meaning 1 mg of semaglutide does not equal 1 mg of tirzepatide in terms of clinical effect.
Our semaglutide to tirzepatide conversion chart provides the clinical equivalencies, while the switching guide covers the practical protocol for transitions. For tirzepatide-specific unit conversions, see our tirzepatide dosage in units guide.
Working with sublingual or oral semaglutide
The unit-to-mg conversion discussed throughout this guide applies specifically to injectable semaglutide. Oral semaglutide drops and sublingual formulations use different delivery mechanisms and different dosing systems. Oral semaglutide (Rybelsus) comes in tablet form measured directly in milligrams, with no unit conversion needed.
If you are comparing GLP-1 medications like Ozempic across different formulations, remember that bioavailability differs between injection and oral routes. The same milligram amount delivers different effective doses depending on how it enters the body.
Traveling with semaglutide
When traveling with semaglutide, keep a written record of your concentration, dose in mg, and dose in units. If your vial label becomes damaged or unreadable during travel, this record ensures you can still dose accurately. Pack backup syringes, as using a different syringe size than usual can affect how you read the markings.
Building a foolproof dosing routine
Knowing the math is one thing. Building habits that prevent errors is another. Here is a system that works.
The five-point verification checklist
Before every injection, run through these five checks:
1. Read the vial label. Confirm the medication name is semaglutide (not something else stored nearby) and note the concentration in mg/mL.
2. Confirm your prescribed dose. Check your prescription label or dosing instructions for the milligram amount. Do not rely on memory, especially if your dose recently changed during titration.
3. Calculate or look up your units. Use the formula, a chart, or a calculator. If using a chart, make sure it matches your exact concentration.
4. Draw the dose. Pull back the plunger slowly and read at the top of the plunger seal. If the first attempt does not land perfectly on the correct marking, push back and redraw.
5. Double-check before injecting. One final look at the syringe to confirm the units match your calculation. This takes two seconds and eliminates the most common errors.
For beginners starting with peptides, this checklist might feel excessive. Give it a few weeks and it becomes automatic, like checking your mirrors before changing lanes. You stop thinking about it, but you never stop doing it.
Keeping a dosing log
Record every injection with the date, time, concentration, milligram dose, and units drawn. A simple notebook works. So does a phone note or spreadsheet. This log serves multiple purposes. It confirms you dosed correctly. It tracks your titration progress. It provides data if you need to discuss your protocol with a healthcare provider.
The log also catches errors retroactively. If you notice side effects that seem disproportionate to your dose, reviewing your log might reveal a calculation mistake or concentration change you overlooked. Speaking of side effects, understanding what to expect helps distinguish normal adaptation from dosing problems, whether that is semaglutide burping, energy changes, or appetite suppression timing.
Semaglutide dosing beyond the basics
Once you have mastered the unit-to-mg conversion, a few advanced topics become relevant to your overall semaglutide protocol.
How long your vial should last
Knowing your dose in both mg and units lets you calculate how many doses one vial contains. A 5 mg vial at a dose of 0.5 mg per week lasts 10 weeks. A 10 mg vial at 1.0 mg per week lasts 10 weeks. A 5 mg vial at 2.4 mg per week lasts just over 2 weeks.
Understanding vial duration helps with refill planning and recognizing when a vial should be running low. If your vial is lasting significantly longer or shorter than expected, it could indicate a dosing error worth investigating. For storage considerations, review semaglutide refrigeration requirements and shelf life after opening.
Combining semaglutide with other compounds
Some protocols combine semaglutide with other peptides or supplements. If these additional compounds require their own reconstitution and injection, each one has its own concentration and conversion math. Never mix medications in the same syringe unless specifically instructed by a healthcare provider.
Popular combinations include semaglutide with phentermine for enhanced weight management, and semaglutide alongside high-protein nutrition strategies. For comprehensive dietary guidance while using GLP-1 medications, see our semaglutide diet plan and food recommendations.
Managing dose adjustments
Dose adjustments happen for many reasons. Side effects, plateaus, changing goals, or provider recommendations can all trigger a dose change. Each time your dose changes, recalculate your units. Do not estimate based on your previous dose. A fresh calculation takes 30 seconds and ensures accuracy.
If you are experiencing a plateau after 4 weeks on semaglutide, the issue might not be dosing at all. Factors like diet quality, protein intake, sleep, and exercise all influence outcomes. But ruling out dosing inaccuracy first is always the right starting point.
For those considering how long to continue therapy, our guide on semaglutide treatment duration covers the evidence-based approach to long-term use, and understanding what happens when stopping semaglutide helps with planning your exit strategy.
Comparing semaglutide conversions with other GLP-1 medications
Semaglutide is not the only GLP-1 medication that requires unit-to-mg conversion. Understanding how the math applies across different medications provides useful context.
Tirzepatide dosing follows the same fundamental formula. Units = (mg x 100) / concentration. The difference is that tirzepatide concentrations, dose ranges, and titration schedules are different from semaglutide. If your provider switches you between the two, you need separate conversion charts for each medication. Our semaglutide to tirzepatide switching chart covers the clinical equivalencies.
Retatrutide, a newer triple-agonist peptide, uses similar injection methods and the same type of conversion math. Cagrilintide combined with semaglutide (CagriSema) introduces another set of concentrations and dose requirements. Each medication has its own conversion table, but the underlying formula never changes.
The universal formula, Units = (mg x 100) / concentration, works for any injectable medication measured with an insulin syringe. Learn it once, use it everywhere. For a broader overview of peptide dosage calculations, our comprehensive guide covers the math behind every common injectable.
For researchers serious about optimizing their peptide protocols, SeekPeptides offers the most comprehensive resource available, with evidence-based guides, detailed conversion tools, and a community of thousands who have navigated these exact questions.
Frequently asked questions
How many units of semaglutide equal 1 mg?
It depends entirely on your vial concentration. At 5 mg/mL, 20 units equals 1 mg. At 2.5 mg/mL, 40 units equals 1 mg. At 10 mg/mL, 10 units equals 1 mg. Always divide 100 by your concentration to find the number of units per milligram. Use the semaglutide dosage calculator for instant conversions.
Is 20 units of semaglutide the same as 1 mg?
Only if your vial concentration is 5 mg/mL. At 2.5 mg/mL, 20 units equals 0.5 mg. At 10 mg/mL, 20 units equals 2 mg. The concentration on your specific vial determines the milligram value of any unit measurement.
What is the difference between units and mg on a syringe?
Units measure volume (how much liquid you draw). Milligrams measure weight (how much active drug is in that liquid). An insulin syringe only shows units. To know the milligrams, you must multiply units by your vial concentration and divide by 100.
Can I use the same conversion chart for all semaglutide vials?
No. Conversion charts are concentration-specific. A chart made for 5 mg/mL will give you the wrong dose if your vial is 2.5 mg/mL. Always verify that any chart you use matches the exact concentration printed on your vial label. See our complete conversion chart for every concentration.
Why did my pharmacy change the concentration of my semaglutide?
Compounding pharmacies may adjust concentrations based on ingredient availability, cost, or formulation preferences. When your concentration changes, your units must change to maintain the same milligram dose. Always recalculate when you receive a new vial.
Is 20 units of semaglutide too much?
That depends on your concentration and your prescribed dose. At 5 mg/mL, 20 units is 1.0 mg, a standard mid-range dose. At 10 mg/mL, 20 units is 2.0 mg, a high dose. At 2.5 mg/mL, 20 units is just 0.5 mg, a relatively low dose. The unit number alone tells you nothing without knowing the concentration.
How do I convert semaglutide units to mL?
Divide units by 100. That is it. 10 units = 0.10 mL. 50 units = 0.50 mL. 100 units = 1.00 mL. This conversion is fixed regardless of medication or concentration because insulin syringes always have 100 units per mL. For detailed volume references, see 20 units in mL and our semaglutide dosage chart in mL.
What happens if I accidentally take too much semaglutide?
Contact your healthcare provider. Symptoms of overdose include severe nausea, vomiting, and potential low blood sugar. Have glucose available. If symptoms are severe, seek emergency medical care. For ongoing management of common side effects at correct doses, see our guides on GLP-1 side effects.
External resources
In case I do not see you, good afternoon, good evening, and good night. May your conversions stay accurate, your doses stay precise, and your results stay consistent.